Chickenpox in Kids: Symptoms, Timeline, and When to Keep Them Home
Sarah Mitchell
Sarah Mitchell is a Registered Pediatric Nurse and a mother of three who has spent over a decade helping families navigate the beautiful, chaotic early years of childhood. She combines evidence-based medical knowledge with real-world parenting experience to offer practical, compassionate advice. At Awesome Parent, Sarah's mission is to help exhausted parents find solutions, trust their instincts, and finally get some sleep.
If you are reading this at 2:47 AM while Googling "red spots turned into blisters", I see you. Chickenpox can look scary, feel miserably itchy, and spread fast in a classroom. The good news is that most healthy kids recover just fine at home with supportive care and a little strategy.
Below, I will walk you through what chickenpox typically looks like, the usual timeline, when your child is contagious, how to keep them comfortable, and the situations where you should call your pediatrician right away.
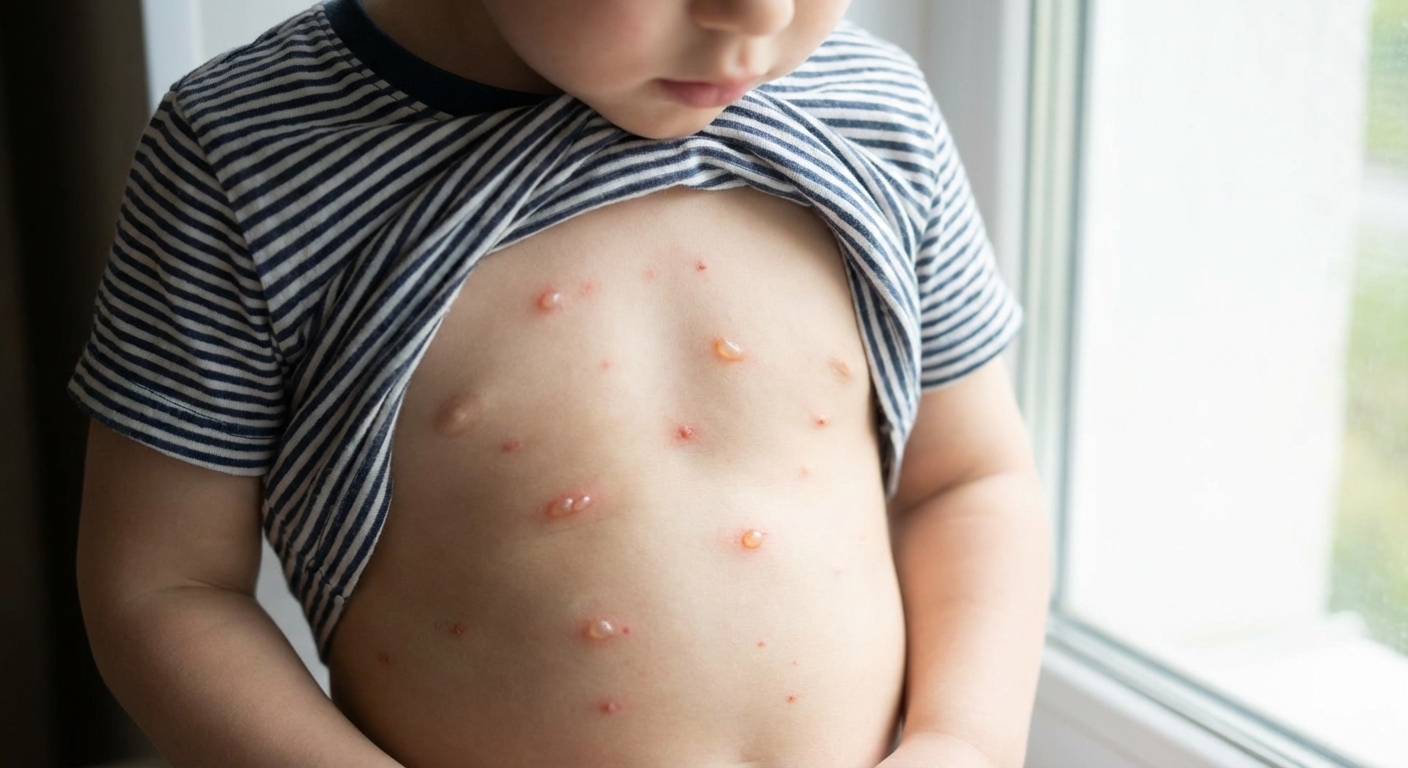
What chickenpox is
Chickenpox is caused by the varicella-zoster virus. It usually starts with mild cold-like symptoms and then a very characteristic itchy rash that comes in waves.
Most kids in the United States are vaccinated, so chickenpox is less common than it used to be. But it still happens, especially in unvaccinated children or as a milder breakthrough infection in vaccinated kids.
Chickenpox symptoms
Early symptoms (often 1 to 2 days before the rash)
- Fever (often low-grade, but can be higher)
- Tiredness, irritability
- Headache
- Decreased appetite
- Sore throat or mild cough in some kids
The chickenpox rash (the classic symptom)
The chickenpox rash is famous for two things:
- It is intensely itchy.
- It appears in multiple stages at once, meaning you can see new red spots, fluid-filled blisters, and scabs all on the same day.

Rash stages
Chickenpox lesions usually move through a predictable set of stages. The timing can vary, but the pattern is consistent.
1) Red spots (macules and papules)
It often starts as small red spots or slightly raised bumps. Many parents initially think it is bug bites, heat rash, or eczema flaring.
2) Blisters (vesicles)
Within about a day, many spots turn into tiny fluid-filled blisters that can look like little dew drops. This is when itching tends to ramp up.
3) Cloudy blisters, then crusting
The blisters can get a bit cloudy, then break or dry out and form scabs (crusts).
4) Scabs fall off
Scabs typically fall off on their own. Try not to pick them. Picking increases the risk of scarring and skin infection.
Nurse-mom tip: Chickenpox comes in waves for several days, so it is normal to see new red bumps even after some spots have already scabbed.
Timeline
Here is the typical timeline most families experience.
After exposure
- Incubation period: Usually 10 to 21 days from exposure to symptoms, most commonly around 14 to 16 days.
- Your child will look and act normal during most of this time.
When symptoms start
- Day 0 to 1: Fever, fatigue, not themselves.
- Day 1 to 5: Rash appears and continues to crop up in new waves for about 3 to 5 days. Some kids keep getting new spots a bit longer.
- Day 5 to 7: Many lesions are drying and crusting over.
- By about 7 to 10 days after rash starts: Many kids are feeling much better, and scabs are present.
Full skin healing can take longer, especially if your child scratches a lot. The main milestone for ending isolation is not “the rash looks better.” It is “no new lesions, and all lesions are crusted or clearly dry.”
When it is contagious
This is the part that matters most for school, daycare, and siblings.
Contagious period
- Classic chickenpox: Contagious from about 1 to 2 days before the rash appears until all lesions have crusted over.
- Breakthrough chickenpox (after vaccination): Lesions may not fully blister or crust. A practical rule used by many public health and school settings is to consider a child contagious until no new lesions have appeared for 24 hours and all existing lesions are drying or crusted.
How it spreads
- Through the air from coughing and sneezing
- Through direct contact with fluid from blisters
Because it can spread before you know it is chickenpox, classroom outbreaks can happen quickly.
School and daycare
Keep them home if
- They have suspected or confirmed chickenpox and any blisters are not yet crusted (or lesions are not clearly dry)
- They have fever and are not feeling well enough to participate
- They cannot stop scratching enough to keep lesions clean
They can go back when
- No new lesions for 24 hours
- All lesions are crusted or clearly dry (no wet blisters)
- They are fever-free for 24 hours without fever-reducing medicine
- They feel well enough for normal activities
For many kids, this ends up being around 5 to 7 days after the rash begins, but some children have new crops longer.
Quick check: If you still see shiny, fluid-looking spots, your child is not ready to return yet.
Home care
Chickenpox care is mostly about keeping your child comfortable and preventing skin infection from scratching.
Fever management
- Use acetaminophen (Tylenol) as directed for your child’s age and weight.
- Avoid aspirin in children with viral illnesses due to the risk of Reye syndrome.
- Ibuprofen (Motrin, Advil): Some evidence suggests it may be associated with more severe skin and soft-tissue infections in chickenpox, but guidance and practice vary. When in doubt, use acetaminophen as first choice and follow your pediatrician’s advice.
- Offer fluids often. Fever plus poor appetite can sneak up on hydration.
Itch relief
- Cool or lukewarm baths. Oatmeal baths can help some kids.
- Calamine lotion on itchy spots (avoid eyes and mucous membranes).
- Loose, soft clothing and a cool room temperature.
- Trim nails and consider socks or mittens at night for younger kids who scratch in their sleep.
- Ask your clinician about an oral antihistamine for nighttime itch if your child is miserable.
Skin care to prevent infection
- Keep skin clean and dry.
- Discourage picking scabs.
- Avoid steroid creams on chickenpox lesions unless your clinician specifically tells you to use them.
- Avoid using topical antibiotics on spots unless your clinician recommends them (they can irritate skin and allergies happen).
- Watch for signs a lesion is getting infected: increasing redness, warmth, swelling, pain, pus, or red streaking.

Antiviral treatment
Most healthy children do not need antiviral medication. But in some situations, a clinician may prescribe an antiviral (like acyclovir), especially if it can be started early in the illness. Children who are immunocompromised, very young, or otherwise high-risk may need urgent evaluation and different treatment.
Breakthrough chickenpox
Yes, a vaccinated child can still get chickenpox. This is called breakthrough varicella.
What it usually looks like
- Milder illness overall
- Fewer spots (often fewer than 50, but not always)
- Lower fever or no fever
- Rash may look more like red bumps with fewer classic fluid-filled blisters
Are they contagious?
They can still spread it, especially to unvaccinated people and those with weakened immune systems. In general, keep them home until no new lesions have appeared for 24 hours and all lesions are drying or crusted.
Does this mean the vaccine did not work?
No. The vaccine’s job is to prevent severe disease and complications. Breakthrough infections are typically much easier on kids than classic chickenpox.
Vaccine basics
The chickenpox vaccine (varicella vaccine) is a routine childhood immunization and has dramatically reduced hospitalizations and serious complications.
Typical schedule
- 1st dose: 12 to 15 months
- 2nd dose: 4 to 6 years
If your child was exposed and is not vaccinated
Call your pediatrician promptly. In some cases, getting the varicella vaccine ideally within 3 days (and up to 5 days) after exposure can reduce the chance of illness or make it milder. There are also special preventive options for certain high-risk people after exposure, but those need clinician guidance.
When to call the doctor
Most healthy children can be managed at home, but chickenpox can cause complications. Call your pediatrician if you are unsure. That is what we are here for.
Call urgently if your child has
- Trouble breathing, persistent chest pain, or severe cough
- Severe headache, stiff neck, confusion, extreme sleepiness, trouble walking, or repeated vomiting
- Fever that is high, or fever that returns after improving
- Signs of dehydration: very dry mouth, no tears, much less urine, unusual lethargy
- Rash near or in the eye, or eye redness and pain
- Skin that looks infected: increasing redness, warmth, swelling, tenderness, pus, or red streaks
Call promptly if your child is higher risk
- Younger than 12 months (higher risk and too young for routine vaccination)
- Has a weakened immune system (or takes immune-suppressing medicines)
- Has a chronic skin condition (like severe eczema) that makes infection more likely
- Has chronic lung disease or other significant medical conditions
Call right away if someone in the home is pregnant or immunocompromised
Chickenpox can be much more serious in pregnancy and in people with weakened immune systems. If your child is diagnosed and you have a pregnant household member, a newborn, or an immunocompromised family member, contact a healthcare professional quickly. Some high-risk exposed people may be candidates for a protective antibody product (often called VariZIG), but timing matters and a clinician needs to guide this.
3 AM questions
How do I know it is chickenpox and not hand, foot, and mouth?
Hand, foot, and mouth disease (HFMD) often causes mouth sores and a rash that is common on hands and feet, and it can also involve the diaper area. Chickenpox often starts on the torso and face and spreads outward, with lesions in multiple stages at once. That said, these illnesses can overlap in real life. Chickenpox can involve the scalp or mouth, and HFMD can show up beyond hands and feet. If you are not sure, a quick call or visit can help confirm.
Can my child shower?
Yes. Gentle washing is fine and can reduce the risk of skin infection. Keep water lukewarm and avoid harsh scrubbing.
Will scars happen?
Most spots heal without scarring, especially if you can prevent scratching and picking. Deep scratching and infected lesions are what typically lead to scars.
Checklist
- Assume your child is contagious from 1 to 2 days before rash until no new lesions for 24 hours and all lesions are crusted or clearly dry.
- Keep them home until they meet the same rule above and are fever-free for 24 hours without medicine.
- Use acetaminophen for fever, avoid aspirin, and ask your pediatrician about ibuprofen.
- Focus on itch control: cool baths, calamine, short nails, nighttime itch support.
- Watch closely for skin infection, breathing issues, dehydration, or unusual sleepiness.
- Call your pediatrician for infants, immunocompromised kids, eye involvement, pregnancy in the home, or any red flags.
If you suspect chickenpox, check in with your child’s pediatrician for personalized guidance, especially if your child is very young, has a chronic condition, or anyone in your household is pregnant or immunocompromised.