Impetigo in Kids: What It Looks Like and How to Stop It Spreading
Sarah Mitchell
Sarah Mitchell is a Registered Pediatric Nurse and a mother of three who has spent over a decade helping families navigate the beautiful, chaotic early years of childhood. She combines evidence-based medical knowledge with real-world parenting experience to offer practical, compassionate advice. At Awesome Parent, Sarah's mission is to help exhausted parents find solutions, trust their instincts, and finally get some sleep.
If you have noticed a patch of red, oozing skin on your child that suddenly turned into a sticky, golden crust, you are not alone. Impetigo is a very common skin infection in kids, especially preschoolers, and it spreads fast in the real world of daycare cubbies, shared dress-up clothes, and constant face touching.
The good news: impetigo is very treatable, and most kids feel better quickly once treatment starts. The key is recognizing it early and tightening up hygiene at home so it does not boomerang back around your family.
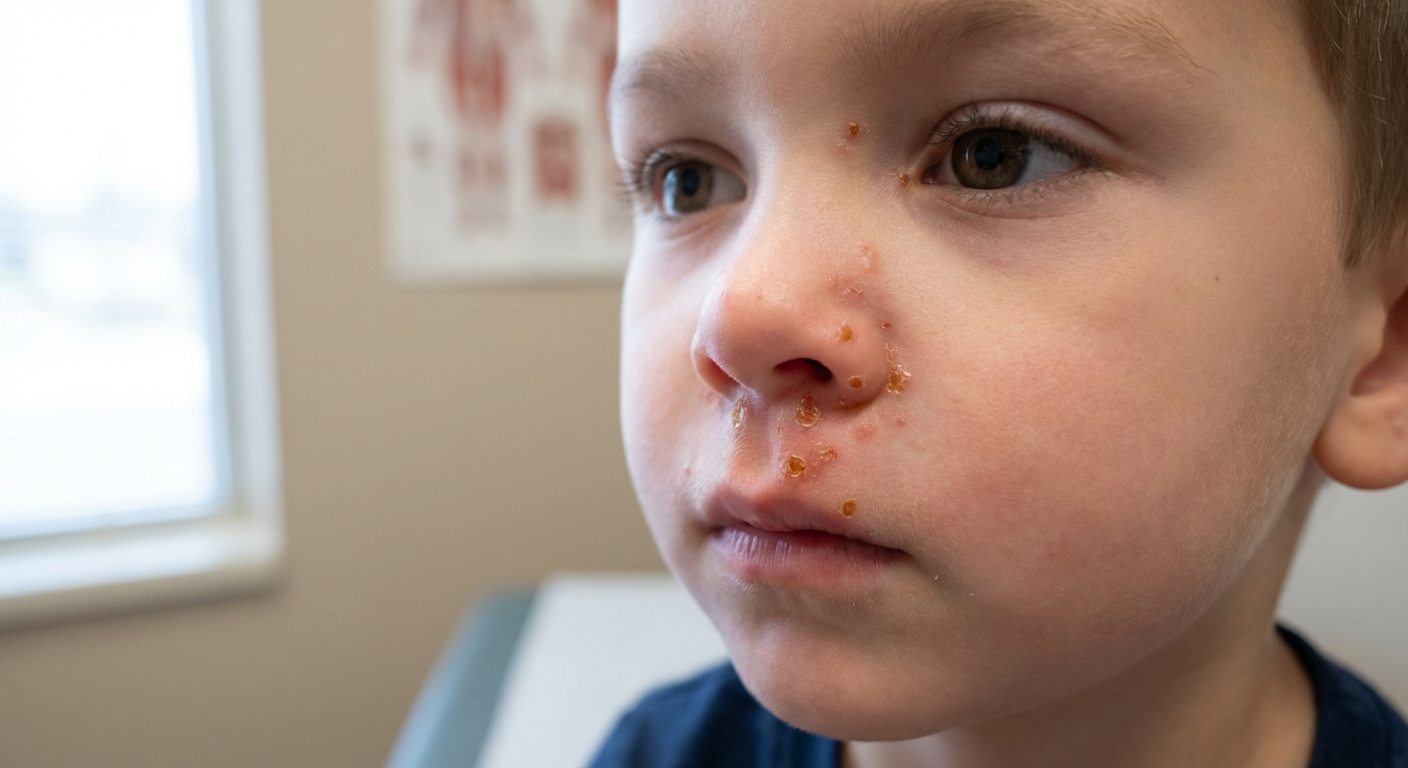
What impetigo looks like
Impetigo is a bacterial infection of the top layer of skin. It is most often caused by Staph (Staphylococcus aureus) or Strep (Group A Streptococcus). It loves places where skin gets irritated or broken, like around the nose and mouth after a runny cold, or on legs after bug bites.
Classic signs parents notice
- Red sores or bumps that may look like pimples, small blisters, or a rashy patch
- Oozing or weeping (clear fluid or pus)
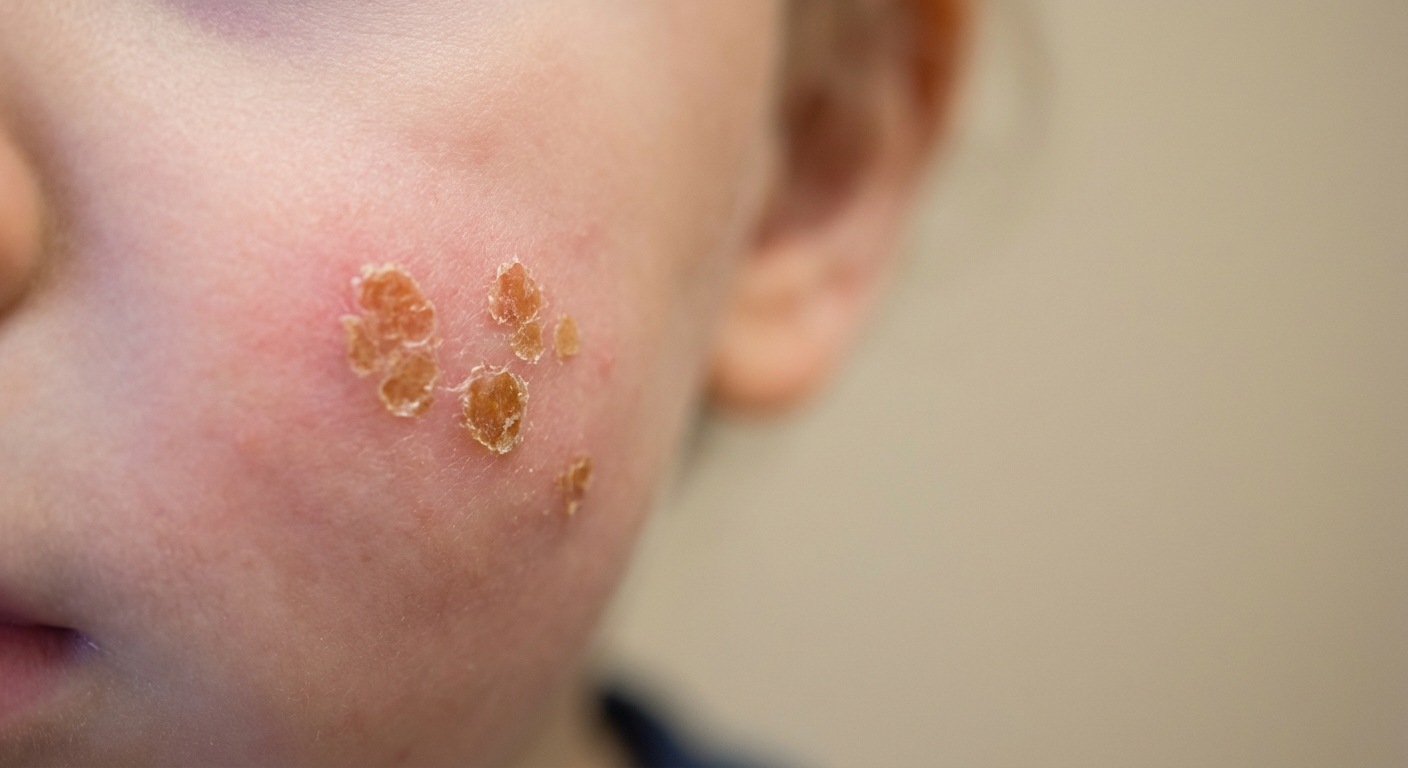
- Honey-colored crust as it dries, often described as golden, sticky, or “cornflake-like”
- Itchiness is common; pain is usually mild, but the area can feel tender
- Spreading clusters that seem to pop up nearby over a day or two
Where it shows up most
- Around the nose and mouth (especially after colds and constant wiping)
- On the hands and arms
- On the legs (often after scrapes or insect bites)
- In areas with eczema or frequent irritation
Non-bullous vs bullous
- Non-bullous impetigo is the most common and causes small blisters or sores that break open and form the honey crust.
- Bullous impetigo causes larger, fluid-filled blisters that can look like a “burn blister.” These can break and leave a shiny raw patch with a rim of scale.
If you are unsure whether you are looking at impetigo or something else, it is worth getting eyes on it. Many rashes overlap, and the treatment plan changes depending on the cause.
How it spreads
Impetigo spreads through direct skin-to-skin contact and through shared items that carry bacteria from one child to another. Kids also spread it to themselves by scratching, touching, and then touching another spot.
Common ways it spreads
- Touching the infected area, then touching another child
- Sharing towels, washcloths, bedding, or blankets
- Sharing clothing (especially hats, dress-up clothes, sports gear)
- Shared personal items like hairbrushes or bar soap
- Scratching itchy skin, bug bites, or eczema patches (breaks in the skin make an easy entry point)
Impetigo can start after something as simple as a runny nose that irritates the skin. The bacteria take advantage of that raw, damp area and multiply quickly.
How long it is contagious
In general, kids are usually much less contagious after about 24 hours of effective antibiotics. Without treatment, impetigo can stay contagious longer, especially while sores are open and weeping.
When to call the pediatrician
Most impetigo can be handled with a routine call or visit, but you should reach out sooner rather than later because treatment helps stop the spread.
Call your child’s clinician if
- You see the honey-colored crust or rapidly spreading sores
- The rash is near the eyes, especially with swelling
- Your child has multiple spots or it is spreading over a larger area
- Your child has fever or seems more ill than you would expect from a skin infection
- The area is getting more painful, hot, swollen, or red is spreading outward
- Your child has eczema and the skin looks suddenly infected
- No improvement within 48 hours of starting treatment
Go to urgent care now if
- Rapidly worsening redness with significant pain
- Red streaking moving away from the sores
- Swelling or infection around the eye, trouble opening the eye, or vision changes
- Your child is a newborn or young infant with suspected impetigo
If your child is immunocompromised or has a history of MRSA skin infections, mention that. It can affect antibiotic choice.
Possible complications (rare, but worth knowing)
Most kids heal without issues. Occasionally, bacteria can spread deeper and cause cellulitis (a more painful, hot, spreading redness). Very rarely, certain Strep-related skin infections are associated with post-streptococcal glomerulonephritis (a kidney complication). This is uncommon, and it is not meant to scare you, but it is one reason clinicians take bacterial skin infections seriously and treat them promptly.
Treatment options
Because impetigo is bacterial, treatment usually involves antibiotics. Exactly which type depends on how widespread it is, where it is located, and your child’s overall health.
Topical antibiotics
If the infection is limited to a small area, clinicians often prescribe a topical antibiotic ointment such as mupirocin or another appropriate option based on local resistance patterns.
- Often used for 5 to 7 days (follow your prescription directions)
- Works best when you gently remove crusts first (more on that below)
- Helps reduce contagiousness once treatment begins
Oral antibiotics
If there are multiple lesions, rapid spread, bullous impetigo, or involvement in tricky areas, an oral antibiotic may be recommended.
- Commonly used medications vary by region and your child’s history
- Finish the full course, even if the skin looks better quickly
- Ask your clinician what to do if your child vomits a dose or refuses medication
What about MRSA?
Some communities see more MRSA (methicillin-resistant Staph aureus). If MRSA is a concern based on local rates, outbreak patterns, or your child’s history, your clinician may choose an antibiotic that covers it.
Do we need testing?
Impetigo is often diagnosed by how it looks. A swab culture may be used in some situations, like outbreaks, recurrent infections, treatment failure, or when MRSA is a strong concern.
What not to do
- Do not use leftover antibiotics from a prior illness.
- Do not pick or scrub aggressively. That irritates skin and can spread bacteria.
- Do not rely on “natural” topical remedies as a substitute for antibiotics when impetigo is suspected. Delaying appropriate treatment is one of the biggest reasons it spreads.
At-home care
Think of home care as doing two jobs: helping the skin heal, and lowering the odds that bacteria get carried to other people or other parts of your child’s body.
Step 1: Soften crusts
Crusts can block topical medicine from reaching the skin. Before applying ointment:
- Wash your hands.
- Soak the area with a warm, wet washcloth for a few minutes.
- Gently wipe away loosened crust. Do not scrub.
- Pat dry with a clean towel or paper towel.
Step 2: Apply medicine
- Use a clean finger or cotton swab.
- A thin layer is usually enough.
- Wash hands again after applying.
Step 3: Cover if you can
If the area is on an arm or leg and your child tends to touch it, a light bandage can help reduce spread. You do not need to wrap the child like a mummy. Just cover the spots that are likely to be touched or rubbed.
Step 4: Manage itching
Keeping nails short and clean helps a lot. Ask your clinician if an age-appropriate antihistamine is okay if itching is intense, especially at night.

Stop it spreading at home
This is the part that feels annoying when you are already tired, but it matters. Many repeat infections happen because bacteria are still hanging out on hands, towels, bedding, and under fingernails.
Hygiene checklist (48 to 72 hours)
- Handwashing for everyone, especially after touching the child’s face, nose, or bandages.
- Separate towels and washcloths. Use fresh ones daily if you can.
- Change pillowcases and consider changing sheets, especially if sores are on the face.
- Wash clothing that touches the lesions. Warm or hot water is helpful when fabrics allow.
- Do not share hats, hairbrushes, sports gear, or dress-up clothing until cleared.
- Keep nails short and clean. Consider socks or mittens for sleep for toddlers who scratch unconsciously.
- Clean high-touch surfaces like bathroom counters, faucets, and doorknobs routinely.
Do we need to wash toys and stuffed animals?
If your child has been snuggling it, yes, it is reasonable to clean it. Launder what you can (stuffed animals, blankets) and wipe down hard toys. Focus on the items your child touches the most, not every single thing in your house.
If more than one family member develops similar sores, call your clinician. Sometimes households need a coordinated plan.
Back to daycare or school
This is the question I heard constantly in triage: “When are we allowed back?” Policies vary, so check your daycare or school rules. In general, return is based on starting appropriate antibiotics and being able to keep sores covered and contained.
Typical guideline
- Many schools and childcare settings allow return after 24 hours of effective antibiotic treatment, as long as lesions can be covered, drainage is controlled, and your child feels well enough to participate.
Keep your child home longer if
- Sores are still actively oozing and cannot be covered
- Your child cannot stop touching or scratching the area (very common in toddlers)
- There is fever or your child is not acting like themselves
If your child is involved in close-contact activities (wrestling, gymnastics with shared mats, some dance classes), ask the coach or school nurse about specific restrictions.
Impetigo vs other rashes
Parents often tell me, “It looks like three different things depending on the lighting.” Fair. Here is a quick, practical comparison.
Hand, foot, and mouth (HFMD)?
HFMD often causes mouth sores and small spots or blisters on the hands and feet, plus fever and sore throat. Impetigo is more about honey crust and local spread, often around the nose and mouth.
Eczema?
Eczema is usually dry, scaly, and chronic. But eczema can get infected, and that infection can look like impetigo. If eczema suddenly becomes weepy, crusty, or rapidly worse, call.
Cold sores?
Cold sores are caused by HSV and often present as grouped blisters that tingle or hurt, typically on the lip line. Impetigo crust is usually thicker and more “sticky,” and spread can be faster across nearby skin.
Ringworm?
Ringworm is usually a round patch with a more defined edge and central clearing. Impetigo is often irregular and crusted.
Prevent it next time
You cannot bubble wrap a preschooler. But you can lower the odds of round two.
- Promptly clean and cover scrapes and bug bites.
- Use a gentle moisturizer for kids with eczema and follow your eczema plan to protect the skin barrier.
- Teach “no sharing” for towels, hats, brushes, and makeup (for older kids).
- Encourage handwashing after nose wiping and before meals.
Will it scar?
Impetigo usually heals without scarring. Sometimes there is temporary discoloration that fades with time. The biggest scar-maker is picking, so this is one of those moments where short nails and distractions really pay off.
If your child gets recurrent impetigo, ask your clinician whether nasal carriage of Staph could be contributing and whether a targeted plan is appropriate.
Quick comfort talk
Impetigo can look dramatic, especially when it is on the face. That does not mean you missed something or did something wrong. This is one of those childhood infections that spreads because kids are kids.
If you start treatment, keep up with handwashing and laundry for a few days, and resist the urge to pick at crusts, you are doing the right things. And yes, it is okay to ask your pediatrician for a quick look when you are not sure. That is what we are here for.
Reminder: This article provides general education and is not a substitute for medical care. If your child has worsening symptoms, eye involvement, significant pain, or fever, contact your pediatric clinician promptly.