Hand, Foot, and Mouth Disease in Babies
Sarah Mitchell
Sarah Mitchell is a Registered Pediatric Nurse and a mother of three who has spent over a decade helping families navigate the beautiful, chaotic early years of childhood. She combines evidence-based medical knowledge with real-world parenting experience to offer practical, compassionate advice. At Awesome Parent, Sarah's mission is to help exhausted parents find solutions, trust their instincts, and finally get some sleep.
If your baby has a fever, is drooling more than usual, and suddenly treats the bottle or breast like it is personally offending them, hand, foot, and mouth disease (HFMD) may be the culprit. And yes, it is unfair: babies cannot tell us their mouth hurts, so they show it by eating less, fussing more, and sleeping worse.
As a pediatric nurse and a mom of three, I want you to hear this up front: most cases are mild and pass on their own. The goal is not to “treat the virus.” It is to keep them comfortable and hydrated while their tiny mouth heals.

HFMD in babies, simply
HFMD is a common viral illness, most often caused by coxsackievirus or other enteroviruses. It spreads easily through saliva, mucus, stool, and fluid from blisters.
In toddlers, the classic pattern is fever first, then mouth sores, then a rash on hands and feet. In babies, it can be sneakier, because they cannot point to their throat or tell you it stings to swallow.
How babies often show it
- Fever (often the first sign)
- Feeding changes: pulling off the breast, taking a few sips then crying, refusing the bottle, shorter nursing sessions
- Extra drooling or chewing on everything more than usual
- Irritability, especially during feeds or when lying down
- Rash: spots or small blisters on the hands, feet, legs, diaper area, or trunk
- Fewer wet diapers if intake drops
Symptoms usually start about 3 to 6 days after exposure (some sources cite up to 7). Many babies feel most uncomfortable for the first 2 to 3 days, but the course can vary. Most improve gradually over a week.
What sores and rash look like
Mouth sores
These can be the biggest problem for babies because they interfere with sucking and swallowing. You might see:
- Small red spots on the tongue, gums, inside cheeks, or back of the throat
- Spots that turn into shallow ulcers that look whitish or yellow in the center
- Swollen, tender gums
Skin rash
HFMD rashes in babies are not always limited to hands and feet. It is common to see:
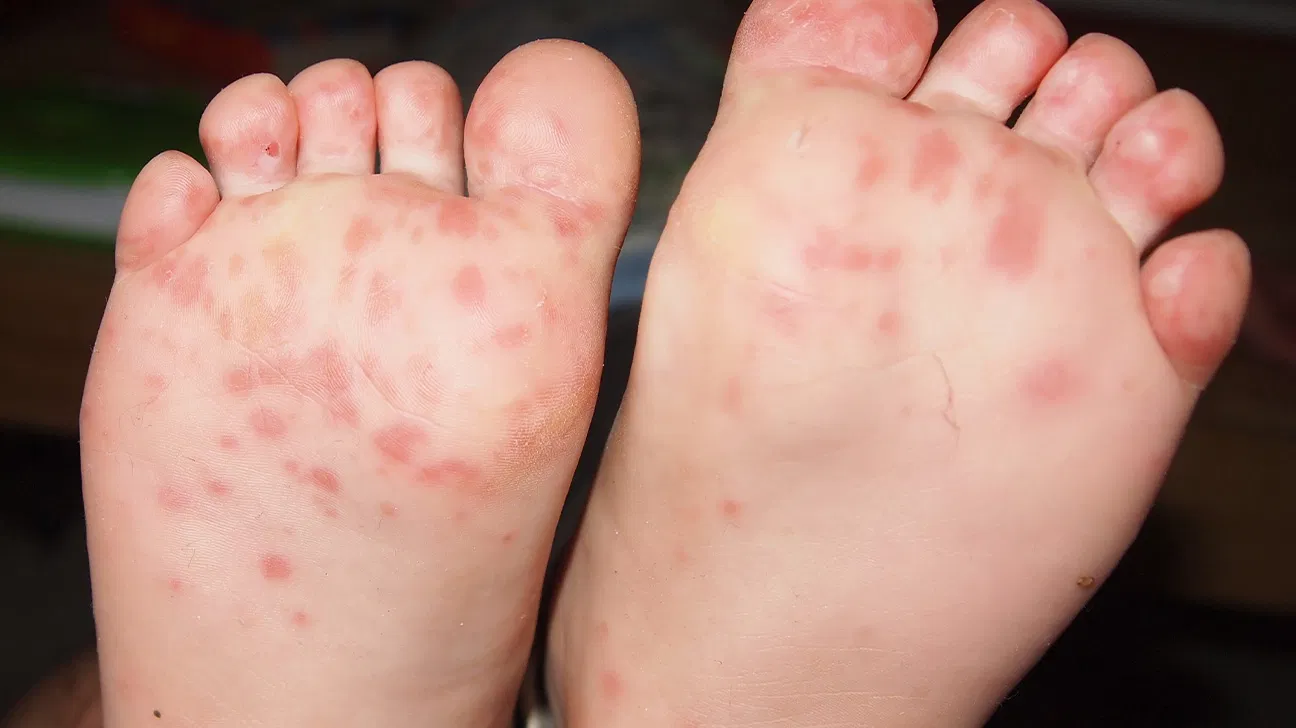
- Small red bumps or blisters on palms and soles
- Rash on knees, elbows, legs, or arms
- Diaper area rash that can look like severe diaper rash with small blisters
HFMD vs teething vs thrush
At 2 AM, everything looks like everything. Here are the most helpful differences:
- Teething: drooling and chewing, maybe a slight temperature bump, but typically not a true fever (not 100.4°F/38°C or higher) and no blisters on hands, feet, or diaper area.
- Thrush: white patches in the mouth that look like milk but do not wipe off easily and may leave a red, irritated base. Usually no hand/foot rash.
- HFMD: fever plus clear feeding pain signs, mouth ulcers, and rash or blisters somewhere on the body.
If you are unsure, a quick call or visit to your pediatrician is reasonable. For babies, feeding and hydration are usually the deciding factors.
Top goal: hydration
Babies can get dehydrated faster than toddlers, especially if mouth pain makes them refuse feeds. Your main job is to keep fluids going in small, frequent amounts.
Signs your baby is getting enough
- Wet diapers continue close to their normal pattern (what matters most is no big drop from baseline)
- Tears when crying (after the newborn stage)
- Moist mouth and tongue
- They perk up between uncomfortable spells
Signs dehydration may be starting
- Fewer wet diapers than usual (for many infants, fewer than about 6 wet diapers in 24 hours can be a concern, but age and baseline matter)
- Very dry lips or mouth
- No tears when crying
- Sunken soft spot (fontanelle)
- Sleepiness that feels unusual, hard to wake, or very weak cry
If dehydration signs are present, call your pediatrician the same day. If your baby is very sleepy, difficult to arouse, or not making wet diapers, that is urgent.
Feeding help for sore mouths
HFMD can turn a normally hungry baby into a tiny, furious critic of your entire feeding plan. These strategies often help.
For breastfed babies
- Offer more often, for shorter sessions. Think snack-style nursing.
- Try different positions. Upright or side-lying can reduce throat discomfort for some babies.
- Start when sleepy. Dream feeds can be easier when they are not fully awake and bracing for pain.
- If latch hurts due to mouth sores, ask your pediatrician about pain control timing so medication peaks before feeds.
For bottle-fed babies
- Smaller volumes more frequently can be more doable than full bottles.
- Check nipple flow. Too slow can frustrate a sore baby; too fast can trigger choking when they are refusing. Stick with what usually works unless your pediatrician suggests otherwise.
- Offer cool formula or cooled expressed milk if your baby accepts it and your pediatrician is comfortable with it. Some babies find cool liquids soothing.
What about water, juice, or electrolyte drinks?
- Under 6 months: typically stick with breast milk or formula unless your pediatrician directs otherwise.
- 6 months and up: your pediatrician may allow small sips of water in addition to usual feeds, but breast milk or formula is still the main hydration source.
- Oral rehydration solution: sometimes recommended if intake is low. Ask your pediatrician before using it in young infants.
Skip acidic liquids like citrus juices. They can sting mouth ulcers and backfire.

Fever: safe medication context
Fever can make babies miserable, and treating it can also improve feeding. But in infants, fever rules are different than for toddlers.
When fever needs a call right away
- Under 3 months: a rectal temperature of 100.4°F (38°C) or higher is an urgent call to your clinician, even if your baby otherwise looks okay.
- 3 to 6 months: call promptly for high fevers, fevers that persist, or if your baby seems very ill.
- Any age: call urgently if your baby has trouble breathing, a purple or blotchy rash, signs of dehydration, extreme sleepiness, or you cannot get them comfortable.
Medication basics (confirm dosing with your pediatrician)
- Acetaminophen (Tylenol) is commonly used in babies. Dose is based on current weight, not age.
- Ibuprofen (Motrin, Advil) is generally used only for babies 6 months and older, again weight-based.
- Avoid aspirin in children due to the risk of Reye syndrome.
If you do not have an up-to-date weight-based dose from your child’s clinician, call and ask. As a triage nurse, this is one of the most common and appropriate questions parents call about.
Comfort tip: If mouth pain is blocking feeding, giving a clinician-approved fever and pain medicine dose about 30 to 45 minutes before a feed can make a noticeable difference.
Mouth sore comfort (skip risky fixes)
Parents are often offered “quick fixes” online for HFMD mouth pain. Many are not safe for babies.
What you can do
- Cool, gentle feeds if your baby accepts them
- Upright cuddles and extra soothing, because pain can feel worse when lying flat
- Saline drops and gentle suction if nasal congestion is making feeding harder
- Keep nails short or use mittens if your baby scratches the rash
What to avoid
- Topical numbing gels (like benzocaine products): they can be unsafe in infants and can also increase choking risk by numbing the throat.
- Honey for soothing: not safe under 12 months due to botulism risk.
- Essential oils on skin or in the mouth: not recommended for babies, and some can cause irritation or toxicity.
There is no antibiotic that treats HFMD itself, because it is viral. Antibiotics are only used if a clinician thinks there is a secondary bacterial infection.
If your baby’s mouth seems extremely painful or they cannot take in enough fluid, your pediatrician can advise next steps. Sometimes the plan is simply tighter pain control and hydration support.
Skin care (including diaper area)
HFMD rash is usually self-limited, but baby skin can get angry quickly, especially under a diaper.
General rash comfort
- Lukewarm baths can soothe. Pat dry, do not rub.
- Loose, breathable clothing helps reduce friction.
- Keep blisters clean and intact when possible. Do not pop them.
Diaper area tips
- Frequent diaper changes to keep the area dry
- Thick barrier ointment (petrolatum or zinc oxide) to reduce irritation
- Warm water rinse instead of wipes if wipes sting

How contagious is HFMD?
HFMD spreads easily, especially in households with older siblings. Babies also put everything in their mouths, which is truly an impressive level of commitment to the germ-sharing lifestyle.
- Kids are often most contagious during the first week, especially with fever, new sores, and lots of secretions.
- Contagiousness is not zero later. Virus can still spread while there are open sores, and it can remain in stool for weeks even after symptoms improve.
- Exclusion does not always prevent spread, because kids can be contagious before you realize what it is.
Practical prevention that works
- Handwashing after diaper changes, before feeding, and after wiping noses
- Disinfect high-touch surfaces: doorknobs, light switches, changing table, toys
- Clean “goes-in-mouth” items often: pacifiers, bottle nipples, teethers (rotate spares if you have them)
- Launder drool-soaked bibs, burp cloths, and sheets on a regular cycle
- Do not share cups, utensils, pacifiers, teething toys
For childcare return rules, follow your daycare’s policy and your pediatrician’s advice. In general, exclusion is often based on fever, ability to participate, and whether drooling from mouth sores is uncontrolled. Since babies cannot control drool, the key practical markers are fever-free status and overall comfort.
When to call (or go in)
Trust your gut. Babies do not have much reserve, and it is always appropriate to call when feeding is affected.
Call the same day
- Your baby is taking significantly less milk than usual, or you cannot get enough in despite frequent attempts
- Wet diapers are decreasing compared to their normal
- Fever lasts more than 48 to 72 hours, keeps returning, or your baby seems worse
- The rash looks infected (increasing redness, warmth, swelling, pus)
- You are not sure it is HFMD and want an exam
Seek urgent care now
- Under 3 months with a rectal temp of 100.4°F (38°C) or higher
- Signs of dehydration: very few wet diapers, very dry mouth, unusual sleepiness
- Breathing difficulty, persistent vomiting, or your baby looks very ill
- Inconsolable crying that does not improve, a stiff neck, or new weakness
When it might be something else
HFMD is common, but babies can look similar with other infections. Call your pediatrician promptly if:
- There are significant mouth ulcers with no rash (could be a related enterovirus pattern like herpangina)
- The rash becomes honey-crusted or rapidly spreads (possible impetigo)
- There are clustered blisters in the diaper area with fever, or your baby seems very uncomfortable during diaper changes (HSV is uncommon but important to rule out in infants)
- Your baby seems unusually sleepy, weak, or hard to wake (rare complications are possible and should be assessed)
How this differs from toddlers
If you have read toddler-focused HFMD articles, you will notice the baby version is less about “keeping them from touching everything” and more about feeding, hydration, and fever safety.
- Babies cannot tell you where it hurts, so feeding behavior becomes a key symptom.
- Medication decisions are more age-sensitive, especially under 6 months.
- Dehydration risk is higher because babies rely on milk feeds and may refuse them with mouth pain.
- Return-to-daycare rules can be trickier for infants due to drooling and constant mouthing.
What recovery looks like
Most babies start to improve within a few days, even if the rash takes longer to fade. Timelines vary, but this is a common pattern:
- Days 1 to 3: fever and fussiness often peak, feeding is hardest
- Days 3 to 5: mouth pain often begins easing, intake improves
- Days 7 to 10: rash and spots resolve for many kids
A small number of children later develop peeling skin on hands or feet or may lose a fingernail or toenail 3 to 8 weeks after HFMD. It looks alarming but is usually temporary. Mention it to your pediatrician if it happens.
My nurse-mom bottom line: If your baby is peeing close to normal, sipping milk more often even in small amounts, and has moments of calm between cranky stretches, you are likely on the right track. If feeding is falling off or wet diapers are dropping, call. You are not overreacting. You are parenting.