Kawasaki Disease in Kids: Fever, Rash, and When to Go to the ER
Sarah Mitchell
Sarah Mitchell is a Registered Pediatric Nurse and a mother of three who has spent over a decade helping families navigate the beautiful, chaotic early years of childhood. She combines evidence-based medical knowledge with real-world parenting experience to offer practical, compassionate advice. At Awesome Parent, Sarah's mission is to help exhausted parents find solutions, trust their instincts, and finally get some sleep.
If you are reading this at 2 AM with a thermometer in one hand and your phone in the other, I want you to hear this first: you are not overreacting. A fever plus a rash can be “just a virus” and it also can be something that needs timely treatment. Kawasaki disease sits in that second category.
Kawasaki disease is uncommon, but it matters because it can inflame blood vessels, including the coronary arteries that supply the heart. The good news is that when kids are evaluated and treated promptly, most do very well.

What it is
Kawasaki disease is an inflammatory illness that mostly affects young children, most often under age 5. It tends to show up as a fever that will not quit, along with a cluster of symptoms involving the eyes, mouth, skin, and hands and feet.
It is not something you can confirm at home. Diagnosis comes from the overall pattern, a physical exam, and often bloodwork and a heart ultrasound called an echocardiogram.
Most parents I meet feel two things at once: relief that there is a name for what is happening, and worry about the heart part. Both feelings make sense. The heart risk is exactly why we take “fever plus specific signs” seriously and move quickly.
The fever pattern
The hallmark is a persistent fever, usually 5 days or more. It is often high, and it tends to stick around day after day rather than clearly improving.
What “persistent” can look like
- Fever every day, with little or no improvement
- A child who looks increasingly uncomfortable or irritable rather than slowly better
- New Kawasaki-type signs showing up as the days pass (rash, red eyes, mouth changes, swollen hands and feet)
Important note: some children are evaluated and treated before day 5 if they have a strong set of other signs. So please do not use “it has only been 3 or 4 days” as a reason to wait if your gut says something is off.
Incomplete Kawasaki
You may also hear clinicians say incomplete or atypical Kawasaki disease. This means a child has the prolonged fever and some concerning clues, but not the full classic checklist.
This is especially important in infants under 12 months. They can have a long fever with only a few visible signs, and they are a group we watch closely because heart involvement can still happen even when the “classic” symptoms are subtle.
Common symptoms
Kawasaki disease is usually discussed as a set of features that show up during the same illness. Your child does not always have every single one, and they may not all appear at once.
Red eyes
This is eye redness without goopy discharge. Parents often say, “His eyes look bloodshot, but it does not seem like pink eye.” That detail matters.
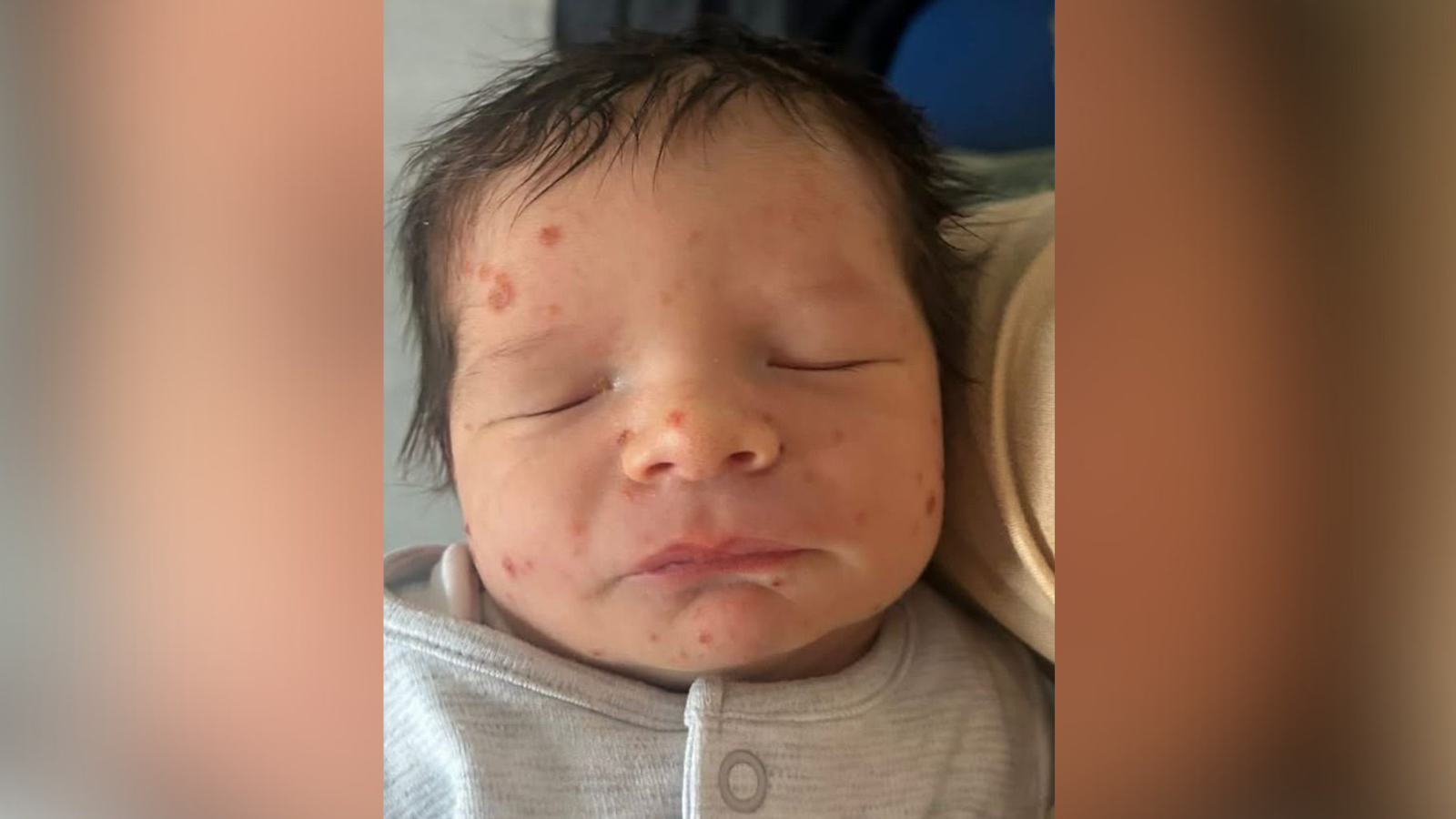
Rash
The rash can vary. It may be patchy, blotchy, or widespread, and it can look different from child to child. The key is rash plus the persistent fever and other signs.
Mouth and throat changes
- Red, cracked lips
- Red mouth or throat
- “Strawberry tongue”, which looks bright red with prominent little bumps

Hands, feet, peeling
One of the more distinctive clues is swelling and redness of the hands and feet. Some kids refuse to walk or want to be carried because their feet hurt.
Later, often after the initial fever phase, you may notice peeling skin, especially around the fingertips and toes. Parents sometimes see the peeling and think it is a separate problem. It can actually be part of the Kawasaki timeline.
Other clues
Some children develop a swollen lymph node in the neck, usually on one side. (In the classic criteria it is often described as enlarged, sometimes larger than about 1.5 cm, but you do not need a ruler at home.)
Another very real sign is behavior: many kids with Kawasaki seem unusually irritable, like they cannot get comfortable no matter what you do. As a triage nurse, that “something is not right” vibe from parents is a piece I take seriously.
Why doctors move fast
Kawasaki disease can cause inflammation in blood vessels, including the coronary arteries. Without treatment, some children can develop changes in these arteries that increase the risk of complications.
This is the reason we push for prompt evaluation. Treatment significantly lowers the risk of heart involvement when started early, and it is often most effective when given within the first 10 days of illness.
If your child is being evaluated for Kawasaki disease, you may hear about:
- Blood tests that look for inflammation and other patterns (for example CRP or ESR, a complete blood count including platelets, liver tests, albumin, and sometimes a urine test)
- Echocardiogram to check the coronary arteries and heart function
- ECG (a heart rhythm tracing) in some cases
- Repeat follow-up with cardiology in some cases
Urgent care vs ER
Because fever and rash are so common, the right level of care depends on your child’s age, appearance, and symptoms. Use this as a safety-focused guide, not a self-diagnosis tool.
Go to the ER now
- Your child has trouble breathing, bluish lips, or severe chest pain
- Your child is hard to wake, very confused, or you cannot keep them awake
- Signs of dehydration: significantly decreased urination (for example no wet diaper in about 6 to 8 hours for infants, or no urine in about 8 to 10 hours for older kids), very dry mouth, no tears, or a sunken soft spot in infants
- A purple or bruise-like rash that does not blanch (does not fade when you press it)
- Seizure
- Your child looks severely ill to you, especially if you are thinking, “This is not my usual kid.”
Get same-day evaluation
- Fever for 5 days or more, especially with any of the Kawasaki-type signs below
- Fever plus red eyes without discharge
- Fever plus rash and red, cracked lips or strawberry tongue
- Fever plus swollen or red hands and feet
- Fever plus new neck swelling (enlarged lymph node)
- A child who is very irritable and not improving as the days pass
- Infants under 12 months with several days of fever and no clear source, even if the classic signs are not obvious
If you are on day 4 of fever and you are seeing multiple Kawasaki signs, I would still recommend same-day evaluation. Waiting for day 5 is not the goal.
What to do on the way
- Write down the fever timeline: when it started, highest temps, and what medicines you have used
- Take photos of the rash and any swelling. Rashes love to fade right at the appointment
- Bring medication doses or the bottles so your clinician can confirm correct dosing
- Do not start aspirin unless your child’s clinician specifically tells you to. Aspirin is often part of Kawasaki treatment under medical supervision, but it is not a DIY at-home step for a fever
Common look-alikes
Fever and rash have a long list of causes. Some of the common “could be this” illnesses include:
- Viral exanthems (common viral rashes)
- Scarlet fever (often with sore throat and a sandpapery rash)
- Hand, foot, and mouth disease (mouth sores plus rash on hands and feet)
- Measles in unvaccinated or under-vaccinated children, usually with a very specific pattern and exposures
- Allergic reactions (often itchy and linked to a trigger)
- MIS-C (a post-infectious inflammatory syndrome that can happen after COVID; clinicians think about it because it can also cause fever, rash, and inflammation)
This is exactly why internet symptom-checking can spiral fast. The overlap is real. Your pediatrician or ER team is looking at the whole picture, including the exam and testing.
If your child is diagnosed
Treatment is handled in the hospital because the goal is to calm inflammation and monitor the heart. Many children receive:
- IVIG (intravenous immune globulin), which helps reduce inflammation and lowers the risk of coronary artery complications
- Aspirin as directed by the care team (dosing and timing are very specific, which is why this is not an at-home decision)
- Other anti-inflammatory medicines in selected cases (for example steroids if a child is higher-risk or not improving)
- Heart monitoring and echocardiograms now and sometimes again later
Most kids start to look noticeably better after treatment. Parents often tell me it is the first time all week they recognize their child again.
Follow-up varies. Some children need repeat echocardiograms over the next weeks or months, especially if there were any coronary changes.
Trust your instincts
If I could put one simple takeaway on a sticky note for your fridge, it would be this: persistent fever plus red eyes, mouth changes, rash, or swollen hands and feet deserves prompt medical evaluation.
You do not need to decide at home whether it is Kawasaki disease. Your job is to notice the pattern, document it, and get your child seen.
If you are unsure where to go, call your pediatrician’s after-hours line and describe: the number of fever days, the highest temperature, hydration and urination, and the specific symptoms you are seeing (red eyes without discharge, cracked lips, strawberry tongue, swelling of hands and feet, rash). If you cannot reach anyone and your child looks unwell, the ER is the right call.
Quick parent gut-check: If you are thinking, “This fever is different and my child is not improving,” I would rather you be evaluated and reassured than stay home worrying.