Corneal Scratches in Toddlers: What to Do After an Eye Poke
Sarah Mitchell
Sarah Mitchell is a Registered Pediatric Nurse and a mother of three who has spent over a decade helping families navigate the beautiful, chaotic early years of childhood. She combines evidence-based medical knowledge with real-world parenting experience to offer practical, compassionate advice. At Awesome Parent, Sarah's mission is to help exhausted parents find solutions, trust their instincts, and finally get some sleep.
If your toddler just took a finger, toy, or a rogue board book corner straight to the eye, you are not alone. In pediatric triage, “eye poke” calls were everyday events. At home, they are the kind of everyday event that somehow always happens right before bedtime.
The tricky part is that a corneal scratch (a scratch on the clear front surface of the eye) can look a lot like pink eye at first. Both can cause redness and watery eyes. But the care is different, and some common “just try this” remedies can make things worse.

Corneal scratch vs pink eye
A corneal scratch often happens after a clear moment of impact, like a fingernail swipe during roughhousing, a sibling’s finger, or a toy to the face. Pink eye (conjunctivitis) is usually viral, bacterial, or allergy-related. Viral and bacterial can spread from person to person. Allergic pink eye is not contagious and is often in both eyes.
More suggestive of a corneal scratch
- Sudden onset right after an injury
- Lots of tearing (watery, not thick)
- Light sensitivity (photophobia), squinting, wanting lights off
- Complaints of pain or “something in my eye”
- Frequent blinking or keeping the eye closed
- Redness in one eye more than the other
More suggestive of pink eye
- Discharge or crusting, especially after sleep (often stickier with bacterial, but viral can crust too)
- Gritty irritation more than sharp pain
- Starts in one eye and spreads to the other within a day or two (common with viral, not a rule)
- Recent cold symptoms (viral) or known exposure at daycare
- Itching and sneezing (allergies), often both eyes
Important nuance: a scratched cornea can still have some discharge, especially after lots of tearing. And pink eye can be one-sided at first. If you are unsure, getting it checked is reasonable.
Why it can look dramatic
The cornea has a lot of nerve endings. Even a tiny scratch can feel very painful and cause intense tearing and squinting. In triage, we used to say: corneas are small but mighty.
This is also why a child with a corneal scratch may look worse than they are, while still needing appropriate evaluation and treatment.
What to do right away
1) Do a quick safety check
- If the injury involved chemicals (cleaning spray, detergent pod, pool chemicals), treat it like an emergency: flush the eye continuously for 15 to 20 minutes with lukewarm water or saline, and get urgent care or ER evaluation. If you can, call Poison Control (US: 1-800-222-1222) while you flush or on the way.
- If something penetrated the eye (rare, but possible with sharp objects), do not rinse or apply pressure. Place a light shield over the eye (like a paper cup taped in place) and get emergency care.
2) Rinse if there might be debris
If your child says “something is in there” and you suspect sand, dirt, or glitter, you can gently rinse with sterile saline if you have it. Preservative-free artificial tears (over the counter) are also a great, safe option for flushing. Clean, lukewarm water can be used in a pinch. The goal is to flush, not scrub.
3) Discourage rubbing
Rubbing can worsen a scratch. If your toddler is a determined face-rubber, this is a good moment for calm distraction: a show, a snack, a cool washcloth on the forehead, or a car ride to urgent care if needed.
4) Consider pain relief
If your child is otherwise healthy and can take them, age-appropriate doses of acetaminophen or ibuprofen can help with pain while you observe or head in for evaluation. Follow your pediatrician’s dosing guidance.
5) Skip contacts and eye makeup
For toddlers this is usually not relevant, but for older kids: no contacts until cleared, and keep the eye clean. Contact lens wearers have a higher risk of serious infection, so have a lower threshold for same-day evaluation.

What not to do
- Do not use leftover antibiotic drops from someone else’s old prescription. Wrong medication, wrong dosing, and contamination risk are real.
- Do not use any steroid eye drops unless a clinician specifically prescribed them for this eye problem. Steroids can slow corneal healing and can worsen certain infections. This is a big reason “pink eye drops” are not interchangeable.
- Do not use numbing drops at home (even if you somehow have access). They can delay healing and mask worsening symptoms.
- Do not patch the eye at home unless instructed. Patching used to be common for scratches, but it is not routinely recommended now because it does not reliably improve healing or pain and may increase infection risk in some situations.
- Do not try to remove something stuck on the eye with tweezers, cotton swabs, or a tissue. If you can see a foreign body that will not rinse out, it needs medical evaluation.
When to get urgent care or ER
Eyes are small, but the stakes are high, and toddlers cannot always describe what they feel.
Go to urgent care today (or call for same-day guidance) if
- Your toddler has significant pain, persistent tearing, or refuses to open the eye after 30 to 60 minutes
- There is light sensitivity that is more than mild
- You see blood in the white of the eye (a subconjunctival hemorrhage) that is spreading, or significant swelling
- There is discharge plus pain, or you suspect infection
- You cannot tell if the eye looks normal because your child will not let you look
Note: a small, stable red patch on the white of the eye after a poke can be harmless, but if there is pain, light sensitivity, or any vision concern, it still deserves a same-day check.
Go to the ER now if
- You suspect a penetrating injury or you see a cut on the eyeball itself
- There was a high-speed injury (projectile toy, bungee cord, lawn equipment nearby)
- Your child has vision changes (says they cannot see, vision is blurry, or one pupil looks different)
- The eye looks cloudy or you see a white spot on the cornea
- There is a chemical exposure (flush immediately for 15 to 20 minutes while heading in)
- Your child is extremely sleepy, vomiting, or has other concerning head injury signs
If your area has access to a pediatric ER with ophthalmology coverage, that is ideal for concerning eye injuries. Otherwise, start with the closest emergency department.
What a clinician may do
Knowing what to expect can lower the stress a notch.
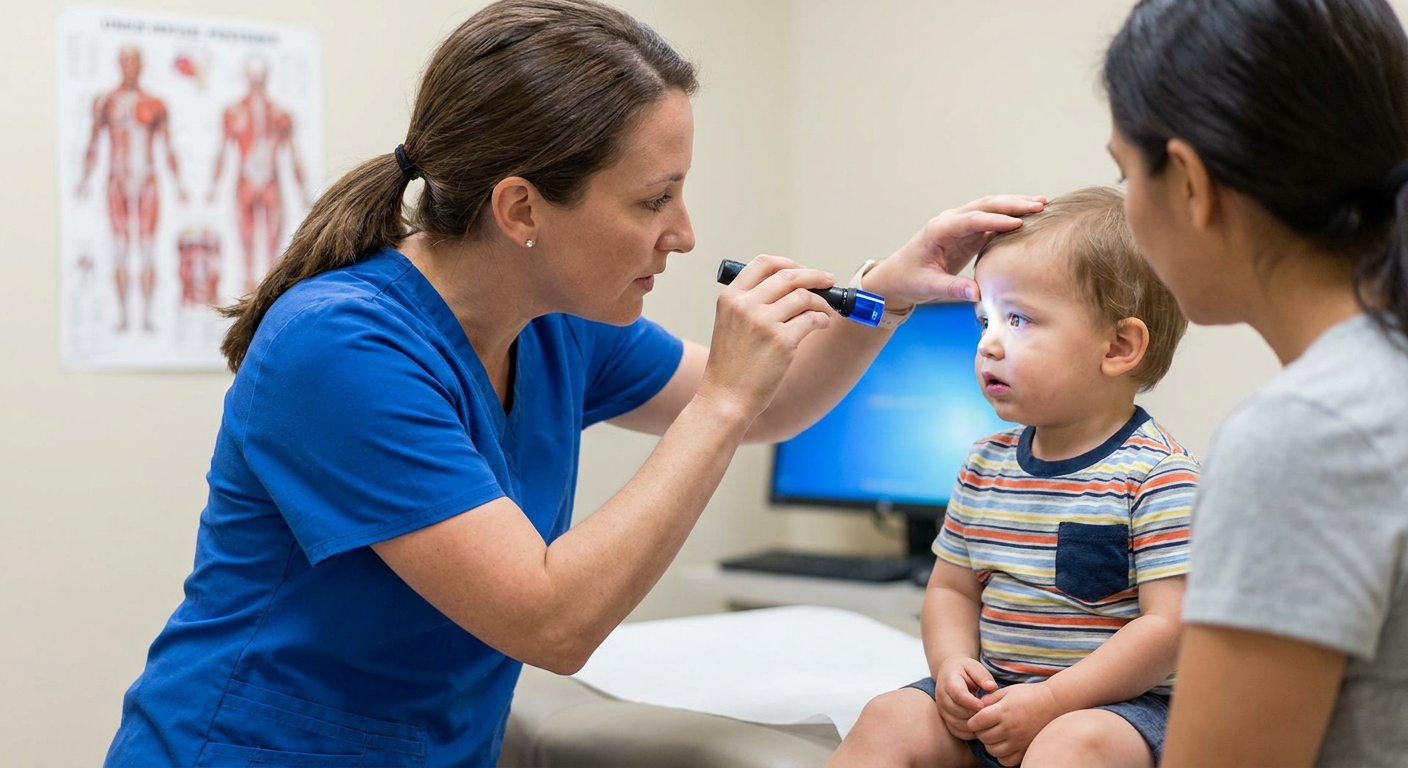
- History and exam with a light to look for obvious injury
- Fluorescein dye test: a drop of dye and a blue light can highlight a scratch
- Pain control: sometimes numbing drops are used in the clinic for the exam, but these are typically not sent home for routine use
- Antibiotic eye drops or ointment: often prescribed to prevent infection while the cornea heals, especially if the scratch is confirmed
- Follow-up plan: some kids need recheck in 24 to 48 hours, especially if symptoms are severe or the scratch is larger
- Occasionally: if the injury involved dirty material or a true penetrating injury, clinicians may also think about tetanus status
If it is pink eye
Pink eye treatment depends on the cause:
- Viral: supportive care (cool compresses, artificial tears, hand hygiene). It often just has to run its course.
- Allergic: allergy meds and/or allergy eye drops, and avoiding triggers when possible.
- Bacterial: sometimes antibiotic drops or ointment are prescribed, especially with significant discharge, daycare requirements, or certain risk factors.
Because the treatments are not interchangeable, it is worth getting eyes checked when the story starts with a poke.
How long healing takes
Many simple corneal scratches start feeling much better within 24 hours and heal within 1 to 3 days. Bigger scratches, ongoing foreign body sensation, or infection can take longer and need close follow-up.
Return for care if symptoms are not clearly improving by the next day, or if they worsen at any point.
Keeping them comfortable
- Dim the lights if they are light-sensitive
- Cool compress over the closed eye for a few minutes at a time
- Hand hygiene for everyone, especially if you are also considering pink eye
- Trim nails (yours and theirs). Most eye pokes are fingernails, not malice
- Give drops or ointment gently: for ointment, a small ribbon inside the lower lid is often easier than aiming a drop at a wiggly toddler
Quick recap
If you just need the highlights:
- Poke plus sudden pain, tearing, and light sensitivity points toward a corneal scratch.
- Itching, crusting, and both eyes involved points more toward pink eye (especially viral or allergic).
- Do not use steroid drops, numbing drops, or someone else’s old prescription.
- Chemical exposure: flush continuously for 15 to 20 minutes and go in.
Preventing the next poke
- Teach “hands to yourself” during play, especially with siblings
- Avoid sharp-edged toys for rambunctious play sessions
- Use age-appropriate toys and supervise projectile toys
- Keep toddler nails trimmed and filed when possible
Bottom line
If your toddler’s eye is tearing a lot, they are squinting, or they are light-sensitive after a poke or toy hit, a corneal scratch is a real possibility and deserves a same-day check if symptoms are more than mild. Pink eye often brings irritation, discharge or crusting, and may come with cold symptoms or allergy symptoms, depending on the cause.
And one last nurse-mom reminder: skip the DIY eye-drop experiments, especially anything with steroids. Your job right now is comfort, keeping little hands from rubbing, and getting the right evaluation when needed.
Medical note: This article provides general education and is not a substitute for medical care. If you are worried about your child’s eye or vision, seek urgent evaluation.