Baby Ear Infection Signs
Sarah Mitchell
Sarah Mitchell is a Registered Pediatric Nurse and a mother of three who has spent over a decade helping families navigate the beautiful, chaotic early years of childhood. She combines evidence-based medical knowledge with real-world parenting experience to offer practical, compassionate advice. At Awesome Parent, Sarah's mission is to help exhausted parents find solutions, trust their instincts, and finally get some sleep.
If you are reading this at 3 AM with a fussy baby on your shoulder, I see you. Ear infections are one of the most common reasons families end up in my old triage line, and they are stressful because the signs can look like everything else: teething, a cold, an off day, a growth spurt, you name it.
The good news is that most ear infections are treatable, and some improve without antibiotics, especially in older toddlers with mild symptoms and reliable follow-up. The key is knowing what to watch for, when to call, and when to head in right away.

What is an ear infection?
Most parents mean a middle ear infection (acute otitis media). That is when fluid gets trapped behind the eardrum and bacteria (and sometimes viruses) can multiply there, often during or after a cold.
Two other common ear problems can look similar:
- Fluid in the middle ear (otitis media with effusion): fluid remains after a cold or infection. It can affect hearing but usually is not painful and often does not cause fever.
- Outer ear infection (swimmer’s ear): infection of the ear canal. The outer ear is often tender, especially when you touch or move the ear.
Baby and toddler signs
Some kids clearly tell you, “My ear hurts.” Babies and young toddlers, understandably, do not. Here are the signs that most often raise my suspicion. Keep in mind, ear pain can also come from teething, swimmer’s ear, a sore throat, or pressure from congestion. An exam is what confirms a true middle ear infection.
Common signs
- Ear tugging or rubbing (especially along with other symptoms). Note: ear pulling alone can also be teething or self-soothing.
- Fussiness or crying that seems different, especially worse when lying flat.
- Trouble sleeping or waking more often.
- Fever (not always present, and can range from mild to high).
- Recent cold symptoms like runny nose or cough in the last few days.
- Less interest in feeding (swallowing can change ear pressure and may be uncomfortable when the middle ear is inflamed).
Other clues
- Balance seems off or more clumsy than usual (in some children).
- New or worsening irritability in the car seat or stroller (positioning and pressure changes can bother some kids).
- Ear drainage that looks like fluid or pus. This can happen if the eardrum perforates (a ruptured eardrum), and it often relieves pain, but it still needs medical guidance.
- Muffled hearing, not responding to quiet sounds, or turning the TV volume up (more common with persistent fluid).
What ear tugging does not always mean: A baby who occasionally plays with their ears but is otherwise happy, afebrile, and sleeping normally is often just exploring or teething.

Why little kids get them
Ear infections are common in babies and toddlers because their Eustachian tubes (the tiny drainage tubes connecting the middle ear to the back of the throat) are shorter and more horizontal than in adults. They clog more easily.
Common risk factors
- Colds and viral infections (the biggest trigger)
- Daycare and frequent exposure to other kids’ germs
- Secondhand smoke exposure
- Pacifier use (especially beyond 6 months, in some kids)
- Seasonal peaks (fall and winter)
- Family history of frequent ear infections
- Bottle feeding while lying flat (may increase risk; milk can pool in the back of the throat and irritate the Eustachian tube)
When to call
If you are unsure, it is always okay to call. This is exactly what pediatric offices are for. Here are practical guidelines I give parents.
Call within 24 hours if:
- Your baby is under 6 months and you suspect an ear infection
- Your child has ear pain that lasts more than a few hours, or is interfering with sleep
- Fever is present and your child seems uncomfortable (many practices consider 102.2°F/39°C or higher a “high fever” in older babies and toddlers, but follow your pediatrician’s guidance)
- You notice ear drainage
- Your child’s ear symptoms are not improving after 48 to 72 hours of good pain control and watchful waiting, or symptoms are worsening at any point
- Your child has had recurrent ear infections or has ear tubes
- You are worried about hearing or speech changes
Same-day care is a good idea if:
- Your child has moderate to severe ear pain
- Your child is very fussy and hard to console
- There is high fever (often 102.2°F/39°C or higher) along with ear symptoms
- Your child looks ill and you cannot tell why
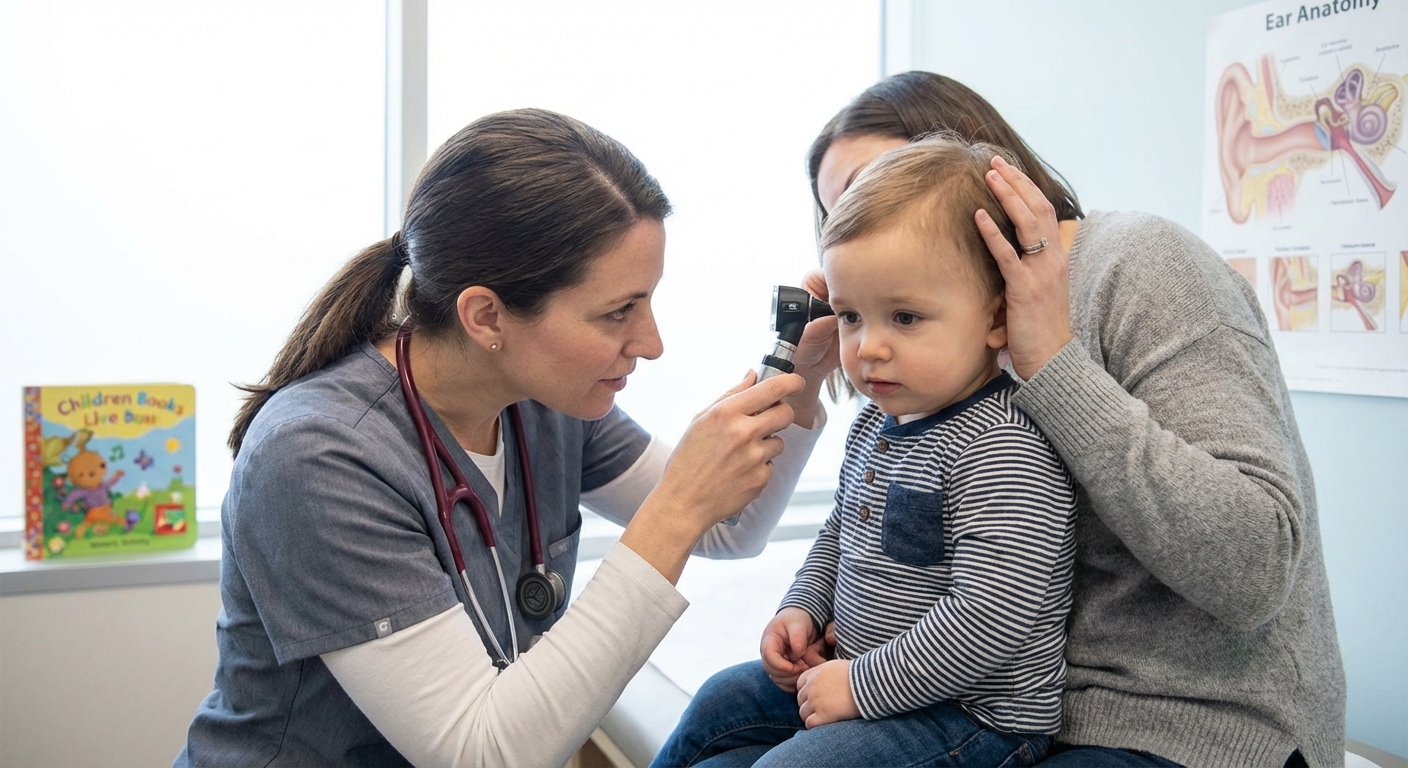
To diagnose a middle ear infection, clinicians need to look at the eardrum with an otoscope. The key findings are middle-ear fluid and a bulging eardrum. Redness can happen with crying or fever, so redness alone is not enough to diagnose an ear infection. (This is why “it looks like an ear infection” over a video visit can be tricky in younger kids.)
When it’s urgent
Most ear infections are not emergencies. But there are a few situations where I want you to seek urgent care or emergency evaluation.
Go now if your child has:
- Difficulty breathing, lips turning blue, or severe lethargy
- Stiff neck, severe headache, confusion, or new sensitivity to light
- Swelling, redness, or tenderness behind the ear, or the ear is pushed forward (this can be a sign of mastoiditis)
- New weakness of the face (drooping on one side)
- Seizure
- Signs of dehydration (very dry mouth, no tears, significantly fewer wet diapers)
- An infant under 3 months with a rectal temperature of 100.4°F (38°C) or higher
If you are on the fence, trust your gut and get eyes on your child. Parents are usually right when they say, “Something is off.”
Treatment options
Treatment depends on age, severity, whether it is one ear or both, and whether the infection looks bacterial or is likely to resolve on its own. Your clinician’s job is to balance helping your child feel better with avoiding antibiotics when they are unlikely to help.
Pain relief first
Even when antibiotics are needed, pain control is what helps a child settle, sleep, and drink, especially in the first 24 hours.
- Acetaminophen or ibuprofen can help with pain and fever. Use the dose recommended by your child’s clinician, based on weight, and do not exceed label dosing.
- Warm compress on the outside of the ear can be soothing.
- Extra fluids and comfort. Being clingy is normal.
Safety notes: Do not give ibuprofen to babies under 6 months unless specifically instructed. Never give aspirin to children. Avoid multi-symptom cold medicines in young children unless your clinician specifically recommends them.
Do they need antibiotics?
No. Many ear infections start with a virus or improve without antibiotics, especially in older toddlers with mild symptoms and reliable follow-up. Some pediatricians use “watchful waiting,” meaning you focus on pain control and recheck if symptoms are not improving within 48 to 72 hours, or if they worsen sooner.
When antibiotics are more likely
- Younger age, especially under 2 years
- Severe symptoms (significant ear pain, pain lasting 48 hours or more, or fever often 102.2°F/39°C or higher)
- Both ears infected in children under 2
- Ear drainage suggesting a perforation (ruptured eardrum)
- Immunocompromised child or certain medical conditions
If antibiotics are prescribed, it is usually because the exam strongly suggests bacterial infection or your child falls into a higher-risk group for complications.
What about ear drops?
For typical middle ear infections, antibiotic ear drops usually do not reach the middle ear unless there is a tube or a perforation. Drops may be used for:
- Swimmer’s ear
- Kids with ear tubes who develop drainage
If ear infections keep happening
If infections are frequent or fluid lingers and affects hearing, your pediatrician may refer you to an ENT to discuss ear tubes. Tubes can reduce the number of infections and make treatment easier if infections happen again.
If your child is on antibiotics
Call your clinician if your child is not improving within 48 to 72 hours, is getting worse, develops new swelling or redness behind the ear, or if you have trouble getting fluids in.
What to do tonight
If it is after hours and your child is miserable, focus on comfort and hydration while you decide whether to seek urgent care.
- Treat pain first: Use appropriate fever and pain medication per your clinician’s guidance.
- Keep them slightly upright for cuddles or feeding if lying flat worsens pain. (For sleep, always follow safe sleep guidelines for babies.)
- Offer frequent fluids. Smaller, more frequent feeds can be easier.
- Use saline and gentle suction for a stuffy nose. Less congestion can help ear pressure.
- Do not put oils or herbal drops in the ear unless instructed by a clinician. If there is a perforation (ruptured eardrum), some substances can irritate or harm the ear.
If your child is stable but uncomfortable, it is reasonable to call the pediatrician in the morning for an ear check. If your child is inconsolable, very lethargic, or has any urgent signs, get care now.
Prevention tips
You cannot prevent every ear infection. Kids are going to kid. But you can reduce risk.
- Stay up to date on vaccines, including flu and pneumococcal vaccines, which reduce certain infections that can lead to ear infections.
- Breastfeeding if possible offers some immune protection. Any amount helps, and formula-fed babies can absolutely thrive too.
- Avoid secondhand smoke. This is one of the biggest modifiable risk factors.
- Hand hygiene and minimizing sick exposure when you can, especially during peak cold season.
- Consider pacifier weaning after 6 months if your child is prone to ear infections.
- Feed babies upright when possible, and avoid bottle propping.

Ear infection FAQ
Can teething cause an ear infection?
Teething does not cause ear infections, but it can cause ear tugging and crankiness, which can look similar. If there is fever, significant sleep disruption, drainage, or cold symptoms, an ear check is worth considering.
Do symptoms come and go?
Yes. Pain can be worse when lying down and better when upright. Some kids have a rough night and a decent morning. If symptoms keep returning or are worsening, get your child examined.
If the ear is draining, is that good or bad?
Drainage can mean pressure released, and sometimes pain improves quickly. But drainage can also suggest a perforation (ruptured eardrum) or tubes, and your child should be evaluated for the right treatment.
Will flying make it worse?
Pressure changes can increase discomfort. If you have upcoming travel and your child has ear pain or a recent ear infection, ask your pediatrician for individualized advice.
Quick checklist
If you want a simple way to decide what to do next, here is my quick mental flowchart from years on the phone lines:
- Any urgent signs (trouble breathing, severe lethargy, swelling behind ear, stiff neck, seizure, under 3 months with 100.4°F+)? Go now.
- Under 6 months with suspected ear infection symptoms? Call today.
- Moderate to severe pain, fever often 102.2°F/39°C+, drainage, or very ill appearance? Same-day care.
- Mild symptoms, drinking okay, no red flags? Treat pain, monitor closely, and call for an exam within 24 hours or sooner if worsening.
And finally, the reminder I wish every anxious parent heard: you are not overreacting by wanting your child comfortable. Ear pain is real. You deserve support, clear answers, and a plan that helps everyone sleep.