Measles in Kids: Rash Stages, Contagious Period, Vaccines, and Isolation
Sarah Mitchell
Sarah Mitchell is a Registered Pediatric Nurse and a mother of three who has spent over a decade helping families navigate the beautiful, chaotic early years of childhood. She combines evidence-based medical knowledge with real-world parenting experience to offer practical, compassionate advice. At Awesome Parent, Sarah's mission is to help exhausted parents find solutions, trust their instincts, and finally get some sleep.
If you are reading this at an odd hour with a worried knot in your stomach, take a breath with me. Measles can sound scary because it spreads easily, but having clear steps helps a lot. This page will walk you through what measles looks like in kids, how the rash usually progresses, when children are contagious, what vaccine status really means, and the basics of isolation and next steps after an exposure.
Quick summary: Think measles when a child has high fever plus the 3 C’s (cough, runny nose, red watery eyes), followed by a rash that often starts on the face and moves downward. Kids are usually contagious from about 4 days before the rash starts through 4 days after. If measles is possible, call your pediatrician or urgent care before you go in.
Quick safety note: If your child might have measles, call your pediatrician or urgent care before you arrive so they can protect other patients in the waiting room.

What measles is
Measles is a viral infection that spreads through the air when an infected person breathes, coughs, or sneezes. It is highly airborne: measles virus can remain infectious in the air for up to about 2 hours after a contagious person leaves a room. Spread from surfaces is considered much less common than airborne spread, but good hand hygiene is still a sensible habit during any illness season.
Most kids recover, but measles can cause serious complications, especially in babies, pregnant people, and anyone with a weakened immune system.
Symptoms before the rash
Measles usually starts like a rough cold, then ramps up. The classic early symptoms include:
- Fever (often high)
- Cough
- Runny nose (coryza)
- Red, watery eyes (conjunctivitis)
- Low energy and poor appetite
Some children develop Koplik spots, which are tiny bluish white spots inside the mouth, often on the inner cheeks. Parents do not always notice them, and that is okay. The overall pattern of symptoms plus rash timing is usually more helpful.

Rash stages
The measles rash has a fairly predictable pattern, although every child is a little different. It often looks like flat red spots that can become slightly raised, and the spots may merge together in places.
Stage 1: Starts on the face
The rash usually starts at the hairline and behind the ears, then spreads across the face and down the neck.
Stage 2: Moves down the body
Over the next day or two, the rash typically spreads to the chest and torso, then to the arms and legs.
Stage 3: Fades in the same order
As your child improves, the rash often fades from the face first, then the torso, then the limbs. Some kids have temporary discoloration or mild peeling as it resolves.
What often goes with the rash: The fever can remain high when the rash appears, and kids usually feel quite unwell during this phase.

When kids are contagious
This is the part that surprises a lot of families: kids are contagious before you see the rash.
- Typical contagious window: about 4 days before the rash appears through 4 days after the rash starts (for most otherwise healthy children).
- That means a child can spread measles when it looks like “just a bad cold.”
Important caveat: People with significant immune suppression can sometimes shed virus longer and may need longer isolation. Your clinician and local public health team will guide you.
If your child has a suspected or confirmed measles infection, think back to close contacts during that window: household members, classmates, playdates, family gatherings, and childcare.
How measles is diagnosed
Clinicians diagnose measles based on symptoms, rash pattern, exposure history, and testing when needed. Testing may include:
- A swab (often a nasopharyngeal or throat swab) for RT-PCR
- Blood work for measles antibodies (such as IgM, sometimes with paired testing depending on timing)
Public health departments may get involved quickly, not to alarm you, but because measles control depends on rapid contact tracing and isolation guidance.
Important: Call ahead before going to a clinic or emergency department. Staff can prepare a separate room and reduce exposure to babies and other vulnerable patients.
Complications and red flags
Most children recover with supportive care, but measles can lead to complications. Higher risk groups include:
- Babies (especially under 12 months)
- Unvaccinated children
- Pregnant people
- People with weakened immune systems
Potential complications can include ear infections, diarrhea, dehydration, croup, pneumonia, and brain inflammation (rare, but serious). There is also a very rare late complication called subacute sclerosing panencephalitis (SSPE) that can occur years later.
Get urgent or emergency care now if your child has:
- Trouble breathing, fast breathing, or ribs pulling in with breaths
- Blue or gray lips or face
- Severe sleepiness, confusion, stiff neck, or seizures
- Signs of dehydration (very dry mouth, no tears, significantly fewer wet diapers, dizziness)
- Fever that seems dangerously high for age or a child who looks very ill to you
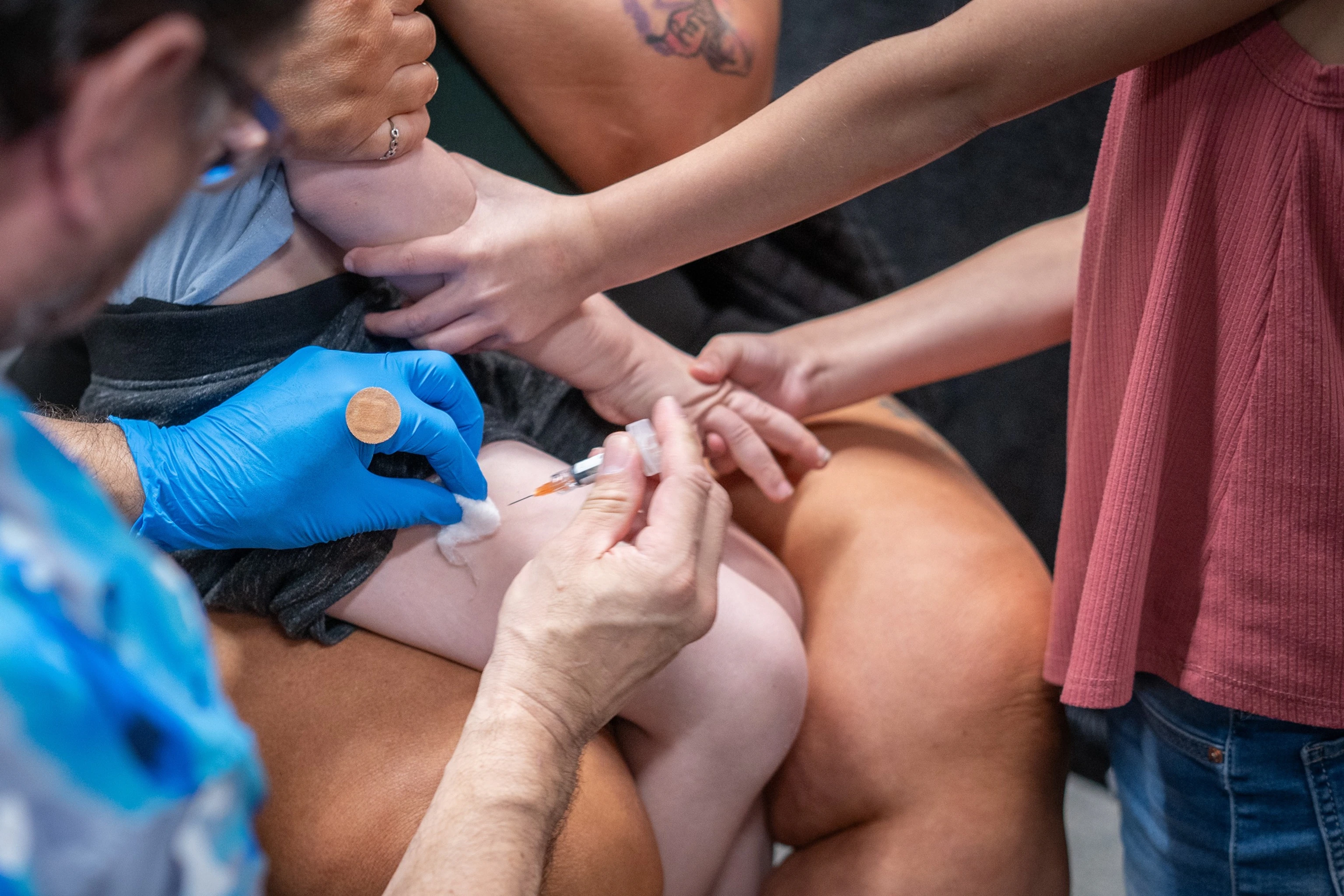
Vaccine protection
The routine measles vaccine is given as part of the MMR series (measles, mumps, rubella). In the United States, the typical schedule is:
- First dose: 12 to 15 months
- Second dose: 4 to 6 years
In outbreaks or for international travel, some children may be eligible for an earlier dose or an accelerated schedule. Your pediatrician or local health department can advise based on your child’s age and local guidance.
How effective is it? The MMR vaccine protects most people: roughly about 93% after one dose and about 97% after two doses.
What if my child is vaccinated? Two doses provide very strong protection. Breakthrough infections are uncommon, and illness is often milder, but no vaccine is 100% for every person. If there is a known exposure, still call your child’s clinician for individualized advice.
Isolation basics
If measles is on the table, isolation is not about blame. It is about protecting infants and medically fragile people who can become seriously ill.
At home
- Stay home and avoid visitors.
- If possible, keep the sick child in a separate room and use a separate bathroom.
- Have one primary caregiver if you can.
- Wear a well-fitting mask if you must be in close contact and your child can tolerate it, especially around others in the home.
- Improve ventilation by opening windows when weather and safety allow.
How long to isolate
Public health guidance commonly recommends isolation through 4 full days after the rash begins (day 0 is the day the rash starts). Your clinician or local health department may adjust this depending on your child’s situation, especially if your child is immunocompromised.
School and daycare
Do not send your child to school or daycare during the contagious period. Even if the fever improves, the contagious window matters more than how “okay” your child looks that day.
What to do after exposure
Measles exposure is usually defined as sharing the same airspace with a contagious person, including being in a room during the infectious period and potentially for up to about 2 hours after the person left. Duration, distance, ventilation, and the setting matter. Even a “brief” time in the wrong place can sometimes count, which is why public health departments use specific criteria.
If you receive an exposure notice from school, daycare, or public health:
- Check vaccine records for your child and other household members.
- Call your pediatrician promptly for next steps. Timing matters.
- Watch for symptoms for up to 21 days after exposure (this is the typical incubation window).
Post-exposure protection (time-sensitive)
Depending on age, vaccine status, pregnancy status, and immune health, clinicians may recommend:
- MMR vaccine within 72 hours of exposure for eligible, susceptible people (this can prevent or lessen illness).
- Immune globulin within 6 days of exposure for certain high-risk contacts (for example: infants too young for routine MMR, pregnant people who are not immune, and people who are severely immunocompromised).
Important: MMR is a live vaccine and is not given during pregnancy, and it may be contraindicated for some people with severe immune suppression. Your clinician will help choose the safest option.
School and work exclusion: After an exposure, quarantine and exclusion rules depend on immunity and local public health instructions. Unvaccinated or not fully vaccinated contacts may be asked to stay home from school, daycare, or work for a specified period.
Home care
There is no at-home cure that makes measles “go away faster.” Care is supportive and focused on comfort and preventing dehydration.
- Fluids first: Offer frequent sips. Popsicles and oral rehydration solutions can help.
- Fever comfort: Use fever medicine only as directed by your clinician. Avoid aspirin in children.
- Rest and low lights: Light can bother kids with red, irritated eyes.
- Watch breathing and hydration closely.
If your child has a chronic condition, is very young, or seems to be worsening instead of gradually improving, call your pediatrician.
What contacts should do
If your child is suspected or confirmed to have measles, it is important to notify close contacts so they can protect vulnerable family members and check immunity.
Contacts should:
- Confirm their MMR vaccination status or documented immunity.
- Ask a clinician promptly if they are pregnant, immunocompromised, or caring for an infant.
- Watch for symptoms for up to 21 days.
Measles vs other rashes
Parents often ask, “Is this measles or something else?” Fair question, because many viruses cause rashes. A few clues that raise measles higher on the list:
- High fever plus the “3 C’s” (cough, runny nose, conjunctivitis)
- Rash that starts on the face and moves downward
- Known exposure or local outbreak
- Unvaccinated or not fully vaccinated status
That said, you cannot confirm measles by photos alone. If measles is possible, call your clinician and avoid waiting rooms until you have a plan.
FAQ
Can my child get measles after MMR?
It is uncommon, especially after two doses, but it can happen. Vaccinated kids who get measles often have milder illness. If there is an exposure, still call your pediatrician for guidance.
Is measles the same as “German measles”?
No. “German measles” refers to rubella, which is a different virus. The MMR vaccine protects against both.
Should I keep siblings home?
If a household member has measles, exposed siblings may need to stay home depending on their immunity and local public health instructions. Your pediatrician or health department can advise for your exact situation.
If you suspect measles
- Call your pediatrician or urgent care first and mention measles concern.
- Keep your child home and avoid visitors.
- Check vaccine records for everyone in the household.
- Follow public health guidance on isolation, testing, and contact notifications.
- Seek urgent care for breathing trouble, dehydration, severe lethargy, seizures, or a child who looks very ill.
You are not overreacting by asking questions. With measles, quick, calm action is the right approach.