Cellulitis in Kids: Warm Red Skin and Fever
Sarah Mitchell
Sarah Mitchell is a Registered Pediatric Nurse and a mother of three who has spent over a decade helping families navigate the beautiful, chaotic early years of childhood. She combines evidence-based medical knowledge with real-world parenting experience to offer practical, compassionate advice. At Awesome Parent, Sarah's mission is to help exhausted parents find solutions, trust their instincts, and finally get some sleep.
If you’re staring at a patch of red, warm skin on your child at 2 AM, you are not alone. I talked to parents about this daily as a pediatric triage nurse, and now I’ve had my own share of “Is this just a bite or something bigger?” moments with my kids.
Cellulitis is a bacterial skin infection that can spread beyond the original scratch, bite, or irritation. The good news is that most kids do very well with quick, appropriate treatment. The important part is knowing when to watch, when to call the pediatrician today, and when to go to the ER now.
What cellulitis looks like
Cellulitis usually starts when bacteria enter through a tiny break in the skin, sometimes so small you never noticed it. Common germs include Group A strep and Staph aureus.
Common signs
- Redness that spreads over hours to a day, rather than staying the same size
- Warmth compared with nearby skin
- Swelling and tenderness or pain
- Skin that looks tight or shiny
- Fever, chills, or your child just seems “off”
- Red streaking traveling away from the area (often needs urgent same-day evaluation)
- Swollen lymph nodes near the area (for example, groin nodes with a leg infection)
On lighter skin tones, cellulitis often looks bright pink or red. On deeper skin tones, it can look more purple, brownish, or like an area of darkened skin. In any skin tone, the combination of spreading, warmth, and tenderness is a big clue.
Cellulitis vs a bug bite
Bug bites can look dramatic, especially in kids who have big local reactions. A bite can be red and swollen and still not be infected.
More likely a bite reaction
- Very itchy is the main symptom
- A clear central bite mark or small bump
- Redness that is annoying but not rapidly expanding
- Swelling that’s worst in the first 24 to 48 hours, then slowly improves
- No fever, and your child is otherwise acting normal
More concerning for cellulitis
- Pain or tenderness is more prominent than itch
- Redness keeps expanding beyond the original bite area
- Increasing warmth and swelling over time
- Fever or your child seems unusually tired, fussy, or unwell
One practical tip: if you suspect infection, you can use a pen to lightly mark the edge of the redness and write the time. If the redness clearly grows beyond that line over a few hours, call your child’s clinician for same-day advice.
Cellulitis vs hives
Parents also confuse cellulitis with an allergic rash.
More like hives
- Very itchy welts that can come and go
- Rash that moves or changes shape over minutes to hours
- Often shows up in multiple areas, not just one spot
More like cellulitis
- One main area that is warm, tender, and expanding
- Pain more than itch
- Sometimes fever or feeling unwell
Cellulitis vs impetigo
Impetigo is another common bacterial skin infection in kids, but it usually stays more superficial than cellulitis.
Impetigo often looks like
- Small blisters or pimples that break open
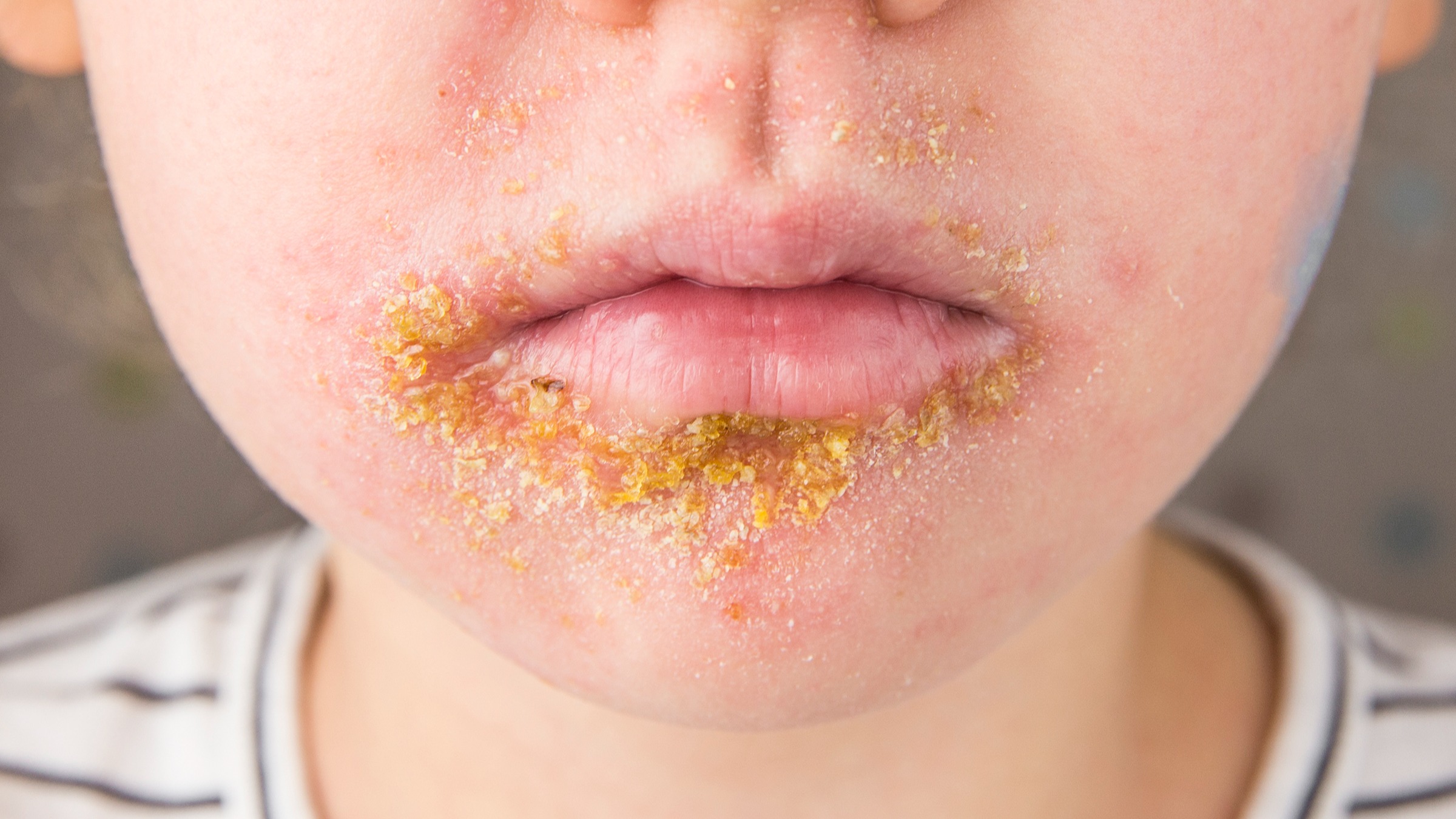
- Honey-colored crusts, especially around the nose and mouth
- Itchiness is common
- Usually minimal swelling and less deep tenderness
Cellulitis is more likely when
- The redness and swelling are deeper and more tender
- There’s increasing warmth and spreading margins
- Fever is present
Common spots in kids
Cellulitis can happen anywhere, but in children I most often saw it in a few predictable places.
- Lower legs and feet (scrapes, insect bites, cuts, athlete’s foot cracks in older kids)
- Arms and hands (playground scrapes, nail picking)
- Face, especially around the nose and cheeks (can start from a small skin break, runny-nose irritation, or impetigo)
- Around a wound or healing abrasion
- After water exposure with an open cut (lakes, pools, hot tubs, ocean). This can change the bacteria involved. Freshwater can involve Aeromonas, salt or brackish water can involve Vibrio, and hot tubs can involve Pseudomonas. Call for same-day medical advice.
If your child has cellulitis on the face or near the eye, take it seriously and seek same-day care. Infections in that area can worsen quickly and sometimes need stronger treatment.
What you can do at home
Home care is supportive, not a cure for true cellulitis. But it can help your child feel better and it can buy time while you arrange prompt medical care.
Helpful steps
- Take a temperature and write it down.
- Circle the border of redness lightly with a pen and note the time.
- Elevate the affected arm or leg when possible to reduce swelling.
- Cool compresses can soothe discomfort.
- Pain control with acetaminophen or ibuprofen if your child can take them safely and you can dose accurately. (In general, avoid ibuprofen in babies under 6 months unless your clinician tells you to use it.)
- Keep nails short and discourage scratching. Scratching can turn a mild bite into a bigger problem.
Please avoid
- Leftover antibiotics or someone else’s prescription
- Cutting, squeezing, or “draining” an area at home
- Topical antibiotic ointment as the only treatment if redness is spreading or the area is clearly warm and tender. Mild skin issues can look similar, but true cellulitis usually needs an oral antibiotic, and sometimes IV antibiotics.
- Steroid cream on a possible infection unless your child’s clinician tells you to use it
If your child has a small, itchy bite with no fever and they are acting normal, it is reasonable to watch closely for 24 hours with the steps above. If it is spreading, painful, or paired with fever, that is a same-day call.
Call today (same-day)
For suspected cellulitis, the safest default is same-day medical advice. Many kids need oral antibiotics, and starting early lowers the chance the infection spreads.
- Redness is spreading or clearly larger than it was earlier
- The area is warm, swollen, and tender
- Your child has fever (especially 100.4°F or higher in a baby under 3 months, which is urgent)
- The infection is on the face, near the eye, on the hand, or near the genitals
- Your child has underlying conditions that affect infection risk (for example, immune suppression) or a history of MRSA
- There is a puncture wound, animal bite, or a cut exposed to lake or ocean water
- Red streaking is present, even if your child seems okay (same-day evaluation is a good idea)
What to expect: your child may be started on an oral antibiotic. Clinicians often choose a medication that covers strep and sometimes staph depending on the appearance and your local resistance patterns. They may outline the area with marker and give you specific return precautions. If there is drainage, they may swab it for a culture. If an abscess is suspected, they may use ultrasound to look for a pocket of pus.
ER now: warning signs
Trust your instincts here. If your child looks seriously ill, it is appropriate to seek emergency care.
Go to the ER now or call emergency services if
- Your child is very sleepy, hard to wake, confused, or you are worried about responsiveness
- Breathing trouble, bluish lips, or signs of severe allergic reaction with swelling of lips or face
- Very fast spreading redness over hours, or sudden worsening pain
- Red streaks plus fever, rapid worsening, or a very ill appearance
- Severe pain out of proportion to what you see on the skin
- Fever with a very ill appearance, shaking chills, or persistent vomiting
- Cellulitis near the eye with swelling, pain with eye movement, or changes in vision
- A baby under 3 months with fever (100.4°F or higher) or a concerning skin infection
- Your child has a known immune system problem and seems worse
These signs can point to infection spreading, dehydration, or (rarely) deeper tissue infections. Rare does not mean never, so if the pain is extreme, the skin is turning dusky or gray, or things are changing quickly, get seen urgently.

When antibiotics help
This is the part that surprises many parents: once antibiotics start, the redness may look the same or slightly worse in the first 24 hours. That can be normal as the body ramps up inflammation while fighting the infection.
Typical timeline
- Within 24 to 48 hours: fever should improve and the area should stop expanding.
- By 48 to 72 hours: redness and tenderness should begin to noticeably improve.
Also normal: the color and swelling can lag behind even when your child feels better. The trend matters.
If your child is getting worse, the redness keeps spreading past your marker line, or fever persists beyond 48 hours on antibiotics, call your clinician urgently. Some kids need a different antibiotic, evaluation for an abscess that needs drainage, or IV medication.
What about an abscess?
Sometimes what looks like cellulitis is actually an abscess, which is a pocket of pus under the skin. Abscesses can occur with or without surrounding cellulitis.
Clues there may be an abscess
- A firm or squishy lump under the red skin
- A visible head or draining fluid
- A central area that is more painful than the rest
Abscesses often need to be evaluated in person. Antibiotics alone may not be enough if there is a collection that needs drainage.
Is cellulitis contagious?
Cellulitis itself is not usually “catchy” through casual contact because the bacteria are inside the skin. That said, the bacteria that cause it can spread through skin-to-skin contact or shared items if there is drainage or open sores.
Simple prevention at home
- Wash hands with soap and water, especially after touching the area or changing bandages.
- Do not share towels, washcloths, razors, or clothing that touches the infected area.
- Keep the area clean and covered if there is any weeping or drainage.
Lower the odds next time
Kids are basically professional scrape collectors, so prevention is about small routines, not perfection.
- Clean cuts and scrapes with soap and water as soon as you notice them.
- Apply a thin layer of petroleum jelly and cover with a bandage if the wound is open.
- Treat itchy conditions that lead to scratching (eczema, bug bites) and keep nails trimmed.
- Address cracked skin on feet in older kids and teens.
Quick guide
- Looks like a simple bite (itchy, stable size, no fever, acting normal): watch closely for 24 hours, use cool compresses, and consider an antihistamine if your pediatrician has said it is appropriate for your child.
- Possible cellulitis (warmth, tenderness, spreading redness, fever): call for same-day pediatric guidance. Many kids need oral antibiotics.
- Emergency signs (very sick appearance, very rapid spread, severe pain, eye involvement, baby under 3 months with fever): ER now.
If you’re unsure which bucket your child is in, that uncertainty alone is a good reason to call. A calm, quick check from your pediatrician or urgent care can save you a long night of worry, and it can prevent a small infection from becoming a bigger one.
My nurse-mom reminder: You do not need to diagnose cellulitis from a photo in your camera roll at midnight. Your job is to notice the pattern (spreading, warmth, fever, pain) and get your child seen in the right time window.
Sources
- American Academy of Pediatrics (HealthyChildren.org): guidance on skin infections and when to seek care
- Centers for Disease Control and Prevention (CDC): information on staph, MRSA, and skin infection prevention
- Infectious Diseases Society of America (IDSA): clinical guidance on skin and soft tissue infections (for general treatment principles)
This article is for education and cannot replace medical advice from your child’s clinician. If you are worried about your child’s symptoms, seek care.