Henoch-Schönlein Purpura (HSP) in Kids
Sarah Mitchell
Sarah Mitchell is a Registered Pediatric Nurse and a mother of three who has spent over a decade helping families navigate the beautiful, chaotic early years of childhood. She combines evidence-based medical knowledge with real-world parenting experience to offer practical, compassionate advice. At Awesome Parent, Sarah's mission is to help exhausted parents find solutions, trust their instincts, and finally get some sleep.
If your child has a sudden purple rash on their legs and now they are limping, complaining of knee or ankle pain, or holding their belly like it hurts, it is completely normal to feel alarmed. One condition that can cause this specific trio is Henoch-Schönlein Purpura, often shortened to HSP.
You may also hear clinicians call it IgA vasculitis. It is the same condition, just the newer name that you might see on discharge papers or in your child’s chart.
As a pediatric nurse, I saw HSP most often after a typical cold. As a mom, I can tell you this is exactly the kind of symptom combo that sends you to the bathroom with your phone at 2 a.m. You are not overreacting. The good news is that most kids recover fully with supportive care and close follow-up, but there are a few red flags that deserve urgent evaluation.
What is HSP?
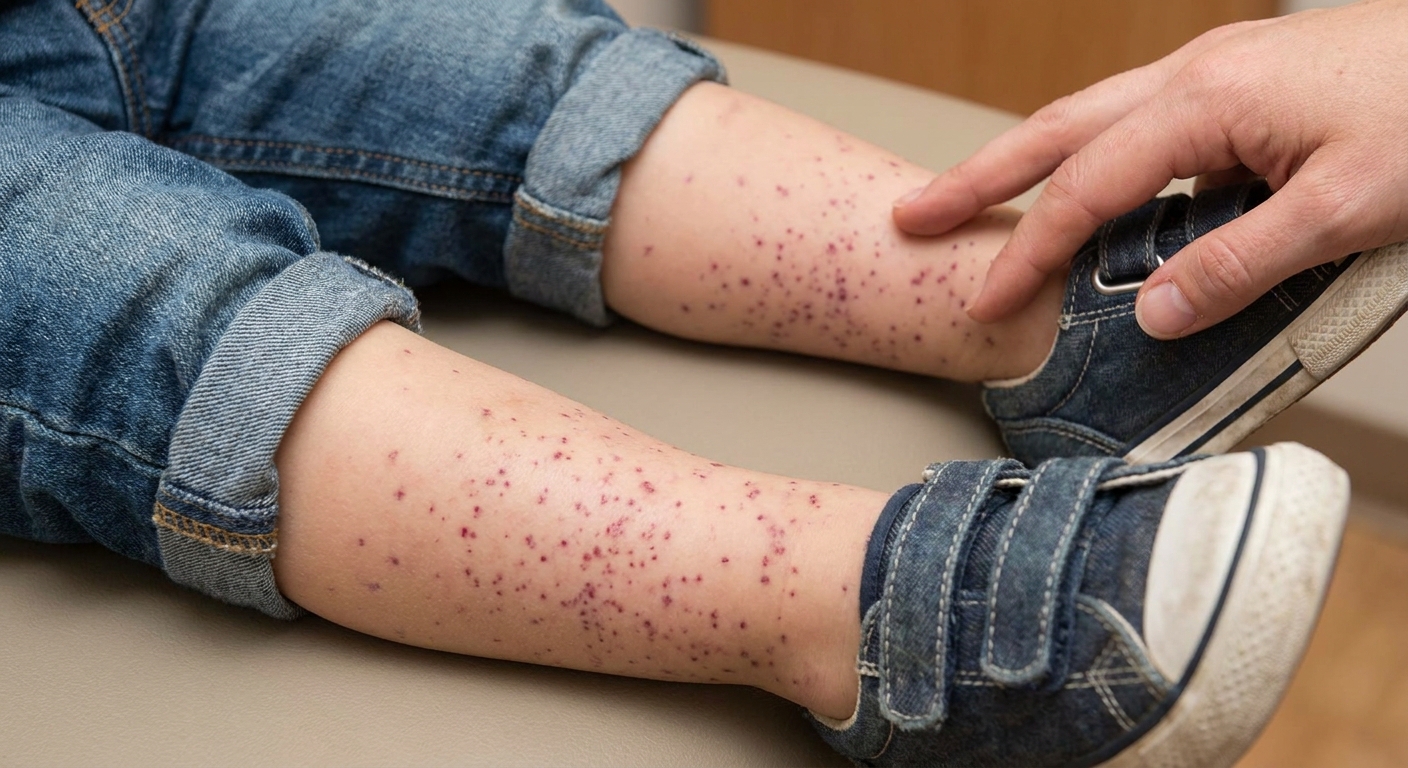
HSP (IgA vasculitis) is a type of inflammation of tiny blood vessels. When those small vessels get irritated, they can leak a bit under the skin, which creates the telltale purple spots. That same process can also affect joints (causing pain and swelling) and the intestines (causing belly pain and sometimes bleeding).
HSP is most common in kids, especially ages 2 to 10. It often shows up after a viral illness like a cold, and sometimes after strep throat.
The HSP rash
The rash is usually the clue that makes clinicians think “HSP.” It has a very particular look and location.
What it looks like
- Purple, red, or bruise-like spots (purpura)
- Raised spots you can feel if you run a finger over them (palpable purpura)
- Can start as small pinpoints and then cluster
- May look like bruises, but often appear in many spots at once
Where it shows up
- Most often on the lower legs, especially shins and around the ankles
- Common on the buttocks
- Can also appear on elbows or upper extremities
- Less commonly on the trunk
Helpful home check: Many rashes blanch (turn pale) when you press on them. Purpura often does not blanch because the blood is under the skin, but early spots can sometimes partially blanch. This is not a diagnosis by itself, but a new purplish rash that does not fade with pressure is a reason to call your child’s clinician promptly.
Joint pain and limping
Joint symptoms are very common with HSP. Parents often tell me their child woke up and suddenly did not want to walk, or they were limping by afternoon.
- Most often affects knees and ankles
- Can cause swelling, warmth, and tenderness
- Pain can come and go over days
Even when the limp looks dramatic, HSP joint inflammation typically resolves without long-term damage. Rarely, symptoms can linger longer than expected, so keep your clinician in the loop if the pain is not improving.
Belly pain: what is normal and what is not
Abdominal pain is another classic HSP symptom. It can range from mild cramping to more intense pain that makes a child curl up or refuse food. Some kids also have nausea, vomiting, or diarrhea.
Why the stomach hurts
Inflammation can also involve the lining of the intestines. That can cause swelling and, sometimes, bleeding.
A complication to know
In a smaller number of kids, HSP can trigger a “telescoping” of the intestines called intussusception. This is one reason an ultrasound may be ordered, and why sudden, severe cramping belly pain is treated as urgent.
Call urgently or go to the ED if belly symptoms include
- Severe, persistent abdominal pain
- Sudden, intense cramping that comes in waves, especially if your child looks pale or very distressed
- Vomiting that prevents drinking or signs of dehydration
- Blood in stool or black, tarry stool
- Swollen, very tender abdomen or your child looks significantly ill
- Testicle pain or swelling in boys (needs same-day evaluation)

How HSP is diagnosed
HSP is often diagnosed based on the pattern of symptoms and a physical exam. Your child’s clinician may also order tests to rule out other causes and to check for complications.
Common tests
- Urine test to look for blood or protein
- Blood pressure check
- Sometimes blood work to assess inflammation, blood counts, and kidney function
- Sometimes stool testing if there are signs of intestinal bleeding
- Occasionally an ultrasound if abdominal pain is significant, especially to check for complications like intussusception
In many cases, kids do not need extensive testing on day one if they are stable, but they do need a plan for follow-up.
Home care: what you can do tonight
Most HSP care is supportive, meaning we focus on comfort and monitoring while the body heals.
Hydration matters
- Offer small, frequent sips if nausea is present
- Use water, oral rehydration solution, soups, or popsicles
- Aim for steady urination and light-yellow urine
Rest and leg comfort
- Encourage rest during painful days
- Elevate legs if swelling is uncomfortable
- Loose clothing can help if the rash is tender
Pain control
Ask your child’s clinician which medicines are appropriate. NSAIDs (like ibuprofen) are often used for joint pain when kidney function is normal and there is no concern for gastrointestinal bleeding. Acetaminophen is often preferred when there are kidney concerns or bleeding risk. Do not guess here, especially if belly pain is significant or there is any blood in stool.
Practical mom note: If your child is limping, set up a “pillow nest” and bring the essentials to them for a day or two. This is not the time to win a screen-time award.
Medical treatment you may hear about
Some children, especially those with significant belly pain or joint swelling, are treated with corticosteroids (like prednisone). Steroids can help symptoms for some kids, but they are not a guarantee against kidney involvement. That is why follow-up urine and blood pressure checks still matter even if your child feels better quickly.
When to go to the ER
Trust your gut. If your child looks very ill, you are always allowed to get urgent help. In general, HSP deserves same-day medical evaluation if it is newly suspected, and emergency evaluation if any of the following are present:
- Severe abdominal pain, guarding, or pain that will not let your child stand up straight
- Sudden, intense cramping belly pain (possible intussusception)
- Repeated vomiting or inability to keep fluids down
- Blood in stool or vomit
- Very decreased urination, marked swelling of face or legs, or signs of dehydration (dry mouth, no tears, unusual sleepiness)
- Severe headache, confusion, fainting, or neck stiffness
- Shortness of breath or trouble breathing
- One leg suddenly much more swollen or painful than the other
- Testicle pain or swelling in boys
The kidney piece, in plain language
This is the part parents deserve a clear explanation of, without scary jargon.
In some kids, HSP inflammation also affects the kidneys. Many children never have a kidney problem. When it does happen, it often shows up as tiny amounts of blood or protein in the urine that you cannot see with your eyes. That is why follow-up urine tests matter even if your child seems better.
What kidney monitoring usually includes
- Urine checks (at the clinic) for blood and protein
- Blood pressure checks
- Sometimes blood tests if urine results are abnormal
How long do we watch?
Follow your clinician’s schedule, but monitoring commonly continues for about 6 months, and in some cases up to 12 months, because kidney changes can appear later even after the rash fades.
Call your clinician promptly if you notice
- Tea-colored or red urine
- New puffiness around the eyes, hands, or feet
- New headaches, dizziness, or high blood pressure readings if you check at home
- Your child seems unusually tired or unwell after the initial illness improves
How long does HSP last?
The rash and aches often improve over a few weeks, but symptoms can come and go. A common pattern is that the rash lasts about 1 to 4 weeks, with possible flares in the first few months. Some kids have recurrences where the rash returns after running around a lot or after another minor illness. That can be unsettling, but it is not always an emergency. It is a reason to update your child’s clinician and keep follow-up appointments.
School, sports, and activity
Most kids can return to school when they feel well enough, are drinking, and pain is controlled. Sports and high-impact activity usually wait until joint pain and swelling are clearly improving. Your clinician can help you decide what makes sense for your child.
Is it contagious?
HSP itself is not contagious. The cold or virus that triggered it can be, so follow your usual “sick day” hygiene rules at home.
What else can look like HSP?
Because HSP involves purpura, it is important not to assume every purple rash is “just HSP.” Other conditions can also cause non-blanching spots and can be more urgent.
Seek same-day medical advice if your child has a new purplish rash plus fever, appears very sick, has neck stiffness, or you are worried about a serious infection or a blood or clotting problem. Examples clinicians consider include meningococcal infection/sepsis, ITP (low platelets), and other less common blood disorders. In triage, we treat those combinations seriously until proven otherwise.
Questions to ask
- Does this rash pattern look like HSP (IgA vasculitis) to you?
- Do we need a urine test today?
- How often should we recheck urine and blood pressure, and for how many months?
- What pain medicine is safest for my child right now?
- Would steroids help in our case, and what would they help (or not help)?
- What belly pain symptoms would make you want an ER visit?
- When can my child return to school and sports?
A final reassurance
HSP can look dramatic and feel miserable, but most children recover fully. Your job is not to diagnose it perfectly at home. Your job is to notice the pattern, support hydration and comfort, and get the right level of care quickly when symptoms cross into the danger zone.
If you are staring at your child’s legs under the hallway light right now, wondering if you should go in, my nurse-brain and mom-heart agree on this: if the rash is purplish and your child has belly pain, joint pain, or is not acting like themselves, it is worth being seen today.
Sources
- American Academy of Pediatrics, HealthyChildren.org: Vasculitis and purpura topics and guidance for families
- Mayo Clinic: Henoch-Schönlein purpura (IgA vasculitis) overview
- UpToDate: IgA vasculitis (Henoch-Schönlein purpura) in children (professional clinical summary used for background)
- EULAR/PRINTO/PRES: Classification criteria for IgA vasculitis (Henoch-Schönlein purpura) in children
- National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK): Kidney health and urine protein basics