Alopecia Areata in Children: Patchy Hair Loss
Sarah Mitchell
Sarah Mitchell is a Registered Pediatric Nurse and a mother of three who has spent over a decade helping families navigate the beautiful, chaotic early years of childhood. She combines evidence-based medical knowledge with real-world parenting experience to offer practical, compassionate advice. At Awesome Parent, Sarah's mission is to help exhausted parents find solutions, trust their instincts, and finally get some sleep.
If you just found a smooth, round bald spot on your child’s head, your brain probably went straight to worst-case scenarios at 2 AM. I get it. In pediatric triage, hair loss questions were some of the most anxiety-filled calls because hair feels so tied to identity and health.
The good news is that patchy hair loss in kids is common. One common cause is alopecia areata, an immune-related condition that typically causes well-defined round or oval patches of hair loss. It is not contagious, and it is not caused by something you did or did not do.
A quick note: This article is general information, not a diagnosis. Your child’s clinician will individualize care based on age, exam, and local infection patterns.
Quick summary
- Smooth, round patch with normal-looking skin can fit alopecia areata.
- Scale, broken hairs, swollen neck nodes can point to tinea capitis (scalp ringworm) and needs oral treatment.
- Book a visit within 1 to 2 weeks for new patches (sooner if pain, oozing, fever, or boggy swelling).
- Nail pitting can be a clue in alopecia areata, but it is not required.
- Regrowth often happens, but timing varies and recurrences can occur.
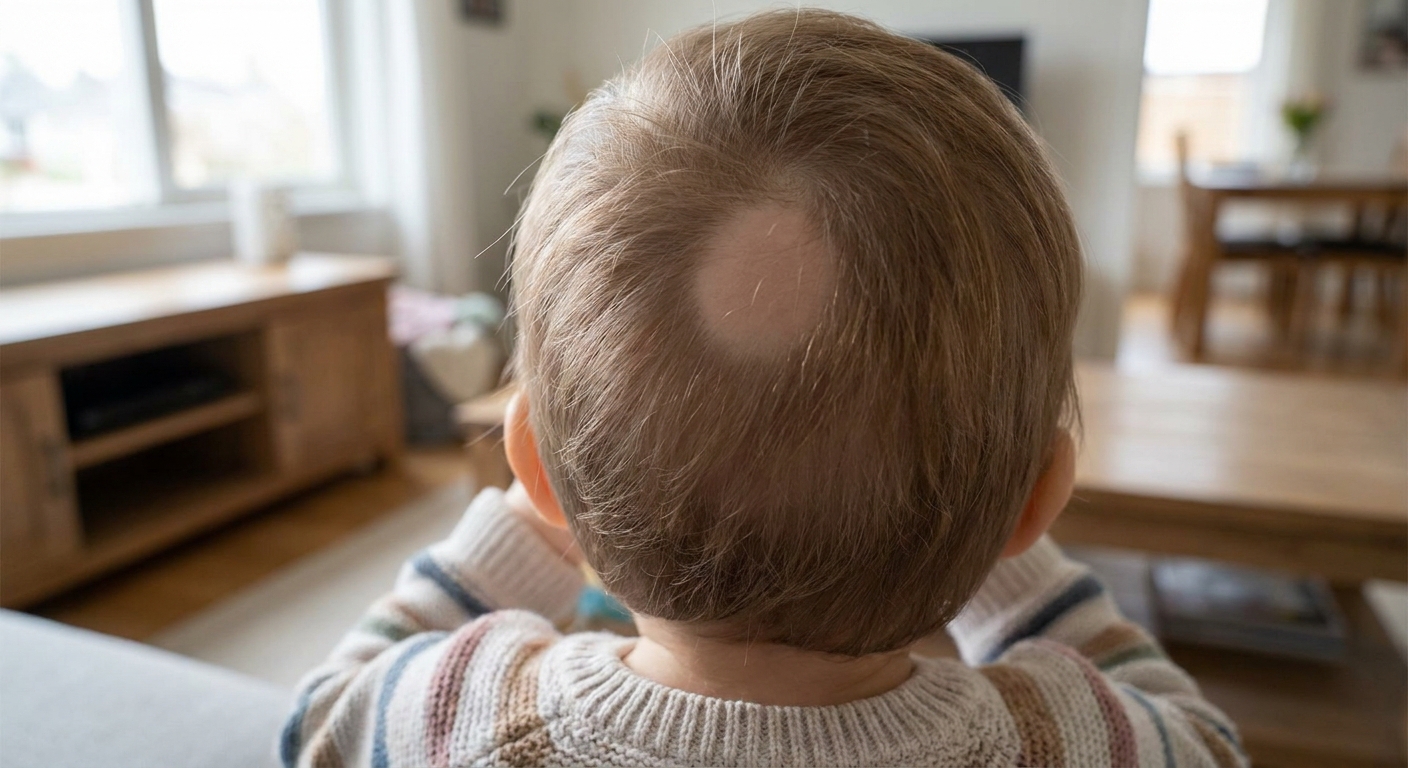
What it usually looks like
Alopecia areata most often shows up as one or more coin-shaped patches of hair loss on the scalp. Sometimes it appears in eyebrows or other body hair, but scalp patches are the classic starting point.
Clues parents notice
- Smooth skin where the hair is missing, without flaking, crusting, or redness
- Sudden discovery during brushing, bath time, or a haircut
- More than one patch, or a patch that slowly enlarges
- “Exclamation point” hairs at the edges (short hairs that are narrower at the base near the scalp and wider toward the tip). Many parents do not notice this, and that is fine.
Some kids have no symptoms at all. Others may mention mild scalp tingling or itch, but significant pain is not typical.
Patterns you might hear
- Patchy alopecia areata: the most common, one or multiple spots
- Alopecia totalis: loss of all scalp hair
- Alopecia universalis: loss of scalp and body hair
Most children with alopecia areata do not progress to total hair loss, but it is understandably scary to read those terms online. Your child’s pattern and exam are what matter most.
Nail clues
This is one of those nurse-triage details that can be surprisingly helpful: alopecia areata can affect nails. It is thought to be related to the same immune inflammation process, not because nails and hair are “made of the same thing.”
What to look for
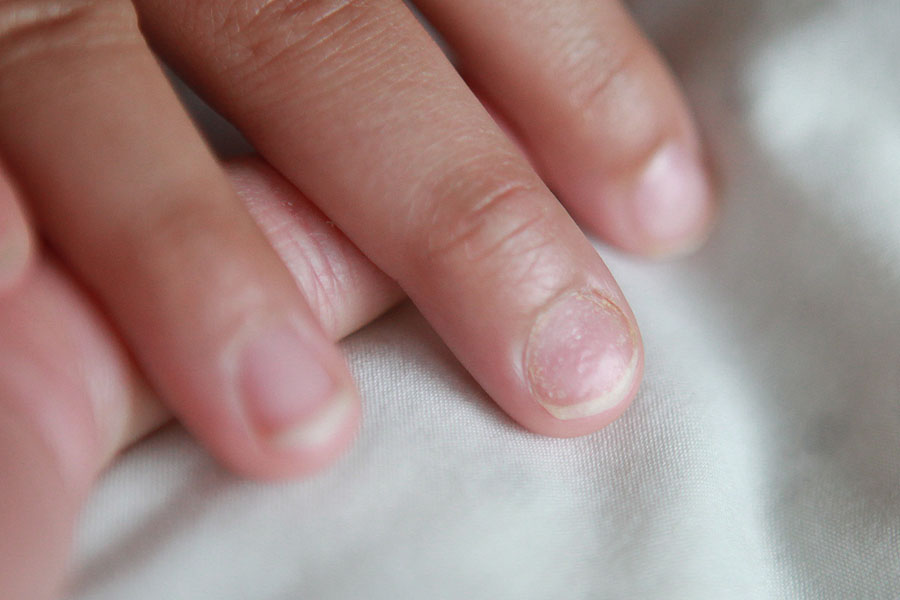
- Nail pitting: tiny dents that look like someone tapped the nail with the tip of a pin
- Ridges or roughness
- Thin, brittle nails
Nail changes do not prove alopecia areata on their own, but they can support the diagnosis. If you notice nail pitting, mention it at the appointment.
What your pediatrician will do
In primary care, the first goal is to figure out what kind of hair loss this is, because several common childhood conditions can look similar at a glance.
Step 1: History
- When you first noticed the patch, and whether it is changing
- Any itching, scaling, or tenderness
- Recent illnesses, new medications, major stressors, or fevers
- Hairstyles that pull (tight ponytails, braids, buns), helmets, or habitual rubbing
- Hair-pulling behaviors (sometimes unconscious), especially during stress or boredom
- Family history of alopecia areata or autoimmune conditions (thyroid disease, type 1 diabetes, vitiligo, celiac disease)
Step 2: Exam
Your child’s clinician will look for:
- Scale and broken hairs that suggest a fungal infection (tinea capitis, commonly called scalp ringworm)
- Redness, swelling, pustules, or tender lymph nodes
- Hair breakage patterns that fit tight hairstyles or friction
- Smooth, well-defined patches more consistent with alopecia areata
- Eyebrows, eyelashes, and a quick nail check
- Signs of scarring hair loss (less common): very shiny skin, loss of visible follicle openings, or skin texture change
Step 3: Testing or next steps
Testing depends on what the exam shows and practice varies.
- If fungal infection is suspected: treatment is usually an oral antifungal because topical treatments alone are not enough for tinea capitis. Your pediatrician may also do a fungal test depending on office setup and local practice.
- If alopecia areata is likely: many children do not need bloodwork right away. Some clinicians consider thyroid screening if there are symptoms, a strong personal or family history, Down syndrome, significant atopy, or other exam clues. Broad autoimmune screening is not routine for every child.
- If the diagnosis is uncertain: referral to dermatology is common. Dermatologists may use a handheld tool (dermoscopy) to look at follicles more closely.
Because hair loss can be emotionally intense, I generally encourage families to book an appointment within the next week or two for new patches. It is rarely an emergency, but you deserve a clear plan and reassurance.
Look-alikes
One reason I do not want you self-diagnosing from photos is that a few other common childhood conditions can mimic a bald patch, and the treatment is very different.
Tinea capitis (scalp ringworm)
- Often causes scaling, broken hairs, and sometimes itch
- May be associated with swollen lymph nodes in the neck
- Is contagious and usually needs oral treatment, not just shampoo
- A severe inflammatory form (kerion) can look like a boggy, tender swelling and should be evaluated promptly
Traction alopecia
- Hair loss from repeated pulling tension from hairstyles
- Often along hairline or areas under stress
- Improves by changing styles and reducing tension
Trichotillomania (hair pulling)
- Hair loss tends to be irregular with hairs of different lengths
- May occur during stress, anxiety, ADHD, or simply habit
- Supportive behavioral strategies and, sometimes, mental health support can help
Telogen effluvium (shedding after stress or illness)
- More diffuse thinning rather than one smooth patch
- Often follows a high fever, surgery, major stress, or significant illness by a few months
Seborrheic dermatitis or psoriasis
- Usually causes scale and irritation rather than a smooth, clean bald spot
- Can coexist with other causes, so it is worth pointing out any flaking you notice
If your child has scaling, crusting, oozing, pain, or rapid spreading, that is a clue to get seen sooner because alopecia areata itself usually does not cause those skin changes.
Myths that spike anxiety
Myth: “Alopecia areata means my child is very sick.”
Alopecia areata is an immune-related condition, but most children with it are otherwise healthy. It is not cancer. It is a diagnosis that deserves evaluation and follow-up, not panic.
Myth: “It is definitely caused by stress.”
Stress can be a trigger for many body changes, but alopecia areata is not simply a stress reaction. Please do not put that weight on your child’s shoulders.
Myth: “We must have a vitamin deficiency.”
Some nutritional issues can contribute to hair thinning, but the classic smooth round patches of alopecia areata are not typically solved by supplements. Your clinician can guide you if testing is appropriate.
Myth: “It is contagious, like ringworm.”
Alopecia areata is not contagious. Your child cannot give it to siblings or classmates by sharing hats or pillows.
Myth: “If it is alopecia areata, nothing can be done.”
There are management options that may help some children and families, and dermatology can be very helpful. At the same time, it is important not to promise a cure. Many cases improve, some recur, and the course can be unpredictable.
What happens next
Here is the most realistic, low-drama way to think about the next steps.
Within 1 to 2 weeks
- Primary-care visit to confirm likely cause and rule out infection
- Photos taken at home can be helpful. Use the same lighting and angle when possible.
Over 1 to 3 months
- Monitoring for new patches or regrowth
- If alopecia areata is suspected, many families are referred to dermatology for confirmation and treatment discussion
Longer term
- Regrowth can happen, but it often takes months
- Many children see meaningful regrowth within about a year, but relapses can happen
- Some features can be linked with a more persistent course (for example: extensive hair loss, certain band-like patterns, or significant nail involvement), but none of these predict an individual child with certainty
If you are waiting for a dermatology appointment, ask your pediatrician what to do in the meantime and what changes would warrant an earlier recheck.
What dermatology might offer
Dermatology treatment is tailored to your child’s age, how much hair loss there is, and how your child is coping. Options vary, but common discussions include:
- Watchful waiting: because spontaneous regrowth is common in limited patchy alopecia areata
- Topical corticosteroids: often a first-line option for kids
- Intralesional corticosteroid injections: sometimes used in older children with small patches (not everyone is a good candidate)
- Minoxidil as an add-on in select cases (usually to support regrowth, not to treat the underlying immune process)
- Topical immunotherapy or other specialty treatments for more extensive cases
What matters most is a plan you understand, plus a follow-up timeline so you are not stuck in limbo.
Supporting confidence
Kids take cues from us. If we act like hair loss is a catastrophe, they learn it is one. If we treat it like a health detail we are handling together, they feel safer.
What to say
- Simple and calm: “Your immune system is being a little overactive around your hair roots. It is not your fault, and we are seeing the doctor to help us understand it.”
- Body-neutral: “Bodies change. This is one of those changes.”
- Permission: “It is okay to feel mad or sad about it.”
What not to do
- Do not force hats or hairstyles if your child hates them
- Do not repeatedly check the patch in front of them like you are monitoring a crisis
- Do not talk about it as if it is a secret or something to be ashamed of
Practical options
- Let them choose: hat, headband, scarf, haircut, or nothing at all
- Talk to the teacher or school counselor if teasing is a concern
- Practice a one-sentence response for curious peers: “It is called alopecia. I’m healthy. My hair is just taking a break.”

When to call sooner
Most patchy hair loss can be handled with a routine appointment. Call your pediatrician sooner or request urgent evaluation if you notice:
- Redness, swelling, oozing, crusting, or significant pain
- Fever or your child seems ill
- Rapidly spreading rash or hair loss with tender bumps
- Large tender scalp swelling or pus-filled areas (including possible kerion)
- Hair loss plus new fatigue, weight changes, constipation, or heat or cold intolerance (possible thyroid concerns)
Prepare for the visit
- Bring a list of hair products used (including new ones)
- Note any recent illnesses, stressors, or changes in routine
- Snap a few clear photos of the patch over time
- Check nails quickly for pitting or ridges
- Write down questions you want answered, especially about school, sports, and teasing
If you feel overwhelmed, start with one goal: leave the visit knowing what the most likely diagnosis is and what the next step will be.
The bottom line
Alopecia areata in children often shows up as smooth, round patches of hair loss, sometimes with clues like nail pitting. It is not contagious, and it is not your fault. The main early job is to confirm the diagnosis and rule out look-alikes like scalp ringworm, then create a realistic plan for monitoring, possible dermatology referral, and emotional support.
If your child is worried about how they look, you are not overreacting by taking that seriously. Confidence is a health issue too, and you do not have to handle it alone.