Ear Tubes for Kids: Signs, Timing, and What Surgery Is Like
Sarah Mitchell
Sarah Mitchell is a Registered Pediatric Nurse and a mother of three who has spent over a decade helping families navigate the beautiful, chaotic early years of childhood. She combines evidence-based medical knowledge with real-world parenting experience to offer practical, compassionate advice. At Awesome Parent, Sarah's mission is to help exhausted parents find solutions, trust their instincts, and finally get some sleep.
If you are reading about ear tubes at 3 AM, you are in good company. In triage, I met so many parents who could list every ear infection by month like it was a part-time job. If your child has had back-to-back ear infections or fluid that just will not clear, your pediatrician may mention “tubes” and suddenly it feels like a big, scary leap.
Here is the reassuring truth: ear tubes are one of the most common pediatric procedures, and for the right child they can mean fewer infections, clearer hearing, and (for some families) better sleep once pressure and pain settle down. Let’s walk through the signs, what an ENT visit is like, what the surgery typically involves, and what still deserves a recheck afterward.
Quick note: This is general information, not medical advice. Your child’s best plan depends on their history, exam, and hearing testing.
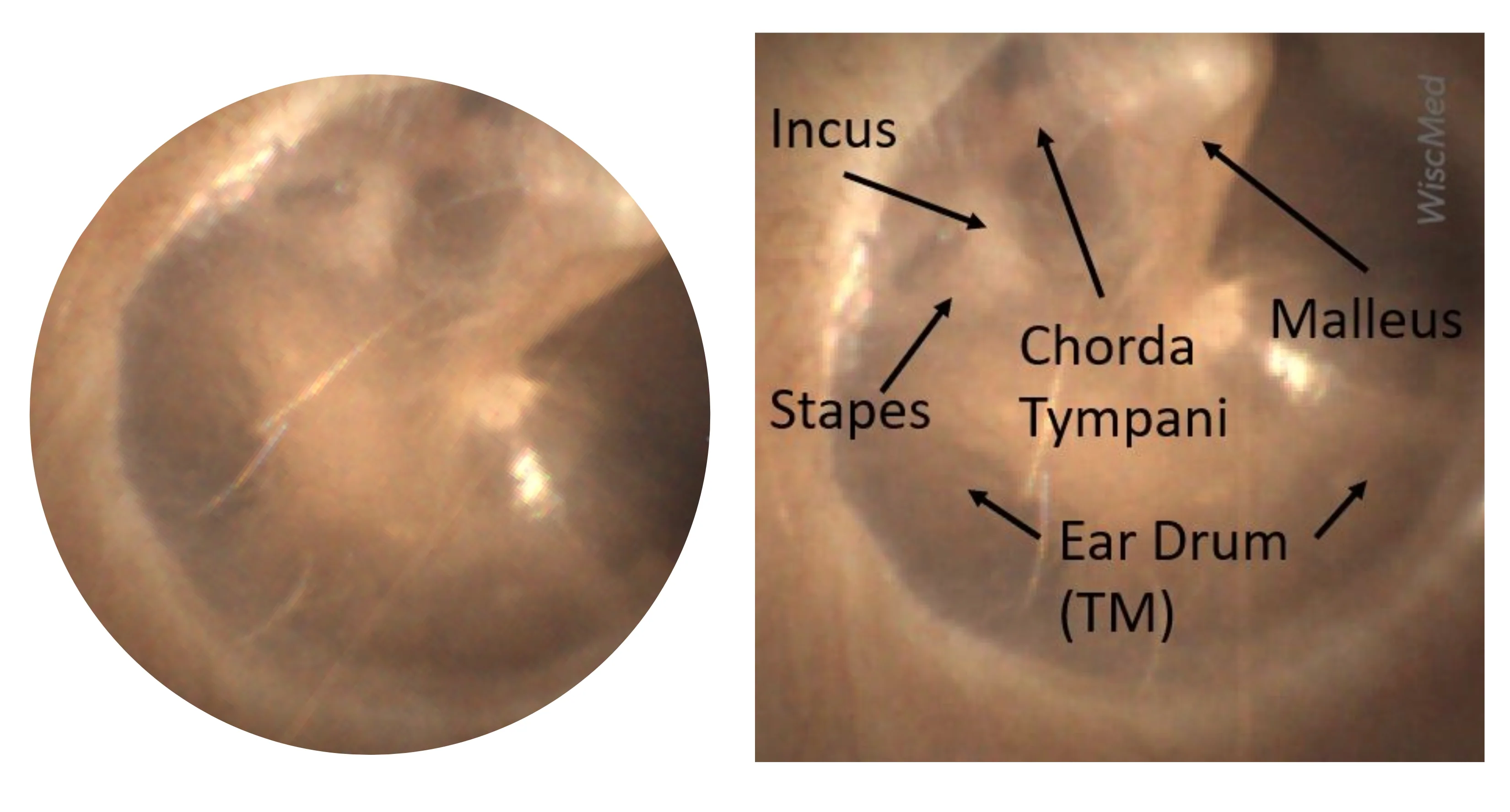
What ear tubes do
Ear tubes, also called tympanostomy tubes, are tiny hollow tubes placed through the eardrum. Their job is simple: let air into the middle ear and let fluid drain out so pressure does not build up.
Most ear problems in little kids trace back to the Eustachian tube, the narrow canal that helps ventilate the middle ear. In toddlers it is shorter and more horizontal, so it clogs easily during colds, allergies, or daycare season. When it stays blocked, fluid can sit behind the eardrum for weeks or months. That fluid can muffle hearing and can also set the stage for repeat infections.
Signs tubes may help
Only an ENT can say for sure, but these are the common reasons tubes come up in real life.
1) Frequent ear infections
Many ENTs use commonly cited AAO-HNS/AAP criteria when discussing tubes for recurrent acute otitis media, such as:
- 3 or more ear infections in 6 months, or
- 4 or more ear infections in 12 months (especially if at least 1 happened in the last 6 months)
Important nuance: tubes are most clearly helpful for recurrent infections when there is middle-ear fluid (effusion) present at the ENT visit (or documented around the episodes). If a child has recurrent infections but no effusion at evaluation, many guidelines recommend a more cautious, individualized approach because the benefit of tubes is less clear.
Either way, the decision is personal. A child who is miserable, missing childcare, needing repeated antibiotics, or getting infections that do not respond well may be a stronger candidate.
2) Persistent fluid (even without infections)
Fluid behind the eardrum that lasts 3 months or longer is called chronic otitis media with effusion. Some kids feel fine, but others have:
- Muffled hearing or “not listening” behavior
- Speech delay or unclear speech
- Balance issues or clumsiness that is new
- Ear pressure, popping, or discomfort
Not every child with fluid needs tubes, but if the fluid is persistent and hearing is affected, tubes can be very helpful.
3) Hearing or speech concerns
Parents often notice the day-to-day signs first:
- TV volume creeping up
- Not responding unless you are close or facing them
- Seeming “spacey” at preschool
- Speech that stalls or becomes harder to understand
Hearing matters most during early language development. If hearing tests show hearing loss from middle-ear fluid, tubes are often recommended.
4) Higher-risk kids
Some children are more vulnerable to the effects of chronic fluid and temporary hearing loss. ENTs may move faster toward tubes for kids with developmental delays, known speech and language disorders, autism, certain craniofacial differences, or other conditions linked to more persistent Eustachian tube dysfunction and effusions.

What the ENT visit is like
ENT visits are typically straightforward and very data-driven. Expect some combination of the following:
- History review: How many infections, how treated, how severe, and how often symptoms return.
- Ear exam: A careful look at the eardrum for fluid, retraction, scarring, or infection.
- Tympanometry: A quick test that checks how the eardrum moves, which helps confirm fluid or pressure behind it.
- Hearing test: Age-appropriate audiology testing. For toddlers it may be a “listening game” (often called conditioned play audiometry), and for babies it may involve specialized measures.
Bring what you have: dates of infections, antibiotics used, any reactions, and notes about sleep, hearing, daycare absences, and speech concerns. If you have videos of loud TV volume or “what?” moments, that is fair game too.
Who is a good candidate
In plain terms, tubes are most likely to help when one of these is true:
- Recurrent ear infections plus effusion at the time of assessment.
- Chronic middle-ear fluid (often 3 months or more), especially with hearing impact.
- Fluid plus developmental or learning risk where hearing clarity matters urgently.
Sometimes the best choice is still “wait and watch,” especially if infections are slowing down or fluid is improving, the child’s hearing is normal, and symptoms are mild. A good ENT will explain the trade-offs without pressure.
What surgery involves
Most ear tube placement is a short, same-day procedure. Here is the usual play-by-play.
Before surgery
- Pre-op instructions: You will get guidance about when your child must stop eating and drinking. Follow these closely for anesthesia safety.
- Health check: If your child has a fever or significant respiratory symptoms right before surgery, the team may postpone. This is frustrating, but it is about airway safety.
During surgery
For young children, ear tubes are usually placed under brief general anesthesia. The surgeon:
- Makes a tiny opening in the eardrum
- Suctions out fluid if present
- Places the tube in the opening
The procedure itself is often under 15 minutes, though you will be at the surgical center longer for check-in, anesthesia, and recovery.
After surgery
- Wake-up: Kids can be groggy or cranky coming out of anesthesia. Some cry hard for a few minutes. It is normal and usually short-lived.
- Pain: Many children have minimal pain. If needed, your surgeon will recommend appropriate dosing for acetaminophen or ibuprofen.
- Ear drops: Some ENTs prescribe drops for a few days, especially if there was thick fluid. Others do not. Follow your surgeon’s specific plan.
- Drainage: A little clear or blood-tinged drainage in the first day can be normal. Your discharge instructions will tell you what is expected.
Back to normal
- Activity: Many kids are back to normal play within 24 hours.
- Daycare and school: Often the next day, depending on how they are acting and your surgeon’s instructions.
Benefits you may notice
Not every child has a dramatic change overnight, but families commonly report:
- Fewer ear infections and fewer antibiotics
- Improved hearing, sometimes immediately if fluid was present
- Less ear pain and pressure during colds
- Better sleep for some children, especially if ear pressure and night waking were a theme
How fast do hearing and speech changes happen? Hearing often improves quickly if fluid was the main issue. Speech may take weeks to months to catch up, and some children still benefit from speech therapy even after hearing clears. Tubes help create a better “sound environment,” but they are not a stand-alone speech treatment.
One of my favorite moments as a nurse is when a parent says, “I did not realize how much they were missing until after tubes.”
Risks and downsides
Ear tubes are very common and generally safe, but no procedure is zero-risk. The ENT should review these with you:
- Ear drainage (otorrhea): Some children get drainage, especially after a cold. It is often treated with ear drops.
- Blocked tube: Sometimes a tube clogs and stops working.
- Tube falls out: This is expected eventually. Many short-term tubes fall out on their own in about 6 to 18 months, depending on the type. Some longer-lasting tubes are designed to stay in longer.
- Need for repeat tubes: Some kids outgrow ear problems after one set, others need another set later.
- Small persistent eardrum hole: Rarely, the hole does not close after the tube comes out and needs repair.
- Scarring: Mild scarring can occur, and in most cases it does not have a major impact on hearing.
Water precautions
Water rules can be confusing because advice varies by surgeon and by child. In general, evidence and many modern ENT recommendations suggest routine earplug use is not necessary for most kids during surface swimming in clean, chlorinated pools. That said, your ENT’s plan should win, especially if your child has a history of frequent drainage.
Baths and hair washing
- Normal bathing is usually fine.
- Try to avoid soapy water being forced directly into the ear canal. Soap lowers surface tension and can travel more easily.
Swimming
- Surface swimming in clean pools: Often fine without ear plugs for many kids.
- Lakes, rivers, ocean, or non-chlorinated water: Many ENTs recommend ear plugs because these waters carry more bacteria.
- Diving or deep submersion: Pressure can push water through the tube. Ear plugs are often recommended.
If your child gets ear pain or drainage after water exposure, that is a clue they may need plugs, a swim band, or adjusted swim habits.

Infections can still happen
Tubes do not make kids immune to ear infections. They change the type of problem you see.
- Instead of pressure building behind the eardrum, you may see ear drainage.
- Kids often have less pain because the tube vents pressure.
- Treatment is commonly ear drops instead of oral antibiotics, depending on your clinician’s assessment.
If you see drainage, do not assume the tubes “failed.” Often it means the tube is doing its job by letting infected fluid out.
When to recheck
I always tell parents: tubes are helpful, not magic. Call your pediatrician or ENT if you notice any of the following:
- Drainage that lasts more than a few days or keeps returning
- Foul-smelling, thick, or green drainage
- Fever with significant ear symptoms
- Ear pain that is severe or not improving with recommended meds
- New hearing concerns or speech regression
- Dizziness, balance changes, or vomiting with ear symptoms
- Swelling or redness behind the ear, ear pushed forward, or significant tenderness of the bone behind the ear
And of course, if your parent gut is waving a red flag, it counts.
Follow-up
Most ENTs like to see kids after surgery to confirm the tubes are open and positioned well. After that, follow-ups may be every 6 to 12 months, often with hearing checks if there were concerns before.
Tubes usually fall out on their own. If a tube stays in longer than expected, the ENT may monitor and discuss removal.
Adenoids and other add-ons
If your child is a little older (often over age 4) or has significant nasal obstruction, chronic mouth breathing, snoring, or persistent fluid issues, the ENT may talk about whether adenoids are part of the story. In select children, an adenoidectomy can be considered along with tubes. This is very individualized, so it is a great question to bring up if symptoms point that direction.
Questions to ask your ENT
- Based on my child’s history, what is the main goal of tubes: fewer infections, better hearing, or both?
- Does my child have fluid today?
- What did the hearing test show?
- For recurrent infections, does the presence or absence of effusion change your recommendation for us?
- What type of tubes are you recommending and how long do they usually last?
- Do you recommend ear plugs for baths or swimming in our situation?
- If we see drainage, do you want us to start drops right away or call first?
- What symptoms would make you want to see my child urgently?
A calm bottom line
Ear tubes are usually considered when ear infections keep piling up (especially when fluid is present at evaluation) or when fluid sticks around long enough to affect hearing and day-to-day life. The surgery is brief, typically same-day, and many families see real relief afterward.
If you are on the fence, that does not mean you are “overreacting” or “not tough enough.” It means you are weighing real pros and cons for your specific child, and that is exactly what a good parent does.