Fifth Disease and Pregnancy
Sarah Mitchell
Sarah Mitchell is a Registered Pediatric Nurse and a mother of three who has spent over a decade helping families navigate the beautiful, chaotic early years of childhood. She combines evidence-based medical knowledge with real-world parenting experience to offer practical, compassionate advice. At Awesome Parent, Sarah's mission is to help exhausted parents find solutions, trust their instincts, and finally get some sleep.
If you are pregnant and someone says the words “fifth disease”, your brain tends to jump straight to worst-case scenarios. I get it. In triage, I took calls like this every spring: a preschool classroom outbreak, a sibling with rosy cheeks, a teacher who just found out she is 12 weeks along.
Here is the reassuring truth: most exposures in pregnancy do not lead to fetal problems. But because parvovirus B19 can occasionally affect a pregnancy, it is one of those infections where your obstetrician may recommend targeted bloodwork and, sometimes, ultrasound monitoring.
This page is different from our child-focused fifth disease article. In kids, the main job is comfort care and knowing when to keep them home. In pregnancy, the job is figuring out whether you are immune, whether a new infection happened, and whether the baby needs closer watching.

Quick refresher: what is fifth disease?
Fifth disease is caused by parvovirus B19. In children it often shows up as:
- Cold-like symptoms (or none at all) at first
- Bright red “slapped cheek” rash
- A lacy rash on the body afterward
Adults may not get a classic rash. They are more likely to have joint pain, mild fever, or just feel run-down.
How it spreads
Parvovirus B19 spreads mainly through respiratory droplets (coughing, sneezing) and close contact. It can also spread through blood products, though that is less common.
The timing detail most parents do not hear
Kids are typically most contagious before the rash appears. In immunocompetent children, once the rash shows up, many are no longer contagious. By the time you see those adorable rosy cheeks, the high-transmission window may already be closing. That does not erase risk entirely, but it helps explain why outbreaks can feel like they come out of nowhere.
Why parvovirus B19 matters in pregnancy
In pregnancy, the concern is not the rash itself. The concern is that parvovirus B19 can infect the fetus and, in a small percentage of cases, interfere with fetal red blood cell production. This can lead to fetal anemia and sometimes hydrops fetalis (a serious condition where fluid builds up in fetal tissues).
Important context: even when a pregnant person is infected, most pregnancies still do well. Your OB’s goal is to identify the smaller group who would benefit from monitoring, so that if anemia develops, specialists can step in early. If you want numbers for your specific situation, your OB or MFM team can talk you through individualized risk based on timing and test results.
Exposure vs infection: the two questions your OB is trying to answer
1) Are you already immune?
Many adults were infected as kids and have lasting immunity. In fact, about 50 to 65% of adults are already immune. If you are immune, an exposure is usually just an unpleasant worry and an extra note in your chart.
2) If you are not immune, did you catch it this time?
If you are susceptible, your OB may test to see whether you have evidence of a recent infection. That helps determine whether you need additional monitoring.
Because symptoms can be mild or absent, testing is often based on exposure history rather than how you feel.
How risk changes with timing in pregnancy
When we talk about “timing,” we mean two things at once:
- Gestational age (how far along you are)
- How long it has been since exposure (which affects what blood tests can show)
Gestational age
Parvovirus-related fetal complications are most often discussed with infections in the first half of pregnancy, though issues can occur later as well. Your OB will individualize advice based on your exact week of pregnancy and your test results.
Timing after exposure
Right after an exposure, bloodwork may not show a new infection yet. That is why some patients have repeat labs a couple of weeks later if the first set does not clearly answer the question.
Parenting reality check: you are not expected to solve this puzzle yourself. Your job is to tell your OB when the exposure happened and how close the contact was. Their job is to pick the right tests and the right follow-up schedule.
A simple timeline
Exact schedules vary, but this is a common roadmap:
- Exposure (day 0): Call your OB, explain the contact, and ask about testing.
- Initial bloodwork (now): IgG and IgM (and sometimes PCR depending on your situation).
- Repeat bloodwork (about 1 to 2 weeks later): If the first set is negative but exposure was recent or high-likelihood.
- Ultrasound monitoring window: If recent infection is confirmed, many practices monitor with serial ultrasounds (often including MCA Dopplers) for a limited period, commonly up to about 8 to 12 weeks after infection, depending on local protocol and gestational age.
What testing your obstetrician may offer
Exact protocols vary by clinic and region, but these are the common tools.
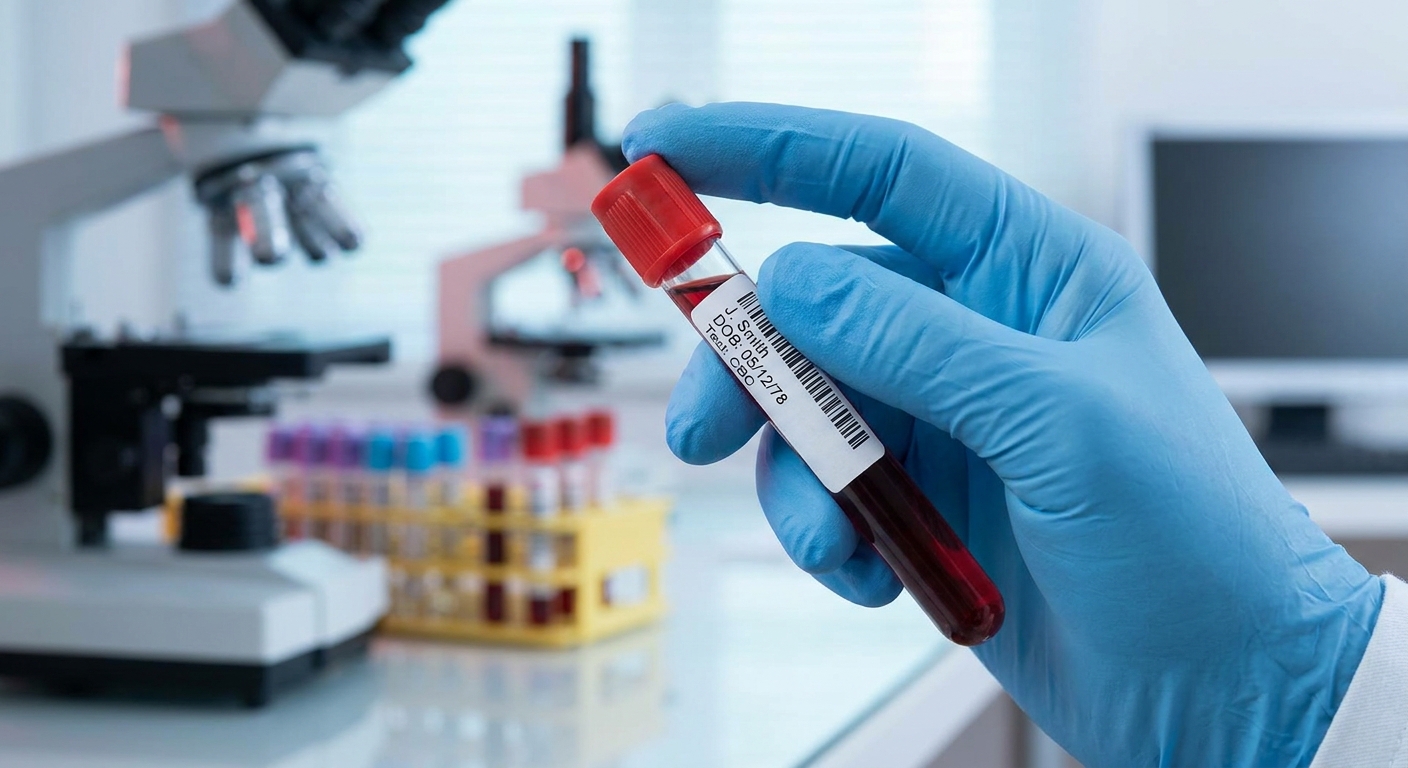
Blood tests: IgG and IgM antibodies
- Parvovirus B19 IgG: suggests past infection and immunity.
- Parvovirus B19 IgM: suggests recent infection. IgM can persist for months and can occasionally be falsely positive, so your OB may confirm with repeat testing and or PCR when results are unclear.
Your OB will interpret these together. The most common patterns are:
- IgG positive, IgM negative: usually indicates you are immune and not recently infected. Reassurance is common.
- IgG negative, IgM negative: suggests you are not immune and there is no evidence of recent infection yet. Your OB may repeat testing after a short interval if exposure was significant or recent.
- IgM positive (with or without IgG): can indicate a recent infection and may trigger additional fetal monitoring.
Sometimes results are borderline or do not fit neatly. In those cases, an OB may repeat antibodies or add other tests.
PCR testing (viral DNA)
Some clinicians use PCR (a test that looks for viral genetic material) in certain situations, especially when antibody results are unclear. Whether it is used depends on your local lab options and your specific clinical picture.
Who is usually reassured vs who is monitored?
Often reassured
- You are IgG positive (immune) and have no signs of recent infection
- You had a very low-risk exposure (for example, brief contact, no close household exposure), and testing is reassuring
If you are immune (IgG positive), you generally do not need repeat testing or ultrasound monitoring unless your OB has a specific concern or your results are unclear.
More likely to be monitored
- Confirmed recent infection (commonly IgM positive and/or supported by repeat testing)
- Susceptible (IgG negative) with a high-likelihood exposure, especially if exposure was within the last couple of weeks and initial labs may be too early
Monitoring is not a sign that something is wrong. It is a sign that your OB is being appropriately cautious with a known, time-limited risk window.
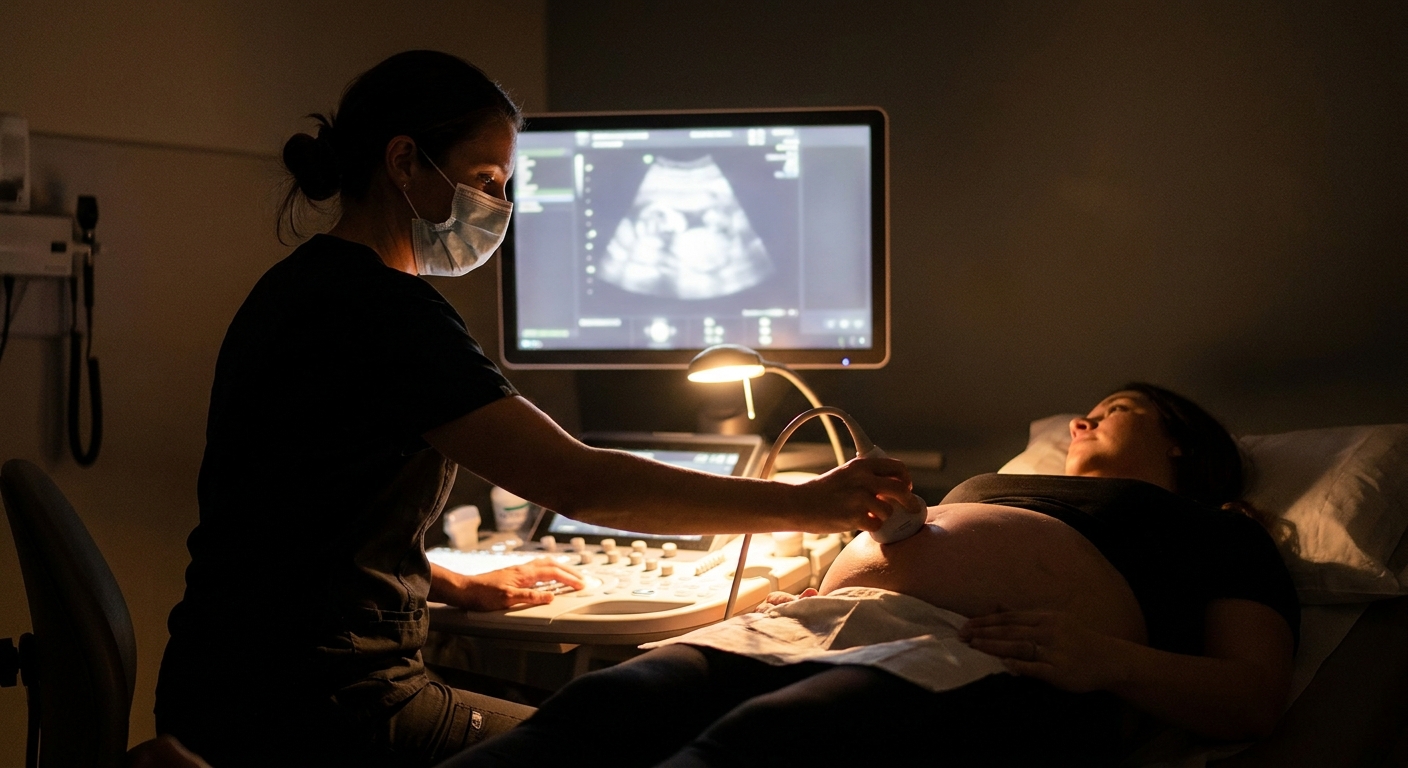
What monitoring can look like
If you have a confirmed recent infection, many obstetric teams recommend serial ultrasounds for a period of time (often several weeks). The exact schedule varies.
Ultrasound checks
Your ultrasound team may look for:
- Signs of hydrops (fluid in certain fetal spaces)
- Placental changes
- Growth and overall fetal well-being
Doppler ultrasound (MCA Doppler)
Many practices use a specialized Doppler measurement of blood flow in the baby’s brain called middle cerebral artery (MCA) Doppler. It is a noninvasive way to screen for fetal anemia. If MCA Dopplers suggest possible anemia, your OB may involve Maternal-Fetal Medicine (MFM) to discuss next steps.
What happens if fetal anemia is suspected?
Depending on gestational age and severity, MFM may discuss options such as:
- Closer monitoring
- Additional diagnostic testing
- Intrauterine transfusion in select cases at specialized centers
This is the part that sounds scary on Google, so let me say it plainly: this is not the most common outcome. The reason you hear about it is because it is the key complication we do not want to miss.
Symptoms in pregnant adults
Some pregnant people have no symptoms at all. Others get:
- Low-grade fever
- Runny nose or sore throat
- Fatigue
- Joint pain or swelling (hands, wrists, knees)
- A mild rash (less common than in children)
Call your OB if you develop symptoms after a known exposure, but also remember: symptoms alone cannot confirm or rule out infection. That is what testing is for.
What to ask your obstetrician
If you are sleep-deprived and anxious, here are questions that get you to a plan quickly:
- “Can we check parvovirus B19 IgG and IgM today?”
- “Based on when I was exposed, do we need repeat labs in 1 to 2 weeks?”
- “Am I considered immune?”
- “If results suggest a recent infection, what monitoring schedule do you use?”
- “Will you refer me to Maternal-Fetal Medicine, or do you manage the ultrasound monitoring in-office?”
- “Will you be using MCA Dopplers to screen for fetal anemia?”
- “For how many weeks after infection do you typically monitor?”
- “What symptoms should make me call right away?”
- “Do I need any work restrictions if I work with young children?”
If you work in a school, daycare, or healthcare setting, it is also reasonable to ask: “If I am not immune, what precautions make sense without completely disrupting my life?”
What you can do after exposure
1) Get clarity on the exposure
Was it close, prolonged contact (household, classroom aide, cuddling a sick toddler), or a brief interaction? If the child has a confirmed diagnosis from a clinician, note that too.
2) Call your OB and ask about testing
This is one of those times where “wait and see” is not as helpful as “test and see,” because immunity status changes the whole conversation.
3) Focus on what helps
Because parvovirus is mainly spread through respiratory droplets, prioritize:
- Handwashing, especially after wiping noses or handling tissues
- Avoiding face-touching (hard, but worth trying)
- Not sharing cups and keeping personal water bottles personal (secondary, but reasonable)
And skip the guilt. If you have preschoolers, you did not “fail” because a virus made it into your house. That is life with little kids.
4) Do not assume a rash means active contagiousness
Remember, contagiousness is often highest before the rash appears, and many children are no longer contagious once the rash is present. Decisions about work or school should be made with your OB and workplace policies.
Work and school notes
This is a frustrating virus from an outbreak-control perspective because people are often contagious before anyone realizes what it is. Exclusion policies vary, and keeping a child with a rash home does not always prevent spread since transmission may have already happened.
If you are pregnant and work with young children (or you have them at home), the most useful step is usually knowing your immunity status and following your OB’s testing plan if you are not immune. If your workplace has employee health, loop them in as well.
How this differs from fifth disease in kids
On the child side, fifth disease is usually a self-limited viral illness. Most kids just need:
- Fluids
- Rest
- Comfort care for fever or itchiness as advised by their clinician
In pregnancy, the focus shifts to:
- Determining immunity (IgG)
- Identifying possible recent infection (IgM and sometimes PCR)
- Monitoring the fetus for anemia or hydrops if infection is confirmed
Same virus, totally different playbook.
When to seek urgent care
Parvovirus exposure itself is usually handled through your OB’s office. Seek urgent medical advice if you have:
- Vaginal bleeding
- Severe abdominal pain
- Persistent high fever or you feel very unwell
- Signs of dehydration (unable to keep fluids down)
- Decreased fetal movement later in pregnancy (follow your OB’s guidance on kick counts)
If you are ever unsure, call. This is exactly what on-call lines are for.
A note for higher-risk situations
If you are immunocompromised or have certain blood disorders (for example, hemolytic anemias), parvovirus can behave differently. If that is you, call your OB promptly after a known exposure so they can tailor testing and follow-up.
A final note for parents with little kids at home
It is unfair, but true: the people most likely to be exposed in pregnancy are the ones doing the most hands-on caretaking. If your child has fifth disease, you do not need to panic-clean your whole house at 2 AM. Focus on basic hygiene, avoid sharing cups, and talk to your OB about testing and next steps.
You deserve information that is calm, accurate, and useful. You also deserve sleep. If you take nothing else from this article, take this: get the bloodwork, get a clear plan, and let your medical team carry the worry with you.
