Canker Sores vs. Cold Sores in Kids
Sarah Mitchell
Sarah Mitchell is a Registered Pediatric Nurse and a mother of three who has spent over a decade helping families navigate the beautiful, chaotic early years of childhood. She combines evidence-based medical knowledge with real-world parenting experience to offer practical, compassionate advice. At Awesome Parent, Sarah's mission is to help exhausted parents find solutions, trust their instincts, and finally get some sleep.
If your child is suddenly refusing their favorite foods, drooling a whole lot, or crying when a toothbrush gets anywhere near their mouth, you are not being dramatic for wondering what is going on. Mouth sores can be brutally painful, and two very common culprits get mixed up all the time: canker sores (aphthous ulcers) and cold sores (herpes simplex virus, usually HSV-1).
They can look similar at first glance, but they behave differently in three big ways: where they show up, what causes them, and whether they are contagious. Let’s sort it out, then talk about what actually helps your child feel better tonight.
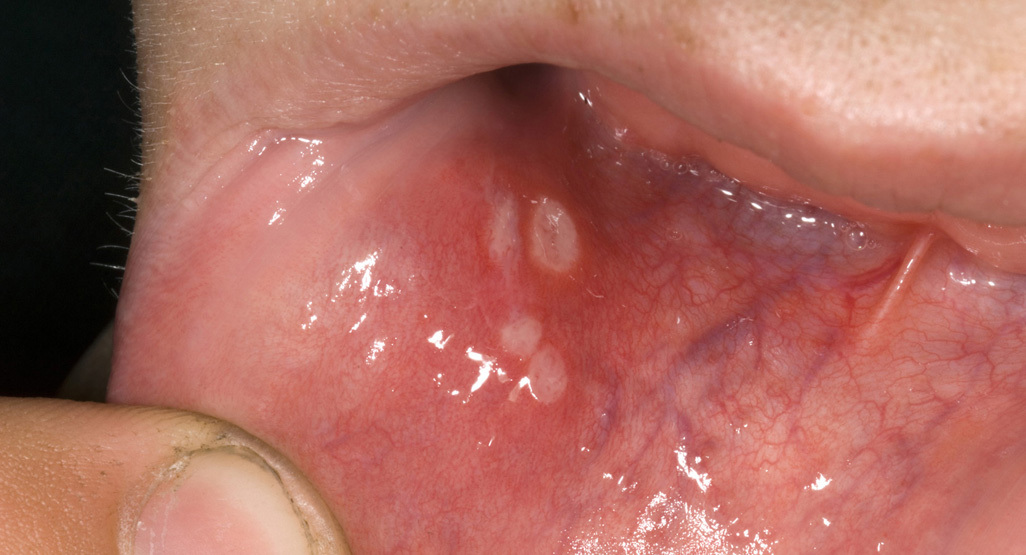
Quick difference: canker sore vs. cold sore
Use this as your fast mental checklist. Then we will go deeper.
| Feature | Canker sore (aphthous ulcer) | Cold sore (HSV-1) |
|---|---|---|
| Where it appears | Usually inside the mouth on softer, non-keratinized tissue: inner lips/cheeks, under or sides of the tongue, floor of mouth, soft palate | Often starts at the lip border or around the mouth. Inside-the-mouth HSV is more likely with a first infection (widespread) or on hard palate/attached gums |
| What it looks like | Round or oval sore with a white or yellow center and a red rim (often looks like one angry crater) | Cluster of small blisters that break open into shallow ulcers, then crust over |
| Contagious? | No | Yes. Most contagious when blisters/ulcers are present and weeping. Shedding can still occur even without visible sores |
| Common triggers | Mouth injury, stress, illness, certain foods, braces; sometimes vitamin deficiencies | Initial exposure to HSV-1; later reactivation triggered by sun, fever, stress, chapped lips |
| Typical duration | 7 to 14 days | 7 to 10 days (first episode can be longer) |
If the sore is inside the lip or cheek and looks like one crater, think canker. If it is on the outside and starts as tiny blisters, think cold sore.
What else could it be?
One quick reality check: not every painful mouth sore is “canker vs. cold sore.” In toddlers especially, hand, foot, and mouth disease (HFMD) is a top contender.
HFMD (Coxsackievirus)
- Mouth: multiple small sores, often toward the back of the mouth (soft palate, throat) and on the tongue
- Body clues: rash or spots on the hands, feet, diaper area, or elbows and knees
- Contagious: yes, spreads easily in daycares
If you see mouth sores plus a hand or foot rash, HFMD jumps to the top of the list.
Other possibilities that deserve a call if things do not fit: thrush (white patches that wipe off and leave redness), strep (severe sore throat, fever, and sometimes red spots on the roof of the mouth), and trauma (a sharp tooth edge or cheek bite that keeps getting re-injured).
What causes canker sores in kids?
Canker sores are not caused by a virus the way cold sores are. They are more like an over-the-top immune response in the mouth lining. The exact reason varies by child, and sometimes we never find one clear “why.”
Common triggers
- Minor mouth injury: biting the cheek, a sharp chip, aggressive brushing, dental work, braces
- Illness or stress: yes, even kid stress counts, and so does traveling or a sleep disruption
- Certain foods: acidic or spicy foods (citrus, tomatoes, pineapple), salty snacks; some kids react to chocolate or nuts
- SLS toothpaste: switching to an SLS-free toothpaste may help some children who get frequent ulcers
- Nutritional deficiencies: iron, folate, vitamin B12, zinc can be associated in some kids
- Underlying conditions (less common): celiac disease, inflammatory bowel disease, immune conditions
Most kids with canker sores are otherwise totally healthy. But if sores are frequent, large, or slow to heal, it is worth discussing patterns with your pediatrician or dentist.
What causes cold sores in kids?
Cold sores are caused by herpes simplex virus, most often HSV-1. Many people are exposed in childhood. After a child is infected, the virus stays in the body and can “wake up” later, causing repeat cold sores.
How kids catch HSV-1
- Kissing from someone shedding the virus (even without a visible sore)
- Sharing items that touch saliva, like cups, utensils, lip balm, toothbrushes
- Close contact in families or daycare, especially with toddlers who put everything in their mouths
Common triggers (reactivation)
- Fever or illness (the classic “fever blister”)
- Sun exposure and wind
- Chapped lips
- Stress and lack of sleep
Important nuance: the first HSV infection in a child can look different than the classic “one sore on the lip.” Some kids get gingivostomatitis, meaning widespread mouth sores plus swollen gums and fever. Recurrent intraoral HSV, when it happens, is more often on hard palate or attached gums than on the inner cheeks. If your child has fever plus lots of sores, call early, mainly to prevent dehydration and to discuss whether antiviral timing makes sense.

Contagious? School and siblings
Canker sores
Not contagious. Your child can go to school or daycare as long as they feel well enough. No special isolation needed.
Cold sores
Contagious, especially when blisters are present, open, or oozing. Once a sore is dry and crusted, it is often less contagious, but HSV can still shed sometimes even when skin looks normal.
Family rules that work
- No sharing cups, utensils, straws, toothbrushes, washcloths, towels, or lip products during an outbreak.
- Hand hygiene after touching the mouth or applying any ointment.
- Keep little fingers busy: if your child picks the sore and then rubs their eyes, HSV can cause a serious eye infection. If you see eye redness, pain, discharge, or light sensitivity with a cold sore, call urgently.
- Sports note: for close-contact sports (like wrestling), ask your coach or pediatrician about return-to-play policies during active lesions.
Pain care that is safe
Whether it is a canker sore or a cold sore, the goals are the same: control pain, keep fluids going, and support healing. Here is what I recommend most often as a triage nurse and a mom.
First-line pain medicine
- Acetaminophen (Tylenol) can be very helpful. Use the dosing on your product label based on your child’s current weight.
- Ibuprofen (Advil, Motrin) can also help for kids 6 months and older. Use label dosing by weight.
- Avoid ibuprofen if your child is vomiting a lot, severely dehydrated, or has been told not to take NSAIDs.
- Aspirin is not recommended for children due to the risk of Reye syndrome.
Foods that hurt less
- Yogurt, smoothies (not too acidic), applesauce
- Popsicles or ice chips (great for numbing and hydration)
- Oatmeal cooled down, mashed potatoes, scrambled eggs
- Warm (not hot) soups can help some kids, but many prefer cold
Skip salty, spicy, and acidic foods for a few days. Even orange juice can feel like rubbing lemon on a paper cut.
Salt-water rinses
For older kids who can reliably spit, a simple salt-water rinse can reduce irritation and keep the area clean.
- Mix 1/2 teaspoon of salt in 1 cup of warm water.
- Swish gently for 15 to 30 seconds, then spit.
- Try 2 to 4 times a day.
If your child is too young to spit, skip rinses and focus on fluids, pain relief, and gentle brushing.
OTC options and cautions
OTC products vary a lot, and some are not appropriate for young kids.
- Barrier pastes and films (often marketed for canker sores): these can cover the sore and reduce pain with eating. Follow package directions carefully.
- Benzocaine numbing gels: many pediatric clinicians recommend avoiding these in young children. Benzocaine has been linked to a rare but serious condition called methemoglobinemia. If you are considering a numbing gel, check the label age limits and ask your pediatrician first, especially for kids under 2.
- Honey (for kids over 1): some families find a small dab soothing on canker sores. Do not use honey under 12 months.
- Cold sore creams: some OTC cold sore products are labeled for older children and adults. For kids, especially under 12, confirm with your pediatrician and follow the label directions.
Also: avoid using leftover prescription mouth medications (like topical steroid dental pastes or “magic mouthwash” mixes) unless your child’s clinician specifically told you to use them for this episode.
Antivirals for cold sores
Prescription antivirals (like acyclovir or valacyclovir) can help certain kids with HSV, especially if started early for a first outbreak or severe symptoms. They are not needed for every child with an occasional small cold sore, but they are worth discussing if:
- Your child has a first outbreak with fever and multiple mouth sores
- They have frequent recurrences that disrupt eating or school
- They have an immune condition or take immune-suppressing medication
Preventing dehydration
The biggest short-term risk with painful mouth sores is that kids stop drinking. A sore that looks “small” can still feel enormous.
Hydration tips
- Offer tiny sips often, like every 5 to 10 minutes.
- Use a straw if it helps bypass a sore (unless your dentist has told you to avoid straws after dental work).
- Try oral rehydration solutions if your child is also sick with vomiting or diarrhea.
- Choose cool liquids over hot, and avoid acidic drinks.
Dehydration signs
- Urinating much less than usual (fewer wet diapers, or not peeing for 8 to 12 hours in older kids)
- Dry mouth, no tears when crying
- Sleepiness, dizziness, fast breathing, or looking “wiped out”
If you are worried about dehydration, call your pediatrician the same day. Dehydration is one of those problems that is much easier to fix early.
When to get medical care
Most canker sores and simple cold sores can be managed at home. But some situations deserve a call or a visit.
Call urgently if
- Your child is not drinking or shows signs of dehydration
- There is high fever, severe sore throat, or your child looks very ill
- Sores are all over the mouth with swollen, bleeding gums (possible primary HSV gingivostomatitis)
- Your child has eye pain, redness, discharge, or light sensitivity along with cold sores
- Your child is immunocompromised
- The sore is on the lip or face with rapidly spreading redness, warmth, or pus (possible bacterial infection on top)
Make an appointment if
- Sores last longer than 2 weeks
- Canker sores are frequent, unusually large, or keep coming back
- Your child has mouth sores plus symptoms like weight loss, chronic diarrhea, recurrent fevers, or poor growth
And trust your gut. If your child’s pain seems out of proportion, they cannot sleep, or you are seeing something you do not recognize, it is completely reasonable to ask for a clinician to take a look.

How to prevent future sores
Canker sores
- Consider an SLS-free toothpaste if your child gets frequent ulcers and your dentist agrees.
- Use a soft toothbrush and gentle technique.
- Limit trigger foods during flare-ups, and watch for patterns.
- If sores are frequent, ask your pediatrician whether checking iron, B12, folate, or zinc makes sense.
Cold sores
- Use lip balm with SPF for kids who get sun-triggered outbreaks.
- Teach “no sharing” of mouth-contact items, especially during outbreaks.
- Talk to your pediatrician about an antiviral plan if outbreaks are frequent or severe.
Bottom line
Canker sores are usually inside-the-mouth ulcers on softer tissue and are not contagious. Cold sores are caused by HSV and are contagious, usually starting as blisters on or around the lips (and in some cases inside the mouth, especially with a first infection). Either way, your best next step is pain control plus being proactive about fluids.
If you want one simple rule for the middle of the night: if your child is not drinking, not peeing, or seems unusually lethargic, do not wait it out. Call your pediatrician and get help early. You are not overreacting. You are preventing a rough problem from becoming an urgent one.
References
- CDC: Herpes Simplex Virus (HSV) (Overview, transmission, and prevention)
- American Academy of Pediatrics: Herpes Simplex Virus Infections (parent education and clinical overviews via AAP resources)
- FDA Drug Safety Communication: Benzocaine and risk of methemoglobinemia
- NIH MedlinePlus: Canker sores and Cold sores
- CDC: Hand, Foot, and Mouth Disease (HFMD)