Keratosis Pilaris in Kids: Bumpy “Chicken Skin”
Sarah Mitchell
Sarah Mitchell is a Registered Pediatric Nurse and a mother of three who has spent over a decade helping families navigate the beautiful, chaotic early years of childhood. She combines evidence-based medical knowledge with real-world parenting experience to offer practical, compassionate advice. At Awesome Parent, Sarah's mission is to help exhausted parents find solutions, trust their instincts, and finally get some sleep.
If your child’s upper arms feel like fine sandpaper or look like tiny “goosebumps” that never go away, you are very likely looking at keratosis pilaris, often nicknamed “chicken skin.” As a pediatric nurse and a mom who has personally bought approximately 47 different lotions at 2 AM, I can tell you this: KP is extremely common, not dangerous, and usually more annoying than anything else.
The goal is not to “scrub it off.” The goal is to keep skin comfortable, smooth it gently over time, and know when bumps are actually something else.
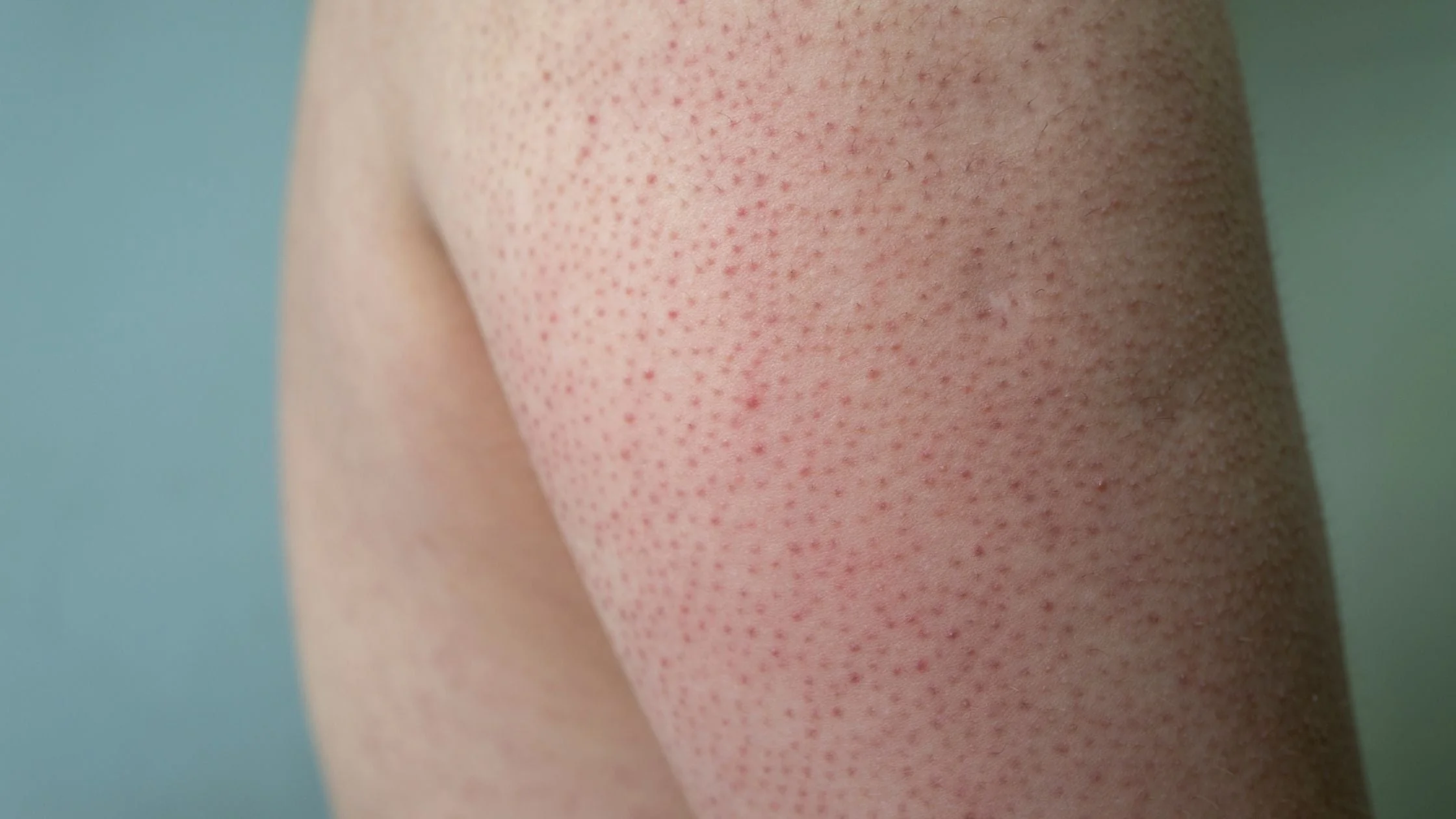
What keratosis pilaris looks like
KP happens when keratin (a normal skin protein) plugs the openings of hair follicles. Those tiny plugs show up as small bumps.
- Size: pinhead-sized bumps
- Texture: rough, dry, “sandpapery” to the touch
- Color: skin-colored, white, pink, or light red (often more noticeable on lighter skin); on deeper skin tones the bumps may look darker or ashy with mild discoloration around follicles
- Common spots: outer upper arms (classic), thighs, buttocks, and sometimes cheeks
- Itch or pain: usually not painful; may be mildly itchy if the skin is very dry
KP often becomes more obvious in cold, dry weather or after long hot baths, and it can run in families. Many kids who have KP also have a history of dry skin, allergies, or eczema, but KP itself is not an allergy and is not contagious.
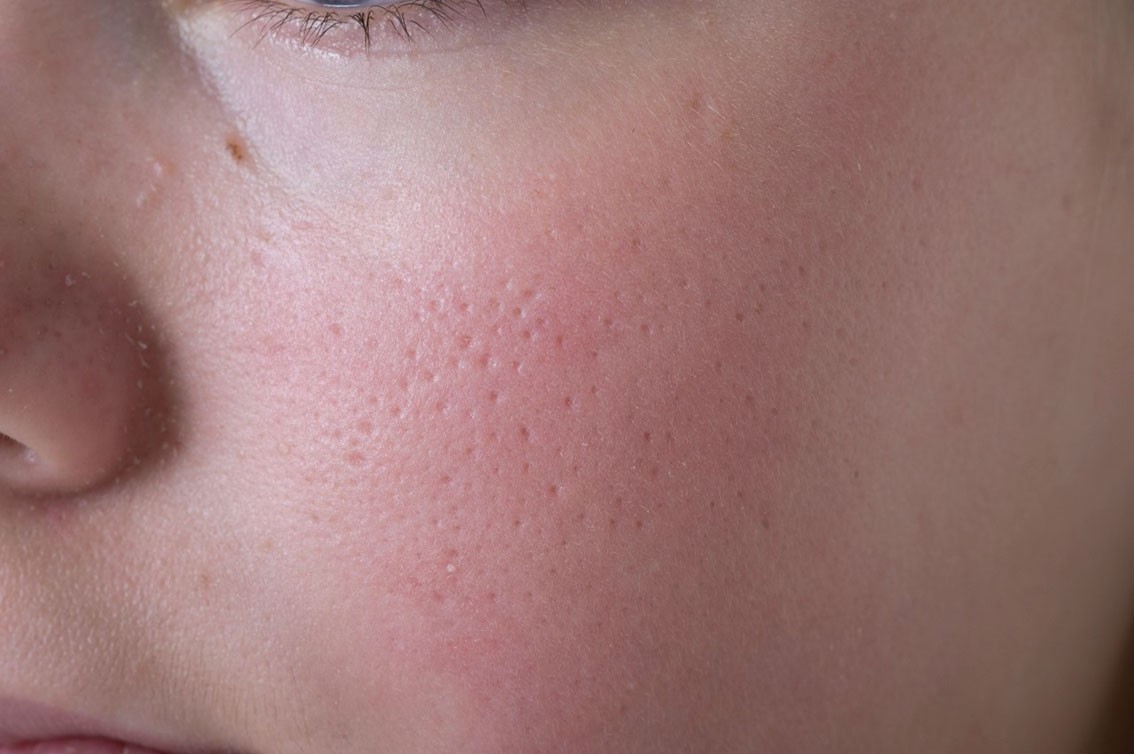
Is KP harmful?
Almost always, no. KP is considered benign, meaning it is harmless even if it is stubborn. It does not turn into anything dangerous, and it is not a sign you missed a hygiene step.
Most kids see it improve gradually with age, often in later childhood or the teen years. Some people still have it as adults, especially in winter, and it tends to come and go.
KP vs eczema vs folliculitis: how to tell the difference
Parents frequently land on three possibilities: KP, eczema, or infection. Here are the practical clues I use in triage when a parent describes “bumps on the arms.”
Keratosis pilaris (KP)
- Tiny, uniform bumps clustered around follicles
- Feels rough and dry
- Usually not very itchy
- Often on outer upper arms, thighs, buttocks, cheeks
- Does not ooze or crust
Eczema (atopic dermatitis)
- More of a patch than uniform bumps, though it can look bumpy when inflamed
- Itchy is the big giveaway, sometimes intensely
- Skin may look red, scaly, cracked, or thickened
- Common in elbow creases, behind knees, wrists, neck, cheeks in younger kids
- May flare with soaps, fragrances, heat, drool, stress, illness
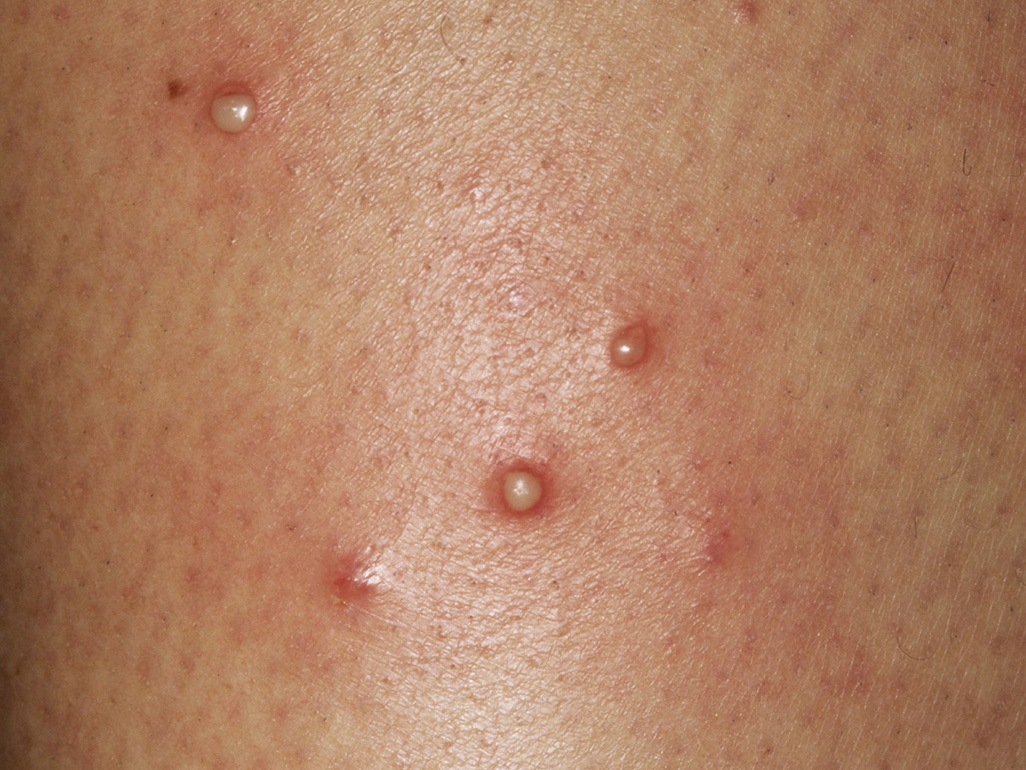
Folliculitis (inflamed or infected follicles)
- Bumps often look like pimples or small pustules
- May be tender, sore, or warm
- Can show a white head, crusting, or drainage
- Often follows sweating, friction, tight clothing, hot tubs, or shaving (older kids/teens)
- Can spread or worsen quickly
If bumps are painful, draining, spreading fast, or your child has a fever, think beyond KP and get medical advice.
What causes KP in kids?
KP is mainly about how your child’s skin naturally builds and sheds keratin. In some kids, that keratin forms tiny plugs in hair follicles instead of sloughing off smoothly.
Things that commonly make KP more noticeable:
- Dry air and low humidity
- Hot water and long baths
- Harsh soaps or frequent scrubbing
- Friction from clothing (sports uniforms, snug sleeves)
- Underlying dry skin or eczema-prone skin
Gentle KP care that actually helps
KP responds best to a steady, boring routine. Think: soften, moisturize, and be consistent. Most families see improvement in a few weeks, but it is normal if it takes longer.
1) Stop the “scrub it off” cycle
I know it is tempting. Those bumps look like they should pop or peel. But picking and aggressive exfoliation can cause irritation, scabs, and post-inflammatory dark marks, especially on cheeks and on deeper skin tones.
- Avoid harsh scrubs, loofahs, and gritty exfoliants
- Avoid picking or squeezing
- Keep nails trimmed if your child scratches when dry
2) Short, lukewarm baths and gentle cleanser
- Keep baths and showers around 5 to 10 minutes
- Use lukewarm water (hot water dries skin out fast)
- Choose fragrance-free, gentle cleansers
- Pat dry, do not rub
3) Moisturize like it is your job (especially right after bathing)
The best timing is within 3 minutes of getting out of the bath or shower, when skin is still slightly damp.
- Use a thick, fragrance-free cream or ointment on arms, thighs, and cheeks
- Apply at least once daily, twice if skin is very dry
4) Consider a “smoothing” moisturizer a few nights a week
For some kids, ingredients that gently loosen dead skin can help KP feel smoother. Common options include:
- Lactic acid
- Urea
- Salicylic acid (often used more in older kids/teens)
Important: These can sting on sensitive skin, eczema patches, or chapped cheeks. Start slowly, use a small amount, and avoid broken skin. For toddlers and preschoolers, ask your pediatrician before using strong “active” products, especially on the face.
5) Protect cheeks from extra irritation
Cheek KP can look worse with wind, drool, and winter dryness.
- Use a gentle, fragrance-free moisturizer twice daily
- In cold weather, add a thin layer of a bland ointment on top as a barrier
- Avoid harsh acne products on kids’ cheeks unless advised by a clinician
How long does it take to improve?
KP is a marathon, not a sprint. With consistent gentle care, many families notice:
- 1 to 2 weeks: less dryness and less roughness
- 3 to 6 weeks: bumps look smaller or less red
- Ongoing: it often returns if you stop all moisturizing, especially in winter
If you are doing the basics and seeing no improvement after about 6 to 8 weeks, it is reasonable to check in with your pediatrician or a dermatologist for tailored options.
When “KP” might be something else
Trust your instincts. If the rash is acting unlike the typical dry, uniform KP bumps, it is worth getting it checked.
Call your child’s clinician if you notice:
- Rapid spreading, significant redness, warmth, swelling, or pain
- Pus, crusting, open sores, or drainage
- Fever or your child seems sick
- Severe itch that keeps your child up at night (more eczema-like)
- Honey-colored crusts (can suggest impetigo)
- Blistering, hives, or swelling of lips/eyes
- A new rash after starting a medication
- Bumps that look like warts, or a rash that is concentrated in body folds with bright redness
Seek urgent care now for:
- Any trouble breathing, wheezing, or swelling of the face or tongue
- Rash with purple spots that do not fade when pressed and your child looks ill
- Signs of dehydration or extreme sleepiness along with a rash
Quick KP checklist for tired parents
- KP is common, harmless, and not contagious.
- It looks like tiny, uniform, rough bumps on upper arms, thighs, buttocks, and sometimes cheeks.
- Moisturize daily, keep baths short and lukewarm, and skip harsh scrubs.
- Do not pick. It can scar or leave dark marks.
- Call the pediatrician if bumps are painful, draining, spreading fast, or paired with fever.
If you needed permission to stop trying to “fix” KP overnight, here it is. Think comfort and consistency, not perfection.