Cat Scratch Disease in Kids
Sarah Mitchell
Sarah Mitchell is a Registered Pediatric Nurse and a mother of three who has spent over a decade helping families navigate the beautiful, chaotic early years of childhood. She combines evidence-based medical knowledge with real-world parenting experience to offer practical, compassionate advice. At Awesome Parent, Sarah's mission is to help exhausted parents find solutions, trust their instincts, and finally get some sleep.
If your child has a mystery lump after a cat scratch, you are not alone. I saw this all the time as a pediatric triage nurse: a perfectly healthy kid, one tiny scratch, and then a week or two later a swollen, tender lymph node that sends the whole household into Google panic mode.
The good news is that cat scratch disease (CSD) is usually self-limited, meaning it tends to get better on its own. The trick is knowing what “normal” looks like, how long the lump can hang around, and which symptoms mean it is time to call your child’s clinician the same day.

What is cat scratch disease?
Cat scratch disease is an infection most commonly caused by a bacterium called Bartonella henselae. Kids usually get it after a scratch or bite from a cat, especially a kitten. The bacterium can also get into the skin when a cat licks an open wound.
One detail many parents do not hear until later: cats typically get Bartonella from fleas. The cat may look completely healthy. So if you are thinking, “But our cat is an indoor angel,” you can still see CSD, especially if flea prevention is inconsistent.
How it spreads
Common ways kids get infected
- Scratch that breaks the skin
- Bite
- Cat saliva contacting an open cut or scab
Less likely scenarios
- Casual petting with intact skin
- Being near a cat that has Bartonella but no scratch, bite, or saliva exposure to broken skin
Cat scratch disease is not typically spread from child to child. It is mainly a cat-associated infection.
One quick note: animal bites (including cat bites) can also cause other infections that are not CSD, like Pasteurella. If your child has a bite puncture, worsening pain, spreading redness, or fever, it is worth calling even aside from cat scratch disease.
Symptoms parents notice first
CSD often comes in two stages.
Stage 1: the skin spot
At the scratch or bite site, you might see a small red bump, blister, or scab. This can show up within a few days and may be easy to miss, especially on busy kid skin that is always sporting a scrape.
Stage 2: swollen lymph nodes (the “lump”)
Then the classic symptom appears: a swollen lymph node near the area of the scratch. Lymph nodes are part of the immune system. When they swell, it usually means the body is doing its job and reacting to an infection.
Common locations include:
- Armpit (after a hand or arm scratch)
- Neck or under the jaw (after a head, face, or scalp scratch)
- Groin (after a leg scratch)
Your child may also have:
- Low-grade fever
- Fatigue or “just not themselves” energy
- Tenderness over the lymph node
- Less often: headache, sore throat, decreased appetite

Timeline
Here is the timeline I share with families most often.
- Day 0: Scratch or bite happens.
- Days 3 to 10: Small bump or scab at the scratch site may appear.
- Weeks 1 to 3: Lymph node swelling commonly starts. This is the “Where did this lump come from?” moment.
- Weeks 2 to 8: The node is usually at its most noticeable, then gradually improves.
- Often 2 to 4 months, sometimes longer: Some lymph nodes stay enlarged for quite a while, even after your child feels fine. They should slowly shrink and become less tender over time.
What makes parents uneasy is that lymph nodes can remain palpable even when the infection is gone. That alone is not automatically dangerous. What matters is the overall trend and the presence or absence of red-flag symptoms.
When it can get complicated
Most kids: mild and self-limited
In otherwise healthy children, cat scratch disease usually stays localized to one region of swollen nodes and resolves with time. Comfort care and watchful waiting are often appropriate, sometimes with antibiotics depending on your child’s symptoms and your clinician’s exam.
Possible complications
Complications are less common, but parents should know the names so they can recognize the patterns.
- Suppurative lymphadenitis: the lymph node forms pus and becomes very painful, red, and swollen. Sometimes it needs drainage.
- Eye involvement (Parinaud oculoglandular syndrome): red, irritated eye with nearby lymph node swelling, usually in front of the ear.
- Hepatosplenic disease: fever with abdominal pain or tenderness, sometimes with enlarged liver or spleen.
- Neurologic complications (rare): severe headache, confusion, balance issues, seizures.
- Bone involvement (rare): persistent focal bone pain, limp.
Kids with weakened immune systems can have more severe disease and should be assessed promptly if exposure is suspected. In some immunocompromised patients, Bartonella can cause unusual blood vessel and organ involvement (your specialist will guide you on what to watch for and when to call).
When to call the doctor
Call your child’s clinician within 24 hours if:
- Your child has a swollen lymph node larger than about 1 inch (2.5 cm), or it is rapidly growing
- Fever lasts more than 3 days or is consistently 102°F (38.9°C) or higher, or per your clinic’s guidance
- The node is very tender, warm, or the skin over it looks increasingly red
- Your child has significant fatigue, poor intake, or weight loss
- The scratch site looks infected (spreading redness, pus, worsening pain)
- Your child has eye redness with nearby swelling, especially after a cat lick or scratch
Seek urgent care or emergency evaluation now if:
- Difficulty breathing or swallowing due to neck swelling
- Severe headache, confusion, stiff neck, new weakness, trouble walking, or seizures
- Signs of severe illness: lethargy, dehydration, persistent vomiting
- Very high fever (for example 104°F or 40°C) or a fever in a young infant per your clinic’s fever policy
If you are unsure, call. In triage, I would always rather talk to a worried parent early than try to catch up after things escalate.
What you can do at home
For the scratch or bite
- Wash with soap and running water for several minutes.
- Apply a thin layer of petroleum jelly to keep it from cracking. If you use an over-the-counter antibiotic ointment, watch for irritation or rash (some kids react to ingredients like neomycin), and remember cleansing is the main event.
- Keep it clean and discourage picking.
For the swollen lymph node
- Warm compress 10 to 15 minutes a few times a day can help soreness.
- Use age-appropriate fever and pain relief (ask your clinician about dosing if you are not sure).
- Encourage fluids and rest.
Avoid aggressively massaging the lymph node. It will not “drain it” and can make it more tender.
Do kids need antibiotics?
Sometimes. Many mild cases improve without them, but antibiotics may be recommended when:
- Symptoms are moderate to severe (significant pain, fever, multiple nodes)
- The lymph node is large or not improving
- There are signs of complications (eye involvement, liver or spleen involvement)
- Your child is immunocompromised
Your clinician will choose an antibiotic based on your child’s age, symptoms, and local guidance. The goal is often to speed improvement in some cases and help with symptom burden. Not every case needs medication to resolve.
When tests or imaging matter
This is where a lot of fear-mongering articles go off the rails. Not every lump needs a battery of tests.
Often, no testing is needed
If your child has a clear story (cat exposure, scratch, localized tender lymph node, mild fever) and looks otherwise well, your clinician may diagnose CSD based on history and exam alone.
Labs that may be considered
- Bartonella blood tests (serology): can support the diagnosis, especially if the story is unclear.
- Basic blood work (like a CBC): sometimes used if fever is prolonged, symptoms are more significant, or the diagnosis is uncertain.
One nuance: Bartonella blood tests are not perfect. Timing matters, and results can be tricky to interpret. That is why your child’s overall picture matters more than any single number on a lab report.
Imaging that may be considered
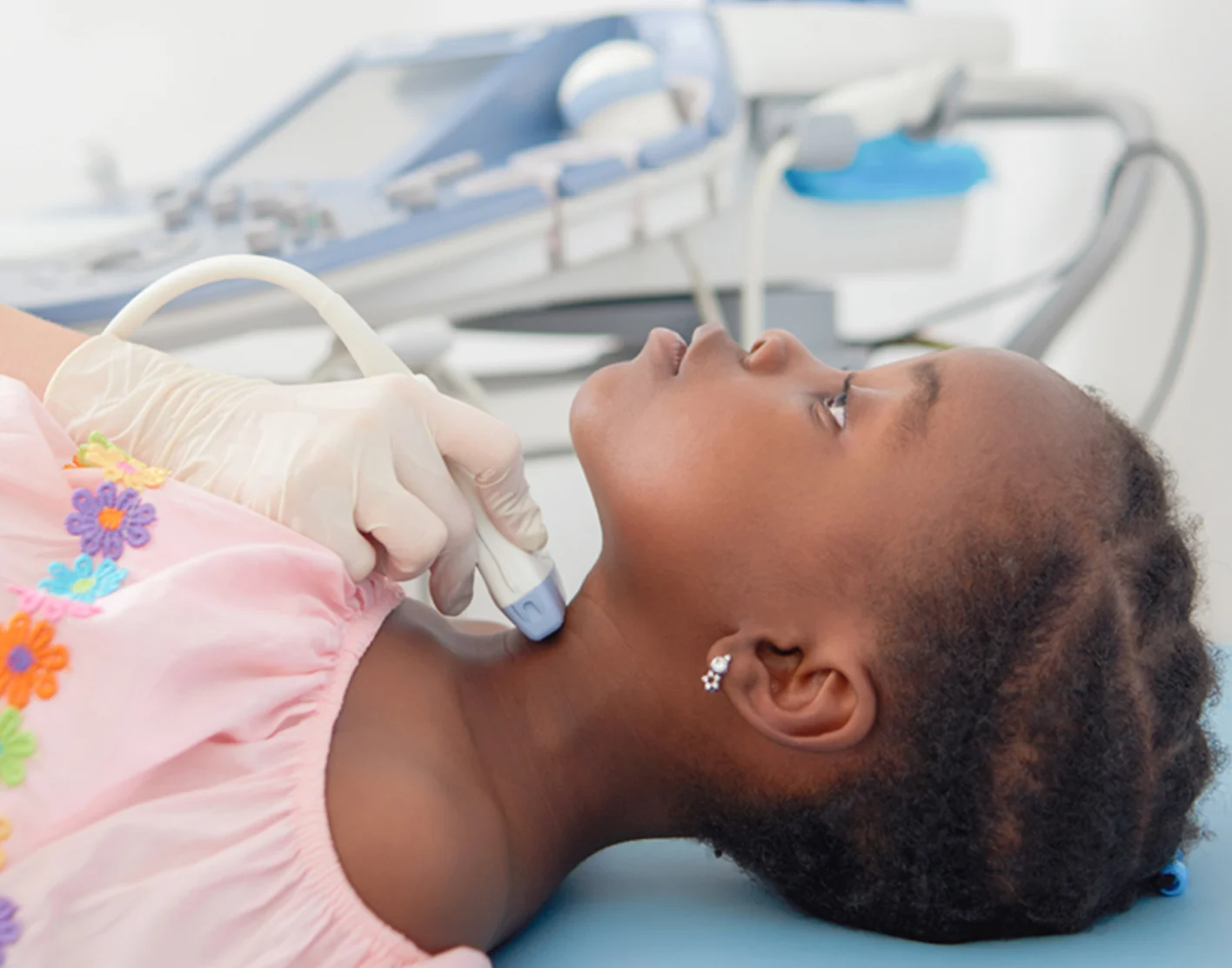
- Ultrasound: often the first choice if a node looks like it might have an abscess (pus) or if the exam is unclear. It is quick and avoids radiation.
- CT or MRI: usually reserved for special situations, like deep neck swelling, concerning symptoms, or when ultrasound does not answer the question.
Imaging is most helpful when the clinician is asking a specific question, like “Is there an abscess that needs drainage?” not simply “Is this lump real?” (It is real. Lymph nodes are very real and can be surprisingly dramatic.)
If it is not CSD
Most of the time, the story and the exam fit cat scratch disease. But your child’s clinician is also watching for other common explanations, like a routine viral illness with reactive lymph nodes, a bacterial skin infection or abscess near the scratch, or (more rarely) other causes of persistent lymph node swelling. This is why the pattern matters: a node that is slowly improving is very different from a node that is steadily enlarging or comes with bigger red-flag symptoms.
How to prevent it
You do not have to rehome the cat. You do not have to wrap your child in bubble wrap. You just need a few practical guardrails.
For your cat
- Flea control is key. Talk to your vet about effective prevention.
- Keep nails trimmed if your cat tolerates it.
- Try to avoid rough play that encourages scratching.
For your child
- Teach “gentle hands,” especially with kittens.
- Avoid letting cats lick open cuts or scabs.
- Wash hands after playing with the cat, particularly before eating.
For the household
- Supervise toddler-cat interactions closely. Toddlers move fast and have big feelings. Cats also have big feelings.
- If your child is immunocompromised, ask your specialist and vet for tailored precautions.

Common questions
Can a swollen lymph node from cat scratch disease be hard?
Yes. Inflamed nodes can feel firm, especially early on. What is reassuring is a node that is tender and gradually shrinking over weeks. Nodes that are persistently enlarging, very hard, fixed in place, or associated with weight loss or night sweats should be evaluated.
Will the lump go away completely?
Usually it shrinks significantly, but some kids will still have a small “leftover” node they can feel for a while. Think weeks to months, and sometimes longer, not days.
Is it dangerous if my child has no fever?
No. Many kids with CSD have little or no fever. The lymph node swelling is often the main feature.
Do we need to test the cat?
Typically no. Management focuses on your child’s symptoms and on flea control for the cat. Your veterinarian can advise if there is any reason to do more.
The bottom line
Cat scratch disease is one of those conditions that feels scarier than it usually is. The classic pattern is a scratch followed by a tender swollen lymph node a week or two later, sometimes with a low-grade fever. Most healthy kids get better with time and supportive care, and some benefit from antibiotics depending on severity.
If the lymph node is rapidly enlarging, very red or painful, your child’s fever is persistent, or you see eye symptoms or signs of more serious illness, call your child’s clinician. Trust your instincts. You know when your kid is “regular sick” versus “something is off.”
Medical note: This article provides general education and is not a substitute for care from your child’s clinician. If you are worried, it is always appropriate to call and be seen.