Athlete’s Foot in Toddlers: Pool Rash vs Eczema vs Dry Skin
Sarah Mitchell
Sarah Mitchell is a Registered Pediatric Nurse and a mother of three who has spent over a decade helping families navigate the beautiful, chaotic early years of childhood. She combines evidence-based medical knowledge with real-world parenting experience to offer practical, compassionate advice. At Awesome Parent, Sarah's mission is to help exhausted parents find solutions, trust their instincts, and finally get some sleep.
If your toddler comes home from swim lessons scratching their toes like they just discovered a new hobby, you're not alone. Pools, splash pads, and locker rooms are perfect places for feet to get wet, warm, and a little too cozy inside shoes. That combo can lead to athlete’s foot (tinea pedis), but it can also look a lot like eczema or simple dry, irritated skin.
One important note up front: the bigger risk is usually wet communal surfaces (pool decks, locker room floors, shared showers), not the chlorinated pool water itself. The water is treated, but the areas around it are where fungi like to spread from bare foot to bare foot.
Let’s sort out what you're seeing, what you can safely try at home, and when it's time to loop in your child’s clinician.

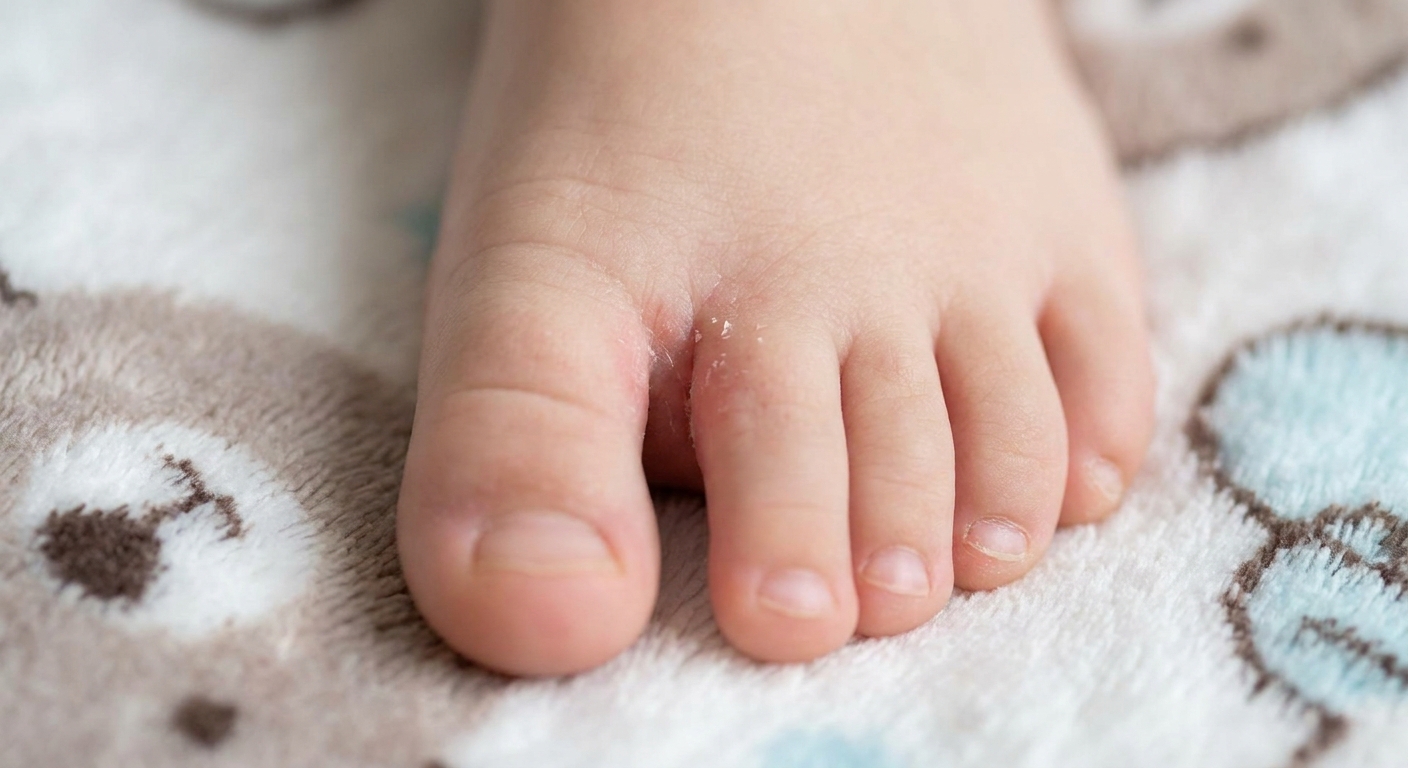
What athlete’s foot looks like
Athlete’s foot is a fungal skin infection. In adults it's common. In toddlers it's less common than in teens, but it absolutely happens, especially with frequent pool use, sweaty feet, and shoes that trap moisture.
Typical clues
- Itching or burning between the toes (often the worst symptom)
- White, soggy, “macerated” skin between toes
- Peeling, cracking, or scaling, especially in the toe webs
- Redness that may spread onto the bottom or sides of the foot
- Sometimes tiny blisters along the arch or sides
- A noticeable odor can happen with damp, irritated skin, but it’s nonspecific and can also be from sweat or bacteria
Athlete’s foot often starts in the spaces between toes because that's where water and sweat like to hang out.
Pool rash vs eczema vs dry skin
Here's the practical parent question: is this fungus, or is my kid’s skin just mad at chlorine, friction, or a new pair of shoes?
Pool or chlorine irritation
- Often shows up after swimming and improves when you take a few days off
- Looks like dry, tight, slightly red skin, sometimes on tops of feet too
- Usually stings more than it itches
- Less likely to cause soggy white skin between toes
Eczema
- Often a history of eczema elsewhere (behind knees, elbows, cheeks)
- Very itchy, can flare with swimming, sweat, and stress
- May look like dry patches and can crack, but the classic toe-web “mushiness” is less typical
- May improve with thick moisturizer and, if prescribed, a topical steroid
Dry skin or friction
- More likely with sandals rubbing, new shoes, or lots of barefoot running
- Peeling tends to be even and superficial rather than concentrated between toes
- Usually improves quickly with moisturizer and better drying habits
More likely athlete’s foot
- Symptoms centered between toes
- White, soggy skin or cracks in the toe webs
- Persistent itch for more than a few days, especially if moisturizer alone doesn't help
- Other family members with athlete’s foot, or shared showers or locker rooms
Why swim places trigger it
Fungus loves three things: moisture, warmth, and skin contact.
Chlorinated pool water is treated, but fungi can still hang out on wet, high-traffic surfaces like decks and locker room floors. After swimming, wet feet often go straight into socks and sneakers. The toe webs stay damp, and that’s a very common setup for tinea pedis.
What you can do at home
Step 1: Dry well
- After baths or swimming, dry between every toe.
- Pat gently rather than rubbing if the skin is tender.
- Change socks if they get damp.
- Choose breathable shoes when possible, and rotate pairs so they can dry fully.
- At home, letting feet air out helps.
Step 2: Consider an OTC antifungal
Many over-the-counter antifungal creams and sprays are marketed for athlete’s foot. Common active ingredients include terbinafine, clotrimazole, and miconazole.
Here's the key for toddlers: product labeling varies by age, and it can vary by brand and region too. For example, some terbinafine products are labeled only for older kids or adults, while some azole creams may have different minimum ages on the box.
For a toddler, the safest plan is:
- Read the package age instructions first.
- If your child is under the labeled age, or you're unsure, call your pediatrician or ask your pharmacist which product is appropriate.
- Use only on the skin where directed, and keep it out of reach. Toddlers touch everything, then touch their mouths.
In general, fungal infections can take 2 to 4 weeks of consistent treatment to fully clear, even if they look better sooner. Stopping too early is a common reason it comes right back.
Step 3: Moisturize (carefully)
If the skin is dry and cracked but not soggy, a bland, fragrance-free moisturizer can help repair the skin barrier. Apply after bathing and at bedtime.
If the skin between toes is macerated (white and wet-looking), go easy on heavy ointments in that area. Sealing in moisture can make fungus happier. In those toe webs, focus on drying and antifungal treatment as advised.
What to skip
- Topical steroid cream without guidance if you suspect fungus. Steroids can calm redness but may allow fungal infections to worsen or spread.
- Scrubbing or picking at peeling skin. It can cause painful cracks and invite bacterial infection.
- Strongly scented lotions that can sting and irritate.
Signs of bacterial infection
Sometimes irritated, cracked skin becomes a doorway for bacteria. This can happen with eczema, with athlete’s foot, or with plain old friction. Call your child’s clinician promptly if you notice:
- Increasing pain (not just itch)
- Spreading redness or warmth on the foot
- Swelling
- Yellow crust, pus, or oozing that seems infected
- Fever or your child acting unusually ill
- Red streaking up the foot or ankle (urgent)
If bacteria are involved, your child may need a prescription topical or oral antibiotic in addition to addressing the underlying skin issue.
OTC vs prescription
OK to start at home
- Mild itch and peeling focused between toes
- No significant redness spreading beyond the toes
- Your toddler seems well otherwise
Call within 24 to 48 hours if
- Your child is under the age listed on the OTC product you want to use
- It's not improving after 7 to 10 days of appropriate treatment and moisture control
- The rash is spreading to the sole, sides of feet, or up the ankle
- Your child has significant eczema and you're not sure which problem you're treating
- Your child is immunocompromised or has diabetes (rare in toddlers, but important)
Prescription treatment may be needed
- The infection is extensive, recurrent, or not responding to OTC treatment
- There are painful fissures or severe inflammation
- A clinician suspects a different diagnosis (like psoriasis) or wants to confirm with a skin scraping test
- There’s nail involvement (thickened, crumbly, yellow or brown toenails) or frequent repeat infections
Prevention after swim lessons
- Rinse and dry feet after swimming. Get into the toe spaces.
- Use clean, dry socks and change them if they get damp.
- Rotate shoes and let them dry fully between wears.
- In locker rooms, use water shoes when appropriate for your facility.
- Don't share towels, socks, or shoes between siblings.
To reduce reinfection at home, wash socks and towels regularly (hot water if the fabric allows) and make sure shoes fully dry before they’re worn again. Also, if an adult in the home has athlete’s foot, treat it. Toddlers are excellent at stepping exactly where you just stepped.
Quick reassurance
Most toddler foot rashes after the pool are treatable, and many aren't emergencies. The key is noticing the pattern: toe-web itch and soggy peeling points toward fungus, while overall dryness after chlorine points toward irritation or eczema. If you're not sure, you don't have to guess your way through it. A quick call to your pediatrician can save you a week of trial and error and a lot of late-night toe scratching.
If you want the simplest first step tonight: wash, dry carefully between the toes, put on clean socks, and take a clear photo in good light. Photos are surprisingly helpful if you need to message your clinic tomorrow.
Common questions
Can toddlers really get athlete’s foot?
Yes, though it's less common than in older kids and adults. It's more likely with frequent swimming, sweaty feet in closed shoes, or exposure to shared wet surfaces like locker room floors and showers.
Is peeling skin always fungus?
No. Chlorine irritation, eczema flares, friction, and even just wet feet in sandals all summer can cause peeling. The location and texture matter. Athlete’s foot often targets the skin between toes and can look white and soggy.
Should I use hydrocortisone on it?
If you strongly suspect fungus, avoid using steroid cream on your own because it can make fungal rashes harder to treat. If you suspect eczema and your child has a known eczema plan, follow that plan, or check with your clinician if you're unsure.
How long until it gets better?
With correct treatment and consistent moisture control, mild cases often start to look better within about a week, but complete clearing can take a few weeks. If it's not improving, it's time to check in with your pediatrician.