Auditory Processing Disorder in Kids
Sarah Mitchell
Sarah Mitchell is a Registered Pediatric Nurse and a mother of three who has spent over a decade helping families navigate the beautiful, chaotic early years of childhood. She combines evidence-based medical knowledge with real-world parenting experience to offer practical, compassionate advice. At Awesome Parent, Sarah's mission is to help exhausted parents find solutions, trust their instincts, and finally get some sleep.
If your child can hear you open a snack bag from two rooms away but somehow “doesn’t hear” you when you ask them to put on shoes, you are not alone. In clinic and at my own kitchen table, I have seen how confusing this can feel. Parents get told, “Their hearing is fine,” yet teachers report missed directions, messy spelling, and total shutdown in noisy classrooms.
One possible piece of that puzzle is Auditory Processing Disorder (APD), sometimes called (C)APD or Central Auditory Processing Disorder. A quick but important note: APD terminology, testing methods, and diagnostic criteria vary across clinics and professional guidelines, and there is ongoing debate about boundaries between APD and language or attention-based challenges. That does not mean your child’s struggles are not real. It means the evaluation needs to be thoughtful and individualized.
This article is here to guide you, not diagnose your child. I will walk you through what APD can look like, how it is different from hearing loss and ADHD, what an evaluation usually involves, what may happen after a diagnosis, and practical supports you can use right now.

What is Auditory Processing Disorder?
Auditory Processing Disorder means a child has difficulty processing and interpreting sounds, particularly speech. Their ears may detect sound at normal volumes, but the brain has trouble sorting, organizing, or filling in what those sounds mean.
Think of it like this: the sound gets into the system, but the “sound-to-meaning” step is glitchy, especially when things get complicated like fast speech, background noise, multiple speakers, or long directions.
Common ways APD can show up
- “What?” and “Huh?” a lot, especially when you are not facing them.
- Trouble following multi-step directions (they catch step 1 and lose the rest).
- Meltdowns or shutdowns in noisy places like the cafeteria or birthday parties.
- Seems to listen better one-on-one than in groups.
- Needs extra time to answer questions, like there is a delay.
- Mixes up similar-sounding words (“fifteen” vs “fifty,” “cap” vs “cat”).
- Reading and spelling struggles, especially with phonics or sounding out words.
- Appears inattentive in class but can hyper-focus on preferred activities.
APD is often noticed in school-age kids because classroom listening is a high-level skill. It requires filtering noise, tracking the teacher’s voice, and remembering what was said, all while writing, reading, and keeping your body calm in a chair. That is a lot for a developing brain.
APD vs hearing loss vs ADHD
From the outside, APD can look like “not listening,” defiance, daydreaming, a language delay, or ADHD. The good news is that sorting this out is possible, and it often takes a team approach.
APD vs hearing loss
Hearing loss is about reduced ability to detect sound. This might be permanent or temporary (like fluid behind the eardrum after frequent ear infections).
APD is about difficulty processing sound even when the child can detect it normally.
Important note from a pediatric nurse standpoint: always start by ruling out hearing issues. Even mild, fluctuating hearing loss from chronic ear fluid can mimic APD and seriously impact school performance.
APD vs ADHD or inattention
ADHD is primarily about attention regulation, impulse control, and executive function. Kids with ADHD may miss information because their attention drifts or they act before they fully process instructions.
APD is primarily about auditory input getting “muddy,” especially in noise. A child may be trying hard, but the message does not come through clearly.
And yes, a child can have both. APD may overlap with ADHD, language disorders, learning disabilities, and sensory processing differences. At the same time, many APD-like symptoms can be fully explained by attention, language, or learning differences. That is why a thorough evaluation matters.
A quick real-life clue
- If your child struggles most when information is spoken, especially in noise, but does better with written instructions, pictures, or demonstrations, APD may be more likely.
- If your child struggles across the board, including with visual tasks and quiet one-on-one situations, or is impulsive and constantly on the move, attention or executive-function challenges may be a bigger driver.
- If the biggest struggle is understanding vocabulary, grammar, or expressing ideas clearly (even when listening conditions are good), a language disorder may be a key piece.

What teachers often notice
Teachers are often the first to raise the flag because classrooms are basically listening obstacle courses. Common school comments include:
- “They don’t follow directions unless I repeat them.”
- “They watch other kids to know what to do.”
- “They seem lost during whole-group instruction.”
- “Their work is incomplete even though they understand the topic.”
- “They struggle with phonics, spelling, or taking notes.”
- “They do better in small groups.”
- “Noise really throws them off.”
If you are hearing these messages, you are not failing. Your child is not lazy. This is data, and it is useful data.
What can contribute to APD?
APD does not have one single cause, and research is still evolving. Some factors that may be associated with auditory processing challenges include:
- Developmental differences in how the auditory system matures.
- History of frequent ear infections or long periods of middle ear fluid, which may affect auditory input during key language years (the evidence is mixed, and this is not a simple cause-and-effect).
- Prematurity or neurologic risk factors in some children.
- Coexisting language or learning differences.
Most parents want a simple reason. I get it. But in pediatrics, we often do not get the satisfaction of a single tidy cause, and that is okay. What matters most is identifying supports that help your child function and feel confident.
How APD is evaluated
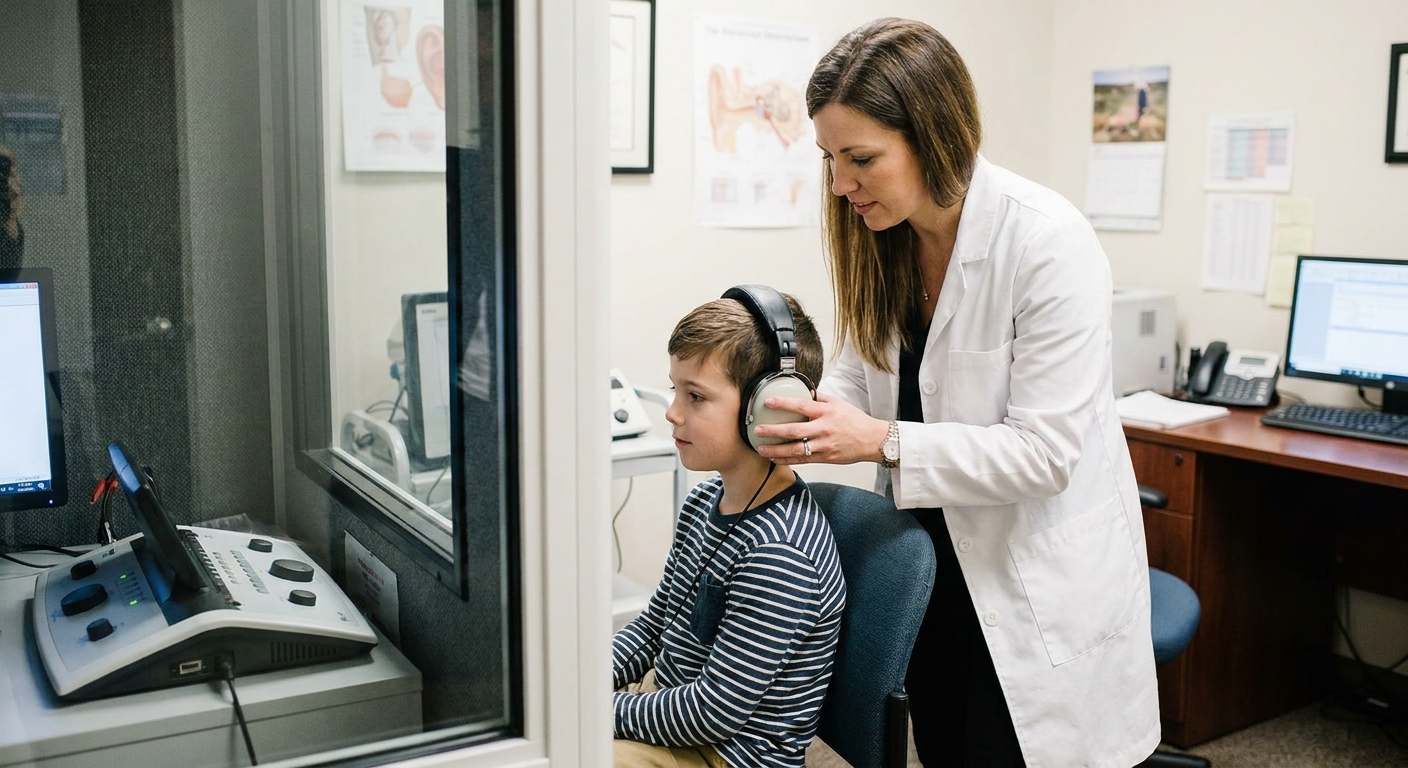
An APD evaluation is typically done by an audiologist with specialized training in auditory processing testing. Many clinics often test children around age 7 or older, because auditory skills, language, and attention need to be mature enough for reliable results. That said, minimum age and test batteries differ by clinic, and some children can be assessed earlier depending on the setting and the child.
Step 1: A full hearing check
Before APD testing, audiologists usually confirm:
- Hearing thresholds (can your child detect sounds at typical volumes?)
- Middle ear status (any fluid or pressure issues?)
- Speech recognition in quiet
If there is hearing loss or middle ear fluid, that may need to be addressed first. A “normal hearing screen” at school is helpful, but it is not the same as a full audiology evaluation.
Step 2: Auditory processing tests
Testing varies by clinic, but it may include tasks like:
- Understanding speech with background noise
- Listening to competing words or sentences in each ear
- Recognizing subtle differences between sounds
- Remembering and repeating auditory information
The goal is to identify specific processing weaknesses so supports can be targeted.
Step 3: Looking at the whole child
Because APD can overlap with other needs, your child may also benefit from:
- Speech-language evaluation (receptive/expressive language, phonological skills)
- Psychoeducational testing through the school or privately (learning profile, working memory, attention)
- Medical review with your pediatrician if sleep, anxiety, or frequent ear infections are part of the story
A quick note about online screeners
It is tempting to rely on online APD checklists and quizzes when you are trying to make sense of things at 11 p.m. (been there). Those tools can help you organize concerns, but they cannot diagnose APD. Many conditions can look similar on a checklist. Formal testing and a full picture of your child is what makes the results meaningful.
What helps after diagnosis
If your child is diagnosed with APD, recommendations are usually practical and school-focused. They often include:
- Environmental supports (better seating, reducing competing noise when possible, clear routines).
- Compensatory strategies (repeat-back, asking for clarification, note supports).
- Targeted skill-building through a clinician or structured program (sometimes called auditory training). Evidence and fit vary, so ask your audiologist or speech-language pathologist what they recommend and how progress will be measured.
- Assistive listening options when appropriate (more on that below).
Prognosis is often encouraging. Many children make significant gains with the right supports, skill-building, and simple maturation. The goal is not perfection. The goal is better access to learning and less daily stress.
What you can do at home
You do not need to wait for a formal label to make life easier. These supports help many kids with listening and processing challenges, regardless of the final diagnosis.
Make directions brain-friendly
- Get close and make eye contact before speaking. Say their name, pause, then give the instruction.
- One step at a time for tricky moments (mornings, bedtime).
- Use a calm, steady pace. Fast speech is harder to process.
- Ask for a repeat-back: “Tell me what you are going to do first.”
Reduce background noise
- Turn off the TV or music when giving instructions.
- Move to a quieter room for homework or reading.
- Consider soft furnishings (rugs, curtains) if echo seems to make things worse.
Support working memory
- Use simple checklists for routines.
- Post visual schedules where they happen (by the door, in the bathroom).
- Pair spoken instructions with a quick gesture or visual cue.
Watch for listening fatigue
Processing speech all day can be exhausting. If your child melts down after school, it may not be “attitude.” It may be overload. A snack, movement, quiet time, and predictable routines can make evenings smoother.
Classroom supports
If APD is suspected or confirmed, classroom supports are often the biggest game-changer. You can request a meeting with your teacher, school counselor, or special education team to discuss accommodations. These may be included in a 504 Plan or an IEP, depending on your child’s needs and school evaluation.
Seating and environment
- Preferential seating near the teacher and away from doors, fans, pencil sharpeners, and chatty neighbors
- Quiet work area option for independent tasks and tests
- Noise reduction strategies when possible (classroom routines that limit side conversations during instruction)
How instructions are given
- Written and verbal directions (both, whenever possible)
- Check for understanding privately, not by calling them out
- Chunking multi-step tasks into smaller parts
- Extra processing time before expecting an answer
Materials and note support
- Access to teacher notes or outlines
- Visual supports, examples, and models of finished work
- Reduced copying from the board
Assistive listening options
Some children benefit from an assistive listening system (often called an FM or remote microphone system), where the teacher’s voice is transmitted more directly to the child, reducing the impact of classroom noise. These systems are typically trialed and fit with guidance from an audiologist and implemented through school accommodations, so everyone understands how and when to use them. This is not appropriate for every child, but it can be very helpful for speech-in-noise difficulty.
Two simple scripts you can use
- To the teacher: “When you can, could you give directions verbally and in writing? Even a quick checklist helps.”
- For your child to practice: “I heard the first part. Can you say the last step again?”

Questions to ask
When you are tired and worried, it is easy to walk into appointments and forget what you meant to say. Here are questions that keep the conversation productive:
For your pediatrician
- Could ear infections or fluid be affecting hearing consistency?
- Should we get a full audiology evaluation (not just a screening)?
- Are sleep problems, anxiety, or attention issues contributing?
For the audiologist
- Is my child’s basic hearing and middle ear function normal?
- Is APD testing appropriate for their age and development?
- Which specific auditory skills are weak (speech in noise, decoding, memory)?
- What accommodations do you recommend for school?
- Should we consider a remote microphone trial, and what would success look like?
For the school
- Can we try accommodations now while we pursue evaluation?
- Can we document which situations are hardest (whole-group, transitions, noisy times)?
- What supports are available through a 504 Plan or IEP?
When to seek help sooner
Most listening and learning concerns are not emergencies, but some situations deserve a faster call to your pediatrician or audiologist:
- New or worsening hearing concerns, especially after illness
- Speech regression or sudden significant academic decline
- Frequent ear pain, drainage, or suspected chronic fluid
- Big emotional distress at school, school refusal, or anxiety related to not understanding
A note from one tired parent to another
If your child is “hearing fine” but struggling to listen, please know this is a real and common experience. It is not a character flaw. It is not a parenting failure. And it is not something you have to solve alone.
Start with a full hearing evaluation, keep a short list of specific examples from home and school, and ask for practical supports that reduce the daily friction right now. When kids feel understood and supported, they do not just perform better. They feel better.
If you want a simple first step: ask the teacher which part of the day is hardest to understand, then choose one accommodation to try for two weeks and reassess. Small changes can have surprisingly big results.