Cat Bites in Kids: Why They Get Infected So Fast
Sarah Mitchell
Sarah Mitchell is a Registered Pediatric Nurse and a mother of three who has spent over a decade helping families navigate the beautiful, chaotic early years of childhood. She combines evidence-based medical knowledge with real-world parenting experience to offer practical, compassionate advice. At Awesome Parent, Sarah's mission is to help exhausted parents find solutions, trust their instincts, and finally get some sleep.
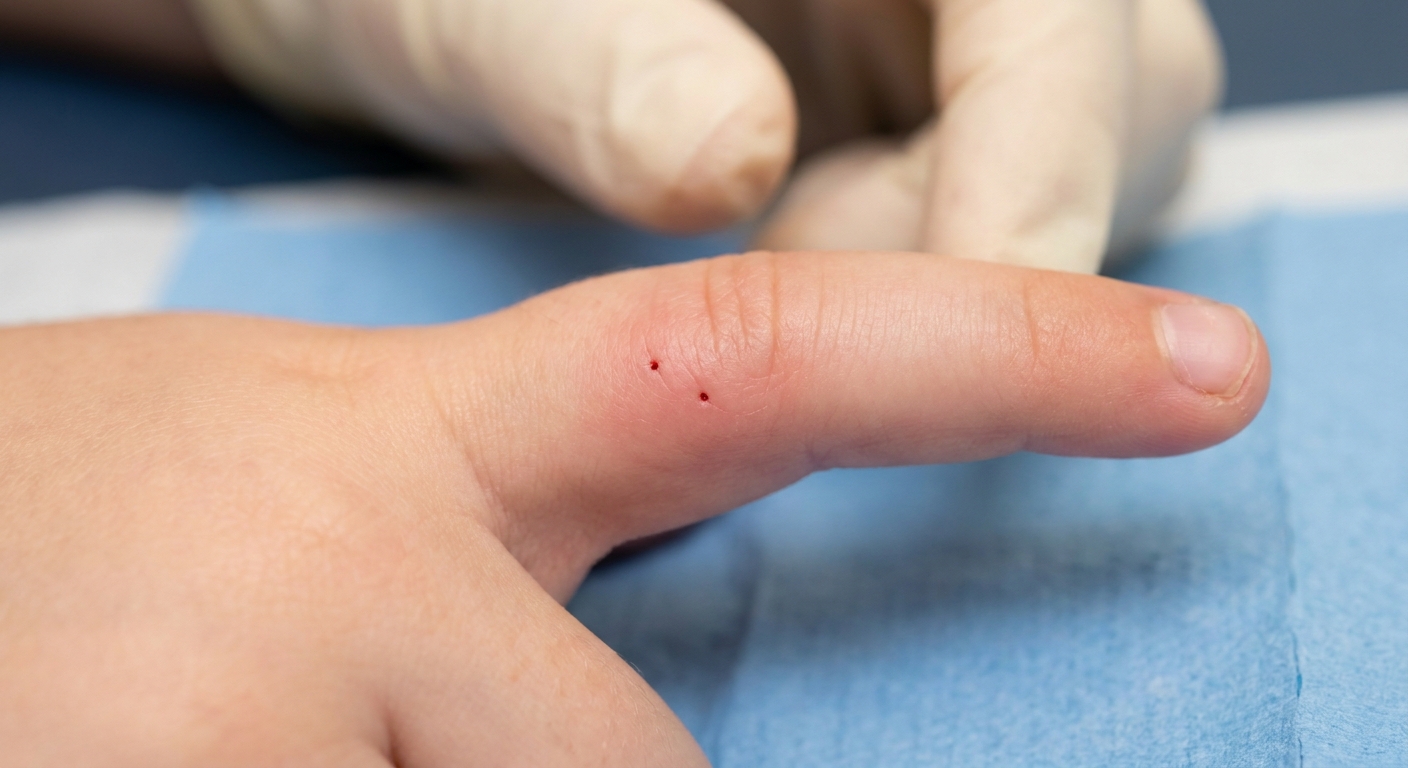
Cat bites have a way of looking “not that bad” at first. Two tiny punctures, maybe a little swelling, and your child is already back to chasing the cat again. But medically, cat bites are a different situation than most minor nips or scratches.
As a pediatric nurse who has triaged a lot of bites, here is the big takeaway: cat teeth are sharp and skinny, which means they can inject bacteria deep under the skin where it gets trapped. That is why cat bites, especially on hands and fingers, can get infected faster than injuries that look more dramatic on the surface.
Quick note: This is general information and not a substitute for medical care. If you are worried, trust your instincts and get your child seen.

Why cat bites are higher risk
Dog bites often cause tearing, bruising, or shallow punctures. Cat bites are usually small, deep punctures. The skin can close over quickly, which is great for stopping bleeding but not great for letting bacteria drain out.
The most common bacteria we worry about from cats is Pasteurella (especially Pasteurella multocida). It can cause a rapidly developing skin and soft tissue infection. In practical parent terms, that means a bite that looked fine at bedtime can look angry by breakfast.
Hand bites matter more
Bites on the hand, fingers, wrist, or near joints deserve extra respect. Those areas have tight spaces, tendons, and joints close to the surface. Infection can spread into:
- Tendon sheaths (can affect motion and cause severe pain)
- Joints (septic arthritis)
- Bone (osteomyelitis)
This is also why clinicians take cat bites to the hand seriously even when the punctures are tiny.
What to do right away
If your child is stable and the bleeding is not severe, you can do immediate first aid at home while you decide whether they need same-day care.
Step-by-step first aid
- Wash your hands.
- Rinse the bite under running water for several minutes.
- Wash with soap. Be gentle but thorough around puncture sites.
- If it is mildly oozing, do not aggressively squeeze or dig into the punctures. If bleeding is more than mild, apply steady pressure with clean gauze or a cloth.
- Apply a thin layer of antibiotic ointment if your child is not allergic, then cover with a clean bandage.
- Elevate the hand or affected area if possible to reduce swelling.
Avoid putting hydrogen peroxide or rubbing alcohol into puncture wounds, since they can irritate tissue. Soap and running water does the heavy lifting. (If you use anything, keep it to cleaning surrounding skin, not flushing inside the puncture.)
What not to do
- Do not close puncture wounds with glue or tight butterfly strips at home.
- Do not “test” the wound by poking it open.
- Do not soak the wound (baths, pools, hot tubs) for the first day or two. Showering and gentle washing is fine.
- Do not ignore a hand bite just because the punctures are small.
Bandage basics: change the dressing at least daily or anytime it gets wet or dirty. Keep it clean and dry.
How fast can infection show up?
With cat bites, infection often shows up within 12 to 24 hours, sometimes as early as a few hours. But it can also develop more slowly over the next several days (24 to 72 hours or longer).
That does not mean every bite will get infected. It means the timeline for “wait and see” is shorter than many parents expect.
Early signs of infection
- Increasing warmth around the puncture
- Spreading redness that grows beyond the immediate bite area
- Swelling that is worsening, not improving
- Throbbing pain or tenderness that escalates
- Pus or cloudy drainage
- Fever, chills, or your child seems unusually tired
- Red streaking traveling up the hand or arm (a sign the infection may be moving through lymph vessels)
If you see red streaking, significant swelling, or fever, it is time to be seen urgently.
When to go to urgent care
For cat bites, I am more “same-day” than most parents expect, especially for certain locations and situations. Consider urgent care today if:
- The bite is on the hand, finger, wrist, foot, face, or near a joint.
- The bite is a deep puncture or there are multiple punctures.
- Your child has increasing pain, warmth, swelling, or spreading redness.
- Your child has fever or looks ill.
- Your child is immunocompromised (for example, on chemotherapy, high-dose steroids, or has certain immune conditions).
- You are not sure your child’s tetanus shot is up to date.
- The bite was from a stray, unknown cat, or the cat cannot be observed.
- The bite happened hours ago and was not cleaned well, or care is delayed.
Why same-day? Because many cat bites need prescription antibiotics early. Clinicians often prescribe preventive antibiotics for cat bites, especially for hand and finger bites, deep punctures, facial bites, immunocompromised kids, or delayed presentation, even before clear infection signs show up.
Helpful details to bring: time of the bite, where on the body it happened, your child’s vaccine status (especially tetanus), and what you know about the cat’s rabies vaccination and whether it can be observed. In some areas, bites may need to be reported to local animal control or public health.

When to go to the ER
Go to the emergency room now or call emergency services if:
- Bleeding will not stop after 10 minutes of steady pressure.
- Your child cannot move a finger or joint normally, or has severe pain with movement.
- The hand or finger becomes very swollen, very painful, or looks tight and shiny.
- There is rapidly spreading redness over hours.
- You see red streaking with fever or your child looks very unwell.
- The bite involves the eye or deep facial structures.
- Your child has pain that feels out of proportion to how the wound looks, especially with a hand bite.
What clinicians may do
Parents are often surprised that a tiny cat bite can lead to a big medical plan. Here are common next steps in a clinic or urgent care setting:
- Thorough irrigation with saline or water to flush bacteria.
- Assessment of motion and sensation, especially for hand bites.
- Antibiotics. Cat bites frequently get an antibiotic that covers Pasteurella. If your child is allergic to penicillin, clinicians choose an alternative.
- X-ray if there is concern for a tooth fragment, foreign body, deep injury, or bone involvement.
- Referral to a hand specialist if the bite is near tendons or joints, or if signs suggest a deeper infection.
Many cat punctures are not stitched because closing them can trap bacteria. If a facial wound needs cosmetic repair, clinicians weigh infection risk versus scarring and choose the safest option.
Rabies: do we need shots?
Rabies risk depends on your region and the situation. It is rare in many places, but it is serious enough that we do not guess. The need for rabies prevention depends on local public health guidance and whether the animal can be observed or tested.
Questions a clinician will ask
- Was it a family pet or an unknown or stray cat?
- Is the cat available to be observed for the next 10 days?
- Is the cat acting normally?
- Is the cat’s rabies vaccination current (if known)?
- Where do you live and what is rabies activity like in your region?
In many jurisdictions, if a healthy dog, cat, or ferret can be observed for 10 days and stays healthy, rabies post-exposure prophylaxis is typically not needed. If the animal is stray, unavailable, or behaving strangely, clinicians may recommend contacting public health and starting rabies post-exposure prevention.
Translation: bring the details you have, and let your medical team and local guidance do the heavy lifting.
Tetanus: the quick check
Tetanus protection depends on your child’s vaccine status and how long it has been since their last tetanus-containing vaccine.
- If your child is fully immunized, they may still need a booster depending on timing and wound type.
- If vaccines are not up to date, clinicians may recommend a vaccine and, in some situations, tetanus immune globulin.
If you are unsure, urgent care can check the schedule with you. No judgment, just a safety step.
Cat bite vs dog scratch
On Awesome Parent you will see dog bite first aid discussed too, and a lot overlaps. The difference is the risk profile:
- Superficial scratches often do well with careful washing and monitoring, as long as the skin is not deeply punctured and your child is otherwise healthy.
- Cat bites are more likely to be deep punctures, and the infection timeline can be faster, especially on hands.
So if you are comparing a superficial scratch on a calf to a cat puncture on a finger, the finger puncture often deserves the earlier medical visit.
How to monitor for 48 hours
If your child was assessed and sent home, or if you and your clinician decide monitoring is reasonable, here is a simple plan:
- Recheck the bite 3 to 4 times a day in good light.
- Look for spreading redness. A small halo is common. Expansion is the issue.
- Feel for warmth compared with nearby skin.
- Check function: can your child bend and straighten fingers without increasing pain?
- Take your child’s temperature if they seem off.
If things are worse at any check, do not wait for the next one.
One extra “later” thing to know: if a scratch happened too, watch over the next couple of weeks for a tender swollen lymph node (often in the armpit or neck) and fever. That can be a sign of cat scratch disease (Bartonella henselae) and is worth a call to your child’s clinician.
Prevention that works
Most cat bites happen during play, when a child misreads a cat’s “I am done now” signals. A few practical strategies:
- Teach kids to watch for tail swishing, pinned ears, or sudden stillness.
- Use toys on strings or wands instead of hands for play.
- Give cats an escape route. A cornered cat is a biting cat.
- Supervise toddlers closely. Toddlers love grabbing. Cats do not love being grabbed.

Quick checklist at 3 AM
- Wash with soap and running water right away.
- Hand or finger bite? Lean toward same-day urgent care.
- Watch for warmth, spreading redness, swelling, fever, red streaks.
- If you see red streaking, fever, fast worsening, motion pain, or pain out of proportion, go urgently.
- Know the basics: tetanus status and whether the cat is known and can be observed.
And if you are staring at a tiny puncture thinking, “Surely this cannot be a big deal,” you are not overreacting by getting it checked. With cat bites, early care is often what keeps it from becoming a bigger deal.