Intussusception in Babies and Toddlers: Crampy Pain and Stool Red Flags
Sarah Mitchell
Sarah Mitchell is a Registered Pediatric Nurse and a mother of three who has spent over a decade helping families navigate the beautiful, chaotic early years of childhood. She combines evidence-based medical knowledge with real-world parenting experience to offer practical, compassionate advice. At Awesome Parent, Sarah's mission is to help exhausted parents find solutions, trust their instincts, and finally get some sleep.
If your baby or toddler is suddenly having episodes of intense, crampy belly pain and then acting mostly fine again, it is the kind of pattern that makes parents feel whiplash. One minute they are screaming and pulling their knees up, the next they are quiet or even playing. That stop-start rhythm is one reason intussusception can be tricky at home and why it is taken seriously in pediatric triage.
Intussusception is when one part of the intestine slides into another part like a telescope. It can block the bowel and cut down blood flow to the tissue. The most important takeaway is simple: this is an emergency that needs prompt medical evaluation. You do not need to diagnose it at home, but you do need to recognize the red flags and seek care quickly.
What the pain can look like
Parents often describe the pain as coming in waves. That is because the intestine spasms and tries to push contents through a partially blocked area.
Classic pain pattern
- Sudden, severe cramping episodes that come on quickly.
- Drawing up legs toward the belly, arching, or curling into a ball.
- Crying that is hard to soothe during the episode.
- Brief periods of relief in between, where your child may look surprisingly okay.
- Episodes repeating on a cycle, often every 15 to 30 minutes, but sometimes more or less frequently.
From a triage nurse perspective, when the pain is intense, then eases, then comes right back in a repeatable pattern, it raises concern for a bowel issue rather than a simple tummy bug.
Between-episode clues
Some kids bounce back between cramps. Others look washed out or unusually sleepy, which can be a major clue.
- Pallor (looking very pale or gray compared with their normal color).
- Lethargy or sudden unusual sleepiness, sometimes even without a fever.
- Low energy or “not themselves” even when they are not actively crying.
- Refusing feeds or acting like swallowing makes them more uncomfortable.
Lethargy is one of those words that gets overused online. In triage, we mean a child who is difficult to keep awake, not engaging the way they normally would, or seems profoundly listless.

Stool and diaper red flags
Stool changes can show up as the bowel becomes irritated and blood flow is affected. Not every child has obvious blood early on, so absence of blood does not rule it out.
Red flag stool appearances
- Blood in the stool, bright red or darker maroon.
- Mucus mixed with stool that looks slimy.
- “Currant jelly” stool, a classic description that looks like dark red jelly mixed with mucus.
- No stool or no gas along with worsening belly symptoms, which can suggest blockage.
One important nuance: “currant jelly” is memorable, but it is not always present, especially early. If your child has the crampy episodes plus any blood or mucus in the diaper, that is an urgent combination.
Other symptoms to watch
- Vomiting, sometimes mild at first (including spit-up) and then becoming more frequent.
- Green or dark yellow vomit (bilious), which is a critical red flag for bowel obstruction and needs immediate ER care.
- Swollen or firm belly or obvious belly tenderness.
- Fever can occur, but many kids do not have one early.
Because vomiting and fussiness are common in childhood, the pattern is what helps: repeated intense pain episodes, sometimes with pallor or sleepiness between them, and any concerning stool.
When it is most common
Intussusception most often happens in infants and toddlers, commonly between about 6 and 36 months, with a peak around 6 to 18 months, though it can happen outside that range.
Many cases have no clear cause. Sometimes it follows a viral illness that causes lymph tissue in the intestine to swell, which can help the telescoping start. True structural “lead points” are more likely in older children.
What you can do at home
To be very clear: if you strongly suspect intussusception, this is not a “wait it out” situation. The goal at home is not to treat it. The goal is to notice patterns and get to the right level of care quickly.
If symptoms are mild or unclear
- Track timing: note when episodes start, how long they last, and how often they return.
- Check diapers: look for blood, mucus, or an unusual dark red, jelly-like appearance.
- Observe between episodes: is your child playful and normal, or pale and unusually sleepy?
- Call your pediatrician or nurse line promptly if you are unsure. Describe the stop-start pain pattern specifically.
What not to do
- Do not give laxatives or enemas at home to “get things moving” if obstruction is a concern.
- Do not force food or drink if your child is actively vomiting or has severe pain.
- Do not delay care for an office visit if episodes are severe, repeating, or paired with red flags.
If your gut is telling you something is off, listen to it. Many parents worry they are overreacting, but this is one of those situations where it is better to be seen and reassured than to miss something time sensitive.
Go to the ER now
Please seek emergency care immediately (or call emergency services if your child is difficult to rouse or looks very unwell) if you notice:
- Severe, intermittent crampy belly pain, especially with drawing up legs.
- Blood or mucus in stool, including currant jelly-like stool.
- Green or dark yellow vomit (bilious).
- Unusual lethargy, limpness, hard to wake, or not interacting normally.
- Repeated vomiting, especially with worsening belly pain or distension.
- Signs of dehydration (very dry mouth, no tears, fewer wet diapers) plus ongoing symptoms.
- Worsening belly swelling or significant tenderness.
- Severe continuous pain (not coming and going), or a child who remains inconsolable.
- Signs of shock such as cold, clammy skin, very weak, fast pulse, or faintness.
Intussusception is time sensitive. Earlier evaluation can mean a simpler treatment and a smoother recovery.
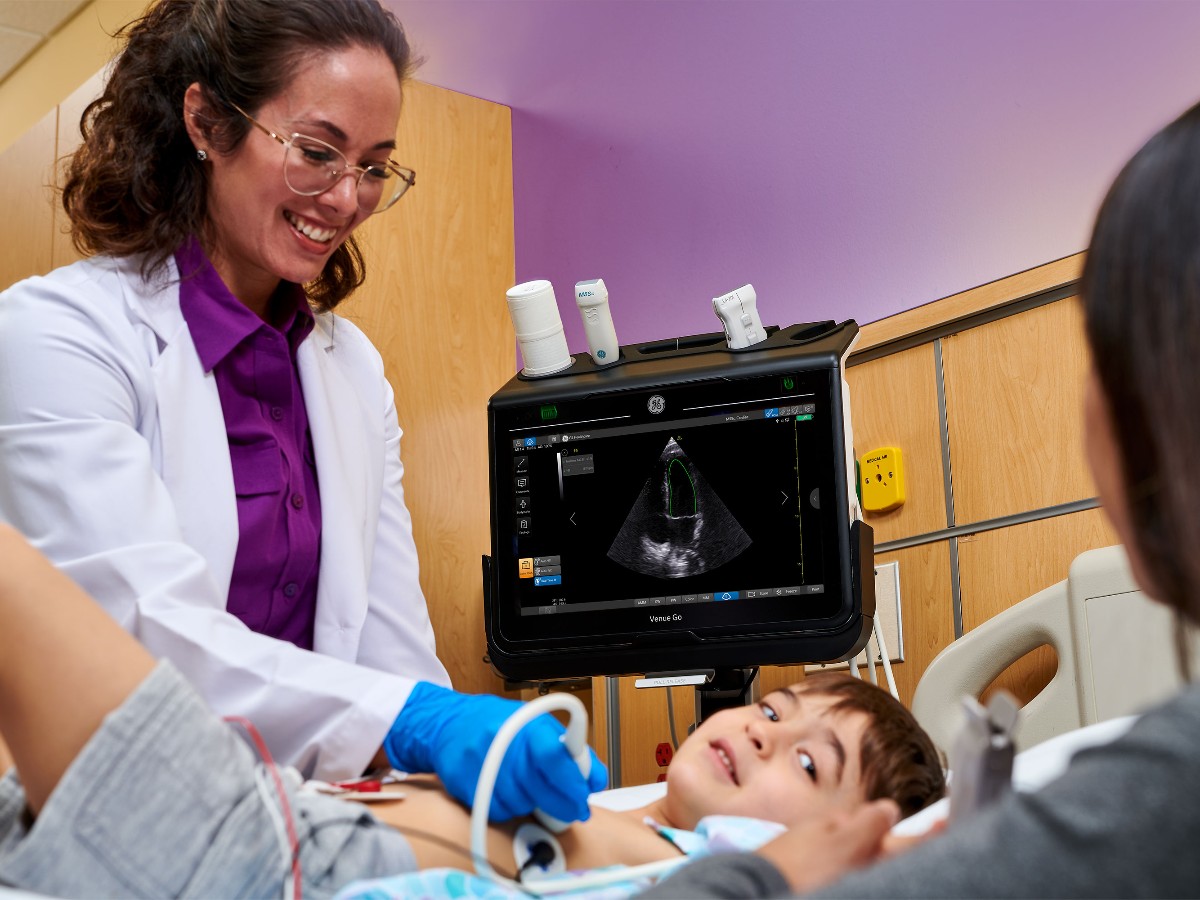
What the ER team may do
If clinicians suspect intussusception, the next steps are usually focused on confirming the diagnosis quickly and treating it safely.
Common tests
- Ultrasound: This is the most common test because it is fast, does not use radiation, and is very good at detecting intussusception.
- Vitals and exam: Hydration status, belly exam, and overall appearance matter a lot.
Common treatment
- Air or contrast enema: In many cases, radiology can use an enema with air or contrast to gently unfold the telescoped bowel. It is both a diagnostic and therapeutic procedure.
- Surgery: If the enema cannot reduce it, if there are signs of complications, or if a specific lead point is suspected, surgery may be needed.
Teams also treat pain, nausea, and dehydration as needed. The exact plan depends on your child’s age, exam, and how stable they are.
Common questions
Could this just be gas or constipation?
Gas and constipation can absolutely cause discomfort and crying. What is different with intussusception is often the intensity and the repeatable, wave-like pattern, sometimes paired with pallor, lethargy, bilious vomiting, or bloody mucus in the diaper.
My child seems fine between episodes. Do we still need to go in?
Yes, if the episodes are severe and keep returning, or if there are any stool red flags, bilious vomiting, or unusual sleepiness. Feeling better between episodes does not guarantee it is safe to watch at home.
If there is no blood, can it still be intussusception?
Yes. Blood or currant jelly stool can be a later sign. Early on, the main clues may be the intermittent severe pain and behavior changes.
The bottom line
Intussusception is one of those pediatric emergencies where pattern recognition is everything: sudden severe cramping episodes, knees pulled up, pallor or lethargy between episodes, vomiting (especially if it turns green or dark yellow), and any blood or mucus in the stool. If you are seeing that combination, trust your instincts and get evaluated urgently.
If you think your child may have intussusception, go to the ER now.