Earwax Buildup in Babies and Toddlers
Sarah Mitchell
Sarah Mitchell is a Registered Pediatric Nurse and a mother of three who has spent over a decade helping families navigate the beautiful, chaotic early years of childhood. She combines evidence-based medical knowledge with real-world parenting experience to offer practical, compassionate advice. At Awesome Parent, Sarah's mission is to help exhausted parents find solutions, trust their instincts, and finally get some sleep.
If you have ever looked in your child’s ear and thought, That cannot be normal, you are in very good company. Earwax can look dramatic. It can be orange, brown, flaky, sticky, or weirdly shiny. And because babies and toddlers cannot exactly say, “Hey, my ear feels full,” it is easy to worry you are missing something important.
Here is the reassuring truth: earwax is usually a good thing. Most kids do not need their ear canals cleaned at home at all. The goal is not “no wax.” The goal is comfortable ears and normal hearing, with safe care when wax builds up.
Quick note: This article is general education, not a diagnosis. When in doubt, your pediatrician is the right call.

What earwax does
Earwax is also called cerumen. It is made by glands in the outer part of the ear canal and mixed with tiny skin cells. It is not dirt, and it is not a sign you are not bathing your child well enough.
Earwax helps by:
- Protecting the ear canal by trapping dust and small particles before they reach deeper.
- Moisturizing the skin inside the canal so it does not crack and itch.
- Reducing infection risk because it has mild antimicrobial properties.
- Self-cleaning: the ear canal naturally moves wax outward over time, like a slow conveyor belt.
Because of that self-cleaning design, most wax belongs exactly where it is. And yes, dark brown wax can still be normal if your child is comfortable and hearing well.
When earwax is too much
Wax becomes a problem when it builds up and blocks the ear canal. This is called impaction. It can happen in babies and toddlers, especially if:
- Someone has been using cotton swabs in the canal, which often pushes wax deeper.
- Your child has narrow or curvy ear canals.
- Your child makes drier, thicker wax.
- Your child uses hearing aids or earplugs (less common in toddlers, but it happens).
- There is a lot of eczema or flaky skin in the ear canal.
One important note from my triage-nurse days: parents often notice wax right at the opening and assume it is blockage. Visible wax is not automatically a problem. We care about symptoms.
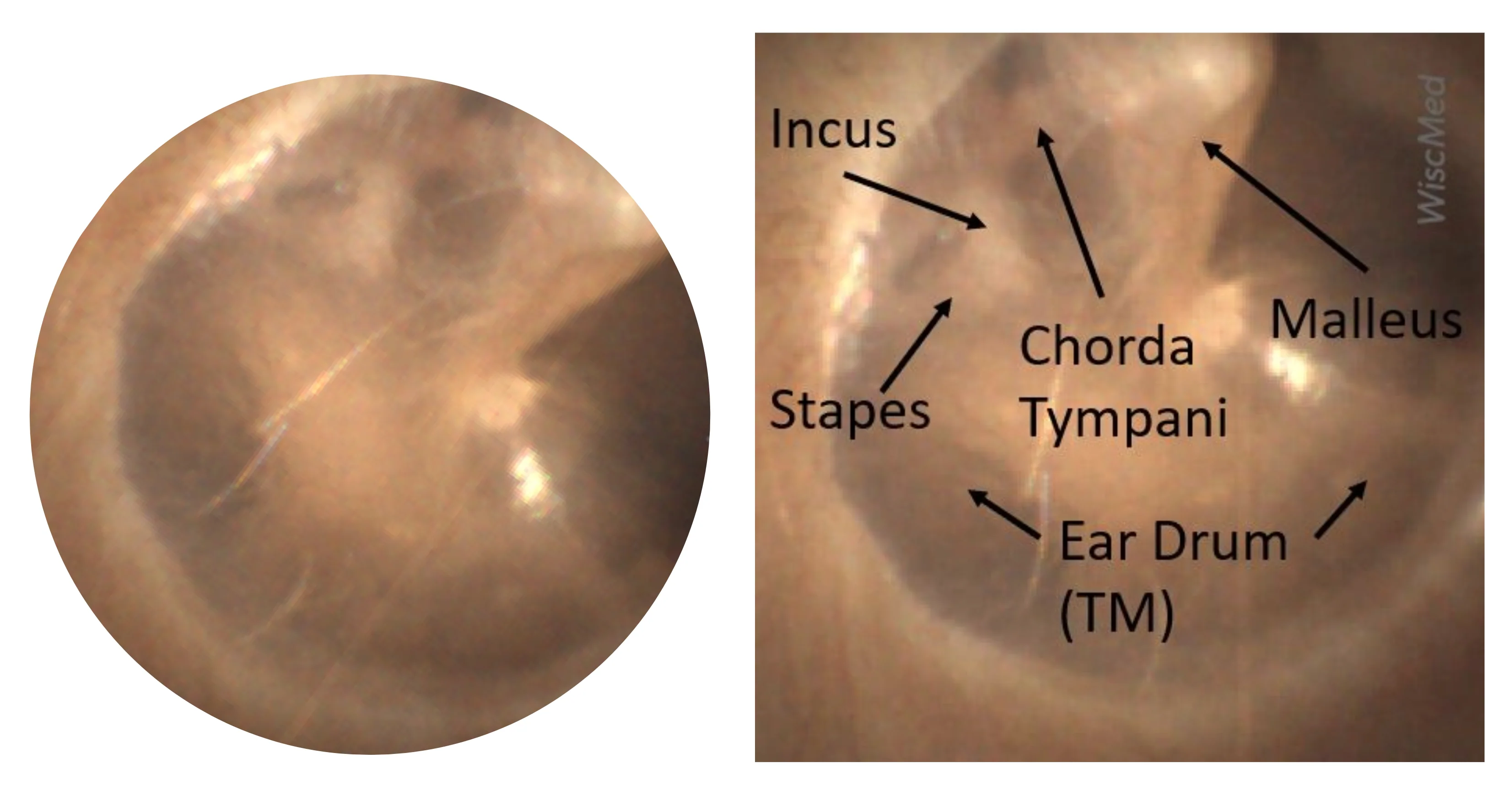
Signs of impacted earwax
In babies and toddlers, impacted wax can look like a lot of things, so it helps to focus on a few consistent clues.
Possible signs
- Hearing seems off: not responding to quiet sounds, needing the TV louder, not reacting to their name like usual.
- Ear pulling or rubbing, especially without other cold symptoms.
- Fullness or discomfort: older toddlers may say the ear feels “blocked” or “funny.”
- Itching inside the ear.
- Wax you can see that looks packed in and does not seem to be moving outward over time.
- Difficulty seeing the eardrum at a doctor visit because wax is in the way. This matters because it can prevent an accurate ear exam.
What earwax does not do
Earwax can cause mild discomfort, but earwax alone does not cause fever. If your child has fever, significant pain, or seems unwell, that is a different situation and needs medical evaluation.
Earwax vs infection
These get mixed up constantly, and understandably. Both can involve ear tugging, fussiness, and sleep disruption.
Wax buildup is more likely when
- Symptoms are mostly muffled hearing, fullness, or itching.
- There is no fever and your child otherwise seems okay.
- Discomfort is mild and comes and goes.
Middle-ear infection is more likely when
- There is moderate to severe ear pain, especially after a cold.
- Your child has fever or is generally ill.
- Sleep and comfort are significantly affected.
- You notice new drainage from the ear (more concerning if your child has tubes, or if you suspect a ruptured eardrum).
Important: you cannot diagnose a middle-ear infection just by looking from the outside. You need an exam of the eardrum, which is another reason we try not to “DIY” deep cleaning at home.
What about swimmer’s ear?
Swimmer’s ear (also called otitis externa) is an infection or inflammation of the ear canal skin. It is more likely after a lot of water exposure, and it often causes tenderness when the outer ear is moved and more noticeable canal pain. Sometimes there is drainage. It is a different problem from wax buildup and a different problem from a middle-ear infection.
If ear pain starts after swimming or bathing and the outside of the ear is very sensitive to touch, it is worth getting checked.
What not to do
This is the part where I gently take the cotton swabs out of your hand at 3 AM.
- Do not put cotton swabs inside the ear canal. They frequently push wax deeper, can scratch the canal, and can even perforate the eardrum if a child jerks.
- Do not use ear candles. They do not safely remove wax and can cause burns.
- Do not use hairpins, fingernails, tweezers, or “ear picking” tools. These can injure the canal and increase infection risk.
- Do not flush the ear with a bulb syringe unless your clinician specifically instructed you and confirmed the eardrum is intact.
If you remember one line: Nothing smaller than your elbow goes in the ear. Corny. Effective.
Safe cleaning at home
For most kids, safe “cleaning” means outer-ear care only.
1) Clean only what you can see
- Use a soft washcloth or cotton ball.
- Dampen with warm water.
- Wipe the outer ear and the crease behind the ear.
- If wax is sitting right at the entrance, you can wipe it away gently, without pushing into the hole.
2) After baths, let ears dry naturally
Water in the outer ear is common after bath time. Tilt your child’s head to each side and gently dry the outside with a towel. Skip inserting anything to “dry inside.”
3) Ask your clinician before using wax-softening drops
Some wax-softening drops are available over the counter (common examples include carbamide peroxide, mineral oil, or saline-based products). They can be helpful in some situations, but in babies and toddlers I recommend using them only if your pediatrician says it is appropriate.
Reasons include:
- If there is an unseen hole in the eardrum, drops can cause pain or complications.
- If your child has ear tubes, some products are not recommended.
- If the problem is actually infection or a foreign object, drops can muddy the situation.
- Peroxide-based products can irritate delicate canal skin if used incorrectly or too often.
If your clinician recommends drops, follow the exact product and dosing guidance they give. More is not better here.
When to see the doctor
Earwax is a great reason to schedule a normal visit when it is affecting hearing or getting in the way of a good ear exam. You do not need to wait until it is an emergency.
Call your pediatrician soon if
- You suspect hearing changes that do not quickly resolve, or last into the next day.
- Your child has ear discomfort that is not improving.
- There is a history of ear tubes, a previous eardrum perforation, or chronic ear problems and you think wax is building up.
- You see wax plus speech delay concerns or your child is missing sounds they used to respond to.
Seek same-day care or urgent evaluation if
- Fever is present with ear symptoms (especially in babies).
- Your child has moderate to severe pain.
- There is drainage from the ear that is new, foul-smelling, bloody, or pus-like.
- Your child seems very ill, unusually sleepy, or inconsolable.
- There is swelling or redness behind the ear, or the ear is pushed forward.
- You suspect a foreign object in the ear (toddlers are impressively creative).
Extra important for little ones: any ear drainage in a young infant should be checked promptly.
If your baby is under 3 months with a rectal temperature of 100.4°F (38°C) or higher, follow your pediatrician’s fever guidance right away.
How doctors remove earwax
In clinic, we have a few safe options depending on your child’s age, cooperation level, and what the wax looks like.
- Gentle curette removal: a small tool used to lift wax out under direct visualization.
- Suction: often used by ENT specialists, especially for sticky wax.
- Irrigation: flushing with warm water in carefully selected cases, usually not the first choice for very young children.
We also check the ear canal skin for irritation and make sure the eardrum looks healthy once the wax is cleared. Sometimes the biggest benefit is simply that we can finally see what is going on in there.
Common questions
Is it normal for my toddler to have a lot of earwax?
Yes. Wax production varies a lot from child to child. “A lot” is only a problem if it is causing symptoms or blocking the canal.
My baby has yellow wax. Is that infection?
Not necessarily. Earwax can be yellow, orange, or brown. Infection concerns are more about drainage that is wet, pus-like, foul-smelling, or associated with pain and fever.
Can earwax affect speech development?
Persistent hearing reduction can impact speech and language over time. If you suspect your child is not hearing well, it is worth getting checked. Most of the time, the fix is straightforward.
Should I clean my child’s ears every day?
Nope. Daily deep cleaning is not needed and can cause more buildup by pushing wax inward. Outer-ear wiping during bath time is plenty.
A simple plan
If you are staring at earwax right now, here is your calm checklist:
- Leave the canal alone.
- Wipe only the outside with a soft damp cloth.
- Watch for symptoms: pain, fever, drainage, or hearing changes.
- Call your pediatrician if hearing seems affected or discomfort persists.
- Get urgent care for significant pain, fever with ear symptoms, or new drainage.
You are not failing because your child has earwax. You are parenting a tiny human with functioning ears. That is a win in my book.
