Lyme Disease in Kids: Tick Bite Signs and What to Do
Sarah Mitchell
Sarah Mitchell is a Registered Pediatric Nurse and a mother of three who has spent over a decade helping families navigate the beautiful, chaotic early years of childhood. She combines evidence-based medical knowledge with real-world parenting experience to offer practical, compassionate advice. At Awesome Parent, Sarah's mission is to help exhausted parents find solutions, trust their instincts, and finally get some sleep.
If you have ever found a tick on your child, you know the instant stomach drop. Take a breath. Most tick bites do not lead to Lyme disease. Risk varies a lot by region and tick species, and when Lyme is caught early, treatment is straightforward and very effective.
As a pediatric nurse and a mom who has done the post-hike “everybody strip at the door” routine more times than I can count, here is what I want you to know: what a tick bite looks like, what early Lyme symptoms in kids can look like (including the classic bullseye rash), how to remove a tick safely, when to call the doctor, and how to prevent bites in the first place.
Tick found: 5 things to do now
- Remove the tick with fine-tipped tweezers or a tick tool.
- Clean the skin with soap and water (or an alcohol wipe).
- Save the tick in a sealed bag or container if you can.
- Write it down: date, where on the body, and your best guess on how long it was attached (when you last did a tick check, or whether it looked flat vs swollen).
- Take a photo of the bite area today so you can compare it later.
Quick Lyme disease reality check
Lyme disease is caused by bacteria (most commonly Borrelia burgdorferi) spread through the bite of infected blacklegged ticks (often called deer ticks). Lyme risk depends on:
- Where you live or traveled. In the U.S., risk is highest in parts of the Northeast, Mid-Atlantic, and Upper Midwest, but Lyme can occur elsewhere.
- What kind of tick it was (not all ticks spread Lyme).
- How long it was attached. Risk rises when a tick is attached longer. Many clinical guidelines use an estimated attachment time of about 36 to 48 hours as a meaningful threshold for higher risk, but it is not absolute.
Many families come to clinic worried that any tick equals Lyme. It does not. The goal is to remove the tick promptly, document what you can, watch for symptoms, and get medical care if signs of Lyme show up.
How to identify a tick bite
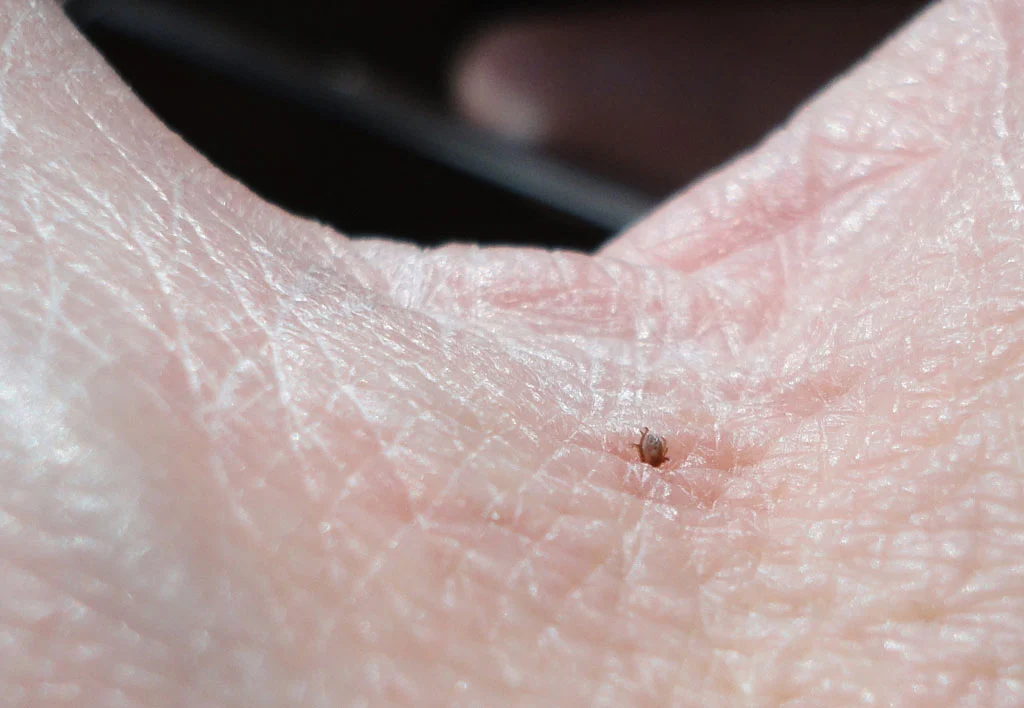
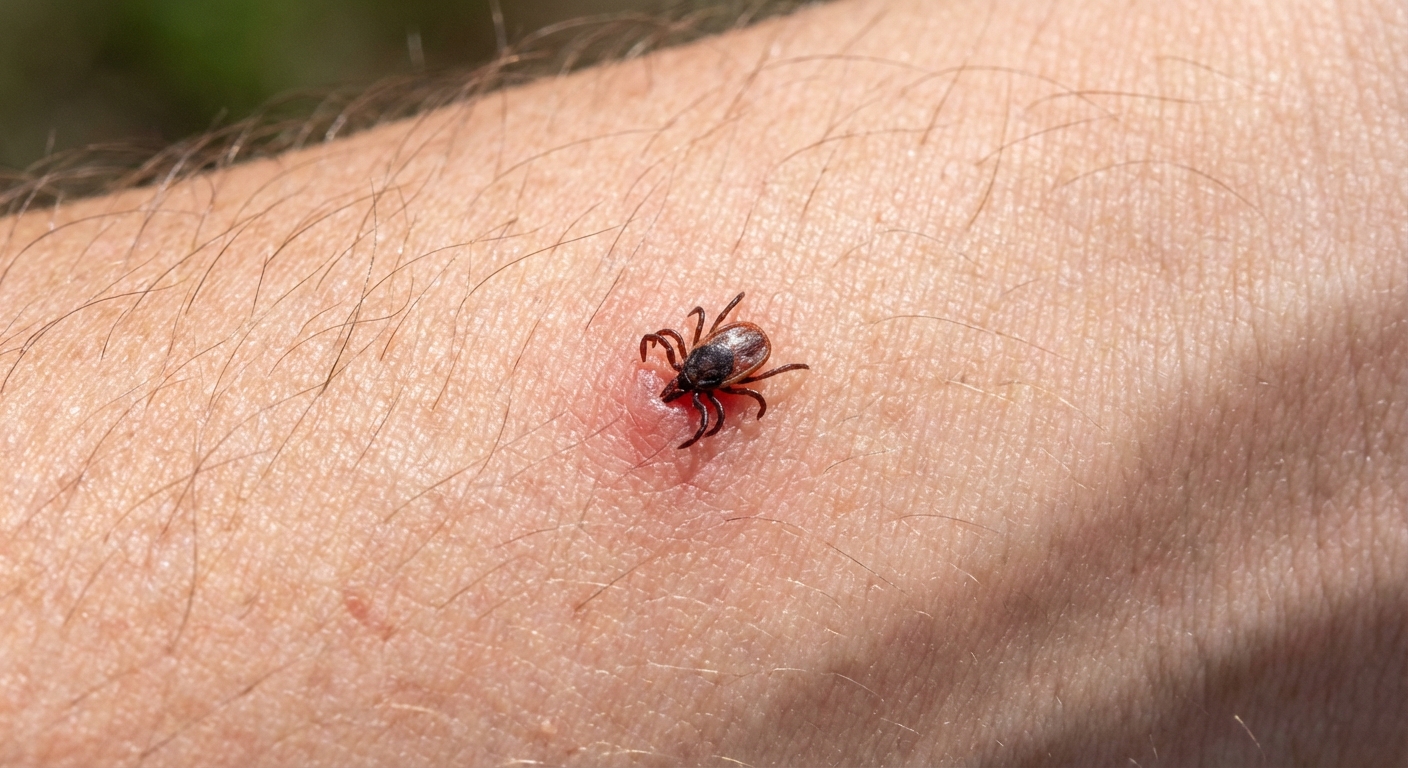
What a tick looks like
Ticks can be tiny. Some are as small as a poppy seed (nymph stage), which is why they are so easy to miss. When they have been feeding, they may look larger and rounder (engorged).
Common hiding spots on kids
If you are doing a tick check, focus on warm, tucked-away areas:
- Scalp and hairline (especially behind the ears)
- Back of the neck
- Armpits
- Belly button
- Waistband and groin area
- Behind knees
- Between toes
On kids, ticks often show up along clothing lines where they can crawl under snug fabric.
What the bite looks like
A tick bite can look like:
- A small red bump, similar to a mosquito bite
- A tiny scab or pinpoint mark
- Mild redness right around the bite
It is also common for the area to be a little itchy or irritated for a day or two. That alone is not a sign of Lyme disease.
Early Lyme symptoms in kids
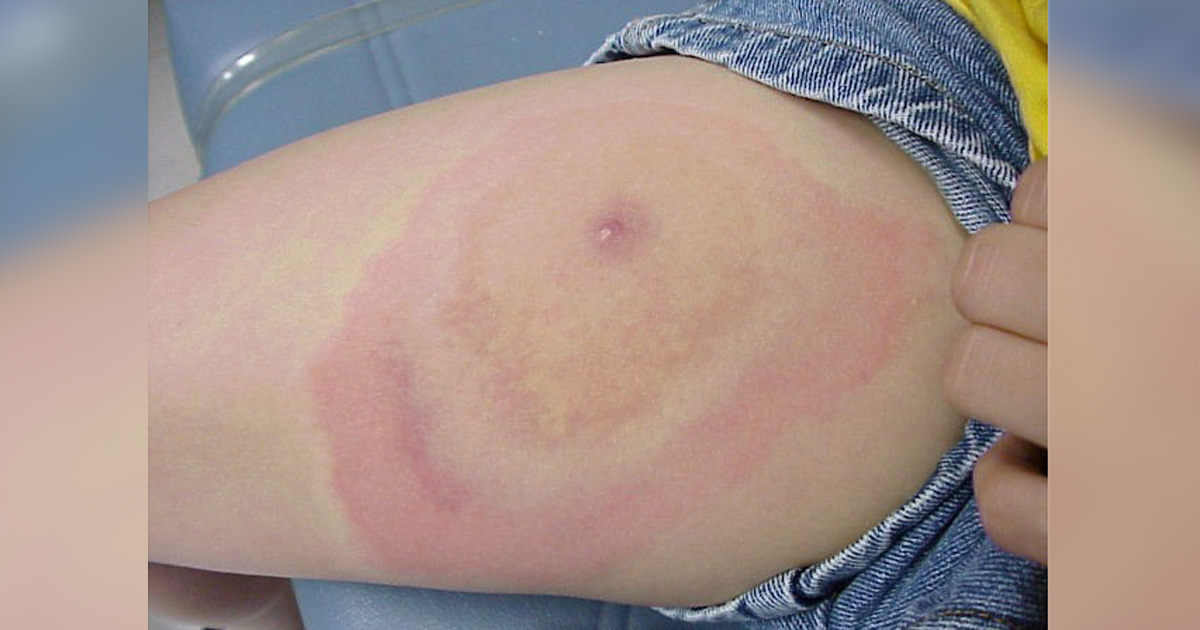
The bullseye rash
The best-known early sign of Lyme disease is a spreading rash called erythema migrans. It is often described as a “bullseye,” but here is the important parent truth: it does not always look like a perfect target.
In kids, the Lyme rash may be:
- Expanding over days
- Round or oval
- Uniformly red (no central clearing)
- Warm but usually not painful
- Not very itchy compared with typical bug bites
Size matters here. Erythema migrans is often larger than 5 cm (about 2 inches) and continues to grow. The rash typically shows up 3 to 30 days after the bite. Some children develop more than one rash spot if the infection spreads.
Early symptoms that look like a virus
Early Lyme disease can also look a lot like “some random summer virus,” which is why your instincts matter. Symptoms can include:
- Fever or chills
- Fatigue that feels out of proportion
- Headache
- Muscle aches or joint aches
- Swollen lymph nodes
If your child has these symptoms and a known tick bite, heavy tick exposure, or a suspicious expanding rash, it is worth calling your pediatrician.
Other tick illnesses
Ticks can carry other infections too, depending on your region (examples include anaplasmosis, babesiosis, and Rocky Mountain spotted fever). If your child develops fever, headache, significant fatigue, new rash, or unusual symptoms after tick exposure, call your child’s clinician even if you never see a bullseye rash.
Later symptoms
If Lyme is not treated early, children may develop symptoms weeks to months later, such as:
- Joint swelling and pain (often a large joint like the knee)
- Facial droop (Bell palsy)
- Severe headache or neck stiffness
- Heart rhythm symptoms (rare, but important)
These deserve prompt medical evaluation.
When to see a doctor
Call your child’s doctor or seek urgent care if:
- You see an expanding rash, especially one that is getting bigger day by day
- Your child has flu-like symptoms within a month of a tick bite or heavy tick exposure
- You cannot remove the tick fully, or the skin looks increasingly red, painful, swollen, or is draining pus
- Your child develops facial weakness, significant joint swelling, severe headache, or neck stiffness
- Your child is under 3 months old and has any fever after a bite
If you are unsure, it is completely reasonable to call. This is exactly the kind of “I just need a quick professional brain on this” situation triage nurses are built for.
How to remove a tick safely
You do not need fancy tools, but you do need the right technique.
What you need
- Fine-tipped tweezers or a tick removal tool
- Soap and water (or alcohol wipes)
- A small container or zip bag (optional, to save the tick)
Step-by-step removal
- Stay calm and hold still. If your child is squirmy, have another adult help or use a distraction.
- Grasp the tick close to the skin. Aim for the head or mouthparts, not the swollen belly.
- Pull upward steadily. Use slow, even pressure. If you are using a tick tool, follow the tool’s instructions.
- Clean the area. Wash with soap and water, or use an alcohol wipe.
- Wash your hands.
Avoid “home hacks” like burning the tick, painting it with nail polish, petroleum jelly, or essential oils. Public health guidance advises against these because they can irritate the tick and may increase the risk of transmission.
Also avoid squeezing, crushing, or popping the tick with bare fingers.

If mouthparts break off
This is common and understandably gross. If tiny parts remain, you can try gently removing them with clean tweezers like you would a splinter. If they will not come out easily, do not dig. Clean the area and call your child’s doctor if the skin becomes increasingly red, tender, or starts draining.
Should you save the tick?
If you can, place it in a sealed bag or small container. Write down the date and where on the body it was found, plus your best estimate of attachment time (flat vs engorged, and when your child was last tick-free). Some clinicians may find it helpful for identification.
Not all areas recommend or rely on tick testing, and a positive tick test does not always mean your child was infected. Still, saving it can be useful information.
Do kids need antibiotics after a tick bite?
Sometimes, but not always. In many cases, the best plan is careful observation and watching for symptoms.
In certain higher-risk situations, clinicians may prescribe a single preventive dose of an antibiotic (often doxycycline) when key criteria are met. Common criteria used in practice include:
- The tick is an Ixodes tick (blacklegged or deer tick) or looks very likely to be one
- Estimated attachment time is 36 hours or more (often based on engorgement and history)
- The tick was removed within the past 72 hours
- Lyme is common in your area (or where the exposure happened)
- No medical reason your child should not receive doxycycline
One more reassuring update for parents: current guidance allows doxycycline prophylaxis for children of all ages in appropriate situations, with clinician guidance.
If your child has an erythema migrans rash or other signs of early Lyme disease, your clinician will typically treat with a course of antibiotics. Common options (depending on age and the clinical situation) include doxycycline, amoxicillin, or cefuroxime.
Also worth saying plainly: most children do not need routine antibiotics or routine blood tests after every tick bite, especially in low-risk situations.
Treatment timeline
For early localized Lyme disease, antibiotic courses are often in the range of 10 to 14 days, depending on the medication (for example, doxycycline is often 10 days; amoxicillin or cefuroxime are often 14 days). Some presentations need longer courses (for example, Lyme arthritis is often treated for about 28 days).
When will my child feel better?
- Fever and energy often improve within a few days.
- Rash may take longer to fade, even as treatment works.
- Aches can take a bit to settle down.
Call the prescriber if symptoms are worsening after starting antibiotics, your child cannot keep medicine down, or you notice new concerning symptoms.
If your child is treated for Lyme and still seems tired for a while, you are not imagining it. Recovery can be gradual. Keep your pediatrician in the loop, and focus on hydration, sleep, and a gentle return to activity.
Will a blood test confirm Lyme?
Sometimes, but timing matters. Early in infection, Lyme antibody blood tests can be negative because the body has not made enough antibodies yet.
When a child has the classic expanding erythema migrans rash, many clinicians treat based on the exam and history rather than waiting on blood tests. If symptoms suggest later disease, testing may be more helpful.
Aftercare at home
- Clean the bite and keep it dry.
- Take a photo of the bite area the day you remove the tick. Then take another if redness spreads.
- Track symptoms for 30 days, especially expanding rash, fever, unusual fatigue, headaches, facial weakness, and joint swelling.
- Relieve itch with a cool compress or an age-appropriate anti-itch option recommended by your pediatrician.
Preventing tick bites
Prevention is not about keeping kids indoors. It is about making tick checks as normal as sunscreen.
Before you go outside
- Dress smart: long sleeves and pants in wooded or grassy areas when possible. Light-colored clothing makes ticks easier to spot.
- Use repellent: choose an EPA-registered insect repellent appropriate for kids and follow the label. Apply to exposed skin as directed, and avoid hands, eyes, and mouth.
- Consider treated clothing: permethrin-treated clothing and gear can reduce tick bites (permethrin is for clothes and gear, not skin).
While playing
- Stay on clear trails when possible.
- Avoid brushing against tall grass and leaf litter.
When you get home
- Do a full tick check right away.
- Shower or bathe soon after outdoor time if you can, which helps wash off unattached ticks and makes checks easier.
- Dry clothes on high heat for at least 10 minutes before washing, when possible. Heat helps kill ticks on clothing.
- Check pets, especially around ears, collar lines, and between toes. Pets can bring ticks inside.

FAQ parents ask at 3 AM
Does every tick bite cause Lyme?
No. Many ticks are not the type that spreads Lyme, and even infected ticks do not always transmit it. Prompt removal reduces risk.
How soon does Lyme show up?
The rash can appear 3 to 30 days after the bite. Other early symptoms may show up in that same window.
My child has a red bump after a tick bite. Is that Lyme?
A small red bump right after a bite is common and does not automatically mean Lyme. What raises concern is a rash that expands over days, especially if it becomes larger than 5 cm (about 2 inches).
Should I put the tick in alcohol?
After removal, you can keep the tick in a sealed container or bag. Alcohol can preserve it, but it is not required. The important part is documenting the date, where it was attached, and your best estimate of attachment time.
Bottom line
If you find a tick on your child, remove it promptly with fine-tipped tweezers (or a tick tool), clean the area, and watch for an expanding rash or flu-like symptoms over the next few weeks. When in doubt, call your pediatrician. You are not overreacting. You are doing exactly what a steady, protective parent does.
Medical note: This article is for general education and does not replace medical care. If your child is ill, has a spreading rash, or you are concerned for any reason, contact your pediatrician or seek urgent evaluation.