Neonatal Hypoglycemia: Jitteriness, Feeding Trouble, and Glucose Checks
Sarah Mitchell
Sarah Mitchell is a Registered Pediatric Nurse and a mother of three who has spent over a decade helping families navigate the beautiful, chaotic early years of childhood. She combines evidence-based medical knowledge with real-world parenting experience to offer practical, compassionate advice. At Awesome Parent, Sarah's mission is to help exhausted parents find solutions, trust their instincts, and finally get some sleep.
Those first hours after birth can feel like a blur of snuggles, paperwork, and someone popping in every 20 minutes to “just check one thing.” If your baby is having blood sugar checks, it can sound scary fast.
Neonatal hypoglycemia is the medical name for low blood sugar in a newborn. It is common enough that most maternity units have clear screening routines, and most cases are short-lived and treatable. The goal is simple: identify the babies who need a little extra support during the transition from “fed through the placenta” to “feeding on the outside.”
These screenings matter because glucose is a key fuel for the newborn brain. Catching significant lows early helps prevent symptoms and keeps babies stable while feeding gets established.

Why babies can have low blood sugar after birth
In the womb, your baby receives a steady stream of glucose from you through the placenta. After delivery, that supply stops, and your newborn has to keep blood sugar stable by doing a few brand-new jobs:
- Use stored glycogen (a quick-access fuel reserve in the liver)
- Burn fat and make ketones (another type of fuel)
- Feed effectively to replace energy
It is normal for glucose levels to dip in the first couple of hours and then rise as feeding gets established. The tricky part is that some babies dip lower than is safe or do not bounce back quickly, especially if they have certain risk factors.
Which newborns are screened (risk factors)
Most hospitals do not poke every baby routinely. Care teams typically screen babies who are more likely to have significant or prolonged low blood sugar, including:
- Babies of parents with diabetes (type 1, type 2, or gestational diabetes)
- Large for gestational age (bigger than expected for weeks of pregnancy)
- Small for gestational age or growth restricted
- Preterm babies (often under 37 weeks)
- Late preterm (34 to 36 weeks), even if they look “basically full term”
- Babies under stress during labor or delivery (your team will tell you if this applies)
- Twins or multiples can be screened more often depending on size and gestational age
- Babies who are not feeding well or who show symptoms (more on those below)
A very common scenario is a baby born to a parent with gestational diabetes. These babies may produce extra insulin before birth. After delivery, insulin can still be “running high” for a bit, which can pull glucose down until things stabilize.

Signs parents might notice
Low blood sugar can be sneaky because many symptoms overlap with normal newborn behavior. Here are the clues that should get your nurse or pediatric team involved promptly:
- Jitteriness or tremors (shaking that looks more than just a startle)
- Poor feeding, weak latch, or falling asleep immediately at the breast or bottle every time
- Lethargy (hard to wake, “too sleepy,” not just milk-drunk sleepy)
- Low tone (feels floppy, not holding arms and legs with usual newborn flex)
- Temperature instability (especially low temperature)
- Color changes (pale or bluish) or breathing that seems off
- High-pitched cry or unusual irritability
More serious symptoms can include pauses in breathing, seizures, or significant difficulty staying awake. Thankfully, that is not the usual course, especially when screening is in place.
Jittery newborn or normal newborn wiggles?
Newborns are twitchy little creatures. Jitteriness can look dramatic, and it is not always hypoglycemia. A common bedside clue is that jitteriness may lessen or stop with gentle holding of the limb, while seizure-like movements typically do not. That said, it is not a perfect test. If you are seeing shaking plus poor feeding, unusual sleepiness, color change, or anything that worries you, call your nurse.
What glucose screening looks like
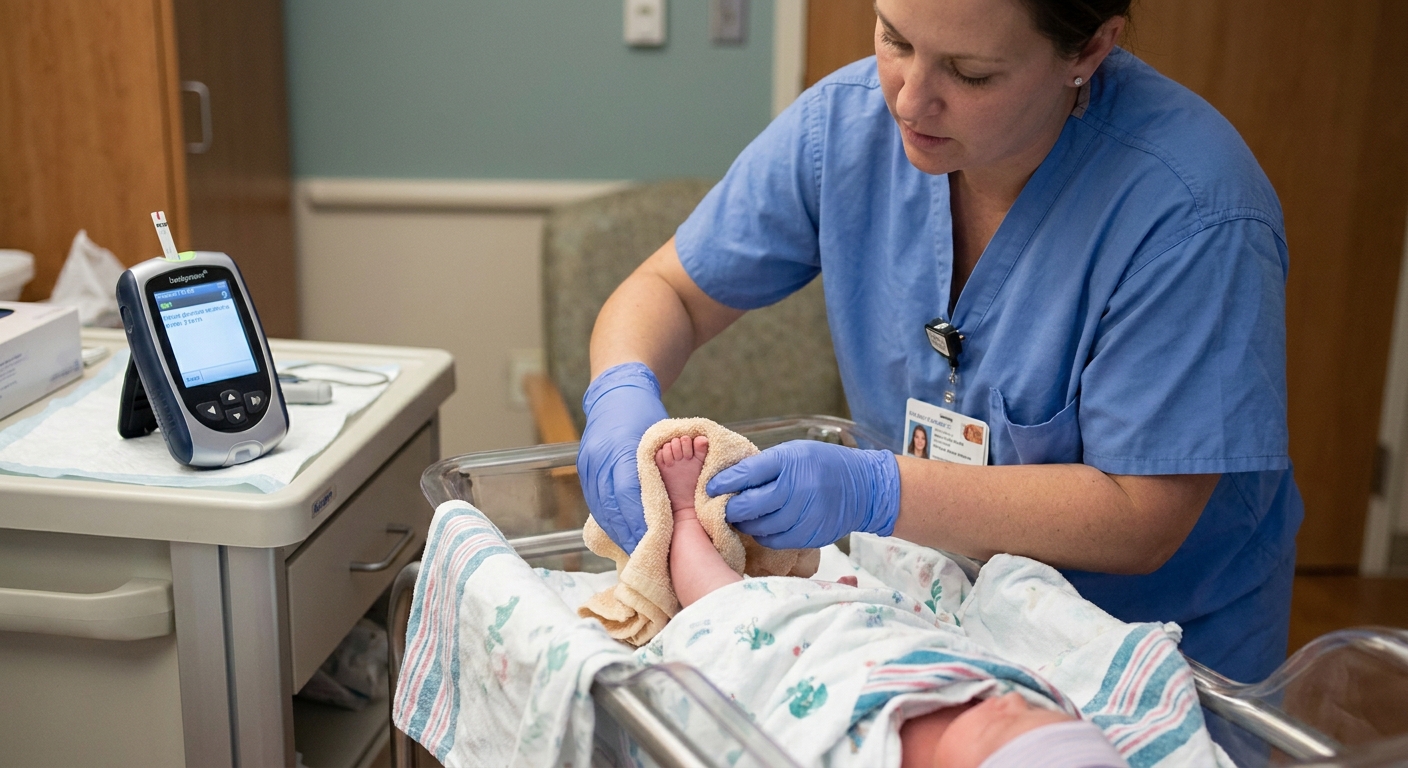
Most newborn glucose checks are done with a heel stick and a bedside meter (similar to what people with diabetes use). The team will usually:
- Check a first glucose within a set time after birth for at-risk babies (timing varies by hospital protocol)
- Recheck before feeds or at scheduled intervals until values are stable
- Confirm with a lab test if a reading is very low or does not match how your baby looks
A quick note on the numbers: bedside meters are helpful for screening, but they can be less accurate at very low ranges, and they may not match the lab’s plasma glucose exactly. That is why you will sometimes hear, “We are sending a confirmatory lab.”
If you are wondering, “How many checks are we talking?” It might be a handful over the first 12 to 24 hours. If numbers are stable and baby is feeding well, the pokes usually stop.
What counts as low
Here is the honest answer: treatment thresholds vary by hospital and by guideline, and they can also change based on hours of life and whether a baby has symptoms.
If you want a ballpark, many protocols treat or recheck more aggressively when glucose is under about 25 to 40 mg/dL in the first several hours, and aim for at least about 45 mg/dL once babies are a bit older and feeding is underway. Some units use different cutoffs. Ask your team two practical questions: “What number are you aiming for at this age?” and “What is the next step if we are below it?”
What happens if the number is low
The treatment plan depends on how low the glucose is, whether your baby has symptoms, and how they respond to feeding. In many cases, the first steps are straightforward and quick.
Step 1: Warmth and a good feed
Cold babies burn more glucose. Also, a low temperature can sometimes be a sign a baby is struggling (for example, with infection), so teams take it seriously. The focus is usually on:
- Skin-to-skin with you (it is powerful stuff)
- Keeping baby warm with a hat, swaddle, or warmer if needed
- Feeding support to improve latch or pacing
Step 2: Supplementation (when needed)
If a baby is too sleepy to feed well or the glucose is below the unit’s threshold, supplementation can be used to raise blood sugar and prevent repeat lows. Options may include:
- Expressed colostrum or breast milk
- Donor milk (available in some hospitals)
- Formula (often used because it is readily available and consistent)
This is usually paired with a recheck of glucose afterward to make sure it improved.
Step 3: Oral glucose gel
Many maternity units use oral dextrose gel, rubbed inside the baby’s cheek, along with feeding. It can be a great middle step that helps some babies avoid IV fluids and NICU transfer. Your team will explain if it is part of your hospital’s protocol.
Step 4: IV dextrose (and sometimes the NICU)
If glucose remains low despite feeds and gel, or if your baby has concerning symptoms, the team may recommend:
- IV dextrose (sugar water through a small IV)
- More frequent monitoring
- NICU or special care nursery for closer observation
This is not automatically a “something terrible is happening” move. It is often the fastest, safest way to stabilize glucose while your baby learns to feed well and regulate on their own.
If lows keep happening
Most newborn hypoglycemia is transitional and resolves within a day or two. If it is persistent, recurrent, severe, or requires higher amounts of IV glucose to keep levels safe, the team may look for an underlying cause. This can include things like infection, higher insulin levels (hyperinsulinism), hormone differences (like cortisol or growth hormone deficiency), or rarer metabolic conditions.
This evaluation is not meant to alarm you. It is the next sensible step when the typical “feed, warm, gel” pathway is not enough.
When to escalate right away
Whether you are still in the hospital or you have just gone home, trust your gut and escalate if your baby seems “off.” Call your nurse immediately in the hospital, or contact your pediatrician or seek urgent care if you are home and you notice:
- Repeated jitteriness, shaking, or rhythmic movements
- Hard to wake or unusually limp
- Refusing feeds or too sleepy to eat for multiple attempts
- Breathing trouble, color change, or persistent grunting
- Seizure-like activity (staring spells with lip smacking, repeated jerking, or body stiffening)
- Fewer wet diapers than expected plus poor intake
If your baby is difficult to arouse, has breathing problems, turns blue, or you suspect a seizure, treat it as an emergency and seek immediate care.
Normal dip vs true hypoglycemia
Here is the reassuring part: many newborns have a brief dip in blood sugar in the first hours as they transition, especially before milk volume increases. Most healthy term babies correct this with normal feeding, warmth, and time.
Care teams worry more when:
- The dip is significant (below your hospital’s treatment threshold)
- Baby has symptoms that match low glucose
- Numbers stay low across repeated checks
- There are strong risk factors like maternal diabetes, prematurity, or growth restriction
If your baby is being screened, that does not mean something is wrong. It usually means your team is being appropriately cautious with a baby who has higher odds of needing a little help.
How parents can help in the first 24 hours
You do not need to do this perfectly. You just need a few supportive basics.
- Prioritize early, frequent feeds: Many newborns do best feeding about every 2 to 3 hours, and sometimes more often. If your baby is very sleepy, your team may recommend waking for feeds.
- Use skin-to-skin: It supports warmth, feeding cues, and regulation.
- Ask for hands-on feeding help: Lactation consultants and nurses can spot small fixes that make a big difference.
- Track output: Wet and dirty diapers give clues about intake.
- Speak up about symptoms: If your baby seems unusually jittery or hard to wake, say so.

Common questions I hear at 3 AM
Will supplementation ruin breastfeeding?
In most cases, no. When supplementation is used thoughtfully for a medical reason, it can be a temporary bridge that keeps your baby safe and energized enough to feed better. Ask your team about protecting supply with hand expression or pumping if supplementation is needed.
Did I do something wrong?
No. Neonatal glucose regulation is a normal transition that some babies need extra support with, especially if they are early, small, large, or exposed to higher insulin levels during pregnancy.
How long does monitoring last?
Often 12 to 24 hours for at-risk babies, sometimes longer if values are borderline or baby is struggling to feed. Your team can tell you the exact stop criteria used on your unit.
Could low blood sugar cause long-term problems?
Severe, prolonged, or recurrent hypoglycemia, especially if not recognized, is associated with neurodevelopmental risk. That is exactly why hospitals screen higher-risk newborns and treat low numbers quickly. Most babies with transitional hypoglycemia who are monitored and treated promptly do very well. If your baby needed a NICU stay, IV glucose for more than a short period, or had repeated lows, ask what follow-up is recommended.
Bottom line
Newborn glucose screening can feel intense, but it is one of those behind-the-scenes safety nets designed for the early transition after birth. If your baby is jittery, too sleepy to eat, floppy, or just not acting like themselves, you are not overreacting by calling the nurse. You are being exactly the kind of parent your baby needs.
If you want, ask your care team two simple questions: “What number are you aiming for at this age?” and “What is the plan if the next check is still low?” Clear answers can make the whole process feel a lot less mysterious.