Acute Bronchitis in Kids
Sarah Mitchell
Sarah Mitchell is a Registered Pediatric Nurse and a mother of three who has spent over a decade helping families navigate the beautiful, chaotic early years of childhood. She combines evidence-based medical knowledge with real-world parenting experience to offer practical, compassionate advice. At Awesome Parent, Sarah's mission is to help exhausted parents find solutions, trust their instincts, and finally get some sleep.
If your child has a cough that will not quit, you are not alone. In clinic, one of the most common questions I heard was: “Is this bronchitis or just a cold, and why are we still coughing?”
Acute bronchitis is basically inflammation of the larger airways (the bronchi), usually after a viral cold. The main symptom is a cough that can hang on long after your child seems fine otherwise. The good news: most cases get better with time and supportive care. The important part is knowing what is normal, what helps, and what is a true breathing red flag.

What it is (and is not)
Acute bronchitis in kids
Acute bronchitis typically follows a run-of-the-mill upper respiratory infection. The airways in the chest get irritated and swollen, which triggers coughing. Many kids also have:
- Runny nose or sore throat at the beginning
- Low-grade fever early on (not always)
- Wet-sounding cough or congestion (the “chest rattle” parents describe), especially when mucus is hard to clear
- Cough that gets worse at night or with running around
Most cases are caused by viruses. That is why antibiotics usually do not help.
Quick myth-buster: Green or yellow mucus can happen with viral infections too. Color alone does not automatically mean it is bacterial or that antibiotics are needed.
Not bronchiolitis (babies)
This is where parents get understandably confused, because the words sound similar.
- Bronchiolitis is most common in babies and young toddlers under age 2. It affects the smallest airways (bronchioles) and can cause wheezing, fast breathing, and feeding trouble. RSV is a classic cause.
- Acute bronchitis is more often discussed in preschool and school-age kids. The main issue is usually a lingering cough after a viral illness.
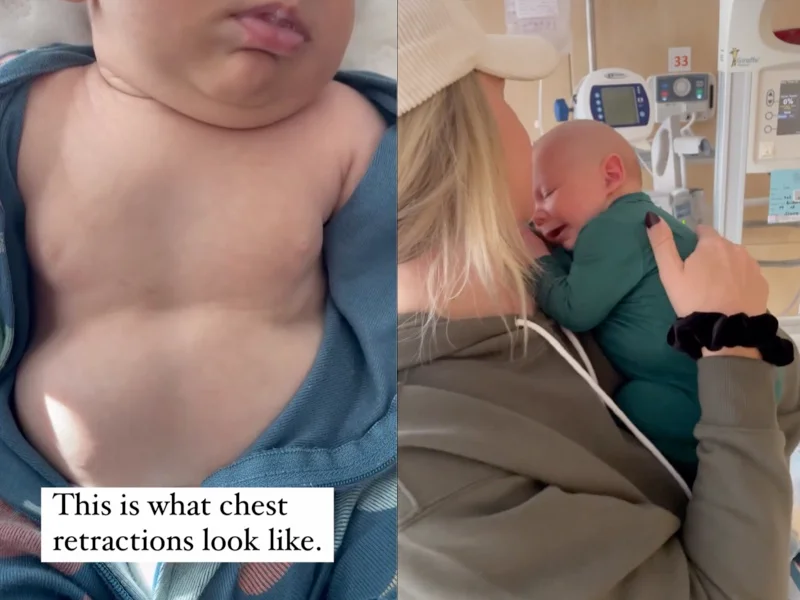
If you have an infant with cough plus rapid breathing, retractions (skin pulling in between ribs), or trouble feeding, think “bronchiolitis” and call your pediatrician promptly.
How long it lasts
This is the part no one wants to hear at 3 AM, but it helps to know what is typical.
- Days 1 to 3: Often starts like a cold. The cough may be dry or occasional.
- Days 4 to 10: Cough usually ramps up. Mucus can increase. Night cough is common.
- Weeks 2 to 3: Many kids are acting better but still coughing, especially with activity, cold air, or at bedtime.
- Up to 4 weeks: A post-viral cough can linger. This can still be within the normal range if your child is breathing comfortably, fever is gone, and energy is improving.
When duration becomes a clue: If the cough is not improving by about 3 to 4 weeks, or it is getting worse again after improving, it is worth a check-in. That can signal asthma, pneumonia, sinus infection with post-nasal drip, pertussis exposure, or another issue.
Home care that helps
Supportive care is not “doing nothing.” It is doing the right basics consistently, and skipping the stuff that is risky or ineffective.
1) Hydration
Fluids help thin mucus so it is easier to clear. Aim for frequent sips throughout the day.
- Water is great.
- Warm fluids (broth, caffeine-free tea) can be soothing for older kids.
- Popsicles count.
Tip from the triage desk: If your child is peeing less, has a dry mouth, or cries without tears, bump fluids and consider calling your pediatrician for guidance.
2) Humidifier (safe use)
A cool-mist humidifier can make coughing less harsh, especially at night. Place it a few feet from the bed and aim for comfortable ventilation in the room.
- Empty, rinse, and dry daily, and deep-clean on the schedule recommended by the manufacturer.
- Use distilled water if you can to reduce mineral buildup.
- Avoid over-humidifying. A simple goal is about 30% to 50% humidity to reduce mold and dust mites.
- Avoid hot steam humidifiers around children because of burn risk.

Honey, saline, and meds
Honey (over 1 year)
Honey has decent evidence for reducing nighttime cough in children older than 12 months. Typical studied doses are about 1/2 to 1 teaspoon (2.5 to 5 mL) about 30 minutes before bed.
- Give it straight, then offer a sip of water.
- Or mix into warm water for a simple “tea” for older kids.
Important: No honey for babies under 1 year due to botulism risk.
Saline for post-nasal drip
When mucus drips down the throat, it can trigger coughing that sounds “chesty” even when the lungs are fine. Saline spray or drops, plus gentle nose blowing (or suction for little ones), can reduce that drip.
Over-the-counter cough and cold meds
Most OTC cough and cold products do not help much and can cause side effects.
- The American Academy of Pediatrics advises avoiding OTC cough and cold medicines in children under 4.
- Many clinicians also recommend caution in children under 6, unless your pediatrician specifically advises otherwise.
If your child is older and you are considering something specific, check with your pediatrician or pharmacist for age-appropriate options and dosing.
What not to do (quick safety list)
- Avoid secondhand smoke and vaping exposure. Smoke is a major cough trigger and can prolong post-viral cough.
- Avoid codeine-containing cough medicines unless specifically prescribed, and even then ask about safer alternatives.
- Be cautious with essential oils around young children. Do not put oils directly into humidifiers, and stop if any irritation or coughing worsens.
Activity and school
Rest or move?
Light activity is fine if your child feels up to it. In fact, gentle movement can help loosen mucus. The rule I use at home is:
- If they are breathing comfortably and have decent energy, quiet play and a normal routine are okay.
- If running triggers a coughing fit, dial it back for a few days.
Back to school?
A lingering cough alone does not always mean contagious. Many kids can return when they:
- Have been fever-free for 24 hours without fever reducers
- Can participate in the day reasonably well
- Do not have significant breathing trouble
Also follow your school’s policy and any current guidance for illnesses like flu, COVID, or pertussis when relevant. If the cough is very frequent and disruptive, it may be kinder to keep them home and focus on rest and fluids for another day.
When to seek care
This is the “trust your gut” section. If your child looks like they are working hard to breathe, do not wait it out.
Go now (urgent or ER)
- Struggling to breathe, gasping, or unable to speak in full sentences (older kids)
- Fast breathing that does not settle with rest
- Retractions (skin pulling in between ribs or at the base of the neck)
- Nostrils flaring with each breath
- Lips or face turning blue or gray
- Extreme sleepiness or difficulty waking
Call soon (same day or next day)
- Fever lasts more than 3 days, or fever returns after a fever-free stretch
- Your child has chest pain or persistent one-sided pain
- They are not drinking well or peeing much less
- Cough lasts beyond 3 to 4 weeks or is steadily worsening
- You hear wheezing or your child has a history of asthma
- You suspect whooping cough exposure (especially if coughing fits cause vomiting or a “whoop”)
- Sudden cough onset after a choking episode, or a new cough with one-sided wheeze or uneven breath sounds (possible foreign body)
Could it be something else?
“Bronchitis” gets used casually, but sometimes a cough points to a different diagnosis. Here are a few clues clinicians consider:
Pneumonia
- Often has fever and a child who looks more ill
- Fast breathing and increased work of breathing are common
- Cough may be productive, but it can be dry too
Asthma
- Cough worse at night or with exercise
- Wheezing or tight chest
- History of eczema, allergies, or prior wheezing episodes
Post-nasal drip or sinus
- Cough worse when lying down
- Thick nasal drainage, bad breath, or symptoms lasting beyond the typical cold window
Pertussis
- Spells of coughing that are hard to stop
- May cause vomiting after coughing
- Can last for weeks
Flu or COVID
- Often has more whole-body symptoms like aches, fatigue, headache, or higher fever
- Testing can be worth considering during surges, before visits with high-risk relatives, or when it changes school and activity guidance
If any of these patterns fit, it does not mean you did anything wrong. It just means your child may benefit from an exam and possibly targeted treatment.
What the visit may include
Parents often expect a chest X-ray or antibiotics, and sometimes those are needed. Often, they are not. A typical evaluation might include:
- Listening to the lungs for wheeze, crackles, or decreased airflow
- Checking oxygen level with a pulse oximeter
- Assessing hydration and overall appearance
- Considering tests only when helpful, like a viral test or chest X-ray if pneumonia is suspected
If bronchospasm is present, your clinician may trial an inhaled bronchodilator. If bacterial pneumonia is suspected, antibiotics may be appropriate. For straightforward acute bronchitis, time and supportive care are usually the plan.
Bottom line
Acute bronchitis in kids is usually a post-viral airway irritation problem, not a bacterial infection problem. Expect the cough to peak in the first week and improve gradually, with some kids coughing for several weeks. Focus on hydration, cool-mist humidification (without over-humidifying), honey for kids over 1 year, keeping the nose clear, and avoiding smoke and other irritants.
And please remember: a cough can be annoying and still be normal. But breathing difficulty is never a wait-and-see symptom. If your child is working hard to breathe or looks “not right,” get medical care.