Amoxicillin Rash in Kids: Harmless Pink Rash vs Concerning Allergy
Sarah Mitchell
Sarah Mitchell is a Registered Pediatric Nurse and a mother of three who has spent over a decade helping families navigate the beautiful, chaotic early years of childhood. She combines evidence-based medical knowledge with real-world parenting experience to offer practical, compassionate advice. At Awesome Parent, Sarah's mission is to help exhausted parents find solutions, trust their instincts, and finally get some sleep.
Few things make a parent’s stomach drop faster than seeing a new rash on a child who just started an antibiotic. I’ve taken those calls as a pediatric triage nurse, and I’ve had that exact moment at home with my own kids, staring at little pink spots and thinking, Is this normal… or dangerous?
The good news: a rash during amoxicillin is common in kids, and many of these rashes are not a true allergy. The tricky part is that some rashes are allergic and need immediate attention.

This guide will help you sort out what you are seeing, what to do today, and what to tell your child’s clinician or prescriber next time. (And a quick reminder: online info cannot diagnose your child. If your clinician gives you different instructions, follow those.)
First, the two big categories
When people say “amoxicillin rash,” they can mean two very different things:
- Non-allergic amoxicillin rash (benign antibiotic eruption): A common, usually harmless pink rash that often appears days into the course. Kids typically look and act well.
- Allergic reaction (often IgE-mediated): Can cause hives, swelling, breathing symptoms, or anaphylaxis. This is the one we take very seriously.
There are also rare but serious delayed reactions that are not the “typical” allergy and still need urgent evaluation. We will cover those too.
Harmless pink rash
Typical timing
A classic non-allergic amoxicillin rash usually shows up:
- Day 3 to Day 10 after starting amoxicillin (sometimes even near the end of the course)
- Occasionally after finishing the antibiotic
Common pattern
Parents often describe it as:
- Small pink spots or slightly raised bumps (think “measles-like” or “morbilliform”)
- Often starts on the trunk (chest, back, belly) and spreads to arms and legs
- Usually symmetrical on both sides of the body
- May itch a little, but many kids are not very itchy
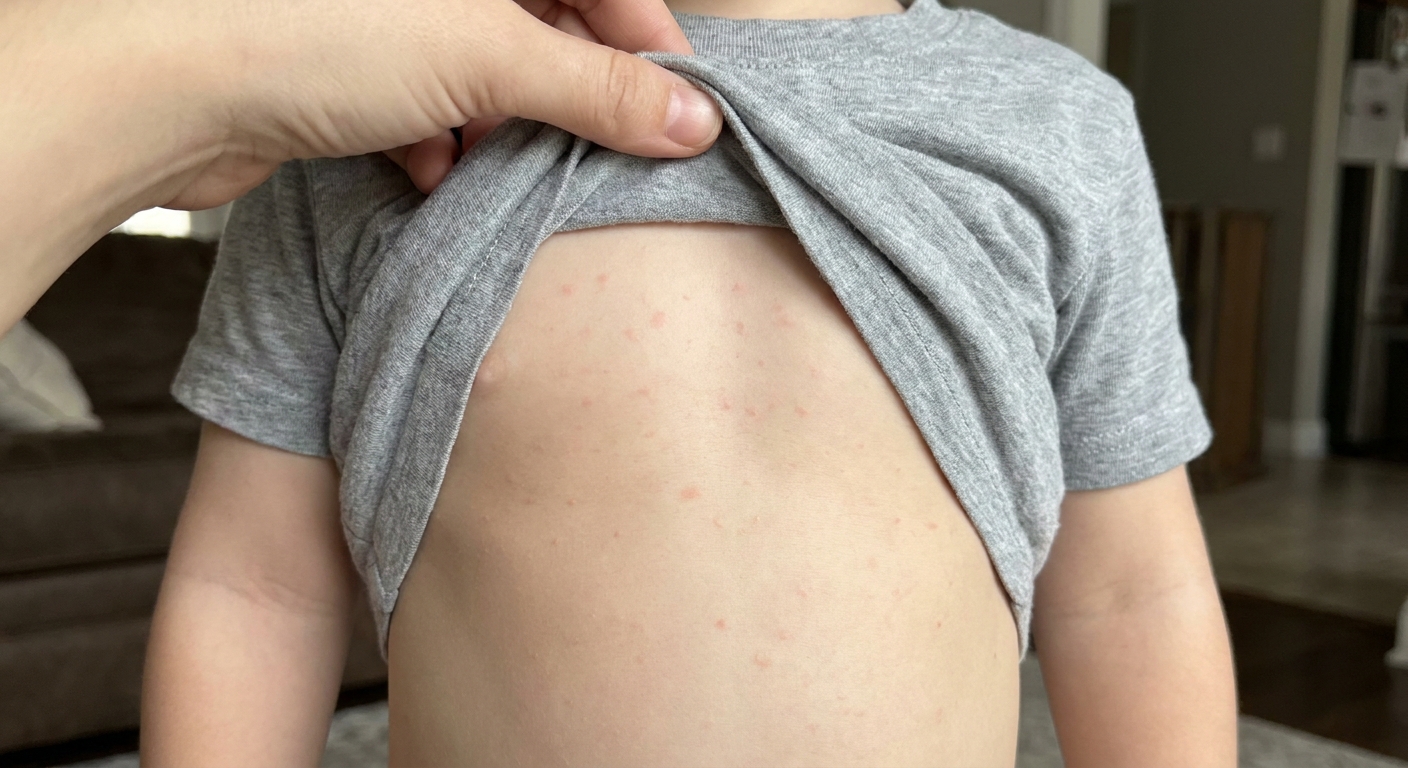
How your child usually acts
With a benign rash, many kids otherwise seem okay. They may still feel crummy from the infection, but they are generally:
- Breathing comfortably
- Not developing new facial or lip swelling
- Not suddenly covered in intensely itchy welts
Why it happens
Sometimes it is simply a medication-related skin eruption. Other times it is the combination of amoxicillin plus a viral illness. One well-known example is EBV (mono), which can trigger a rash during aminopenicillin antibiotics (amoxicillin and ampicillin).
Important nuance: infections can overlap, but so can tests. For example, some kids carry strep in their throat and can still have a viral illness. That means a positive strep test does not always prove strep is the cause of every symptom. So the rash does not automatically mean “wrong diagnosis,” and it also does not automatically mean “allergy.”
Concerning for allergy
Immediate allergy and anaphylaxis (emergency)
A true immediate allergy tends to happen quickly:
- Typically within minutes to 1 to 2 hours after a dose
- Often after the first few doses, but it can happen later too
Also worth knowing: hives that show up later in the course can still be allergic and should be discussed with your child’s clinician the same day.
What it looks like
These patterns are more concerning:
- Hives (urticaria): raised, very itchy welts that can move around the body, come and go, and change shape or location over hours
- Swelling (angioedema): puffy lips, eyelids, face, tongue
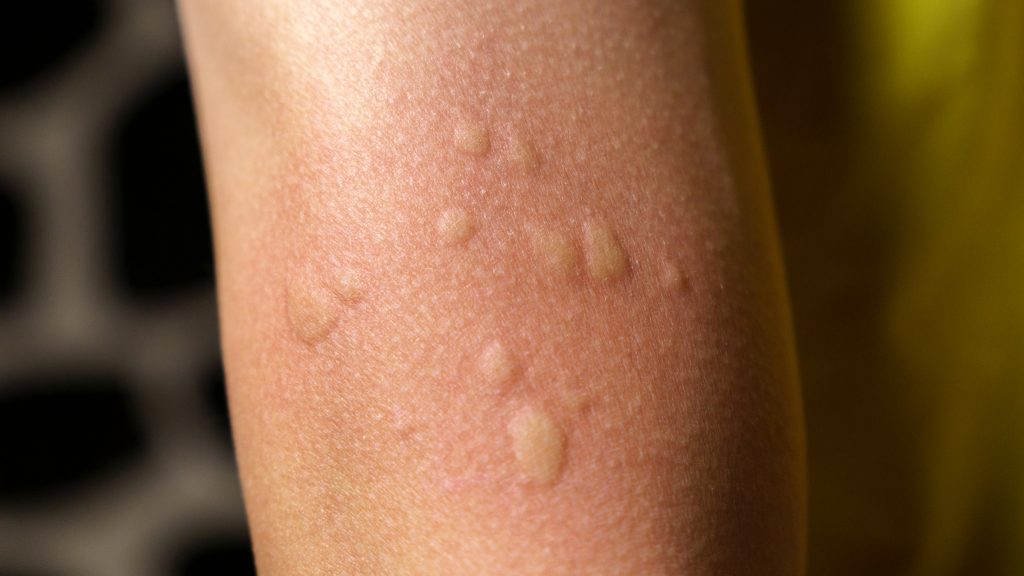
Symptoms that make it urgent
Call emergency services or go to the ER now if your child has any of the following after taking amoxicillin:
- Trouble breathing, wheezing, or throat tightness
- Hoarse voice, drooling, or trouble swallowing
- Swelling of the lips, tongue, or face
- Repeated vomiting or severe belly pain especially if it happens soon after a dose and with rash or hives
- Dizziness, fainting, extreme sleepiness, or looking pale and floppy
If your child has a known history of anaphylaxis and you have an epinephrine auto-injector, use it as directed and seek emergency care immediately.
Rare but serious rashes
Most rashes with amoxicillin are not emergencies, but a few types should be evaluated urgently because they can signal a more serious reaction or another illness.
Get same-day care if you see:
- Blistering or peeling skin
- Painful rash (more pain than itch)
- Rash involving the eyes, mouth, or genitals (sores, crusting, swelling)
- Purple or bruise-like spots that do not blanch when pressed
- High fever or your child looks very ill
- Widespread rash plus facial swelling or swollen lymph nodes
Three “do not wait” patterns
- Stevens-Johnson syndrome or toxic epidermal necrolysis (very rare): painful rash, blisters, skin peeling, and mouth or eye involvement.
- Serum sickness-like reaction: rash or hives plus fever and joint pain or swelling. Timing is often 1 to 3 weeks after exposure (and can be sooner if your child has had the medicine before).
- DRESS (drug reaction with eosinophilia and systemic symptoms): a delayed reaction that can include fever, widespread rash, facial swelling, swollen lymph nodes, and sometimes internal organ involvement. You cannot confirm this at home, but that combination is a reason to get urgent evaluation.

These are not meant to scare you. They are meant to help you feel confident about what actually requires urgent help.
Should you stop amoxicillin?
This is the part where I wish I could see your child and the rash, because the right answer depends on the pattern and symptoms.
If there are emergency allergy symptoms
Do not give another dose. Seek emergency care.
If it looks like hives or there is swelling
Assume possible allergy until proven otherwise:
- Hold the next dose and call your child’s clinician or prescriber the same day
- Ask what they want you to do about antihistamines and whether to switch antibiotics
- Do not re-challenge at home (do not “try one more dose to see”). If an oral challenge is appropriate, it should be clinician-guided
If it is a mild, spotty pink rash and your child is otherwise well
Call your child’s clinician or prescriber for guidance. Some clinicians will have you continue, especially if the antibiotic is important for the infection being treated and the rash truly fits the benign pattern. Others may stop it and choose an alternative. Either approach can be reasonable depending on your child’s history and the infection.
Practical tip: Take clear photos in good light and note the time of the last dose. Those two details help your child’s clinician a lot.
Quick comparison
| Clue | More like a harmless amoxicillin rash | More like an allergy |
|---|---|---|
| Timing | Day 3 to Day 10 (often later) | Typically within minutes to 1 to 2 hours after a dose (but later hives can still be allergic) |
| Appearance | Fine pink spots or small bumps, often on trunk | Hives: raised, very itchy welts that move around |
| Itch | None or mild | Often intense |
| Swelling | Usually none | Lips, face, eyelids, tongue can swell |
| Breathing | Normal | Wheeze, throat tightness, trouble breathing possible |
| What to do | Call clinician or prescriber for guidance, monitor closely | Hold dose and seek same-day care, ER if any breathing or swelling |
What to tell the clinician next time
One of the biggest long-term issues I saw in clinic was kids getting labeled “penicillin allergic” based on a vague rash years earlier. That label can follow them for life and can lead to using broader antibiotics that may be less effective, more expensive, or more likely to cause side effects.
Bring these details to every visit
- Which medication: amoxicillin, Augmentin (amoxicillin-clavulanate), or another antibiotic?
- Day of illness and day of antibiotic when the rash started
- Time from last dose to rash onset (30 minutes vs 5 days is a huge clue)
- Rash type: flat pink spots, small bumps, or raised welts that move?
- Other symptoms: itch, facial swelling, wheeze, vomiting, fever, joint pain, mouth sores
- What happened when you stopped or continued the medication
- Photos if you have them
Ask this specific question
If your child had a mild delayed rash without hives or breathing symptoms, ask: “Do you think this is a true penicillin allergy, and should we consider allergy testing or an oral challenge in the future?”
Many children who are labeled allergic are not truly allergic when evaluated later. Only your child’s clinician or an allergist can guide this safely, but it is absolutely worth discussing.
What about other antibiotics?
Parents often ask about cephalosporins (like cefdinir or cephalexin). Many kids with a non-severe delayed rash can still take certain cephalosporins, but the safest choice depends on your child’s reaction history and the infection being treated. Let your child’s clinician make that call.
Common parent questions
“My child is on amoxicillin for strep. Is this scarlet fever instead?”
It could be. Scarlet fever is a strep-related rash that typically feels like fine sandpaper and often comes with a sore throat and fever. It can appear around the time you start antibiotics because the illness is already in progress. Your clinician can help distinguish this from a medication rash, especially if the rash started before the first dose or within the first day of illness.
“If it is a benign rash, how long will it last?”
Often a few days, sometimes up to a week. It may fade even if the antibiotic is continued (depending on your clinician’s plan). Call if it is rapidly worsening, becoming very itchy, or your child develops new symptoms.
“Can I give Benadryl?”
For itch or hives, clinicians sometimes recommend an antihistamine, but dosing depends on age and weight and the specific product. In triage we always asked families to call for dosing guidance, especially for younger children. If there are breathing symptoms or swelling, antihistamines are not enough. That is emergency territory.
“Does this mean my child can never have penicillin again?”
Not necessarily. A delayed, non-hive rash does not always equal a lifelong allergy. The safest path is to document what happened and discuss next steps with your clinician or prescriber. In some cases, referral to an allergist for evaluation is the best way to get a clear answer.
When to call vs urgent care
Call within 24 hours if:
- New pink, spotty rash on day 3 to day 10 and your child is otherwise okay
- Mild itch with no hives
- No facial swelling, no breathing issues
Call same day (urgent) if:
- Rash looks like hives
- Rash is rapidly spreading
- Fever returns or your child seems significantly worse
- There is new joint pain or swelling
- Widespread rash plus facial swelling or swollen lymph nodes
Go to the ER now if:
- Any trouble breathing, wheezing, throat tightness
- Swelling of lips, tongue, or face
- Fainting, severe weakness, or repeated vomiting soon after a dose with rash or hives
- Blisters, peeling skin, or mouth or eye sores
Bottom line
If your child develops a rash while taking amoxicillin, you are not overreacting by pausing and checking. Most of the time, what parents are seeing is a benign pink rash that starts days into the course, especially during viral season.
But if the rash is hives, comes on quickly after a dose, or is paired with swelling or breathing symptoms, treat it as a possible allergy and get urgent care.
And whatever happens, jot down the timing and snap a photo. Future you, future prescribers, and your child’s medical record will thank you.