Juvenile Idiopathic Arthritis in Kids: Morning Stiffness and Swollen Joints
Sarah Mitchell
Sarah Mitchell is a Registered Pediatric Nurse and a mother of three who has spent over a decade helping families navigate the beautiful, chaotic early years of childhood. She combines evidence-based medical knowledge with real-world parenting experience to offer practical, compassionate advice. At Awesome Parent, Sarah's mission is to help exhausted parents find solutions, trust their instincts, and finally get some sleep.
If your child wakes up moving like a tiny 90-year-old, or you keep noticing the same puffy knee that never quite goes back to normal, you are not being dramatic. You are paying attention. And when joint swelling and morning stiffness keep showing up, it is worth thinking beyond “growing pains.”
One of the most common chronic inflammatory arthritis conditions in childhood is juvenile idiopathic arthritis (JIA). “Idiopathic” simply means we do not have one single clear cause. JIA is not caused by a child being “too active,” cracking their knuckles, or eating the wrong food. It is an immune system problem that leads to ongoing inflammation in joints, and sometimes beyond the joints.
This page will help you recognize the patterns parents often miss at first, understand the main JIA subtypes in plain language, know when to push for evaluation, and learn why eye checks are not optional.
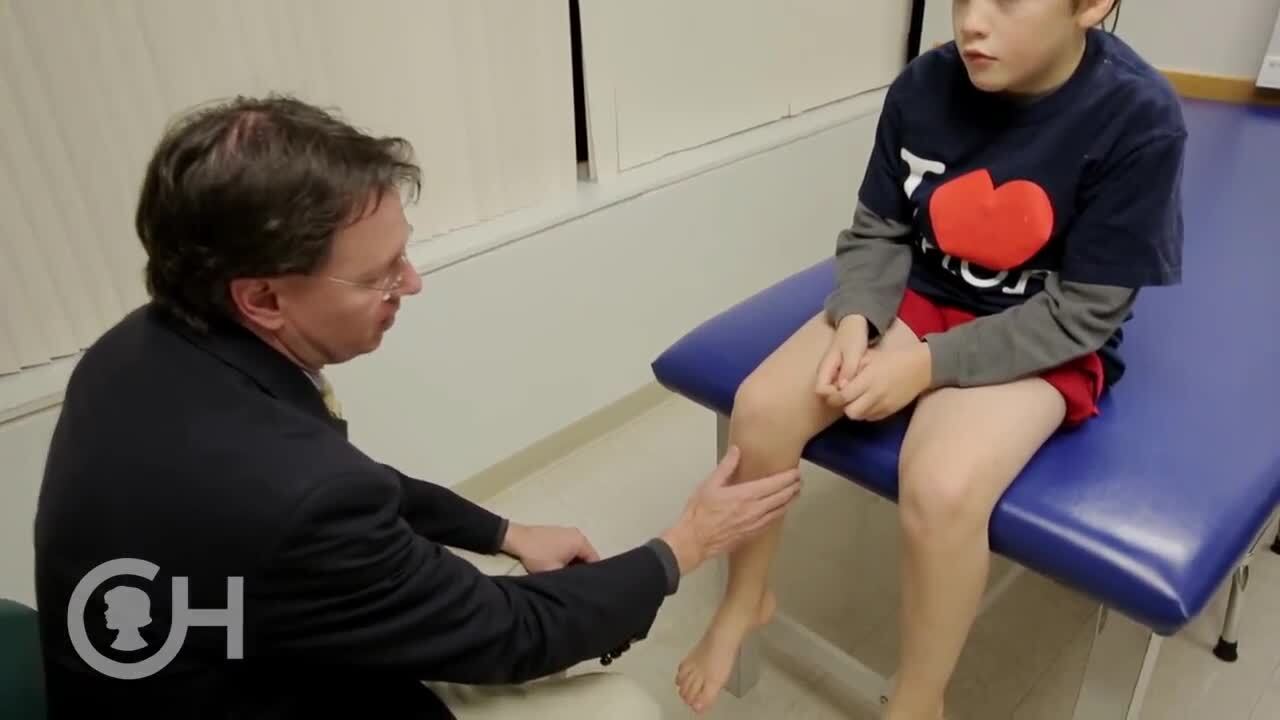
What it looks like at home
In pediatric clinics, families often say, “It comes and goes,” or “They seem fine by lunchtime.” That can still be JIA. Inflammatory arthritis can be most obvious after rest, especially in the morning.
Common signs parents notice
- Morning stiffness that lasts long enough to delay getting moving, often more than 15 minutes. Kids may shuffle, avoid stairs, or need time to “warm up.”
- Joint swelling that is persistent or keeps returning in the same joint (often a knee or ankle).
- Limping that is worse after waking up or after sitting, and improves as the day goes on.
- Reduced use of a limb (not wanting to crawl, climb, run, or use a hand) without a clear injury.
- Complaints of tightness rather than sharp pain, especially in younger kids who cannot describe sensations well.
- Fatigue or irritability, sometimes more noticeable than pain.
Important nuance: many kids with JIA do not have dramatic pain. Some hardly complain at all. Their body just quietly adapts, and the limp becomes “their normal” until someone sees them next to peers.
Also, joints can look “just a little bigger” without obvious redness. Subtle swelling and reduced range of motion can still be meaningful.
Swollen knee vs growing pains
Growing pains are real, common, and frustrating. But they have a very different “personality” than inflammatory arthritis.
Typical growing pains
- Usually felt in both legs (often calves, shins, or behind knees)
- Often show up in the evening or at night
- Come and go, with normal activity during the day
- No visible swelling, warmth, or persistent limp
- Massage and reassurance often help
Clues that point more toward JIA
- One joint keeps swelling (a single puffy knee is a classic starting point)
- Morning stiffness or stiffness after sitting
- Limp that lasts more than a few days without a clear injury
- Joint looks bigger or your child cannot fully straighten or bend it
- Symptoms present most days for weeks
A practical note: clinicians use “arthritis for 6 weeks or longer” as part of the formal definition of JIA. But you do not need to wait 6 weeks to seek care. If a joint is swollen for more than a week or two, or a limp is not clearly improving, it is appropriate to book an evaluation.
From my time in pediatric triage, the phrase that always made my ears perk up was: “It’s not getting better, it’s just… there.”

JIA types in plain language
JIA is a group of conditions. The subtype matters because it can change which symptoms to watch for, what labs might show, and what follow-up is needed.
Oligoarticular JIA
Most common in younger kids. Involves 1 to 4 joints, often knees or ankles. Many children look well otherwise. The biggest “hidden” risk is silent eye inflammation (more on that below).
Polyarticular JIA
Affects 5 or more joints. Can involve small joints of hands and feet, and can look more like adult rheumatoid arthritis. Morning stiffness can be prominent, and daily function like gripping a pencil or opening containers can be affected.
Systemic JIA
This subtype can involve joints, but it is also a whole-body inflammatory illness. It may include high fevers and a rash, along with fatigue and swollen lymph nodes. Some children can also develop inflammation of organs such as the liver or spleen, or inflammation around the heart or lungs (serositis). Joint symptoms may appear later.
There is also a rare but serious complication called macrophage activation syndrome (MAS). It can look like a child with systemic JIA suddenly becoming much more ill, with persistent high fever and marked worsening. If your child has suspected or known systemic JIA and suddenly looks very unwell, this is an urgent situation.
Enthesitis-related arthritis (ERA)
Inflammation occurs where tendons and ligaments attach to bone, often causing heel pain or pain around knees, and sometimes lower back symptoms in older kids or teens. It is more common in boys and can be linked with certain genetic markers.
Psoriatic JIA
Associated with psoriasis in the child or sometimes a strong family history. Clues can include scaly patches, pitted nails, or a whole finger or toe that looks swollen (“sausage digit”).
If you are thinking, “My child does not fit neatly into one box,” you are not alone. Subtypes can be clarified over time, and pediatric rheumatology is used to sorting out patterns.
Fever patterns and red flags
Most kids with JIA do not have fevers day-to-day. But systemic JIA is the exception, and fever patterns can be a major clue.
Systemic JIA fever pattern
- High spikes, often once daily
- Child may look quite ill during the spike, then surprisingly better when it comes down
- Sometimes accompanied by a salmon-pink rash that comes and goes
Any child with persistent fevers plus significant lethargy, trouble breathing, severe headache, stiff neck, dehydration, or a child who looks very unwell needs urgent medical evaluation. Fevers have many causes, and you do not want to assume it is “just inflammation” without a clinician assessing them.
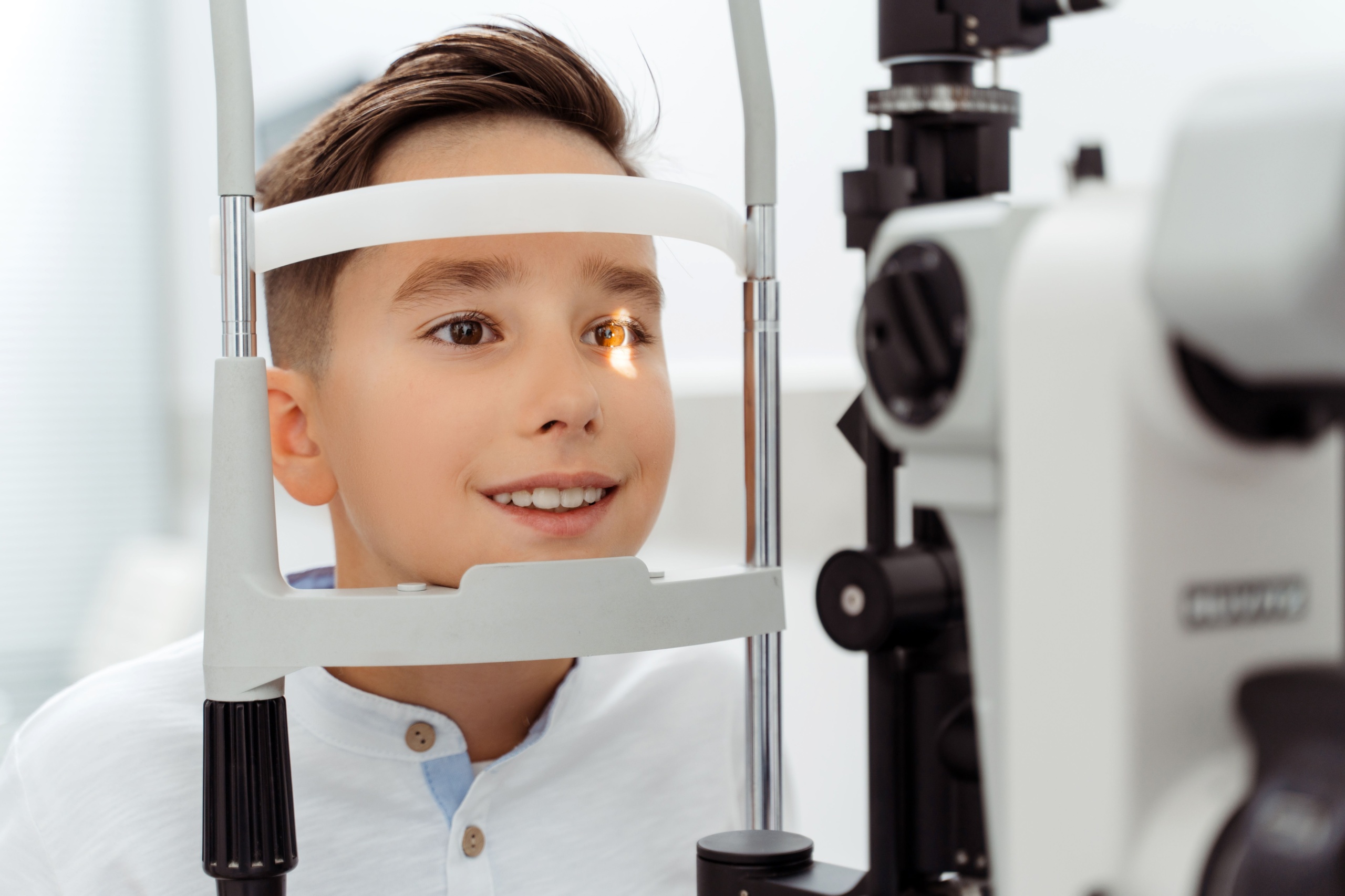
Why eye screening matters
This is the piece I wish every family heard early: some kids with JIA can develop uveitis, an inflammation inside the eye. It can be silent at first, meaning no redness, no pain, no obvious vision complaints.
That is why your child may need routine screening with a pediatric ophthalmologist using a slit lamp. This is not the same as a quick vision check at school or the pediatrician’s office.
Who is at higher risk?
- Many children with oligoarticular JIA
- Kids who are ANA-positive (a lab marker your rheumatologist may discuss)
- Younger age at arthritis onset
Risk and screening frequency are guided by a combination of subtype, ANA status, age of onset, and how long they have had arthritis. Also, uveitis can happen in ERA too, but it is more often an acute, painful, red-eye presentation. Either way, eye symptoms in a child with JIA should be taken seriously.
The screening schedule depends on risk level. If your child is diagnosed with JIA, ask: “How often should we see ophthalmology, and when is the next appointment due?”
How JIA is diagnosed
There is no single test that “proves” JIA. Diagnosis is based on the pattern of symptoms, the physical exam, and ruling out other causes.
What clinicians may use
- History: Which joints, how long, morning stiffness, fevers, rashes, infections, injuries
- Exam: Swelling, range of motion, gait, and signs of inflammation
- Labs: Markers of inflammation and certain antibodies (these can be normal in some kids with JIA)
- Imaging: Ultrasound or MRI can show inflammation that is not obvious from the outside
A quick “what else could it be?” list that clinicians often consider includes injury or overuse, reactive arthritis after an infection, Lyme disease in areas where it is common, septic arthritis (joint infection), and in rare cases malignancy. This is one reason persistent swelling or a limp deserves a thoughtful workup.
One practical tip: take a quick photo of the swollen joint during a flare, and note dates. Symptoms sometimes calm down right before the appointment because kids are talented that way.
Treatment basics
JIA treatment is individualized, but the goal is consistent: stop inflammation early to protect joints, support normal growth, and keep kids doing kid things.
Common treatment tools
- NSAIDs (anti-inflammatory medicines): sometimes enough for mild cases
- Joint steroid injections: can calm a stubborn swollen joint, especially in oligoarticular JIA
- DMARDs such as methotrexate: reduce immune-driven inflammation
- Biologics: targeted medicines often used for more persistent or severe disease
- Physical and occupational therapy: strength, flexibility, joint protection, school accommodations
Parents often worry about “strong medicines.” That is a real and valid concern. But uncontrolled inflammation can also be “strong” in the worst way. Your care team can help you weigh risks and benefits based on your child’s symptoms and goals.
If your child is on medicines that affect the immune system, ask about lab monitoring, vaccine timing, and what to do about fevers and infections. The details vary by medication, but you deserve a clear plan.
Sports and activity
Most kids with well-controlled JIA can participate in sports and active play. Movement is generally good for joints. The tricky part is returning gradually after a flare, a new diagnosis, or a medication change.
A realistic pacing plan
- Start low and slow: short practices, fewer drills, extra warm-up time
- Watch the next morning: inflammation often “votes” the morning after activity
- Use a simple stiffness check: “How stiff are you when you wake up, 0 to 10?” Track trends, not single bad days
- Prioritize form over intensity: fatigue can change mechanics and increase injury risk
- Schedule rest days: especially after high-impact activity
- Coordinate with PT and coaches: modifications are not a failure, they are a strategy
When to scale back and call the care team
- Swelling returns or increases
- New limp
- Morning stiffness lengthens noticeably
- Night pain that is unusual for your child
My parenting rule of thumb: we do not “push through” inflammation. We problem-solve it.
When to get urgent care
Please seek same-day medical care or urgent evaluation if your child has:
- A hot, very swollen, very painful joint with fever (needs urgent evaluation for infection)
- Severe pain with inability to bear weight after an injury
- Persistent high fevers, looking very ill, trouble breathing, or signs of dehydration
- New eye pain, significant redness, light sensitivity, or sudden vision changes
And if your child has had joint swelling or a limp for more than 1 to 2 weeks, even without an emergency, it is appropriate to make an appointment and ask directly whether inflammatory arthritis is being considered.
Prognosis
It is normal to feel anxious reading about chronic illness. The hopeful reality is that many children with JIA do very well. With modern treatment and close follow-up, a lot of kids achieve excellent control and some reach remission. The earlier inflammation is identified and treated, the more we can protect joints, eyes, school life, and confidence.
Questions to bring
- Which joints are involved, and does this pattern fit a JIA subtype?
- What should we track at home (stiffness minutes, swelling photos, activity limits)?
- Do we need imaging like ultrasound or MRI?
- What else are you considering, and what signs would change the plan?
- What is our plan if symptoms do not improve in 2 to 4 weeks?
- When is the first ophthalmology screening, and how often after that?
- What can school do to help (extra time between classes, PE modifications, pencil grips, elevator access)?
If you are tired of feeling like you have to “prove” something is wrong, you are not alone. Persistent swelling and morning stiffness are enough reason to ask for a thorough evaluation. Trust the pattern you are seeing.