Herpangina in Toddlers
Sarah Mitchell
Sarah Mitchell is a Registered Pediatric Nurse and a mother of three who has spent over a decade helping families navigate the beautiful, chaotic early years of childhood. She combines evidence-based medical knowledge with real-world parenting experience to offer practical, compassionate advice. At Awesome Parent, Sarah's mission is to help exhausted parents find solutions, trust their instincts, and finally get some sleep.
If your toddler suddenly spikes a fever and then refuses their favorite foods like you served them betrayal on a plate, herpangina might be the reason. It is a common childhood viral illness that causes painful blisters and ulcers toward the back of the mouth, often with a pretty miserable sore throat.
As a pediatric nurse and a mom, I will tell you the reassuring part up front: herpangina is usually self-limited. The big goals are pain control and hydration, plus knowing the red flags that mean it is time to be seen.

What it is
Herpangina is most often caused by enteroviruses, commonly coxsackievirus. It tends to show up in the warmer months but can happen any time of year, especially in daycare and preschool settings.
It spreads through respiratory secretions (cough and sneeze), saliva, and stool, and also by touching contaminated hands and surfaces. Translation: toddlers share it enthusiastically.
Symptoms
Herpangina usually comes on fast. Many parents tell me, “They were fine at breakfast and miserable by lunch.” Common symptoms include:
- Fever, often high at the start
- Sore throat and pain with swallowing
- Decreased appetite and drinking less than usual
- Drooling (often because swallowing hurts, not because something is stuck)
- Fussiness, poor sleep, “clingy” behavior
- Sometimes headache, tummy pain, or vomiting
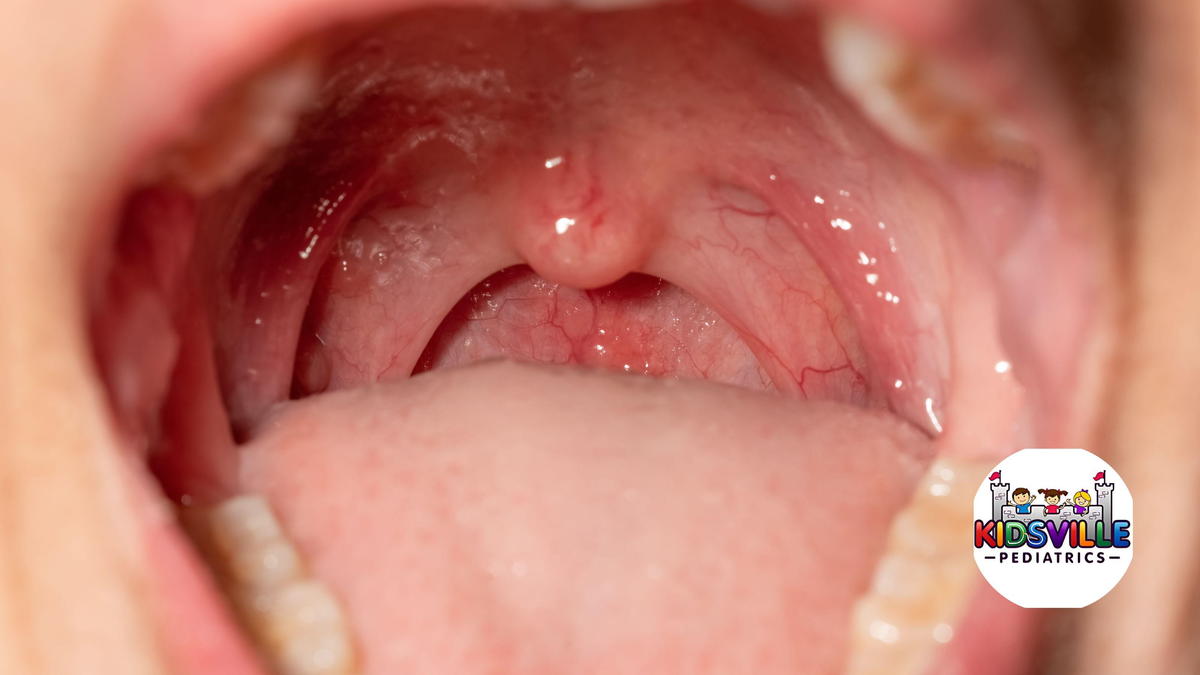
The signature finding is in the mouth: small blisters that turn into shallow ulcers.
Mouth sores
In herpangina, the sores typically show up in the back of the mouth:
- Soft palate (the soft part at the back of the roof of the mouth)
- Tonsillar pillars
- Uvula (the little dangly part)
- Back of the throat
They often look like tiny gray-white blisters or ulcers with a red rim. There might only be a few, or there can be a cluster.
Herpangina vs HFMD
These two get mixed up constantly because they can be caused by similar viruses and both can involve mouth sores. The pattern is usually what separates them.
Herpangina
- Sores are mostly back of the mouth and throat
- No rash on hands and feet in many cases
- Can start with a high fever
HFMD
- Mouth sores can happen, but many kids also get sores more toward the front of the mouth
- Often includes a rash or blisters on hands, feet, and sometimes buttocks
- Fever varies depending on the virus strain
Real life note: some kids get overlap, and not every case reads the textbook. If you are unsure, focus on hydration and pain control either way and call your pediatrician if you are worried.
How it is diagnosed
Most of the time, clinicians diagnose herpangina by history and exam, meaning symptoms plus where the sores are. Testing is rarely needed unless your child is very ill, immunocompromised, there is an outbreak setting, or the diagnosis is unclear.
How long it lasts
Most toddlers start to turn the corner within a few days. Typical patterns look like this:
- Fever: often 1 to 3 days, sometimes a bit longer
- Mouth pain and ulcers: often 3 to 7 days
- Energy and appetite: can lag behind for a few extra days
If your child is still having significant symptoms beyond a week, or the fever returns after improving, it is worth a call.
Pain relief
When it hurts to swallow, toddlers protect themselves by refusing everything, including water. So pain relief is not “extra”. It is one of the best ways to prevent dehydration.
1) Use the right medicine
- Acetaminophen (Tylenol) or ibuprofen (Motrin, Advil) can reduce fever and throat pain.
- Follow weight-based dosing on the label or what your pediatrician gave you.
- For the first 24 to 48 hours, many families do best giving doses regularly while awake, rather than waiting until the pain is severe.
Do not give aspirin to children. And do not use ibuprofen under 6 months unless your clinician tells you to.
2) Cold and soft foods
- Popsicles, ice chips (if age-appropriate and safe), slushies
- Yogurt, smoothies, pudding, applesauce
- Chilled soup broths
Avoid acidic or spicy foods that sting, like orange juice, tomato sauce, and salsa.
3) Skip numbing gels
I caution parents about over-the-counter mouth-numbing gels or sprays, especially in toddlers. They can be hard to dose safely and may increase choking risk by numbing the throat.
A special note on benzocaine products: they are not recommended for young children because of a rare but serious risk called methemoglobinemia. Also, viscous lidocaine is generally not used for routine sore throat or mouth ulcers without clinician guidance. If you are considering anything topical, check with your pediatrician first.
Hydration
Your mission is simple: keep fluids going in small, frequent sips. Toddlers with sore mouths usually do better with “tiny amounts, often” than big cups that feel overwhelming.
Best fluids
- Water (cool or cold often feels better)
- Oral rehydration solution (like Pedialyte) if they are drinking very little
- Milk is fine if they will take it, but some kids find it irritating when their throat is very sore
- Popsicles and smoothies count as fluids
How much pee is enough?
A practical home check: urine should stay a pale yellow, not dark like apple juice. For many toddlers, a common rule of thumb is at least one good wet diaper or pee about every 6 to 8 hours. Fewer wet diapers over the day, very small amounts, or dark urine can mean they are falling behind.
Drooling
Drooling is common with herpangina because swallowing hurts. That is annoying but not automatically dangerous.
Call your pediatrician urgently or seek same-day care if drooling comes with:
- Trouble breathing, noisy breathing, or wheezing
- Inability to swallow even small sips
- Muffled “hot potato” voice, neck stiffness, or severe one-sided throat pain
- Jaw pain or difficulty opening the mouth
- Signs of dehydration (below)
These can suggest more than a typical viral sore throat.
Dehydration red flags
This is the main reason toddlers with herpangina end up needing an urgent visit.
Seek care now if your child has
- No wet diaper or pee for 8 hours (or very minimal urine)
- Very dry mouth, cracked lips
- No tears when crying
- Sunken eyes or a sunken soft spot (in infants)
- Extreme sleepiness, hard to wake, or unusually weak
- Persistent vomiting or cannot keep fluids down
If you are on the fence, call. A quick check can prevent a longer, harder illness.
What else could it be?
Not every sore throat with mouth pain is herpangina. Call your pediatrician if symptoms do not fit, your child seems worse than expected, or you are seeing any of the red flags above. A few look-alikes:
- Strep throat (more common in older kids): fever, sore throat, sometimes belly pain, usually no cough. It does not typically cause blisters in the back of the mouth.
- HSV gingivostomatitis: very painful sores more toward the front of the mouth plus swollen, bleeding gums, and it can last longer.
- Thrush: white patches that wipe off and leave a raw surface, more common in babies.
- Canker sores: a few isolated ulcers, usually without high fever.
- Deep throat infections (like peritonsillar or retropharyngeal abscess): severe one-sided pain, hot potato voice, drooling, neck stiffness, or trouble opening the mouth. These need prompt evaluation.
Contagious period
Herpangina is most contagious in the first few days of illness, especially while fever is present. However, the virus can be shed longer, including in stool for weeks.
Most childcare policies follow practical rules:
- Keep your child home until they are fever-free for 24 hours without fever-reducing medicine
- They should be drinking reasonably well and able to participate
Even after return, good handwashing matters a lot, especially after diaper changes and before meals.
Prevention
You cannot prevent every virus, but you can lower the spread:
- Wash hands after diaper changes, wiping noses, and before eating
- Clean high-touch surfaces and shared toys regularly
- Avoid sharing cups, utensils, and toothbrushes during illness
When to call the doctor
Call your pediatrician if:
- Your toddler is under 6 months old and has fever or mouth sores
- Fever lasts more than 3 days or is very high for age
- Your child has significant trouble drinking or you suspect dehydration
- Pain is not controlled with appropriate acetaminophen or ibuprofen dosing
- You see a new rash and want help sorting out HFMD vs other illnesses
- Your child is immunocompromised or has complex medical needs
Seek urgent or emergency care for breathing trouble, bluish lips, severe lethargy, signs of severe dehydration, or if your parent gut says something is off.
What to do tonight
If it is 2 a.m. and everyone is unhappy, here is your simple plan:
- Give weight-based acetaminophen or ibuprofen (whichever you use safely for your child)
- Offer small sips every few minutes, or a popsicle if they will take it
- Stick to cool, soft foods and skip acidic drinks
- Watch urine output and energy level, not just the thermometer
- Plan a pediatrician call if drinking is still poor by morning
Herpangina can look dramatic because mouth pain is no joke. But with hydration support and steady pain control, most toddlers bounce back faster than you expect.