15-Month Sleep Regression
Sarah Mitchell
Sarah Mitchell is a Registered Pediatric Nurse and a mother of three who has spent over a decade helping families navigate the beautiful, chaotic early years of childhood. She combines evidence-based medical knowledge with real-world parenting experience to offer practical, compassionate advice. At Awesome Parent, Sarah's mission is to help exhausted parents find solutions, trust their instincts, and finally get some sleep.
If your toddler was sleeping fairly well and now bedtime feels like negotiating with a tiny, loud union rep, you are not imagining things. Around 15 months, many kids hit a bumpy patch that looks like a sleep regression: sudden bedtime tantrums, new night waking, early mornings, and naps that fall apart for no good reason.
One quick, nerdy-but-helpful caveat: not every expert labels this as a distinct, official “regression.” But parents recognize the pattern, and the solutions are the same either way.
As a pediatric nurse and a mom of three, I want you to hear this clearly: this is common, it is usually temporary, and you do not have to “pick a perfect method” to get through it. At this age, sleep struggles are often a mix of development (hello, language explosion), discomfort (teeth), and the very normal toddler job of testing boundaries.

What it looks like
Not every child checks every box, but these are the patterns I hear most often in clinic and in my own house:
- Bedtime resistance: crying when you start the routine, arching away from pajamas, screaming when you approach the crib.
- New separation anxiety: needing “one more hug” times 37, panicking when you leave the room.
- Night waking: waking and calling for you, sometimes multiple times.
- Nap refusal: fighting the nap, taking a short nap, or skipping it then melting down at 4 PM.
- Early morning wake-ups: up for the day at 5 to 6 AM and ready to party.
- More intense emotions: bigger tantrums around transitions like leaving the bath or turning off lights.
This phase often sits between the better-known 12-month and 18-month bumps, which is why it can feel like it came out of nowhere.
Why sleep gets wobbly
1) A language burst that revs the brain
Many toddlers around 15 months are suddenly understanding more and attempting more words. That is exciting, and it is also activating. A busy brain can mean:
- Harder time winding down
- More night waking as they practice sounds or seek reassurance
- More frustration when they cannot communicate what they want
2) Boundary testing is developmental
Your toddler is learning cause and effect. They are also learning that they can say “no” with their whole body. Bedtime is a perfect laboratory for testing: “If I cry, do I get picked up? If I stand up, does Mom come back? If I throw the pacifier, does Dad return?”
This is not manipulation. It is learning. Your job is to be steady and predictable.
3) Teething and discomfort
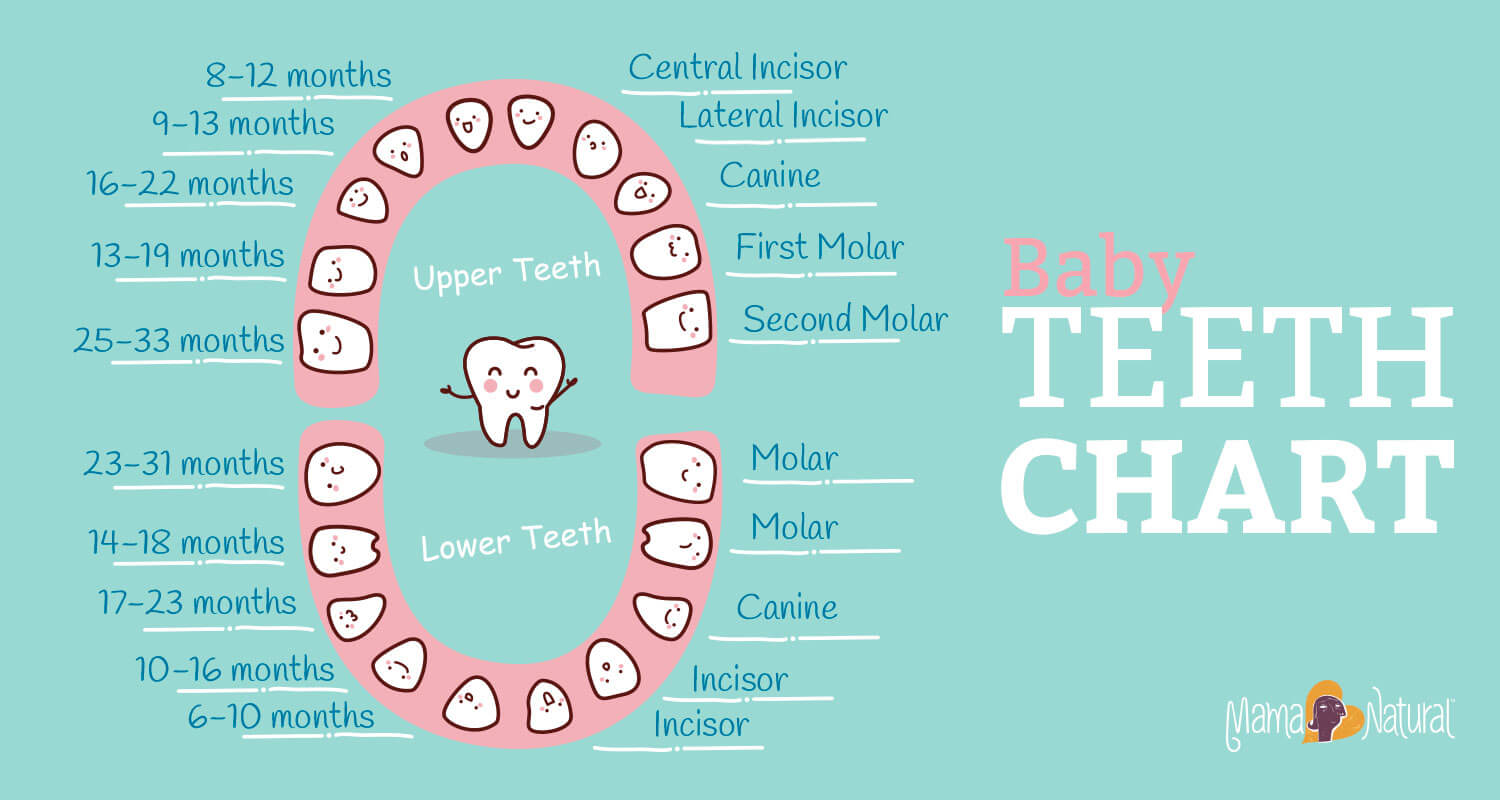
First molars often show up between 13 and 19 months. These teeth are bigger and can be more uncomfortable than earlier ones. Teething can cause extra drooling, chewing, crankiness, and night waking.
Teething can sometimes come with a slight temperature bump, but it should not cause a true fever or a truly sick child. If your child has a temperature of 100.4°F (38°C) or higher, significant diarrhea, or seems genuinely ill, do not chalk it up to teething. Call your pediatrician.
4) Schedule transitions and sleep pressure
At 15 months, many toddlers are on one nap, and plenty are still transitioning from two naps. Even toddlers solidly on one nap can temporarily need a slightly earlier bedtime if naps shorten.
When sleep pressure is off, you often see the classic combo: fighting bedtime but also waking more at night.
Quick check-in first
When sleep suddenly falls apart, I like parents to do a simple triage first. Ask:
- Is my child sick? New cough, ear tugging, congestion, vomiting, rash, fever, or unusual sleepiness warrants a call to your pediatrician.
- Is something in the environment different? Travel, new daycare room, a move, a new sibling, loud construction, room temperature changes. Many toddlers sleep best around 68 to 72°F (20 to 22°C).
- Are they getting enough calories during the day? Toddlers can get distractible with eating and then genuinely wake hungry at night.
- Is the schedule age-appropriate? Too much or too little daytime sleep can both cause night issues.
If your gut says “something is off,” trust that. This phase is common, but you know your child best.
Typical schedule
Every toddler is different, but most 15-month-olds do well with:
- Total sleep: about 11 to 14 hours in 24 hours
- One nap: usually 1.5 to 3 hours
- Wake windows: roughly 5 to 6 hours before nap, then 5 to 6 hours before bedtime
Sample day
- 6:30 AM wake
- 12:00 to 2:00 PM nap (adjust earlier if wake time is earlier)
- 7:30 PM bedtime
If your toddler is waking very early, pushing bedtime later usually backfires. Overtired toddlers tend to wake more, not less.

Bedtime routines that calm
At 15 months, the routine should be soothing, short, and repeatable. Think 20 to 30 minutes, same order every night. The goal is to lower stimulation and remove surprises.
A simple routine
- Bath or warm washcloth wipe-down
- Pajamas and diaper
- Brush teeth or wipe gums
- Two books
- Sleep sack, lights low
- Song, cuddle
- Into crib awake but calm (or drowsy if that is your current step)
And a note for the parents who just tensed up at “awake but calm”: this is not a requirement or a moral issue. For some toddlers, it is a long-term goal you work toward gradually. Responsive, step-by-step approaches count.
Two tweaks that matter
- Put connection first: 5 minutes of fully present snuggling before you ask them to separate can reduce protests.
- End with the same words: toddlers love predictability. A consistent phrase becomes a cue for sleep.
Night after night, your calm consistency teaches: “Bedtime is safe. You are loved. The plan is the plan.”
Scripts for boundaries
You do not need a big speech. You need a calm, boring script you can repeat like a lullaby. Say it kindly, then follow through.
When they scream as you leave
Script: “You are safe. It is sleep time. I love you. I will check on you.”
When they want one more book, snack, hug, anything
Script: “All done. Books are finished. It is bedtime.”
If you can offer a tiny choice without reopening negotiations, do it:
Script: “Do you want the bunny or the bear? Then we sleep.”
When they stand up in the crib
Script: “Time to lie down.”
Then gently lay them down with minimal eye contact and minimal conversation. Repeat as needed. The first nights can be repetitive. Your steadiness is the point.
When separation anxiety spikes
Script: “I hear you. I am right outside. I will see you in the morning.”
If check-ins make your child more upset, it is okay to choose fewer check-ins. If check-ins help, keep them brief and consistent.
Teething comfort (without new habits)
If you suspect first molars, comfort is reasonable. The trick is separating pain relief from new sleep associations.
What can help
- Cold teether before bed
- Gum massage with a clean finger
- Appropriate medication if needed (commonly acetaminophen or ibuprofen for this age), using label directions and your pediatrician’s guidance for your child’s weight and health history
- Extra hydration during the day
What to avoid
- Over-the-counter numbing gels with benzocaine unless your pediatrician specifically recommends it
- Amber teething necklaces (choking and strangulation risk)
- Adding new overnight “rules” you cannot live with long-term, like rocking for 45 minutes every wake
If pain seems severe or your toddler is waking crying in a way that feels different from protest, call your pediatrician. Ear infections can mimic teething, and I have seen many “regressions” that were actually ears.

Night waking at 2 AM
This is where parents get stuck, because you are tired, your toddler is loud, and nobody is thinking in full sentences.
A quick decision tree
- If they are sick, in pain, or the cry is unusual: respond and assess, then help them settle.
- If it sounds like protest: keep the response brief, calm, and consistent with your bedtime plan.
- If you suspect hunger: consider whether daytime intake has dipped or dinner was tiny. Then decide on a plan rather than improvising nightly.
Keep the room boring
- Lights dim
- Minimal talking
- No play, no snacks unless part of your intentional plan
- Back to sleep quickly
The more interesting the night becomes, the more likely your toddler will request it again tomorrow. This is one of the most common patterns I see.
When and how to cap night feeds
Some 15-month-olds are still nursing or taking a bottle overnight. That is not automatically “wrong,” but it can become the main reason for frequent waking.
In general, many healthy toddlers at this age can get their calories during the day. If your child is growing well and your pediatrician is not concerned, you can consider reducing night feeds if they are disrupting sleep.
Signs it is more habit than hunger
- They wake at the same times nightly like an alarm clock
- They take a small amount, then pop awake again soon after
- They fall asleep only while feeding and wake when transferred
Two gentle options
- Reduce volume or minutes gradually: every 2 to 3 nights, decrease a little. Keep the rest of the routine the same.
- Delay and resettle first: when they wake, offer comfort without feeding for a set period (for example 10 minutes). If they do not settle, feed. Over time, many kids drop the wake naturally.
If you choose to wean night feeds, expect some pushback for a few nights. That does not mean you are harming your child. It means they noticed the pattern changed.
Should you move bedtime?
Sometimes the fix is as simple as shifting bedtime earlier, especially if naps have shortened or childcare sleep is messy.
Try earlier bedtime if
- Nap is under 1.5 hours most days
- They are melting down in the hour before bed
- Night waking increased after a series of short naps
Try this
Move bedtime earlier by 15 to 30 minutes for 3 to 5 nights and reassess. Early bed can feel counterintuitive, but overtired toddlers often sleep more restlessly.
Consider later bedtime only if
- Your toddler is happily awake in the crib for 45 to 60 minutes before falling asleep
- They are taking a very long nap late in the day
In that case, you may need to wake from nap or shift the nap earlier rather than repeatedly pushing bedtime later.
Nap refusal
Nap battles at 15 months are often about timing or control.
Reset nap conditions
- Same pre-nap mini routine (diaper, book, sleep sack)
- Dark room and white noise if you use it
- Enough awake time before nap, often about 5 hours after morning wake
Use a crib break if they are furious
If your toddler is escalating, a brief reset can help you both.
- Calmly end the attempt after about 15 to 20 minutes of intense crying
- Do a quiet activity for 10 to 15 minutes (snuggle, look at books)
- Try again once
If nap truly does not happen, protect bedtime with an earlier sleep time. Skipping the nap and keeping the same bedtime usually leads to a long, crunchy evening.

Early mornings
Early morning wake-ups are common in this phase. A few practical levers that often help:
- Protect bedtime: early wakes often improve with an earlier bedtime, not a later one.
- Keep the room dark: treat anything before your target wake time like night. Blackout curtains can be a game changer.
- Bright light after wake: once it is “morning,” open blinds and get outdoor light early in the day to anchor the body clock.
Daycare sleep is messy
If your toddler is in daycare, you may have very limited control over nap timing or length. On daycare days with a short nap, an earlier bedtime is often the kindest fix. Think of it as a temporary “catch-up” bedtime, not a new permanent schedule.
Common mistakes
- Changing the plan every night: toddlers learn patterns fast. Consistency is kinder than constant experimentation.
- Accidentally rewarding stalling: extra snacks, extra play, extra screen time when they protest teaches “protest works.”
- Letting naps drift late: a late nap can steal sleep pressure from bedtime.
- Too much excitement before bed: roughhousing and bright screens right before sleep can backfire.
Safe sleep reminder
When you are exhausted, it is easy to make a desperate choice at 2 AM. Do your best to keep sleep spaces safe: use a firm crib mattress with a fitted sheet, and keep pillows, loose blankets, and soft items out of the crib if your guidance recommends a clear sleep space. If you ever bring your toddler into your bed, avoid couches and armchairs, which carry a high risk of accidental suffocation.
How long it lasts
Many families see improvement within 1 to 3 weeks once they stabilize the schedule and respond consistently. If it drags on, it usually means one of these is still in play: ongoing discomfort, a schedule mismatch, or a new habit that formed during the rough patch.
When to call the pediatrician
Reach out if you notice any of the following:
- Fever, persistent vomiting, or signs of dehydration (very few wet diapers, dry mouth, lethargy)
- Ear pain or frequent ear tugging with irritability
- Snoring most nights, pauses in breathing, or significant mouth breathing
- Reflux symptoms that seem painful, especially with poor weight gain
- Night waking with inconsolable crying that feels unlike your child’s normal upset
You are never “overreacting” by asking. Sometimes the most loving sleep strategy is treating the underlying issue.
A realistic 7-night plan
If you are exhausted and want a simple roadmap, here is one I would give a family at my triage desk:
- Night 1: Set a bedtime routine (20 to 30 minutes) and pick your script. Keep your response boring and consistent overnight.
- Night 2: Check schedule. Aim for a solid wake window before nap and bedtime. Do not chase a late nap.
- Night 3: If teething is likely, add comfort steps before bed. Consider appropriate pain relief if needed.
- Night 4: Decide what you will do about night feeds. Keep it consistent for the next few nights.
- Night 5: If naps are short, move bedtime earlier by 15 to 30 minutes.
- Night 6: Hold steady. This is often the night toddlers test hardest because they sense you are serious.
- Night 7: Reassess. Keep what is working, tweak one thing at a time.
You do not need perfection. You need repeatability.
One last reassurance
This age is intense. Your toddler is learning words, emotions, independence, and how to be a tiny human in a big world. Sleep disruptions are often part of that growth. You are not creating a “bad sleeper” by responding with love. The goal is to respond with love and clear boundaries.
If tonight feels like a lot, make the plan as simple as possible: calm routine, predictable response, and a bedtime that protects your child from overtired chaos. You can do hard nights and still be a great parent.