Cow’s Milk Protein Allergy in Babies
Sarah Mitchell
Sarah Mitchell is a Registered Pediatric Nurse and a mother of three who has spent over a decade helping families navigate the beautiful, chaotic early years of childhood. She combines evidence-based medical knowledge with real-world parenting experience to offer practical, compassionate advice. At Awesome Parent, Sarah's mission is to help exhausted parents find solutions, trust their instincts, and finally get some sleep.
If you are staring at a diaper at 2 a.m. thinking, Is this normal? you are in good company. Cow’s milk protein allergy, often shortened to CMPA, is one of the more common food allergies in infancy, and one of the most confusing. It can show up like reflux, colic, eczema, or poop changes, and it can make parents feel like they are playing whack-a-mole with symptoms.
This article will help you recognize the common patterns, understand the difference between IgE and non-IgE reactions, and know what feeding options typically look like. It is not a substitute for medical care, but it can help you walk into your baby’s appointment with clearer questions and a plan.

What CMPA is (and what it is not)
Cow’s milk protein allergy is an immune reaction to proteins in cow’s milk, most commonly casein and whey. The reaction can happen whether the milk protein comes from:
- Standard cow’s-milk-based infant formula
- Dairy in a breastfeeding parent’s diet, with small amounts of milk protein passing into breast milk
- Later, foods containing dairy
CMPA is different from lactose intolerance. Lactose intolerance is a problem digesting lactose (milk sugar), not an immune reaction to milk proteins. Primary lactose intolerance is uncommon in young infants. When parents say “my baby is lactose intolerant,” it is often not true lactose intolerance. It may be CMPA, reflux, normal newborn digestive immaturity, or in some cases a temporary lactose problem after an illness (secondary lactase deficiency).
CMPA vs lactose intolerance
- CMPA: immune driven. Can cause skin symptoms (eczema, hives), GI symptoms (blood or mucus in stool, vomiting), and sometimes respiratory symptoms. May affect growth and overall comfort.
- Lactose intolerance: digestive enzyme issue. Typically causes gas, bloating, watery diarrhea after lactose exposure. It does not cause hives or eczema.
IgE vs non-IgE CMPA
CMPA generally falls into two buckets. Some babies have one type, and some have a mixed picture. The type matters because it changes how symptoms show up and how clinicians usually confirm the diagnosis.
IgE-mediated (faster)
IgE reactions involve an allergy antibody called immunoglobulin E. Symptoms usually happen quickly, often within minutes to 2 hours after exposure.
- Hives or widespread redness
- Swelling of lips, face, or eyelids
- Vomiting soon after feeding
- Wheezing, coughing, noisy breathing
- Severe reactions can include anaphylaxis, which is an emergency
Non-IgE (delayed)
Non-IgE reactions are immune mediated but do not involve IgE antibodies. Symptoms tend to be delayed, showing up hours to days after exposure. These are the cases that can be hardest to connect to milk.
- Blood or mucus in stool
- Persistent diarrhea
- Constipation (can happen, but is less classic)
- Reflux-like symptoms, frequent spit-ups with discomfort
- Ongoing fussiness with feeds
- Eczema that is stubborn despite good skin care
- Poor weight gain in more significant cases
One classic non-IgE pattern is allergic proctocolitis, where a baby otherwise seems well but has blood-streaked or mucus-filled stools. It is scary to see, but many babies improve dramatically with removal of the triggering protein under pediatric guidance.
One quick clarification: there are other non-IgE food reactions too. For example, FPIES (food protein-induced enterocolitis syndrome) is a different condition that can cause repetitive, severe vomiting and lethargy after a trigger food, sometimes including cow’s milk. If vomiting is intense or your baby seems limp, unusually sleepy, or dehydrated, get urgent medical help.
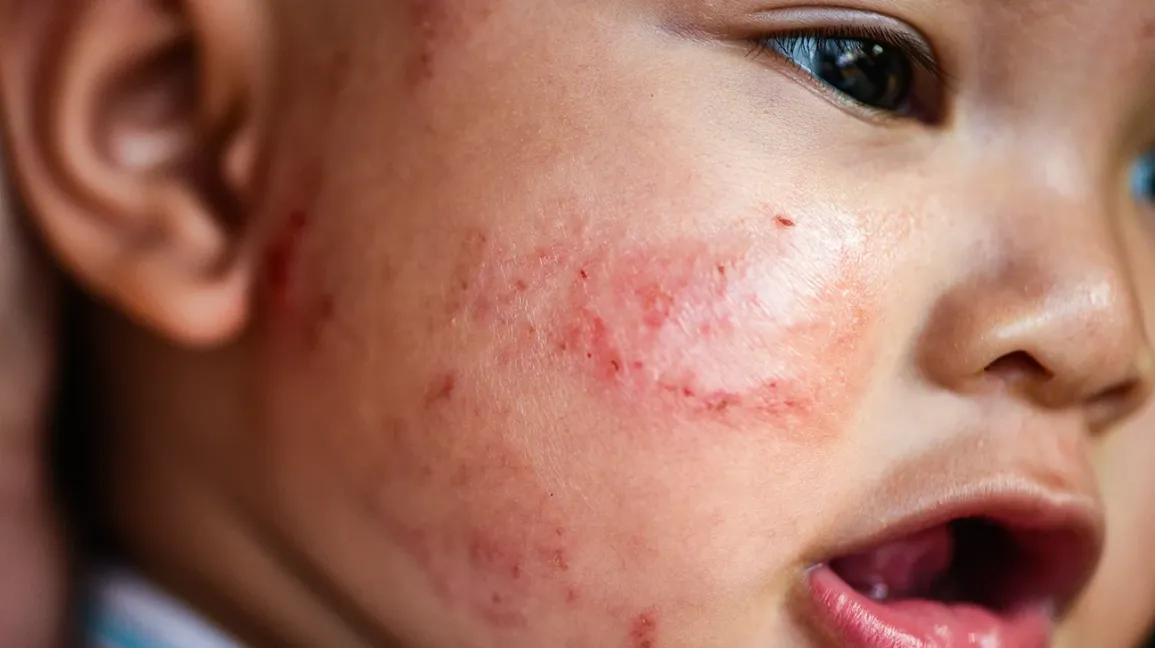
Common CMPA symptoms
CMPA can look different from baby to baby. Patterns matter more than any one symptom. Your pediatrician will look at timing (right after feeds or delayed), the symptom cluster, and growth.
GI symptoms
- Blood or mucus in stool
- Vomiting (more than typical spit-up, or vomiting with distress)
- Diarrhea or very frequent stools
- Constipation, painful stools, or straining that seems excessive (can be part of the picture)
- Reflux symptoms with discomfort, arching, feeding refusal
- Gassiness and fussiness that seems tied to feeds
Skin symptoms
- Eczema flare-ups
- Hives
- Persistent diaper rash that is hard to clear (sometimes, not always)
Breathing symptoms
Breathing symptoms are more commonly associated with IgE reactions and need careful evaluation.
- Wheezing
- Persistent cough soon after feeds
- Noisy breathing associated with milk exposure
A note from the triage desk: many of these symptoms can also come from reflux, viral illnesses, normal newborn stool variation, or other feeding issues. That is why the workup is usually structured. Non-IgE CMPA is often identified through a careful history plus an elimination and reintroduction plan. IgE-mediated CMPA is often evaluated with history plus testing, and sometimes a supervised food challenge.

Call your pediatrician
You never need to “wait it out” if your gut is telling you something is off. Call your pediatrician if your baby has:
- Blood in stool, especially if it is more than a tiny streak or keeps happening
- Vomiting that is forceful, frequent, or paired with lethargy
- Feeding refusal, painful feeds, or worsening reflux symptoms
- Eczema that is severe, infected-looking, or not improving
- Poor weight gain or fewer wet diapers
Get urgent help now if
- Swelling of lips, tongue, or face
- Wheezing, struggling to breathe, blue or gray color around lips
- Repeated vomiting with sudden hives or sleepiness
- Any signs of anaphylaxis
If your child has known or suspected IgE-mediated allergy, ask your clinician whether an epinephrine auto-injector is needed and what your emergency plan should be.
How CMPA is diagnosed
There is no single perfect test for every baby with suspected CMPA. In real life, diagnosis is often based on:
- A detailed symptom and feeding history
- Response to eliminating cow’s milk protein
- Return of symptoms with reintroduction, when appropriate and guided
Testing: useful sometimes
- IgE-mediated CMPA: skin prick testing and or blood IgE testing can be helpful alongside history. Your pediatrician may refer you to an allergist. Some families also need a supervised oral food challenge for clarity and safety.
- Non-IgE CMPA: skin and blood IgE tests are often negative. Diagnosis is usually clinical with elimination and re-challenge.
Because babies can have overlapping issues, your pediatrician may also consider reflux disease, infections, anal fissures, or other GI concerns depending on symptoms and age.
Formula options
If your baby is formula-fed or combo-fed, changing formula is often part of the plan. This should be done with your pediatrician’s input, especially for young infants or babies with poor growth. The goal is not to try every can on the shelf. It is to choose the next most likely step and give it enough time to be meaningful.
1) Extensively hydrolyzed
These formulas contain cow’s milk proteins that are broken into smaller pieces, which many babies with CMPA can tolerate. They are often recommended first for mild to moderate CMPA.
- Commonly used for non-IgE symptoms and many IgE cases
- Some babies still react, especially with more sensitive allergies
2) Amino acid
These formulas use proteins in their simplest form (amino acids) and are tolerated by the vast majority of babies with CMPA. They are often used when:
- Symptoms are severe
- There is poor weight gain
- There is no improvement on extensively hydrolyzed formula
- There are multiple food allergies suspected
3) Soy (sometimes)
Soy formula may be an option for some babies, depending on your clinician’s guidance and your baby’s symptom type. Because some babies with CMPA also react to soy protein, and because recommendations vary by age and guideline, some clinicians prefer to consider soy later in infancy (often after 6 months in some guidance).
Gentle or lactose-free?
This is a common trap, and it is not your fault. “Gentle,” “sensitive,” or lactose-free formulas may help with lactose-related fussiness or mild digestive discomfort, but they often still contain cow’s milk protein. If CMPA is the issue, lactose-free alone usually does not fix it.

Breastfeeding notes
If you are breastfeeding, you did not cause this. And you do not automatically have to stop breastfeeding. In many cases, babies improve when the breastfeeding parent removes cow’s milk protein from their diet for a period of time.
Typical elimination
- Remove dairy (milk, cheese, yogurt, butter, cream, and foods containing milk ingredients) under your pediatrician’s guidance.
- Watch for timing: GI symptoms may improve within a few days to 2 weeks. Skin symptoms (like eczema) can take a few weeks to settle.
- Track symptoms: jot down stools, skin changes, spit-ups, and overall comfort. Sleep-deprived brains deserve receipts.
Hidden dairy is real
Milk can show up in ingredient lists as casein, whey, milk solids, and other milk-derived ingredients. Also, “non-dairy” on a label does not always mean milk-protein-free. If label reading makes your eyes cross, you are not alone. Ask your clinician if a dietitian referral makes sense, especially if more than one food needs to be removed.
Do you need soy-free too?
Sometimes. For certain non-IgE presentations, clinicians may recommend removing soy as well if symptoms do not improve with dairy elimination alone. Do not remove multiple food groups without medical guidance, especially if you are postpartum and already running on fumes.
Nutrition matters
If you are dairy-free, make sure you are getting adequate calcium and vitamin D through fortified alternatives or supplements recommended by your clinician. Your body is doing a lot right now.
Elimination and reintroduction
Most babies with CMPA improve with time, and many outgrow it in infancy or early childhood. Timelines vary widely, but it is common for symptoms to show up in the first months of life and for tolerance to develop sometime between ages 1 and 3. Your clinician can help you decide when and how to test for outgrowing safely.
Step 1: Elimination trial
- Remove cow’s milk protein via formula change and or maternal diet changes (if breastfeeding)
- Monitor for symptom improvement as directed by your pediatrician
Step 2: Confirming
Because babies can improve for reasons unrelated to milk removal, many clinicians recommend a supervised reintroduction at an appropriate time. This is especially important before committing to long-term restriction.
Step 3: Reintroduction
- Non-IgE CMPA: reintroduction is often done gradually at home with pediatric guidance, sometimes starting with baked milk in older infants if appropriate.
- IgE-mediated CMPA: reintroduction may require allergist oversight, and sometimes an in-office oral food challenge for safety.
Do not try reintroduction on your own if your baby has had immediate reactions like hives, swelling, or breathing symptoms.
When to see an allergist
Your pediatrician may manage many CMPA cases without a specialist. An allergist is often helpful when:
- Symptoms suggest IgE-mediated allergy (hives, swelling, wheeze, immediate vomiting)
- There is a history of a severe reaction
- Multiple food allergies are suspected
- Eczema is moderate to severe and food triggers are unclear
- You need guidance on safe reintroduction or an oral food challenge
Day-to-day tips
- Give changes enough time. It is tempting to switch formulas every two days, but that can make symptoms harder to interpret.
- Read labels like a detective. Look for “contains milk” statements, and remember that “non-dairy” does not always mean milk-free.
- Protect the diaper area. If stools are irritating, a thick barrier cream and gentle cleaning can help while the gut calms down.
- Ask about weight checks. If feeding has been stressful, periodic weight checks can reassure you that baby is growing well.
- Trust your instincts. You know your baby’s “normal,” even if you cannot perfectly explain it.
Bottom line
CMPA can be a messy, confusing season, but it is also a solvable one. The most important steps are identifying the pattern, choosing the right feeding plan, and working with your pediatrician to eliminate and reintroduce safely. If symptoms include immediate reactions like hives or breathing changes, loop in an allergist quickly and treat it as urgent.
If you are in the middle of this right now: take a breath, write down what you are seeing, and call your pediatrician. You are not overreacting. You are parenting.