Infant Choking First Aid: Back Blows and Chest Thrusts
Sarah Mitchell
Sarah Mitchell is a Registered Pediatric Nurse and a mother of three who has spent over a decade helping families navigate the beautiful, chaotic early years of childhood. She combines evidence-based medical knowledge with real-world parenting experience to offer practical, compassionate advice. At Awesome Parent, Sarah's mission is to help exhausted parents find solutions, trust their instincts, and finally get some sleep.
If you are reading this with your heart racing, take one breath with me. Choking is terrifying, but the response for babies is straightforward: back blows and chest thrusts, repeated until the blockage clears or help takes over.
This page focuses on rescue skills (what to do in the moment). If you are looking for prevention and choking hazards, that is a different topic and worth reading too. Right now, we are staying laser-focused on the emergency steps for birth to 12 months.
First, know the difference: gagging vs choking
Babies gag. A lot. Gagging can look dramatic, but it is often noisy and effective. Choking means the airway is blocked partly or completely, so air is moving poorly or not at all.
Signs your baby is gagging (air is moving)
- Coughing or spluttering
- Noisy breathing
- Babies may turn red, watery-eyed, or spit up
- They can still cry or make sounds
Signs your baby is choking (little or no air is moving)
- Cannot cry or make much sound
- Weak or silent cough, or no cough at all
- Struggling to breathe, or not breathing
- Lips or skin may look bluish or gray
- Sudden distress while eating or with a small object nearby
If your baby is coughing forcefully or making noise, let them keep coughing. Stay close, watch carefully, and be ready to act if it worsens.
What to do now (quick checklist)
- Assess fast: Is your baby truly choking (silent or ineffective cough)? If you are unsure and breathing is not effective, treat it as choking.
- Call for help: If you are not alone, have someone call 911 (or your local emergency number) right away and put it on speaker.
- Start back blows and chest thrusts: Alternate 5 back blows and 5 chest thrusts until one of these happens: the object comes out, your baby can breathe or cough or cry effectively, trained help takes over, or your baby becomes unresponsive.
These steps are consistent with widely taught pediatric first aid guidance (such as American Heart Association and Red Cross courses). The most important thing is to act quickly and keep going.
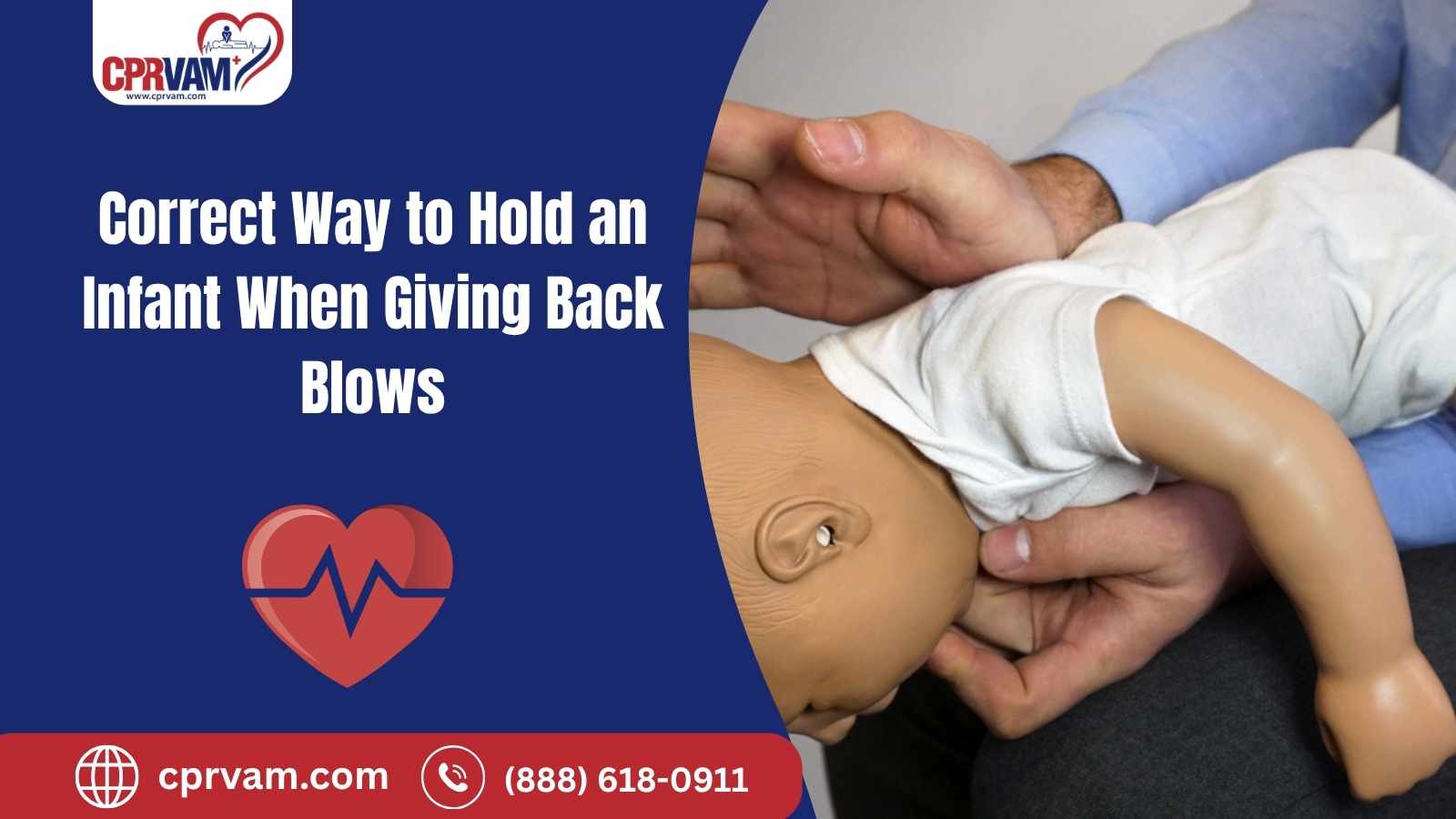
Back blows (under 12 months)
Back blows use gravity plus firm strikes to help dislodge the object.
How to do 5 back blows
- Position baby face-down along your forearm, supported on your thigh if sitting. Keep the head lower than the chest.
- Support the head and jaw with your hand. Avoid squeezing the soft tissues of the throat. Think “support the jawline,” not “grab the neck.”
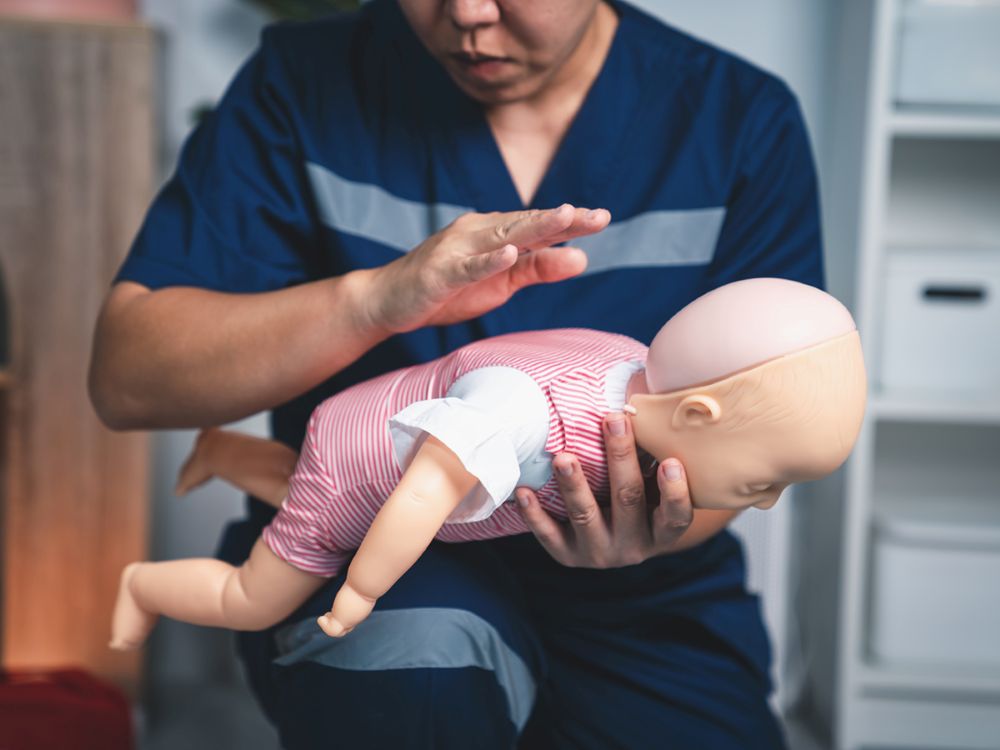
- Using the heel of your free hand, give 5 firm back blows between the shoulder blades in rapid succession.
- Then look to see if the object is out and breathing improves. If not, move straight to chest thrusts.
How hard? Firm and controlled. You are not tapping. You are delivering purposeful blows, aimed between the shoulder blades, while keeping the head lower than the chest. Oxygen matters.
Chest thrusts (under 12 months)
Chest thrusts are the infant version of abdominal thrusts. We use the chest because an infant’s abdomen and organs are more vulnerable.
How to do 5 chest thrusts
- Turn baby face-up while keeping the head lower than the chest, supported on your forearm and thigh.
- Find the spot: Place 2 fingers on the center of the chest on the breastbone, just below the nipple line.
- Give 5 quick chest thrusts straight down, firmly, in rapid succession.
- Then look to see if the object is out and breathing improves. If not, go right back to back blows.
Keep alternating 5 back blows and 5 chest thrusts until the blockage clears, your baby can breathe or cough or cry effectively, help takes over, or your baby becomes unresponsive.

When to call 911 (and if you are alone)
Call 911 immediately if:
- Your baby is not breathing, turning blue or gray, or becomes limp
- Your baby has a silent or ineffective cough and cannot cry
- You are doing back blows and chest thrusts and the blockage is not clearing quickly
If you are alone
- Start back blows and chest thrusts right away.
- If your phone is within reach, call 911 on speaker while you continue.
- If you cannot reach a phone and you would have to leave your baby to call, give about 2 minutes of care, then call 911 as soon as possible and return to your baby immediately.
Dispatcher coaching can be incredibly helpful, especially when your brain is running on adrenaline and no sleep.
If your baby becomes unresponsive
If your baby stops responding, treat this as a life-threatening emergency.
- Call 911 (or have someone call). If you are alone and have not called yet, call now.
- Start infant CPR right away.
- Each time you open the airway to give breaths, look in the mouth. If you can see the object, remove it. If you cannot see it, do not do a blind finger sweep.
CPR is a whole skill set, and I strongly recommend taking an in-person infant CPR class. Even one evening course can make you feel much steadier in a crisis.
What not to do
- Do not do abdominal thrusts (Heimlich) on a baby under 12 months. For infants, use back blows and chest thrusts.
- Do not do a blind finger sweep. Sweeping without seeing the object can push it deeper.
- Do not use tools (tweezers, cotton swabs) to try to pull something out.
- Do not try to “wash it down” with water, milk, or food.
- Do not hang the baby upside down by the feet. It is unsafe and wastes time.
- Do not repeatedly pound the back while the baby is upright. Positioning with the head lower than the chest matters.
How this differs for older kids
For children over 1 year (and adults), first aid often uses abdominal thrusts because it can rapidly increase pressure and expel the object. Infants have different anatomy and higher injury risk, so the recommended approach is back blows and chest thrusts.
If you have kids in multiple age groups, it is worth learning both techniques. In my house, this is exactly the kind of thing I keep on a quick-reference card, because memory gets fuzzy under stress.
After the object comes out
If your baby starts breathing normally and seems comfortable, you can take a breath too. Then do a quick check-in.
Call your pediatrician or seek urgent care if:
- Your baby had a significant choking episode and seems hoarse, wheezy, or is coughing persistently
- You hear noisy breathing like stridor (a harsh sound on inhale), or you suspect the object may have been inhaled into the airway
- Your baby vomits repeatedly, is unusually sleepy, or just “is not right”
Always go to the ER or call 911 if breathing looks labored, lips look blue or gray, or your baby is struggling.
Quick mental script
“Is my baby coughing and noisy? If yes, let them cough. If not, call for help and do 5 back blows, 5 chest thrusts, repeat. If unresponsive, call 911 and start CPR.”
You do not need to be perfect. You just need to start.
A note from a pediatric nurse and a mom
In clinic, I saw parents blame themselves after a choking scare. Please do not. Babies explore with their mouths, feeding is a learning curve, and even very careful families can have an emergency.
The best time to prepare is when you are calm. If you can, take an infant CPR class, practice the hand positions on a doll, and make sure caregivers know the basics too. Future you will be grateful at 3 AM.
Medical disclaimer: This article is general education and does not replace hands-on training or medical care. If your baby is choking or you are worried about breathing, seek emergency help immediately.