Common Baby Rashes: What’s Normal and What’s Not
Sarah Mitchell
Sarah Mitchell is a Registered Pediatric Nurse and a mother of three who has spent over a decade helping families navigate the beautiful, chaotic early years of childhood. She combines evidence-based medical knowledge with real-world parenting experience to offer practical, compassionate advice. At Awesome Parent, Sarah's mission is to help exhausted parents find solutions, trust their instincts, and finally get some sleep.
If you have ever looked at your baby’s skin at 2 AM and thought, Was that bump there earlier? you are in very good company. Baby skin is sensitive, brand new to the world, and prone to rashes that look dramatic but are often harmless.
This guide covers six of the most common rashes parents Google in a panic: heat rash, baby acne, milia, contact dermatitis, hives, and fifth disease. I will walk you through what each one typically looks like, why it happens, what you can do at home, and the clear signs it is time to call the doctor.
Quick note on scope: This article focuses on these six, but babies also commonly get diaper rash, eczema (atopic dermatitis), cradle cap (seborrheic dermatitis), hand-foot-and-mouth disease, and infections like impetigo. Many rashes overlap, so if you are unsure, a photo plus a quick call to your pediatrician can save a lot of stress.
Quick safety check
Most rashes are not emergencies. But a few situations deserve quick medical attention.
Call 911 or seek emergency care now if
- Your baby is having trouble breathing, wheezing, or persistent coughing with the rash.
- There is swelling of the lips, tongue, or face.
- Your baby seems very sleepy, hard to wake, limp, or severely ill.
- The rash is purple or looks like bruising and does not blanch (does not turn white) when you press a clear glass against it.
Call your pediatrician today if
- Your baby is under 3 months and has a fever (many clinics use 100.4°F or 38°C rectal). In young infants, fever is usually urgent. Call for guidance rather than giving fever medicine first unless your clinician has already told you to.
- The rash is spreading quickly, very painful, oozing, or crusting.
- You see blisters, especially around the mouth, eyes, or diaper area.
- Your baby is not feeding well, has fewer wet diapers, or seems uncomfortable in a way that worries you.
- You suspect a medication reaction.
If your baby looks well overall, is feeding, and the rash is mild, you usually have time to observe and use gentle home care.
Heat rash (miliaria)
Heat rash is one of the most common “surprise” rashes in babies, especially in warm weather or when they are bundled a little too enthusiastically (we have all done it).
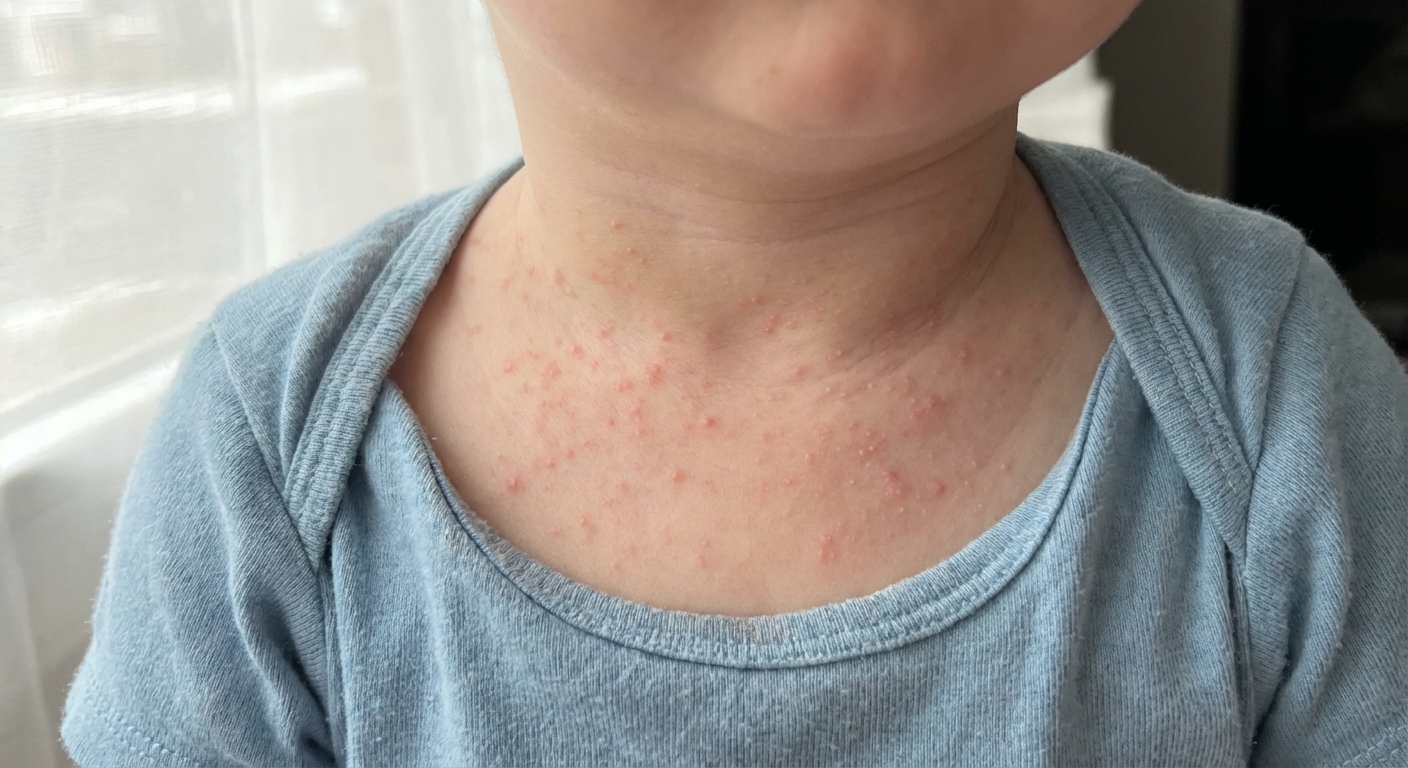
What it looks like
- Clusters of tiny red or pink bumps, sometimes like pinpricks.
- Can look like rough or sandpapery skin.
- Often in skin folds: neck, armpits, chest, back, groin, or under the diaper waistband.
What causes it
Sweat ducts get blocked easily in babies. Trapped sweat irritates the skin, especially in warm, humid conditions or when clothing is tight.
What you can do at home
- Cool the skin down: move to a cooler room, use a fan at a distance, and dress baby in breathable layers.
- Keep it dry: gentle patting after baths can help.
- Skip thick, greasy layers while it is active. Heavy ointments can trap heat and sweat. If friction is a problem (like in a neck fold), a very thin layer of a simple barrier can help, but cooling and drying still come first.
- Short, lukewarm baths can help, then pat dry.
- Choose loose cotton clothing.
When to call the doctor
- If it is not improving after 2 to 3 days of cooling measures.
- If the bumps become pustules (whiteheads), ooze, or the area becomes very tender, which can suggest infection.
- If your baby also has fever or seems unwell.
Baby acne (neonatal acne)
Baby acne is incredibly common and tends to show up right when you are hoping for those perfect newborn photos. Of course it does.
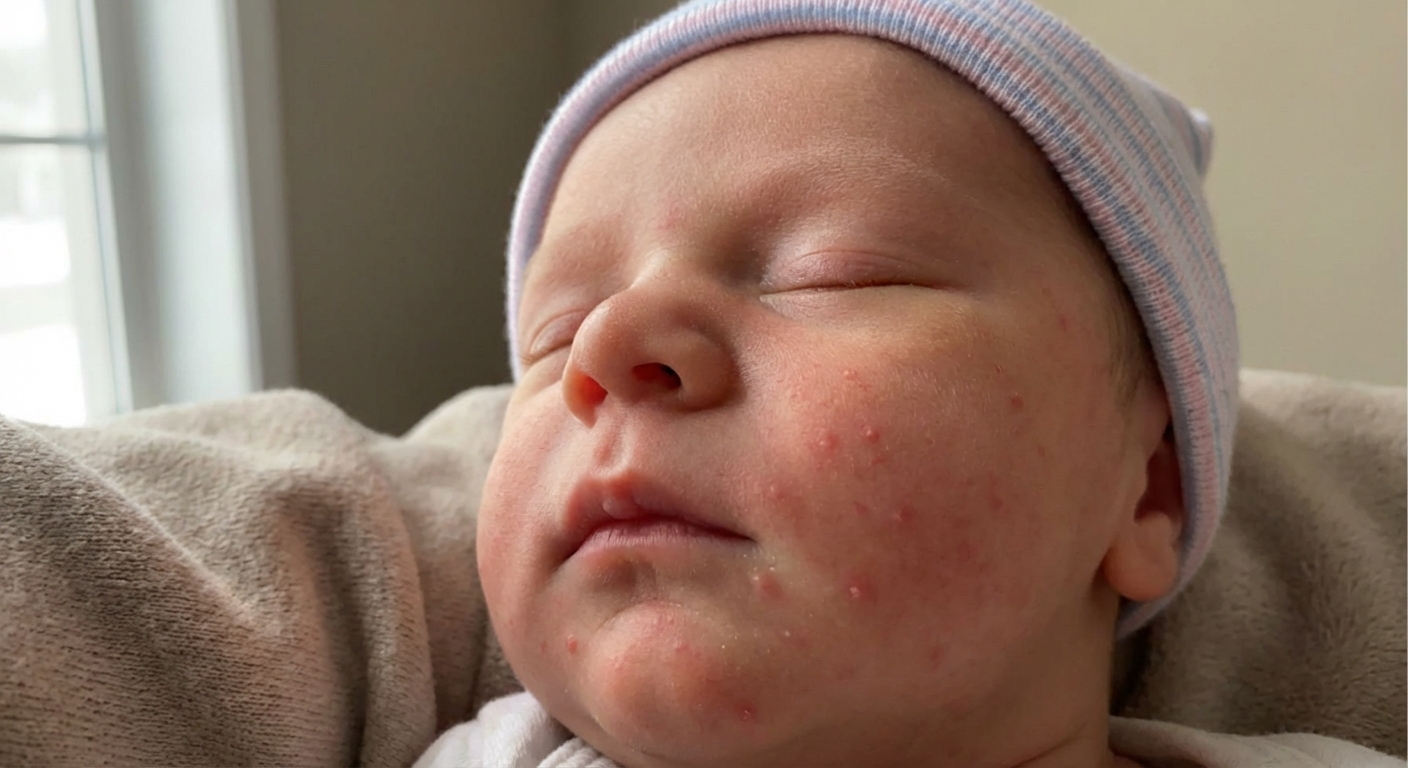
What it looks like
- Small red bumps and sometimes tiny pimples.
- Usually on the cheeks, chin, and forehead.
- Often starts in the first few weeks of life and can come and go.
What causes it
The exact cause is not always clear. It is thought to be related to hormones (from pregnancy) and normal skin changes. It is not from poor hygiene.
What you can do at home
- Keep it simple: wash gently with water (or a mild, fragrance-free baby cleanser) once a day.
- Avoid picking or scrubbing. Baby skin is delicate and irritation makes it worse.
- Skip acne products unless your pediatrician specifically recommends something. Do not use benzoyl peroxide or salicylic acid on a newborn unless you have explicit medical guidance.
- Avoid oily lotions on the affected area if they seem to clog things up.
When to call the doctor
- If the rash is spreading beyond the face or looks very inflamed.
- If you see honey-colored crusting, which can suggest a skin infection (often called impetigo).
- If you are unsure whether it is acne or something else, especially with fever or poor feeding.
Milia
Milia are those tiny white dots that make parents squint and wonder if their baby has “whiteheads.” They are normal and temporary.
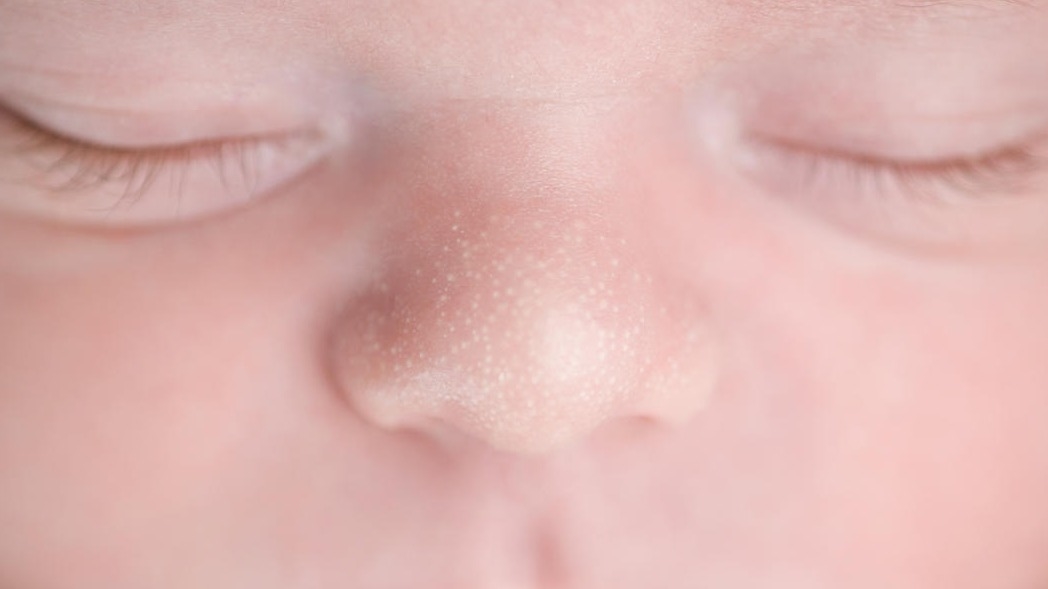
What it looks like
- Very small white or yellow-white bumps.
- Common on the nose, cheeks, and sometimes the forehead.
- Not red, not itchy, not oozing.
What causes it
Milia are tiny trapped keratin cysts. Basically, baby skin is learning how to exfoliate.
What you can do at home
- Do nothing is the correct answer most of the time.
- Wash gently and avoid heavy oils over the area.
- Do not squeeze them. They resolve on their own, usually within a few weeks.
When to call the doctor
- If the bumps become red, swollen, or start draining.
- If they persist for months and you want a quick confirmation at a routine visit.
Contact dermatitis
Contact dermatitis is irritation or allergy from something touching the skin. In baby life, “something” can be soap, drool, wipes, detergent, a new outfit, or even that adorable fuzzy blanket from grandma.
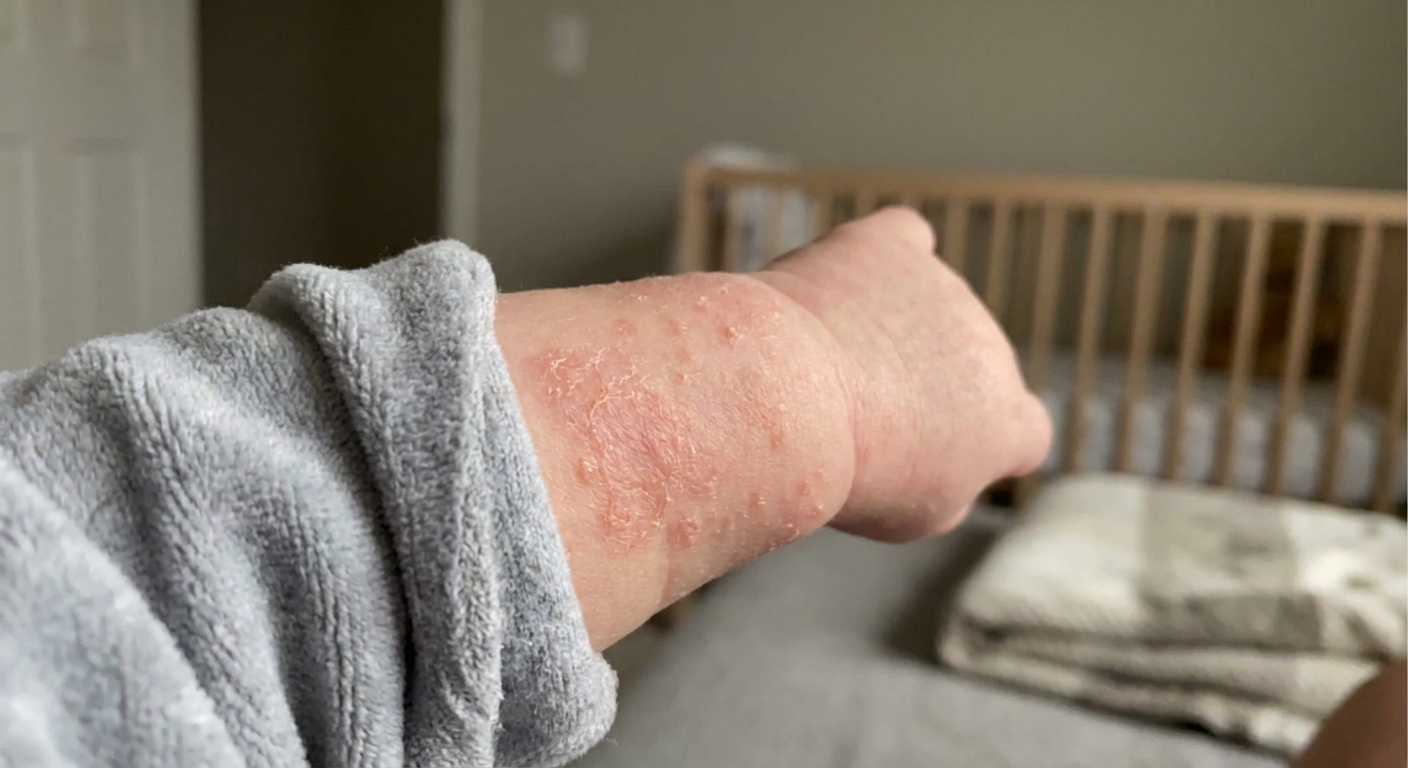
What it looks like
- Red, patchy areas that can look dry or slightly scaly.
- May be itchy (baby may rub their face on you or seem fussy).
- Often appears in a pattern that matches exposure, like around the mouth (drool), on hands (wipes), or along clothing seams.
What causes it
- Irritant contact dermatitis: saliva, urine, stool, soaps, wipes, fragrance, rough fabrics.
- Allergic contact dermatitis: less common in young infants but possible (fragrance, preservatives, topical products).
What you can do at home
- Remove the trigger if you can identify it. Switch to fragrance-free detergent and gentle, dye-free products.
- For drool rash: gently pat dry and use a thin layer of barrier ointment (like petroleum jelly) before feeds or sleep.
- Moisturize with a fragrance-free cream after bathing.
- Keep baths short and lukewarm, and avoid bubble baths.
- Skip steroid creams unless advised. Over-the-counter hydrocortisone is sometimes used in older children, but for infants you should ask first, especially on the face or near the eyes.
When to call the doctor
- If the rash is worsening despite avoiding triggers for 3 to 5 days.
- If there is weeping, crusting, or increasing tenderness.
- If the rash is around the eyes or your baby seems very itchy and uncomfortable.
- If you think your baby may need a prescription anti-inflammatory cream.
Hives (urticaria)
Hives can be startling because they show up fast, change shape, and move around. The good news is that most hives in kids are triggered by common viruses and go away.
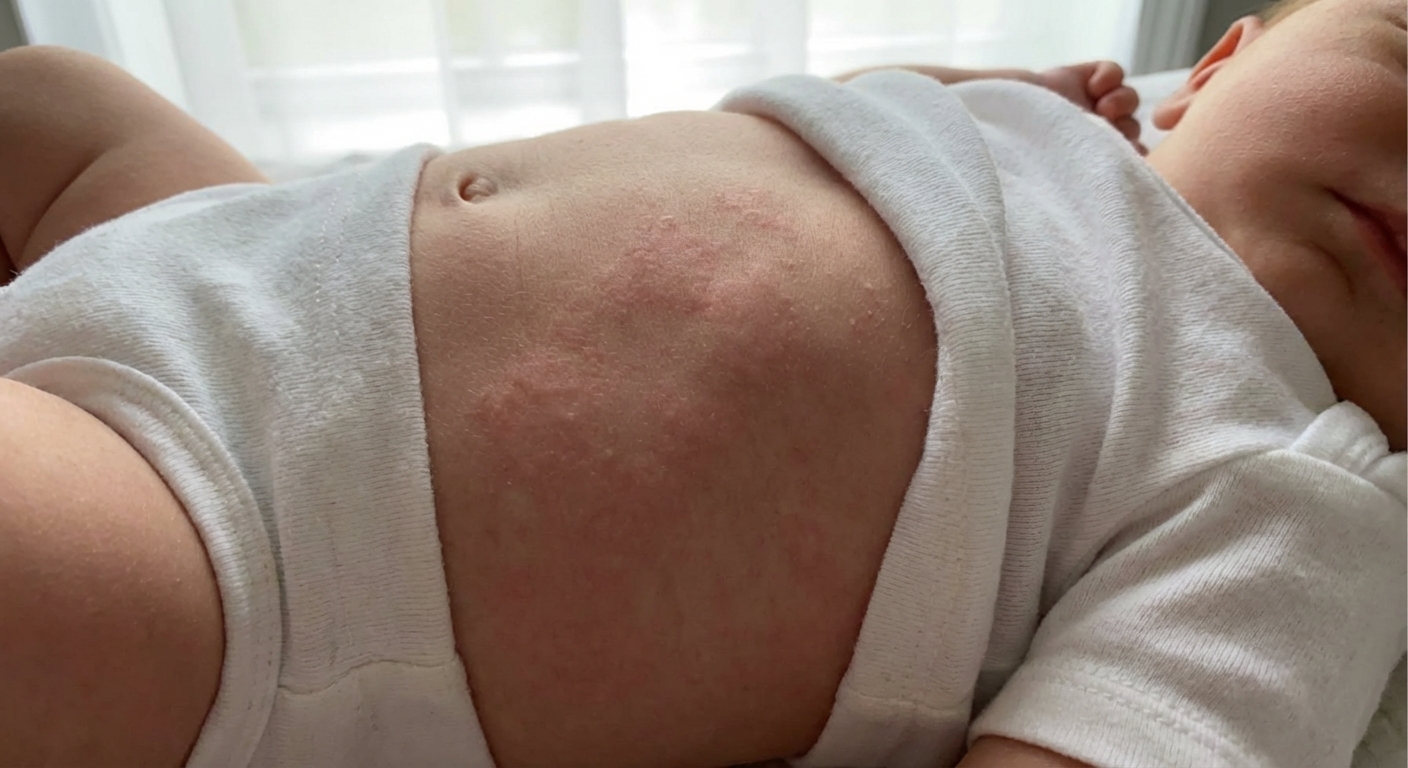
What it looks like
- Raised, puffy welts that are pink or red, often with paler centers.
- They can change location or shape over hours. Individual spots often fade within a day, while new ones can pop up.
- Often itchy.
What causes it
- Viral infections are a very common cause in children.
- Foods, medications, insect bites, or environmental triggers can also do it.
What you can do at home
- Try a cool compress and keep nails short to reduce skin damage from scratching.
- Dress baby in loose, breathable clothing.
- Ask your pediatrician before giving any medication. Some antihistamines are used in infants, but dosing and choice depend on age and weight.
- If you suspect a trigger, stop it and note timing, foods, and new products to discuss with your clinician.
When to call the doctor
- Immediately if hives come with breathing trouble, repeated vomiting, facial swelling, or your baby seems very unwell.
- If hives are severe, your baby is miserable from itching, or you are worried.
- If hives keep coming back or last more than a few days. (Acute outbreaks can linger even if each individual hive fades quickly.)
- If hives started right after a new medication or a new food.
Fifth disease
Fifth disease is a common childhood virus (parvovirus B19). It is most common in preschool and school-aged kids, but babies can get it too, especially if there are older siblings around. The rash has a very recognizable pattern.
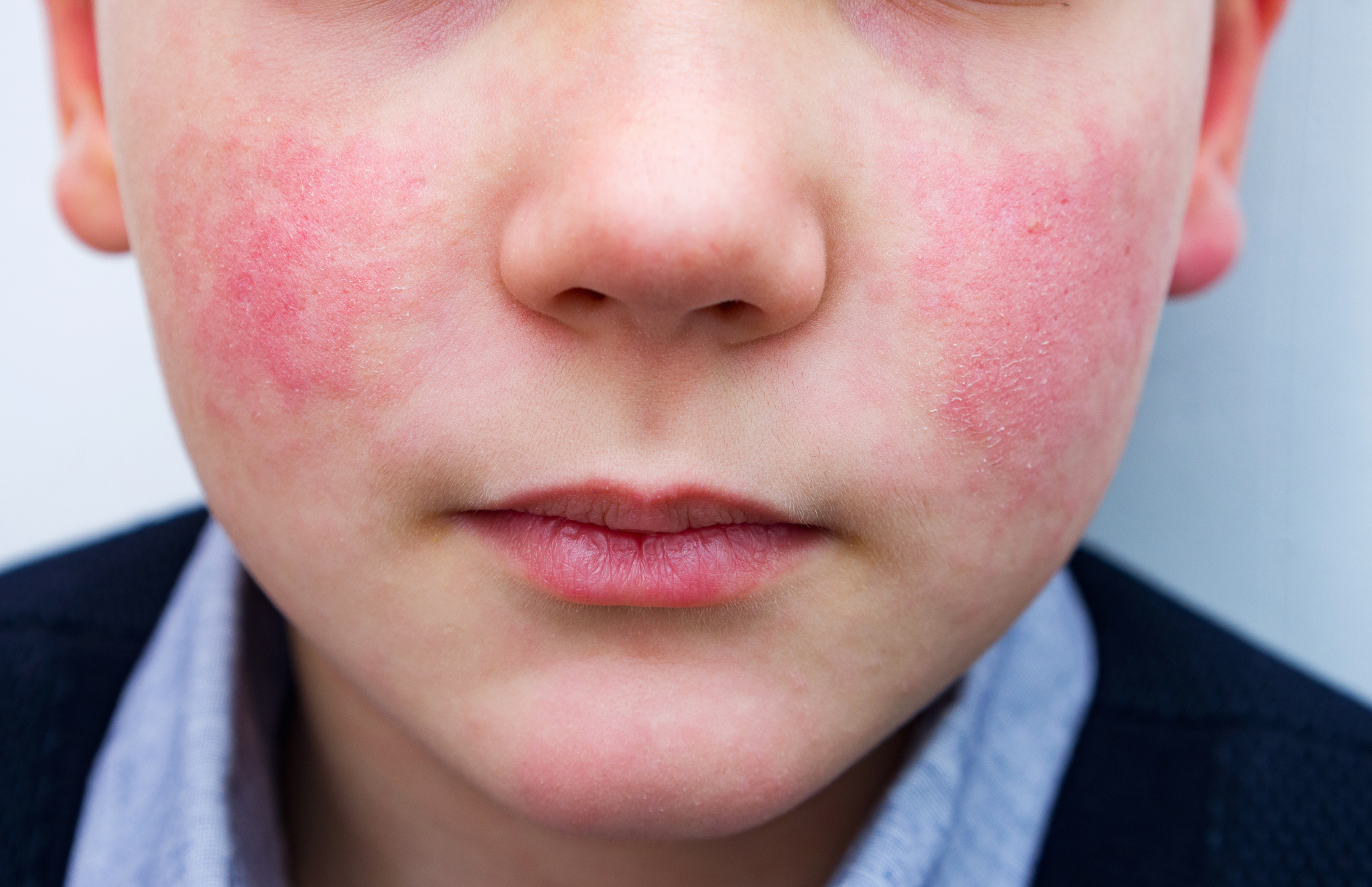
What it looks like
- Classic “slapped cheek” redness on the face.
- After that, a lacy, pink rash may appear on the trunk, arms, or legs.
- Rash can come and go for days to weeks, especially after warmth or sun exposure.
What causes it
A viral infection. Kids are often most contagious before the rash appears. By the time you see the rash, they usually feel better.
What you can do at home
- Focus on comfort: fluids, rest, and age-appropriate fever care if needed.
- Cool baths and loose clothing can reduce itchiness if present.
- Keep your baby home based on how they feel and your local childcare policies. Many kids can return once fever is gone and they are otherwise well.
When to call the doctor
- If your baby has a high fever, looks very ill, or you are worried about dehydration.
- If your baby has an immune condition or certain blood disorders (ask your clinician for individualized advice).
- If there is a pregnant person in the household or close contact circle who may have been exposed, it is worth a call to their OB or midwife for guidance.
Spot the difference
If all rashes look the same when you are tired, here are a few practical patterns that can help:
- Tiny red bumps in folds after warmth points toward heat rash.
- Red pimples on cheeks in a young newborn often points toward baby acne.
- Tiny white bumps on the nose are usually milia.
- Patchy redness exactly where something touched suggests contact dermatitis.
- Raised welts that move around are classic hives.
- Bright red cheeks then a lacy body rash is a fifth disease pattern.
Safe care for mild rashes
When you are not sure what you are looking at, gentle skin care is a safe place to start.
- Use lukewarm water for baths and keep them short.
- Choose fragrance-free cleanser and moisturizer.
- Avoid frequent product switching. “Trying everything” often irritates baby skin more.
- Skip essential oils and strongly scented creams on baby skin.
- Avoid using steroid creams unless your pediatrician has advised it for your baby and for that location on the body.
- Take a clear photo in good light. It helps you track changes and can be useful if you call your pediatrician.
A practical tip: when you call about a rash, clinicians often focus on how your baby is acting. A mild rash on a baby who is feeding well, peeing normally, and behaving like themselves is usually less urgent than a subtle rash on a baby who looks unwell.
Do not wait and see
Even if a rash seems minor, trust your instincts and call if something feels off. In addition to the emergency signs above, reach out promptly if you notice:
- Fever in a young infant or fever plus a rapidly spreading rash.
- Blistering or skin that looks burned.
- Signs of infection: warmth, swelling, pus, increasing pain, or honey-colored crust.
- Dehydration: significantly fewer wet diapers, very dry mouth, no tears when crying.
- Rash plus new medication or a new food exposure.
FAQ
Should I put lotion on a baby rash?
Often yes, but choose a fragrance-free cream and keep it simple. For heat rash, heavy ointments can trap sweat, so focus on cooling and drying first.
Is it normal for a rash to look worse when baby cries?
It can be. Crying increases facial blood flow, which can make redness more noticeable. If the rash is otherwise stable and baby seems well, this is not automatically a red flag.
Do I need to change laundry detergent?
If you suspect contact irritation or your baby has sensitive skin, switching to a fragrance-free, dye-free detergent is reasonable. Also skip fabric softeners and dryer sheets, which can leave residues.
A final note
Most baby rashes are a normal part of infancy, and many clear with time and gentle care. If you are unsure, take a photo, check how your baby is acting, and call your pediatrician. You are not overreacting. You are parenting.