Lead Poisoning in Kids
Sarah Mitchell
Sarah Mitchell is a Registered Pediatric Nurse and a mother of three who has spent over a decade helping families navigate the beautiful, chaotic early years of childhood. She combines evidence-based medical knowledge with real-world parenting experience to offer practical, compassionate advice. At Awesome Parent, Sarah's mission is to help exhausted parents find solutions, trust their instincts, and finally get some sleep.
If you are a parent of a baby or toddler, “lead” is one of those words that can send your brain straight into late-night panic mode. Take a breath with me. Most kids will never have a harmful lead exposure, and there are clear steps you can take to lower risk. The tricky part is that lead can be sneaky, and the symptoms can be subtle or look like a lot of other everyday kid things.
This page will help you spot the common hidden sources, understand the early clues, and know the typical screening ages so you can make a plan with your child’s pediatrician without spiraling.
What lead is and why kids are more vulnerable
Lead is a metal that used to be common in paint, plumbing, and some consumer products. When lead dust or chips get into a child’s body, it can affect the brain and nervous system. Young children are at higher risk because they crawl, put hands and toys in their mouths, and absorb more lead than adults do.
Important and reassuring: lead exposure is preventable, and finding an elevated blood lead level early gives you a chance to stop the source and protect development.
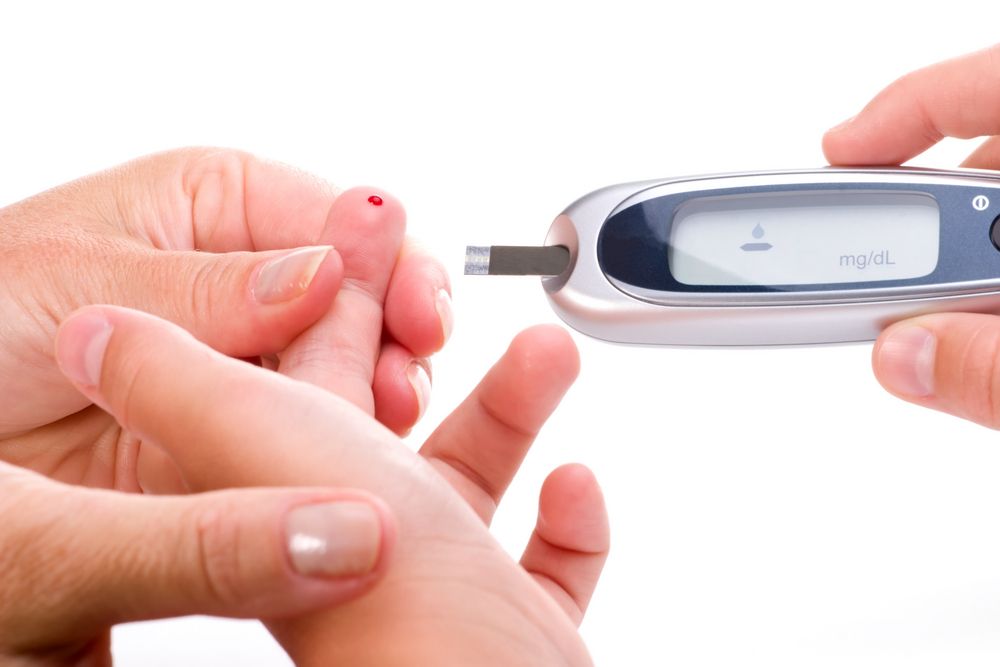
What “elevated” means
A blood lead test is measured in micrograms per deciliter (µg/dL). In the US, the CDC uses a blood lead reference value of 3.5 µg/dL to flag children with levels higher than most kids and to guide follow-up. Also important: no level of lead is considered completely safe. Even “low” levels can matter over time, which is why prevention and early detection are so helpful.
Hidden sources of lead most parents do not expect
When families think about lead, they usually think “old paint.” That is a big one, but it is not the only one. Here are the sources I see surprise parents most often.
Homes built before 1978
In the US, lead-based paint was banned for residential use in 1978. Homes built before then may have lead paint under newer layers. The biggest risk is paint that is chipping, peeling, or disturbed during renovations. (And yes, there can still be lead risks after 1978 in certain situations, but pre-1978 housing remains the key cutoff used for screening and prevention.)
- High-risk areas: windows, window wells, doors, stairs, baseboards, and porches where friction creates dust.
- Renovations: sanding, scraping, and demolition can create a lot of lead dust fast.
Lead in water from older plumbing
Some older homes have lead service lines, lead solder, or older fixtures. Lead can leach into water, especially when water sits in pipes overnight.
- Tap testing is most actionable. City water reports are helpful for system-wide trends, but they do not tell you what is happening at your specific faucet. If you are concerned, consider testing your home’s tap water (often with a “first-draw” sample and a flushed sample).
- If you use a filter, make sure it is certified to reduce lead and that you replace cartridges on schedule.
Soil around older buildings and busy roads
Lead can linger in soil from old exterior paint and past vehicle emissions. Kids can track it inside on shoes or get it on hands while playing.
Think: bare dirt near an older house, along a foundation, or in an urban area with heavy traffic history.
Imported products and certain traditional remedies
Some imported items have been found to contain lead, including certain spices, cosmetics, remedies, candies, and pottery glazes. This does not mean all imported goods are unsafe, just that it is worth being thoughtful about sources and recalls.
- Spices and powders: especially if purchased from informal markets or brought from abroad.
- Traditional remedies: some have been associated with lead contamination.
- Candy and foods: occasional recalls involve contamination from ingredients or packaging.
- Ceramic dishware and leaded crystal: lead can be in glazes or crystal and may leach into food or drinks, especially with acidic liquids.
Toys, jewelry, and older consumer items
Some toys or children’s jewelry (especially older, imported, or recalled products) have been found to contain lead. It is less common than paint, but it is not zero.
- Check recall lists if you have concerns about a specific product.
- Be cautious with old painted toys or hand-me-downs with unknown history.
Jobs and hobbies that bring lead dust home
Lead can hitch a ride on clothing, shoes, skin, and gear.
- Construction, renovation, painting, plumbing, battery manufacturing or recycling, and certain industrial jobs
- Hobbies like making stained glass, using lead sinkers or fishing weights, indoor firing ranges, furniture refinishing, or working with old painted items

Symptoms: what lead exposure can look like
One of the hardest parts is that many children with elevated blood lead levels have no obvious symptoms. When symptoms do show up, they can look like common childhood issues.
Possible early clues
- More irritability than usual
- Trouble paying attention or increased distractibility
- Sleep problems
- Lower appetite
- Stomach pain, constipation, nausea, or vomiting
- Headaches
- Slower growth
- Developmental delays or learning difficulties over time
- Anemia (often picked up on labs, sometimes with fatigue or pallor)
When to call the pediatrician promptly
Call your child’s pediatrician if you have a known exposure (for example, peeling paint your child mouthed, a renovation dust event, or a product recall) or if you are seeing a cluster of symptoms and you live in a higher-risk setting like an older home. You do not have to “prove” anything to ask for guidance. That is what your child’s care team is here for.
Parenting reality check: toddlers are chaotic, picky, and occasionally constipated. The goal is not to diagnose lead poisoning from behavior. The goal is to notice risk factors and screen when appropriate.
Screening ages: when kids are tested
The most reliable way to know if a child has been exposed is a blood lead test. Screening recommendations vary by state, insurance, and your child’s risk factors.
Common screening timeline
- Around 12 months: many children are screened or assessed for risk at the 1-year visit.
- Around 24 months: a repeat test is common in higher-risk settings. In many states, this is required for children enrolled in Medicaid.
- Ages 3 to 6 years: children who were not screened earlier or who have ongoing risk factors may need testing during these years.
Risk-based screening
Your pediatrician may recommend testing sooner or more often if your child:
- Lives in or regularly visits a home built before 1978, especially with peeling paint or recent remodeling
- Has a sibling or playmate with elevated blood lead levels
- Has pica (eating non-food items) or frequent hand-to-mouth behavior beyond what is typical
- Uses certain imported products, spices, remedies, or cookware with possible lead exposure
- Has a household member with a lead-related job or hobby
- Recently immigrated, been adopted internationally, or spent time in settings with less regulated consumer products
Finger prick vs. blood draw
Many offices start with a finger prick (capillary) screening. If that result is elevated, your child may need a confirmatory venous blood draw (from the arm). Finger prick samples can pick up lead from skin contamination, so the confirmation step is important.
Confirmatory testing timing
If a capillary screening test is high, your pediatrician will recommend a venous confirmation within a specific timeframe based on the result. Higher screening levels are confirmed sooner. If you are ever unsure what timeline applies, ask directly, “When should we confirm this with a venous test?”
What happens if a level is elevated?
If your child’s blood lead level is higher than it should be, the next steps usually focus on:
- Confirming the result (if needed)
- Finding the source (home, water, product, soil, work or hobby exposure)
- Stopping exposure as quickly as possible
- Follow-up testing based on the level and local guidance
- Checking for iron deficiency and anemia and treating if present
- Supporting nutrition and overall health, which can reduce absorption when deficiencies are addressed
In some cases with higher levels, children may need additional medical evaluation and specific treatments. Your pediatrician can also connect you with local public health resources, including environmental investigations and home risk assessments in some areas.
Simple ways to reduce exposure at home
You do not need to turn your house upside down overnight. Start with the highest impact steps, especially if you live in an older home.
If you live in a pre-1978 home
- Wet-clean, do not dry dust. Use a damp mop or damp cloth on floors, windowsills, and window wells.
- Wash hands often. Before eating and after playing on the floor is the big one.
- Keep paint intact. Do not scrape or sand old paint yourself. Use an EPA lead-safe certified professional for renovation.
- Remove shoes at the door to reduce tracking soil and dust inside.
- Cover bare soil where kids play with grass, mulch, or other safe ground cover.
Water habits that help
- Use cold water for cooking and mixing formula since hot water can leach more from pipes.
- Flush the tap by running cold water until it runs cold if it has not been used for several hours. (This is often 30 seconds to 2 minutes, but follow your local utility guidance, especially if a lead service line is suspected.)
- Consider a certified lead-reducing filter if you have any reason to be concerned.
Food and nutrition support
Nutrition cannot “detox” lead or quickly lower an already-elevated blood lead level. But addressing deficiencies can reduce how much lead a child absorbs and supports a growing brain.
- Iron: lean meats, beans, lentils, iron-fortified cereals (and treat iron deficiency if present)
- Calcium: dairy, fortified alternatives, tofu, leafy greens
- Vitamin C: berries, citrus, peppers, tomatoes (helps with iron absorption)
Work and hobby precautions
- Change clothes and shoes before coming inside if you work with lead
- Wash work clothes separately
- Shower as soon as possible after exposure
- Keep hobby materials and tools away from kids and common living areas

Quick risk checklist
If you want a fast gut-check, here it is. Consider asking your pediatrician about testing if you answer “yes” to any of these:
- My child lives in or regularly visits a home built before 1978.
- We have peeling paint, old windows, or recent remodeling in an older home.
- My child spends time around bare soil near an older building.
- Someone in our household has a lead-related job or hobby.
- We use imported spices, remedies, cosmetics, candy, or older pottery or crystal for food or drinks.
- A sibling or close contact has had elevated lead levels.
When to seek urgent help
Severe lead poisoning is uncommon, but if your child has concerning symptoms like extreme lethargy, repeated vomiting, seizures, or significant confusion, seek urgent medical care right away. If you know your child had a significant exposure event, call your pediatrician or Poison Control for guidance (US: 1-800-222-1222).
The bottom line
Lead is worth taking seriously, but it is also something you can tackle in a calm, practical way. Focus on risk factors, keep dust under control, be careful with renovations and certain imported products, and follow your pediatrician’s screening guidance. If you are worried, you are not overreacting. You are doing what good parents do, noticing and asking.
Bring your child’s age, where they spend time, and the year your home was built to your pediatrician so you can decide on the most sensible next steps together.