CMV in Newborns: Screening, Breast Milk, and Next Steps
Sarah Mitchell
Sarah Mitchell is a Registered Pediatric Nurse and a mother of three who has spent over a decade helping families navigate the beautiful, chaotic early years of childhood. She combines evidence-based medical knowledge with real-world parenting experience to offer practical, compassionate advice. At Awesome Parent, Sarah's mission is to help exhausted parents find solutions, trust their instincts, and finally get some sleep.
If you have just heard the words cytomegalovirus or CMV next to your newborn’s name, take a breath. CMV is common, and most babies who are exposed after birth (including through close contact or breast milk) do very well. And even with congenital CMV (infection during pregnancy), most babies are asymptomatic at birth. The tricky part is that the internet tends to treat CMV like a five-alarm fire, when what most families actually need is a clear plan, good follow-up, and a pediatrician who will interpret results in context.
This page will walk you through what CMV is, how screening and testing work in pregnancy and after birth, what “detected” can mean, how breastfeeding fits in, and the symptoms that deserve a prompt call.
What is CMV, and why do doctors talk about it with newborns?
CMV is a very common virus in the herpesvirus family. Many adults have had CMV at some point, often with mild cold-like symptoms or no symptoms at all.
The reason CMV comes up in newborns is simple: CMV can be passed to a baby during pregnancy (congenital CMV). When that happens, most babies still look perfectly healthy. A smaller group may have symptoms at birth or develop certain issues later, most importantly hearing changes.
Key terms you might hear
- Congenital CMV: infection acquired before birth and confirmed by testing within the first few weeks of life.
- Perinatal or postnatal CMV: infection acquired during delivery or after birth, including from close contact or sometimes breast milk. In healthy full-term babies, this is usually mild.
- Primary infection: the pregnant person gets CMV for the first time.
- Reactivation or reinfection: CMV becomes active again in someone who has had it before, or they are infected with a different strain. This can happen without symptoms and can lead to viral shedding.
How babies are screened and tested for CMV
There are two big pathways to diagnosis: prenatal testing (during pregnancy) and newborn testing (after birth). Not every family will need either. Often, testing is prompted by a specific clue.
When CMV testing comes up
- A prenatal ultrasound shows certain findings that can be associated with CMV.
- A pregnant person has a CMV blood test that suggests recent infection.
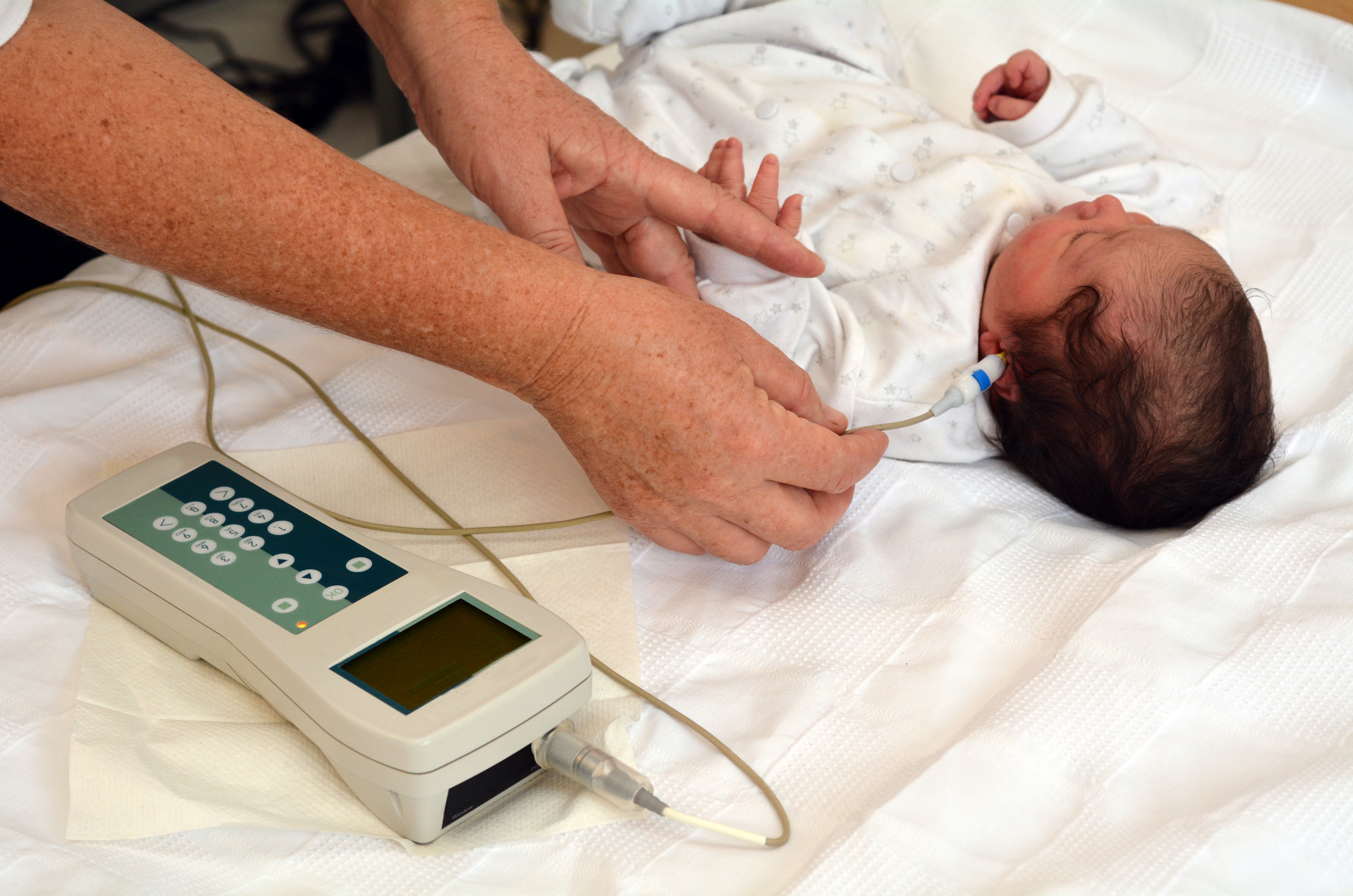
- A newborn fails the initial hearing screen.
- A baby is small for gestational age, has significant or prolonged jaundice, low platelets, or other concerning signs.
- Your state or hospital runs a targeted or universal CMV screening program.
Prenatal ultrasound findings (not specific)
When CMV is suspected in pregnancy, clinicians may pay closer attention to ultrasound findings such as growth restriction, ventriculomegaly, intracranial calcifications, abnormal fluid around organs, or liver and spleen enlargement. These findings are not unique to CMV, but they can be a reason your care team recommends additional testing and follow-up.
Pregnancy blood tests can be tricky
CMV blood work in pregnancy (IgG, IgM) can be hard to interpret, and sometimes additional testing like IgG avidity is used to help estimate timing. If you are told your results suggest a recent infection, it is reasonable to ask whether a maternal-fetal medicine specialist should be involved.
Newborn CMV testing basics (timing matters)
To confirm congenital CMV, testing should be done as early as possible, ideally within the first 21 days of life (many clinicians use this cut-off). That window matters because after a few weeks, it becomes harder to tell whether CMV was acquired during pregnancy or after birth.
Screening means a test that is good at catching possible cases. Confirmation means a follow-up test used to firmly establish the diagnosis.
Common newborn tests include:
- Saliva PCR (screening): a quick, sensitive screening test. Because breast milk can contain CMV, a saliva test is often collected at least 1 hour after feeding (follow your hospital or lab protocol). If saliva is positive, it is commonly confirmed with urine.
- Urine PCR (confirmation): often used to confirm congenital CMV.
- Blood tests: sometimes used as part of the evaluation, but urine and saliva are typically first-line for diagnosis.
If testing was not done in the first 21 days, ask your pediatrician what options exist. In some settings, clinicians may consider dried blood spot PCR from the newborn screening card to retrospectively support congenital infection, but availability and sensitivity vary.

What “CMV detected” can mean
Seeing “detected” on a lab result is a gut-punch. Here is the calm interpretation:
- “Detected” means the test found CMV genetic material in that sample. It does not automatically tell you when the baby acquired it or whether it will cause long-term problems.
- A positive saliva test often needs confirmation (commonly with urine PCR), especially if the baby is breastfeeding.
- Timing and sample type matter. A positive urine or saliva PCR in the first 21 days supports congenital CMV. A positive test later can represent postnatal infection.
- Many babies with congenital CMV have no symptoms and never develop problems. The main reason follow-up matters is to monitor hearing and development.
CMV “infection” vs CMV disease
Clinicians often talk about whether a baby is asymptomatic (no signs of disease) or symptomatic (signs like small head size, rash, liver issues, low platelets, or hearing concerns). That distinction influences how urgently specialists are involved and whether antiviral treatment is considered.
Breast milk and CMV
This is the part that tends to spiral parents in the middle of the night, so let’s keep it grounded.
CMV can be present in breast milk. Postnatal transmission through milk is more common when a parent is CMV-seropositive and has viral shedding, often related to reactivation or reinfection. In most healthy, full-term babies, postnatal CMV from breast milk is typically mild or even silent.
Should you stop breastfeeding?
In most cases, no. Breastfeeding has significant benefits, and for most full-term babies, those benefits outweigh the CMV risk. Where the conversation gets more nuanced is with:
- Very premature infants (especially extremely preterm) or babies with very low birth weight
- Medically fragile infants or those with certain immune concerns
In NICU settings, you may hear options like freezing and thawing milk, heat treatment, or using pasteurized donor milk in certain situations. Those decisions are individualized and usually guided by neonatology.
A practical note about saliva testing
If your baby has a saliva CMV test, ask whether there were instructions to collect it at least 1 hour after feeding (or per your lab protocol). This helps reduce the chance that CMV from milk in the mouth confuses the result. If the test is positive, it is common to confirm with a urine PCR.

Symptoms and red flags
Many newborns with CMV look completely normal, especially at first. Still, it helps to know what deserves a call.
Call your pediatrician promptly if your newborn has:
- Yellowing of the skin or eyes that seems significant, is worsening, or lasts longer than expected
- Poor feeding, very sleepy behavior, or difficulty waking for feeds
- Fever (in babies under 3 months, any fever needs urgent guidance)
- Unusual bruising or tiny red or purple spots on the skin (petechiae)
- Breathing trouble
- Repeated forceful vomiting (not typical small spit-up) or signs of dehydration (very few wet diapers)
- Seizure-like activity or abnormal movements
Longer-term: hearing and development
The most important follow-up for many babies with congenital CMV is hearing monitoring. Congenital CMV related hearing loss can be present at birth, late-onset, or progressive (worsening over time). That is why your pediatrician may recommend repeat hearing tests even if the first one looks okay.

What happens after a positive or suspected CMV test?
The next steps depend on your baby’s age, symptoms, and test results. Your pediatrician may recommend some combination of:
- Confirmatory testing (often urine PCR if saliva was positive)
- Repeat hearing evaluation or referral to pediatric audiology
- Blood work to check liver enzymes and platelet counts if there are concerns
- Imaging (sometimes a head ultrasound or other studies) if the baby is symptomatic or there are prenatal findings
- Eye exam (ophthalmology) in some cases, because congenital CMV can affect the retina
- Referral to pediatric infectious disease, neurology, audiology, and early intervention or developmental specialists as needed
A simple follow-up roadmap (general)
Every plan is individualized, but many families are guided by a straightforward rhythm: confirm diagnosis early when possible, assess hearing, consider vision screening, and keep developmental check-ins on the calendar. If congenital CMV is confirmed, ask your pediatrician to write down the hearing schedule and which specialists (if any) should be seen in the first year.
Antiviral treatment
Some babies with symptomatic congenital CMV may be considered for antiviral medication, most commonly valganciclovir (oral) or ganciclovir (IV). This is a specialist-guided decision because it depends on the baby’s specific presentation and because antivirals require careful monitoring (including blood counts).
Treatment is typically considered for moderate to severe symptomatic congenital CMV and in some guidance may be discussed for certain cases involving hearing loss. Antivirals are not routinely used for postnatal CMV in healthy term infants. If you are offered this option, it is appropriate to ask about benefits, risks, monitoring labs, timing, and what outcomes the treatment is meant to improve.
Questions to ask your pediatrician
If your brain feels like scrambled eggs, you are not alone. Here are questions that tend to get families the clearest plan:
- Was my baby tested within the first 21 days? If not, how does that affect what we can conclude?
- Which test was positive? Saliva, urine, blood, or something else?
- Was this a screening test or a confirmatory test? Do we need confirmatory urine testing?
- Is my baby considered symptomatic or asymptomatic? What signs are you basing that on?
- What follow-up hearing schedule do you recommend? When is the next hearing test?
- Do we need an eye exam? If yes, when?
- Do we need any blood work or imaging? What are you looking for?
- Should we see pediatric infectious disease? If yes, how soon?
- Are there any breastfeeding changes you recommend for our situation? (Especially if your baby was premature or in the NICU.)
- What symptoms should make us call the same day? And what would be an emergency?
Why you may be hearing about CMV more often
Some states and hospital systems have started universal or more robust targeted newborn CMV screening (often tied to hearing screen results), and legislation around newborn CMV screening has been a growing trend. This is one reason families may suddenly hear “CMV test” even when a baby looks healthy.
How CMV spreads and simple prevention
CMV is often spread through close contact with body fluids, and toddlers are famous for sharing theirs generously. If you are pregnant now or may be pregnant in the future, simple habits can reduce risk:
- Wash hands after diaper changes, wiping noses, or handling pacifiers
- Avoid sharing utensils, cups, or toothbrushes with young children
- Try to kiss little ones on the forehead instead of the lips when you are pregnant
These steps are not about fear. They are about stacking the odds in your favor during pregnancy, especially if you spend a lot of time around toddlers.
What about a CMV vaccine?
There is no CMV vaccine available at this time, so prevention relies on practical hygiene and risk reduction, plus appropriate testing when there is a reason to look.
A final, reassuring note
CMV sounds scary because it is unfamiliar, not because every positive test equals a bad outcome. Most babies are okay, and for the babies who do need closer follow-up, having the right testing and a clear monitoring plan makes a real difference.
If you have results in hand and you are not sure what they mean, bring them to your pediatrician and ask for a step-by-step interpretation: what we know, what we do not know yet, and what happens next. That is the path out of Google panic and into an actual plan.