Cold Sores in Kids: Contagiousness and Treatment
Sarah Mitchell
Sarah Mitchell is a Registered Pediatric Nurse and a mother of three who has spent over a decade helping families navigate the beautiful, chaotic early years of childhood. She combines evidence-based medical knowledge with real-world parenting experience to offer practical, compassionate advice. At Awesome Parent, Sarah's mission is to help exhausted parents find solutions, trust their instincts, and finally get some sleep.
If you just noticed a little cluster of blisters on your child’s lip, you are probably having two thoughts at the same time: Is this a cold sore? and Is everyone else about to get it? Take a breath. Cold sores are extremely common in childhood, and while they are contagious, there are clear, practical ways to lower the spread and help your kid feel better.
As a pediatric nurse and a mom of three, I have seen the whole spectrum, from “Is this acne?” to “My preschooler kissed the baby, what now?” Let’s walk through what’s going on, what to do today, and when it’s worth calling your pediatrician.

What cold sores are
Most cold sores are caused by herpes simplex virus type 1 (HSV-1). Once a child is infected, the virus stays in the body and can “wake up” later, causing future cold sores.
How HSV-1 spreads
HSV-1 spreads through direct contact with saliva or the sore itself. In real life, that usually looks like:
- Kissing (hello, well-meaning relatives)
- Sharing cups, water bottles, straws, utensils, lip balm, toothbrushes
- Sharing pacifiers, teethers, or anything that goes in a baby’s mouth
- Touching the sore and then touching someone else (or shared toys)
- Close face contact and kissing between older kids and teens
Many kids catch HSV-1 from someone who does not have an obvious blister at the moment. The virus can still shed from the mouth even when the skin looks normal, especially around an outbreak.
First infection vs. repeats
A child’s first HSV-1 infection can be subtle, or it can be more intense. Some kids get a single cold sore. Others get gingivostomatitis, which is a mouth-wide outbreak that can include fever, swollen or bleeding gums, lots of drool, and painful sores that make kids refuse to eat or drink.
Later outbreaks tend to be more predictable: tingling, then a blister, then a scab, then healing. Stress, illness, sun exposure, chapped lips, and poor sleep can all trigger flare-ups.
Stages (what you will see)
Cold sores often follow a consistent pattern. Knowing the stages helps you understand when it is most contagious and when treatments are most helpful.
Typical stages
- Prodrome (hours to 1 day): tingling, itching, burning, or “my lip feels weird.” Skin may look normal.
- Blister stage (often 1 to 2 days): small fluid-filled blisters, often in a cluster, usually on the lip edge.
- Weeping/ulcer stage (often 2 to 4 days): blisters pop and ooze. This is often the most contagious stage.
- Crusting/scab stage (often 2 to 4 days): a crust forms. Cracking and bleeding can happen, especially if the area gets dry.
- Healing (several days): scab falls off and skin returns to normal. Total time is often 7 to 14 days, but it can vary. First infections can last longer and feel more intense.
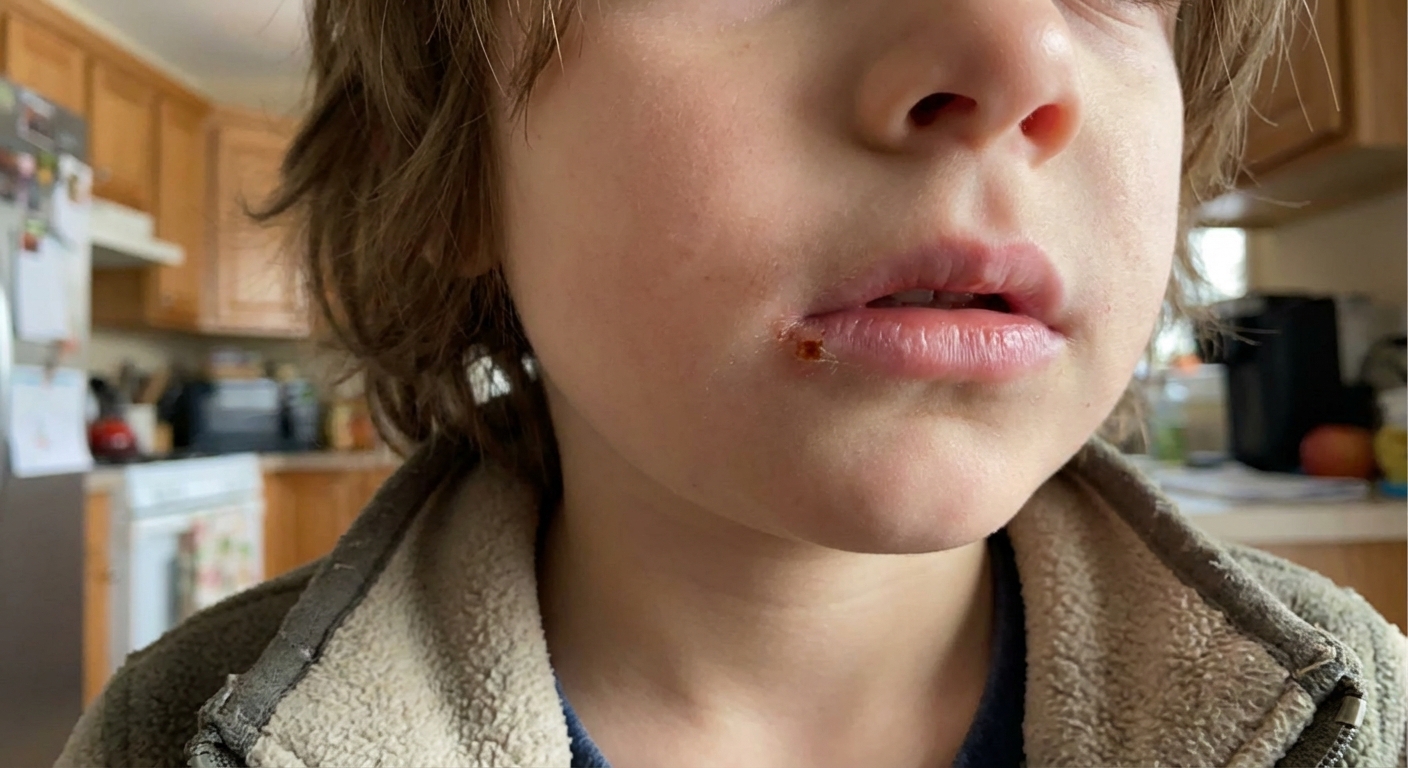
Are they contagious?
Yes. Cold sores are most contagious before you can see them (during tingling) and while there are open or oozing sores. Risk usually drops once the skin is fully healed, but it is worth remembering that HSV can sometimes shed even when the skin looks normal. That means you can lower risk a lot, but you cannot reduce it to zero.
When is it most contagious?
- Highest risk: from the tingling stage through the blister and weeping stages
- Still a risk: during scabbing, especially if the scab cracks or is picked
- Lower risk: once the skin is completely healed with no scab and no open areas (while keeping in mind occasional asymptomatic shedding can still happen)
If you want a simple rule that works in real life: If it is wet, open, or scabby, treat it as contagious.
School and daycare
In most cases, kids do not need to stay home for a typical cold sore if they feel well enough to participate, can keep hands off the sore, and are able to follow basic hygiene (hand washing, no sharing drinks).
Consider keeping your child home or calling your pediatrician for guidance if:
- Your child is very young and cannot stop touching the sore
- There is a lot of drooling (common with first infections)
- Your child has fever, widespread mouth sores, or seems dehydrated
- Your child has eczema with rapidly spreading painful lesions (possible eczema herpeticum)
- Your child cannot reliably avoid close contact (for example, constant mouthing of toys)
Also, many child care centers have their own policies, and some may exclude if lesions cannot be covered or hygiene cannot be maintained. When in doubt, ask the nurse or director what they require.
Safe at-home care
Most cold sores in healthy kids get better on their own. Treatment is about comfort, preventing cracking, and sometimes shortening the outbreak if you catch it early.
Comfort that actually helps
- Cool compress: a clean, cool washcloth held on the area for a few minutes can reduce pain and swelling.
- Petroleum jelly: a thin layer can keep the sore from cracking and can make eating less miserable.
- Hydration: cold drinks, smoothies, or popsicles can be easier than warm foods.
- Pain relief (if needed): acetaminophen or ibuprofen can help. Use age-appropriate dosing from your child’s clinician or the label.
- Do not use aspirin in children unless your clinician specifically instructs you.
OTC antiviral creams
Parents often ask about creams like docosanol (commonly sold as Abreva). Here is the honest, non-judgy truth:
- They work best if started very early, ideally at the tingling stage.
- In studies (mostly in adults), benefit is usually modest, often shortening symptoms by about a day. Evidence in children is less certain, and many products have age restrictions.
- Always follow the product’s age label and your pediatrician’s guidance.
If your child is little and everything ends up in their mouth, sticking with petroleum jelly and comfort measures is often the safest move.
What to avoid
- Topical numbing gels in young kids: products with benzocaine can be risky in infants and young children and are not recommended for teething. Ask your pediatrician before using them for mouth pain.
- Picking the scab: it increases spread, bleeding, and the chance of bacterial infection.
- “Essential oil” remedies: many can irritate skin and do not have strong safety data for kids.
- Topical steroids on the sore: can worsen viral infections unless specifically directed by a clinician.

When antivirals help
Prescription antivirals (like acyclovir or valacyclovir) can help most when started early. They are not necessary for every cold sore, but they can be a big deal in certain situations.
Call your pediatrician promptly if:
- This looks like a first outbreak and your child has fever, significant mouth pain, or multiple sores
- Your child is not drinking, has fewer wet diapers, or shows signs of dehydration (dry mouth, no tears, very sleepy)
- The cold sore is in a child with a weakened immune system
- Your child has eczema and suddenly develops many painful, similar-looking blisters (especially with fever)
- The sore is near the eye or your child has eye redness, eye pain, light sensitivity, or drainage
- Outbreaks are frequent or severe and you want a prevention plan
Why timing matters
Antivirals work best in the first 24 to 48 hours of symptoms. If you call when the sore is already fully scabbed, your clinician may focus on comfort care instead.
Do we need testing?
Usually, no. Cold sores are often diagnosed clinically (by appearance and history). A swab test may be considered if the rash is atypical, severe, near the eye, not improving as expected, or if your child is immunocompromised.
How to prevent spread
You cannot bubble-wrap a kid through a cold sore. You can reduce spread with a few high-impact habits.
At home
- No sharing cups, utensils, straws, toothbrushes, washcloths, towels, lip balm
- No sharing pacifiers, teethers, or anything that goes in the mouth
- Hand washing after touching the face, applying ointment, or wiping drool
- Use a cotton swab to apply petroleum jelly so you are not contaminating the container
- Separate towels for the child with the sore
- Avoid kissing the baby or siblings until the skin is healed
At school or daycare
- Send your child with their own labeled water bottle if allowed
- Remind older kids: “Hands off the sore” and wash hands before snack time
- If your child plays contact sports (wrestling is a classic risk), ask the coach about return-to-play rules and covering lesions
Preventing spread on their own body
HSV-1 can spread from the mouth to other areas, especially during the first infection.
- Eyes: avoid rubbing. Eye symptoms need same-day medical advice.
- Fingers (herpetic whitlow): painful blisters on a finger can happen, often in thumb-suckers. Call your pediatrician if you see this.

Look-alikes
Because kids are tiny chaos magnets, not every lip spot is HSV-1. A few common look-alikes:
- Canker sores: inside the mouth on the cheek or gum, not usually on the outer lip, not contagious.
- Impetigo: honey-colored crusts around the mouth or nose, very contagious bacterial infection, needs medical treatment.
- Chapped lips: cracks without a cluster of blisters.
- Hand, foot, and mouth disease: mouth sores plus rash on hands and feet, common in daycare.
One tricky point: cold sores can also form a yellowish crust as they heal. If you are not sure whether you are looking at a cold sore, impetigo, or both, take a clear photo in good light and message your pediatrician. It is one of the easiest ways for us to triage quickly.
When to seek urgent care
Most cold sores are uncomfortable but not dangerous. Get urgent medical advice if your child has:
- Signs of dehydration or cannot keep fluids down
- Eye pain, red eye, light sensitivity, or a sore on the eyelid
- Rapidly spreading blisters, especially with eczema
- Severe headache, stiff neck, confusion, or a very ill appearance
- A newborn in the home exposed to someone with an active cold sore (call your pediatrician immediately for guidance)
Quick FAQs
Can my child get cold sores from sharing toys?
It is less common than direct kissing or sharing cups and utensils, but it is possible if toys are wet with saliva and another child puts them in their mouth soon after. Good hand hygiene and not sharing mouth items are the biggest wins.
How long does a cold sore last in kids?
Often 7 to 14 days. First infections can last longer and feel more intense.
Is HSV-1 the same thing as genital herpes?
HSV-1 most often causes oral cold sores. HSV-2 more often causes genital herpes, but either type can infect either area. For children, the typical concern is oral HSV-1.
Will my child have cold sores forever?
The virus stays in the body, but not every child gets frequent recurrences. Many kids have occasional outbreaks that get less frequent over time.
A calm next step
If your child has a small, typical cold sore and feels okay, focus on comfort care, keep lips protected with petroleum jelly, and tighten up the “no sharing” rules for a week or two. Avoid direct contact with the sore until the skin is healed, and remember that occasional silent shedding can still happen. If this is a first outbreak, your child is miserable, the sore is near the eye, or hydration is a concern, call your pediatrician early. You are not overreacting. You are parenting.
Parenting-at-3-AM tip: If you are unsure whether it is a cold sore or impetigo, snap a photo now in good light. Things always look different (and usually worse) in the morning.