Molluscum Contagiosum in Kids: What It Is and When It Goes Away
Sarah Mitchell
Sarah Mitchell is a Registered Pediatric Nurse and a mother of three who has spent over a decade helping families navigate the beautiful, chaotic early years of childhood. She combines evidence-based medical knowledge with real-world parenting experience to offer practical, compassionate advice. At Awesome Parent, Sarah's mission is to help exhausted parents find solutions, trust their instincts, and finally get some sleep.
If you’ve just spotted a cluster of tiny, shiny bumps on your child and your brain immediately went to ringworm? warts? chickenpox? Take a breath. Molluscum contagiosum is a very common childhood skin infection. It looks strange, it can hang around longer than anyone would like, and it is usually harmless.
As a pediatric nurse and a mom of three, I can tell you this is one of those “looks alarming, usually isn’t” situations. The hardest part is often the waiting and the worry, not the bumps themselves.
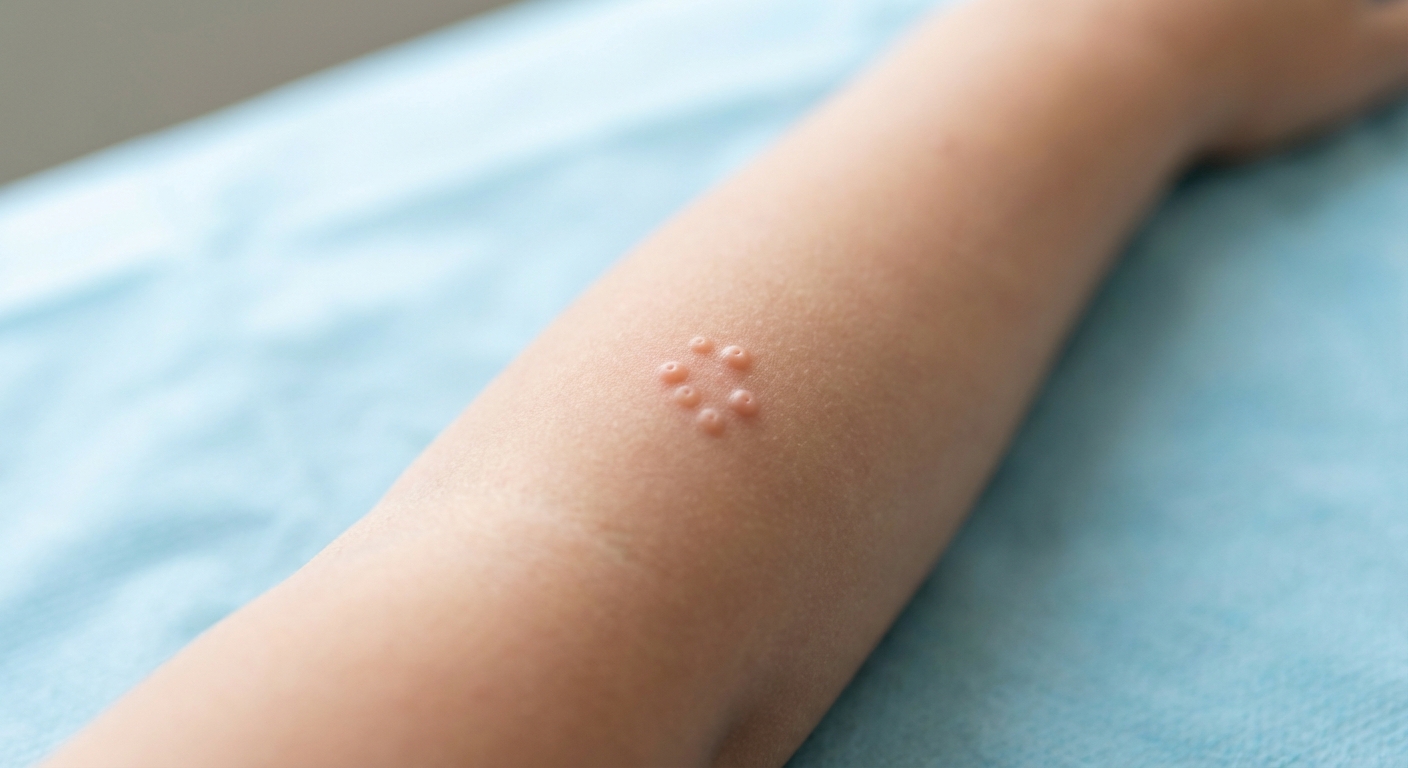
What it is
Molluscum contagiosum is a skin infection caused by a poxvirus (the molluscum contagiosum virus). It stays in the top layer of the skin and causes small, raised bumps.
In healthy kids, it is considered a benign, self-limited condition. In plain language, it is not dangerous and it usually goes away on its own with time.
- Most common age group: toddlers through elementary school kids, but anyone can get it.
- How common is it? Very common in childhood and often shows up in daycare and school-age years.
What the bumps look like
Molluscum has a fairly classic look, once you know what you’re looking for.
Typical appearance
- Small, round, raised bumps (often 2 to 5 mm, but sometimes larger).
- Skin-colored, pearly, or pink.
- Smooth and dome-shaped.
- A tiny “dimple” or pit in the center (called umbilication). This is a big clue.
- Single bump or clusters, and the number can slowly increase over weeks or months.
Common locations in kids
- Trunk (belly, chest, back)
- Arms and armpits
- Behind knees or in skin folds
- Face (less common, but possible)
Note: In children, bumps can sometimes appear in the diaper area from routine skin contact and scratching. If lesions are on or near the genitals, it does not automatically mean sexual contact, but clinicians do evaluate carefully because there are multiple possible causes. It is worth having them checked rather than trying to self-diagnose.
What it feels like
Many kids are not bothered at all. The most common complaint is itching, especially if your child has eczema or sensitive skin.
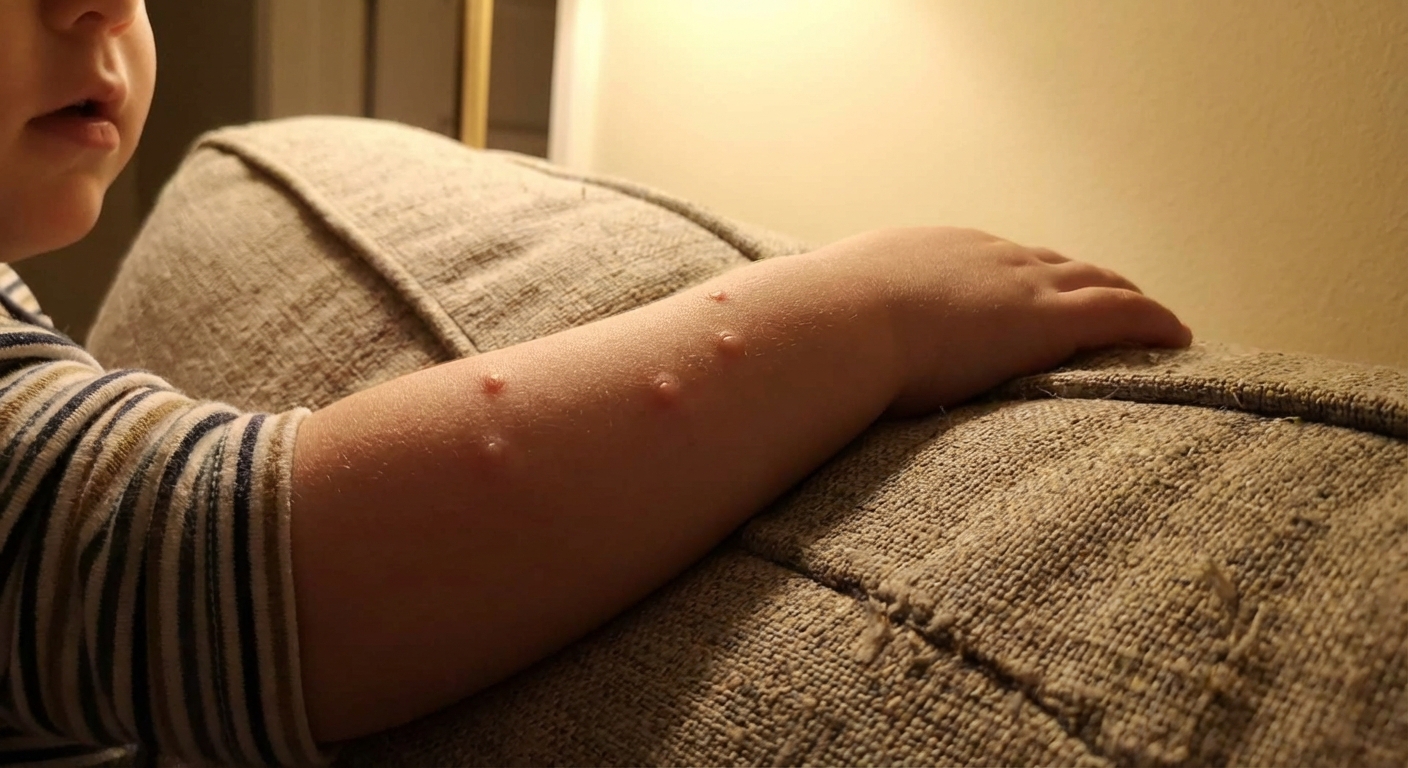
How kids catch it
Molluscum spreads through skin-to-skin contact or by touching objects that carry the virus. It does not spread through the blood. And in the vast majority of healthy kids, it does not mean their immune system is “weak.”
That said, molluscum can look more intense or last longer in kids with eczema (because the skin barrier is disrupted and scratching spreads it) and in children who are immunocompromised or on immune-suppressing medications.
Common ways it spreads
- Direct skin contact: wrestling, roughhousing, hand-holding, contact sports.
- Shared towels and washcloths: bath time, swim lessons, sleepovers.
- Shared sports gear: mats, pads, helmets, or anything that rubs the skin.
- Swimming environments: spread is thought to be more related to shared towels and equipment and close contact around wet skin than to pool water itself.
- Autoinoculation: scratching a bump and then touching another area of skin can “seed” new bumps.
Incubation period: After exposure, bumps can show up anywhere from about 2 weeks to 6 months later (often 2 to 8 weeks, but it varies). This long delay is why parents often cannot pinpoint where it came from.
When it goes away
Here is the honest answer: molluscum is more of a marathon than a sprint.
- Many cases clear in 6 to 12 months.
- Some kids take longer, often 12 to 18 months.
- Occasionally it can last 2 years or more, especially with lots of scratching, significant eczema, or immune suppression.
The bumps usually resolve when your child’s immune system recognizes the virus and clears it. That is why “doing nothing” is sometimes the recommended plan, even though it can feel very unsatisfying.
What healing can look like
Bumps can get red, crusty, or a little inflamed before they disappear. This can be part of the normal immune response. However, redness can also mean irritation from scratching or a secondary skin infection, so context matters.
Why waiting is common
In a healthy child, molluscum is typically self-limited. Many pediatricians and dermatologists recommend watchful waiting because:
- Treatments can be uncomfortable (some sting, blister, or require scraping or freezing).
- Scarring is possible from both treatment and from kids picking at bumps.
- The infection often resolves on its own without any intervention.
- The goal is symptom control (itching, irritation) and preventing spread, not “urgent removal.”
That said, waiting is not the only option. If bumps are spreading quickly, causing distress, or interfering with school, sports, or sleep, it is reasonable to discuss treatment.
Treatment options
The best treatment depends on your child’s age, the location of the bumps, how many there are, and how bothered your child is. Some families choose treatment to reduce spread or because the bumps are persistent.
At-home supportive care
- Hands off policy: easier said than done, but reducing picking and scratching helps a lot.
- Itch control: fragrance-free moisturizer, short nails, and for some kids, your clinician may recommend an anti-itch topical.
- Manage eczema: molluscum often spreads more in kids with eczema because the skin barrier is disrupted.
In-office treatments
- Cantharidin: a topical medicine that is applied by a clinician to cause a controlled blister and help remove lesions. Application is quick, but blistering is expected and it can sting later. Availability can vary by clinic and region.
- Cryotherapy (freezing): can work but may be painful and is sometimes difficult for younger kids.
- Curettage (gentle scraping or removal): effective in some cases, but can be uncomfortable and may require numbing.
- Topical prescription options: sometimes used, especially for older kids, depending on clinician preference and the child’s skin. Results vary.
A quick safety note: Please do not try “popping” molluscum bumps. The core material can spread the virus to nearby skin, and it increases the risk of infection and scarring.
Molluscum and eczema flare
Some kids get an eczema-like rash around the bumps called molluscum dermatitis. It can look like red, dry, itchy patches surrounding (not necessarily on top of) the bumps.
This does not automatically mean an allergy or that something “went wrong.” It usually means the skin is irritated and the immune system is noticing the virus. Treating the surrounding eczema and controlling itch can help prevent spreading from scratching.
What else could it be?
Several common skin issues can look like molluscum at first glance. If you are not sure, it is reasonable to check with your pediatrician.
- Warts: often rougher and do not usually have a central dimple.
- Impetigo: can form honey-colored crusts and spreads easily.
- Folliculitis: small pimples centered around hair follicles.
- Chickenpox (varicella): typically comes with many itchy blisters in different stages and often other symptoms.
- Insect bites: tend to be itchy, come and go, and lack the classic dimple.
Preventing spread
You do not need to put your child in a bubble. The goal is to reduce skin-to-skin transfer and keep bumps covered when practical.
At home
- Do not share towels, washcloths, or bath sponges. Give each child their own.
- Keep bumps covered with clothing or a bandage when they are in an area that gets touched a lot.
- Wash hands regularly, especially after applying lotion or touching the area.
- Short nails help reduce scratching damage and spread.
- Separate razors for older kids and adults. Do not share.
- Clean high-contact items like bath toys and sports pads when feasible.
School, daycare, and sports
- Attendance is usually fine. Most schools and daycares do not exclude children for molluscum. If your child feels well, they can usually go.
- Cover lesions for close-contact sports (wrestling, gymnastics) with a secure bandage and clothing when possible.
- Bring your own towel to swimming and sports.
- Avoid sharing helmets, pads, and uniforms when possible.
If your child’s program has specific rules for skin conditions (some sports do), check with the coach or school nurse.
When to call the pediatrician
Molluscum is usually straightforward, but you should check in with your child’s clinician if:
- The bumps are near the eyes or on the eyelids.
- The area becomes very red, warm, swollen, painful, or draining pus (possible secondary infection).
- Your child has significant eczema and bumps are spreading quickly.
- The diagnosis is uncertain (totally fair, many rashes can mimic each other).
- Bumps are in the genital area and you want an accurate diagnosis and guidance.
- Your child is immunocompromised or on immune-suppressing medication.
- The bumps are not improving over time and you want to discuss treatment options.
Get urgent care
- Rapidly spreading redness, especially with fever or your child seeming very ill.
- Eye involvement with significant irritation, swelling, or pain.
Common questions
Is molluscum the same as warts?
No. They can look similar, but molluscum is caused by a poxvirus and often has that central dimple. Warts are caused by HPV and usually have a rougher surface.
Is it dangerous?
In healthy children, it is typically not dangerous. The main issues are annoyance, itching, and spread.
Can my child go swimming?
Usually, yes. Use your own towel, avoid sharing equipment when possible, and cover bumps that are easy to cover. Transmission is generally thought to be more related to shared items and close contact than the water itself.
Will treating it make it go away faster?
Sometimes, especially if you can treat multiple lesions early and reduce scratching. But treatment is not guaranteed to be faster for every child, and some treatments can irritate the skin. This is a good “talk it through with your pediatrician” decision.
The bottom line
Molluscum contagiosum is a common childhood skin virus that causes small, pearly bumps, often with a tiny dimple in the center. It spreads through skin contact and shared items like towels. For many kids, the best plan is watchful waiting plus itch control and good hygiene, because it usually clears on its own over months.
If bumps are spreading quickly, causing stress, or getting infected, you are not overreacting by asking about treatment. You deserve a clear plan and some peace of mind.