Breast Abscess While Breastfeeding
Sarah Mitchell
Sarah Mitchell is a Registered Pediatric Nurse and a mother of three who has spent over a decade helping families navigate the beautiful, chaotic early years of childhood. She combines evidence-based medical knowledge with real-world parenting experience to offer practical, compassionate advice. At Awesome Parent, Sarah's mission is to help exhausted parents find solutions, trust their instincts, and finally get some sleep.
When you are breastfeeding, it is normal to wonder, Is this just mastitis… or is something more going on? Most breast infections improve with the right plan. But sometimes a pocket of infection forms that antibiotics alone often cannot fix. That is called a breast abscess, and it deserves quick, calm, confident care.
I am going to walk you through what makes an abscess different from mastitis, the warning signs that should move you from home care to a same-day call, what ultrasound and drainage are like in real life, and how to protect your milk supply during treatment.

Mastitis vs. abscess
Mastitis is inflammation in the breast that can be infectious or noninfectious. It often comes with soreness, a firm area, redness, and flu-like symptoms. With early support, effective milk removal, and antibiotics when indicated, it often starts to improve within 24 to 48 hours.
By “effective milk removal,” I mean frequent, comfortable feeding or pumping that keeps milk moving without causing more nipple damage. For most people, that looks like feeding on your usual schedule (or close to it), checking latch and positioning, and using a pump that fits well if you are pumping.
A breast abscess is when infection becomes walled off into a localized pocket of pus. That pocket usually cannot drain through normal milk flow, so symptoms tend to persist or worsen even when you are doing “all the right things.” An abscess often requires drainage in addition to antibiotics, although small abscesses may sometimes improve with close follow-up and medication alone.
Think of it like this: mastitis is a spreading fire in the tissue. An abscess is when the fire has created a sealed hot spot. You may need a procedure to release it.
Signs it may be more
These symptoms do not prove you have an abscess, but they are strong reasons to call your OB, midwife, primary care provider, or lactation medicine team the same day:
- A distinct lump that feels fluctuant or “squishy” in the center, like there is fluid under the skin
- A localized area that keeps getting bigger or more painful over time
- Symptoms not improving after 24 to 48 hours of an appropriate mastitis plan, or symptoms that improve then quickly return
- Persistent fever or feeling systemically unwell despite antibiotics
- Redness that becomes more sharply defined over one spot, sometimes with shiny or tight-appearing skin
- Nipple drainage that looks like pus (thick, yellow or green), not just milk
- New swelling near the areola or worsening pain with latch or pumping
One extra clue I see in clinic: parents describe a very specific “point” of pain that makes them flinch, rather than a broader sore quadrant. That pinpoint tenderness can happen with mastitis too, but when it persists, it raises my suspicion.
When to go in now
Go in urgently or to the ER if you have any of the following:
- High fever, shaking chills, or you feel faint
- Rapidly spreading redness or significant swelling
- Severe pain that is escalating quickly
- New shortness of breath, confusion, or signs of dehydration
- You are immunocompromised or have poorly controlled diabetes and you are getting sicker
Trust that instinct that says, “This is not right.” You are not being dramatic. You are being safe.
How it is diagnosed
Clinicians can suspect an abscess based on exam, but the most common test to confirm it is a breast ultrasound.
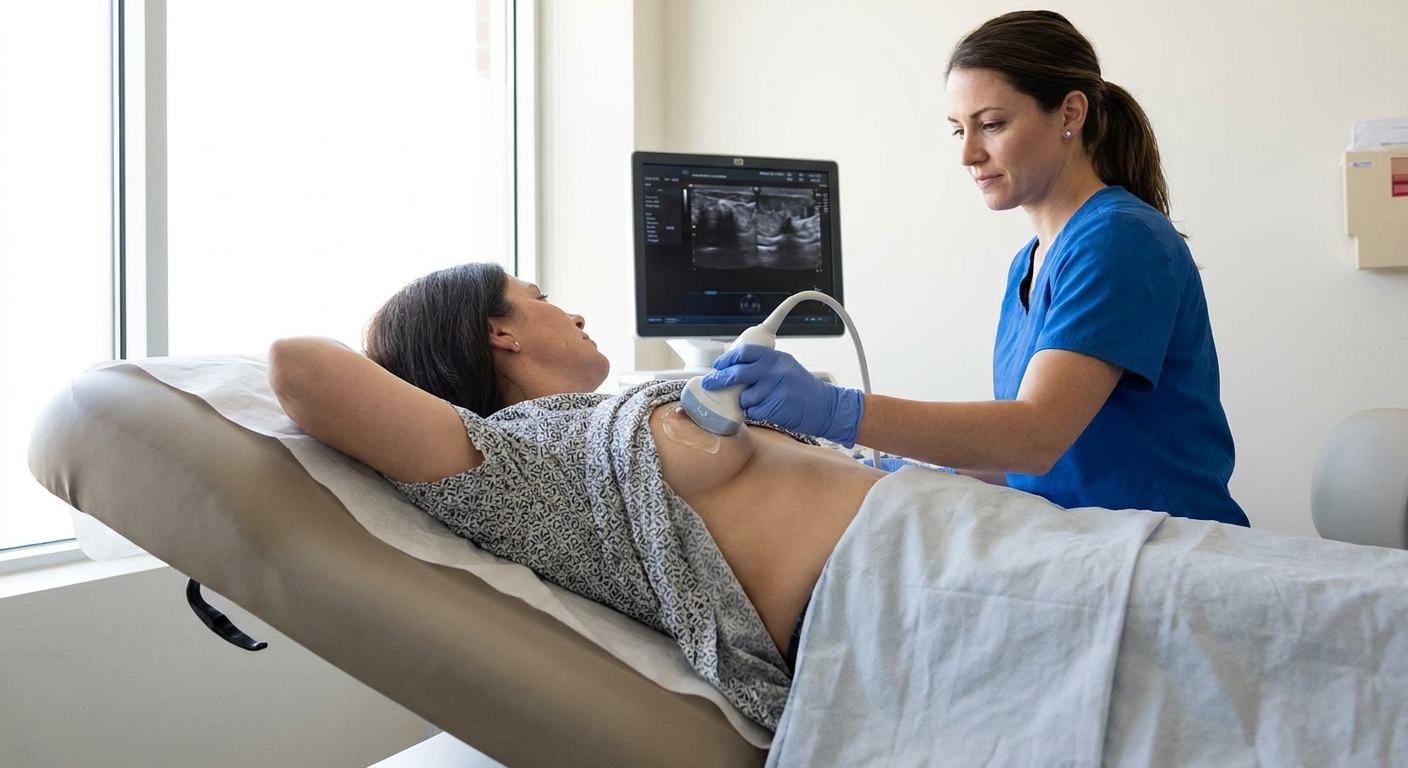
What ultrasound is like
Ultrasound is quick and does not involve radiation. A technician or clinician will use gel and a handheld probe to look for a fluid pocket. If they see an abscess, they can often measure it, describe its location, and help guide next steps.
Treatment
If an abscess is present, treatment is usually two parts:
- Antibiotics to treat the infection in the surrounding tissue and reduce spread
- Drainage to remove the trapped fluid pocket so the area can actually heal
Antibiotic choice depends on your history, local resistance patterns (including MRSA in some communities), and culture results when fluid is collected.
Drainage options
Your clinician will recommend an approach based on size, location, how close it is to the skin or areola, and whether it has multiple pockets. Drainage is often outpatient and may be done by radiology (ultrasound-guided), breast surgery, or a clinician with the right training and setup.
- Needle aspiration: A clinician uses a needle to draw fluid out, often guided by ultrasound. Sometimes it needs to be repeated on another day, especially if the abscess refills.
- Small catheter drainage: A tiny tube may be left in place briefly to keep draining, which can reduce repeat procedures.
- Incision and drainage: Sometimes needed for larger or complex abscesses, or when aspiration or catheter drainage is not working.
Most parents tell me the anxiety is worse than the procedure. There can be pressure and soreness afterward, but many feel relief quickly once the “locked in” pain is released.
What happens to the fluid
Clinicians often send the fluid for culture to identify the bacteria and ensure you are on the most effective antibiotic. If you are not improving on your current medication, this information can be very helpful.
Do I need to stop breastfeeding?
In many cases, no. Continuing to breastfeed or pump is often encouraged because regular milk removal supports healing and protects supply. That said, there are situations where your clinician may recommend temporary adjustments, like pumping instead of direct feeding on that side if latch is too painful, or modifying feeding if there is active drainage.
One practical nuance: if drainage, an open incision, or a drain is positioned where fluid could contact your baby’s mouth, your clinician may suggest pumping instead (and sometimes discarding milk if it could be contaminated by pus or blood). In many other setups, feeding can continue with careful dressing and hygiene. Ask for a clear, specific plan for your anatomy and your baby’s safety.
If anyone tells you to stop breastfeeding completely, ask what the specific reason is. Sometimes it is necessary, but often it is not.
Protect your supply
An abscess can make feeding feel complicated. Your goal is to keep milk moving without turning every session into a battle.
Helpful do’s
- Keep milk removal consistent: Aim for your usual feeding frequency if possible.
- Use comfort measures: Cool packs after feeding can reduce swelling. Gentle warmth before feeding can help with letdown if that feels good.
- Adjust positions: Side-lying or football hold can reduce pressure on a tender area.
- Use a properly fitted pump flange: Poor fit can worsen nipple trauma and make pain spiral.
- Use pain relief as directed: Many breastfeeding parents can use acetaminophen or ibuprofen if safe for them, but confirm with your clinician.
What to avoid
- Aggressive massage or “trying to smash the clog out.” With infection and inflamed tissue, this can worsen swelling and pain.
- Overpumping to “empty completely” every time. This can drive oversupply, which can make inflammation harder to calm.
- Skipping feeds because it hurts. If nursing is too painful, switch to gentle pumping or hand expression, but try not to let long gaps build up pressure.
If you have a drain or open area
Ask your clinician for specific guidance on feeding around dressings, how to keep the area clean, and whether to nurse on that side. Many parents can continue with some modifications, but safety depends on your exact situation and whether drainage could contact your baby’s mouth.

Recovery
Most families want one thing: a timeline. Every case is different, but here is a realistic general pattern:
- After drainage: Many people notice less intense, “throbbing” pain within 24 hours, though tenderness can linger.
- Over the next week: Swelling and redness should steadily improve. You may still feel a firm area as inflammation settles.
- Follow-up: You might need a repeat ultrasound, repeat aspiration, or a check to ensure the pocket is resolving.
If you are not improving day by day after the plan is in place, call back. You are not bothering anyone. That follow-up is part of good care.
Milk supply
An abscess can affect supply, but many parents maintain or regain supply with consistent milk removal and good support.
Supply can dip because:
- pain makes feeding less effective
- swelling can compress ducts temporarily
- illness and dehydration reduce output
- you may feed less on the affected side for a period
The good news is that breasts are resilient. With a workable pumping plan when needed and a gradual return to comfortable nursing, many families do very well.
Questions to ask
- Do you suspect an abscess, and can we do an ultrasound today or tomorrow?
- What is the size and location of the fluid pocket?
- Will you culture the fluid to tailor antibiotics?
- Can I keep breastfeeding, and if so, what adjustments do you recommend?
- How often should I pump or feed while this heals?
- When do you want to see me back, and what symptoms mean I should return sooner?
- Who will do the drainage if I need it (radiology, breast surgery, OB, other)?
Reduce the chance of recurrence
Abscesses can recur, especially if the underlying causes are not addressed. Prevention is not about being perfect. It is about reducing strain on your breast tissue.
- Address milk flow issues early: painful latch, tongue-tie concerns, pump problems, oversupply, or skipped feeds are common triggers.
- Avoid pressure points: tight bras, underwire, heavy diaper bag straps, or sleeping positions that compress one spot.
- Get help for nipple damage: cracks can be a doorway for bacteria and also make feeding inefficient.
- Follow your treatment plan through: finish antibiotics as prescribed and attend follow-up if recommended.
When it is not infection
Most persistent lumps in breastfeeding are still related to inflammation, plugged ducts, or infection. Rarely, a non-lactation issue can mimic mastitis or fail to improve with standard treatment.
If a lump, skin change, or redness does not resolve after treatment, keeps returning in the same spot, or you notice signs like skin dimpling, new nipple inversion, or bloody nipple discharge, insist on follow-up. You may need repeat imaging and a broader evaluation to rule out other causes.
A final note
If you are reading this at 3 AM while your baby finally sleeps and your breast is throbbing, I want you to hear this clearly: you do not have to tough it out.
Mastitis is common, and abscesses happen even to parents who are doing everything right. Prompt evaluation can mean faster relief, less disruption to breastfeeding, and fewer repeat visits.
If your symptoms are worsening, you have a persistent lump, or you are not improving within 24 to 48 hours of a solid mastitis plan, call for same-day care. You deserve to feel better, and you deserve support while you get there.
Sources
- Academy of Breastfeeding Medicine (ABM) Clinical Protocol #36: The Mastitis Spectrum (Revised 2022)
- American College of Obstetricians and Gynecologists (ACOG) patient guidance on breastfeeding challenges
- World Health Organization (WHO) breastfeeding resources and management of breastfeeding complications