Newborn Screening (Heel Prick): What Hospitals Test For and What Abnormal Results Mean
Sarah Mitchell
Sarah Mitchell is a Registered Pediatric Nurse and a mother of three who has spent over a decade helping families navigate the beautiful, chaotic early years of childhood. She combines evidence-based medical knowledge with real-world parenting experience to offer practical, compassionate advice. At Awesome Parent, Sarah's mission is to help exhausted parents find solutions, trust their instincts, and finally get some sleep.
If you gave birth in a hospital or birth center, you probably remember it: a nurse warming up your baby’s tiny foot, a quick little poke, a few drops of blood on a card, and then… you are sent home with a newborn and about a million questions.
That heel-prick test is called newborn screening. It is one of the most important “quiet hero” tests we do in pediatrics, because it can catch rare but serious conditions before a baby looks sick.
And if you are here because you got a call about an “abnormal” result, take a breath with me. In my years as a pediatric triage nurse, I made a lot of these calls and answered a lot of panicked questions. Most abnormal screens are not a diagnosis. They are a signal that your baby needs a closer look.
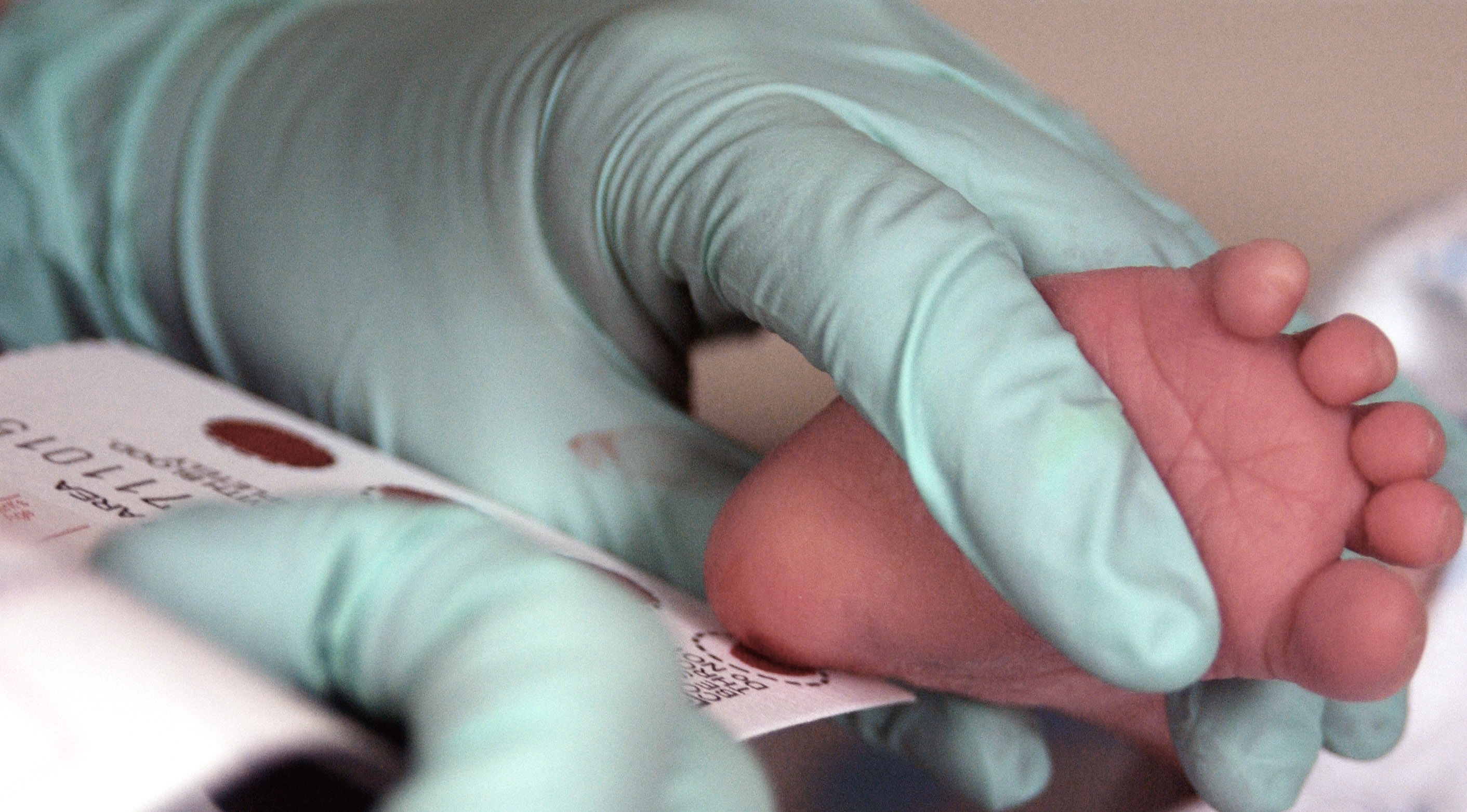
What it is (and is not)
Newborn screening is a set of tests done in the first days of life to look for certain metabolic, genetic, hormone, and blood conditions that can cause serious problems if they are not treated early.
Here is the key distinction that saves a lot of worry:
- Screening asks: “Is there a chance this condition is present?”
- Diagnostic testing answers: “Does your baby definitely have it?”
A screening test is designed to be extra sensitive. That means it is more likely to flag a possible issue, because we would rather recheck a healthy baby than miss a baby who truly needs treatment.
When it is done
Most hospitals collect the newborn screen at about 24 to 48 hours after birth. Some babies, especially those discharged early, may have it done closer to 24 hours or even earlier depending on local policy.
Timing matters because many of the markers we measure change quickly after birth as babies start feeding, their hormones shift, and their bodies adjust to life outside the womb.
One more important timing note: some regions routinely do two newborn screens as standard (for example, a first screen in the first days of life and a second screen in the following week or two). Your baby may be “due” for a repeat even if everything is normal. Your local program sets the schedule.
Why a repeat is needed
Your baby might need a repeat heel prick if:
- The first sample was collected too early (before enough feeding or metabolic changes occurred).
- The blood spot card did not have enough blood or was not processed ideally.
- Your baby was born premature or had a NICU stay, which can affect results and schedules.
- Your baby received a blood transfusion. This most directly affects screening for hemoglobin and blood disorders (like sickle cell), and it can also influence a few other markers. Many programs try to collect a sample before transfusion when possible, and may repeat after.
If your pediatrician recommends a repeat, it is usually about getting the most accurate information possible, not because anyone assumes something is wrong.
What is screened
The exact panel varies a lot by state or country. In the U.S., many states screen for a few dozen to 50+ conditions, and some places include tests that others do not. If you want the most accurate list, your state or country’s newborn screening program site is the best source.
That said, most programs screen for a similar set of categories. Here are the ones you will most commonly hear about, explained in plain language.
1) Metabolic disorders
These conditions affect how a baby breaks down proteins, fats, or sugars. Without treatment, certain substances can build up and become harmful.
Examples you may see on a report:
- PKU (phenylketonuria): difficulty processing a specific amino acid. Treatment is typically a special diet started early.
- MCAD deficiency and other fatty-acid oxidation disorders: trouble using fat for energy, especially during long stretches without feeding. Treatment often focuses on avoiding prolonged fasting and having a sick-day plan.
- Galactosemia: difficulty processing a sugar found in milk. Treatment involves changing feeds quickly if confirmed.
2) Endocrine disorders
Hormones help regulate growth, metabolism, and stress responses. Two common screening targets:
- Congenital hypothyroidism: low thyroid hormone. Early treatment supports normal brain development.
- Congenital adrenal hyperplasia (CAH): an adrenal hormone issue that can, in some forms, cause dangerous salt imbalance. Early detection can be lifesaving.
3) Hemoglobin and blood disorders
These involve the red blood cell proteins that carry oxygen.
- Sickle cell disease and related conditions can be identified early so babies can start protective care (like certain medications and careful infection monitoring) before problems show up.
4) Cystic fibrosis
Many screening programs include cystic fibrosis (CF). Screening often begins with an enzyme level (IRT) and may include genetic markers depending on the program.
If CF screening is abnormal, next steps depend on the state or regional algorithm. Many babies go on to a sweat test, while some programs use repeat IRT and or additional DNA testing before scheduling a sweat test. An abnormal screen does not automatically mean CF.
5) SCID
SCID (severe combined immunodeficiency) is a rare immune system condition. Babies may look well at birth, but can become severely ill from infections. Screening allows precautions and treatment planning early. Not all jurisdictions include SCID, so your local panel matters.
6) Hearing screen
Most hospitals also do a newborn hearing screen before discharge. A “refer” result often means baby needs a repeat test, not that permanent hearing loss is confirmed.
7) Heart screen
Many hospitals also perform screening for critical congenital heart disease (CCHD) using a little sensor on baby’s hand and foot to check oxygen levels. Not every country or region includes this in the newborn screening bundle, but it is common in many places.
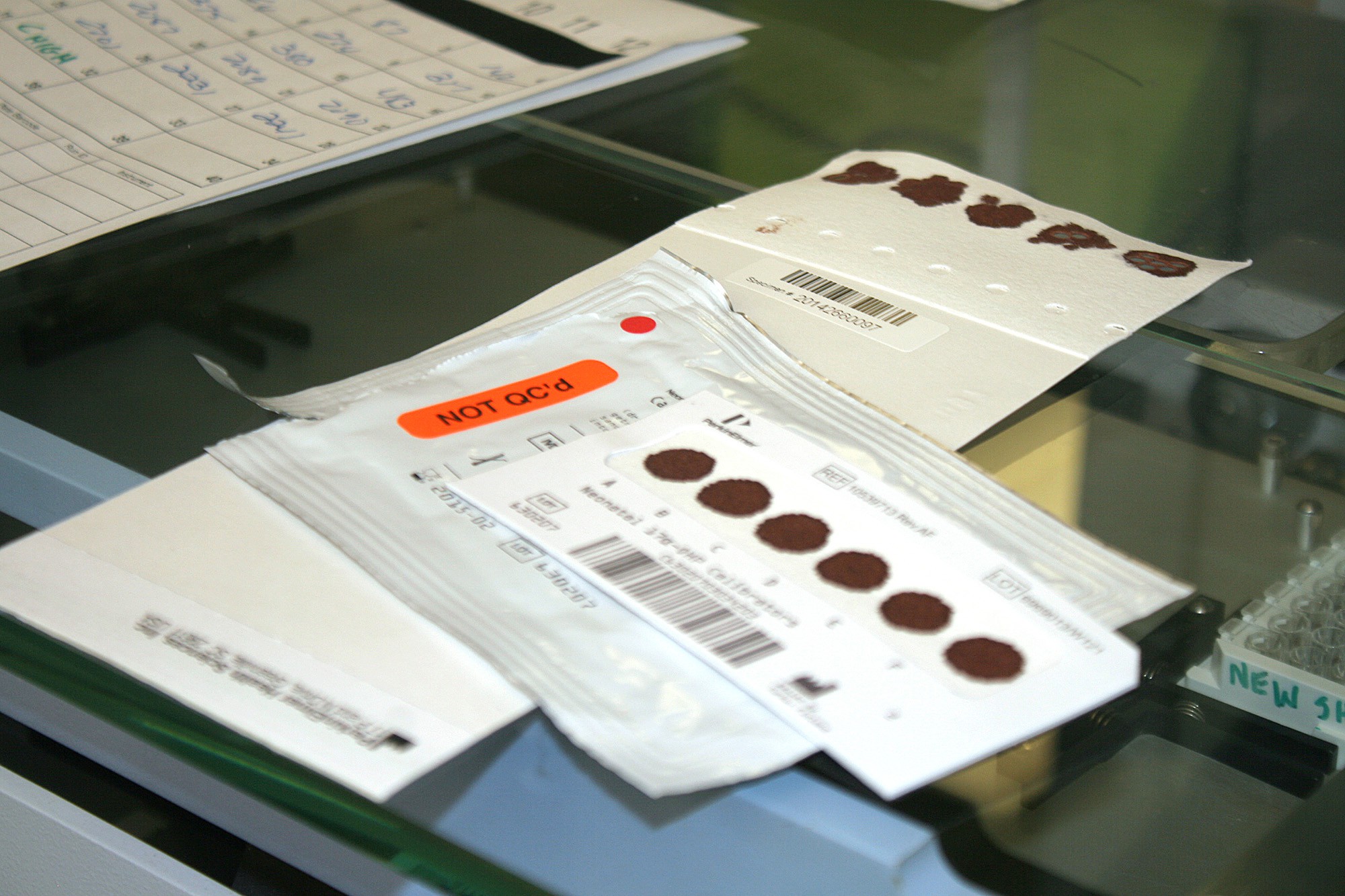
What “abnormal” means
When parents hear “abnormal,” they often hear “your baby is sick.” In newborn screening, it more often means:
- The result was outside the expected range for a screening test.
- Your baby needs follow-up to sort out whether this is a true condition or a false positive.
Words you might hear
- Borderline or inconclusive: not clearly normal, not clearly high risk. Often this means a repeat screen or a targeted blood test.
- Unsatisfactory specimen or QNS (quantity not sufficient): the lab could not run the test reliably (not enough blood, a smudged spot, sample issue, or timing). This is not the same as an abnormal result, but it still needs a repeat.
Why screens flag
- Sample collected early (especially before 24 hours).
- Prematurity or low birth weight.
- NICU factors: IV nutrition, illness, medications, oxygen support, or stress on the body.
- Feeding patterns: dehydration or low intake early on can shift some values.
- Normal newborn physiology: hormone levels and metabolism are changing rapidly.
- Laboratory cutoffs are intentionally set to catch as many true cases as possible, even if it means more rechecks.
As a nurse, I used to tell families: newborn screening is built to be a wide net. A wide net catches the fish we need to find. It also catches some seaweed.
Some abnormal results require quick follow-up, so it is important to take the call seriously even while you try not to spiral.
False positives and negatives
A false positive means the screen suggests a condition, but confirmatory testing shows the baby does not actually have it.
False positives happen because screening tests are optimized to avoid false negatives. In other words, the system leans toward “better safe than sorry.”
Some screens are more likely to have false positives in:
- Premature babies
- Babies in the NICU
- Babies screened early
False negatives
Much less common, but possible, is a false negative, where the screen looks normal but a baby still has a condition. This is one reason pediatricians still take symptoms seriously even if the newborn screen was “normal.” Screening is powerful, but it is not perfect.
What happens next
Follow-up depends on which part of the screen was abnormal. Your pediatrician may:
- Order a repeat newborn screen (another heel prick).
- Order blood tests that measure the specific chemical or hormone more directly.
- Order urine testing for certain metabolic concerns.
- Refer you to a metabolic specialist, geneticist, endocrinologist, pulmonologist, or hematologist.
- Schedule a diagnostic test such as a sweat test for cystic fibrosis, depending on your local algorithm.
A quick safety note about feeding changes
It can be tempting to change formula, stop breastfeeding, or wake baby constantly after a call about a metabolic screen. Please do not make major feeding changes unless your clinician specifically tells you to. A few conditions have very specific precautions, but the safest plan is the one tailored to the exact marker that was flagged.
Questions to ask
- Which condition or marker did the screen flag, and was it “borderline” or “high concern”?
- Is this an abnormal result, or an unsatisfactory specimen (QNS) that just needs a repeat?
- Does my baby need testing today, or is this a routine repeat?
- Is there anything I should do differently right now?
- What symptoms should make me seek urgent care while we wait?
- When will we get results, and who will call?

How results are shared
In many places, the blood spot card goes to a state or regional lab, and results are sent to your baby’s hospital and or pediatrician. Families are often contacted only if something needs follow-up.
This is also why you might hear later than expected. Sometimes it is just the normal pace of processing, shipping, weekends, and reporting pathways. If you are unsure whether screening was done or you never saw results, it is completely reasonable to ask your pediatrician to confirm.
While you wait
Waiting is often the hardest part. Your brain fills in blanks with worst-case scenarios, especially when you are postpartum, sleep-deprived, and already running on adrenaline.
Grounding reminders
- An abnormal screen is not a diagnosis. It is a prompt to double-check.
- Many, and often most, babies with abnormal screens end up being fine. Follow-up urgency varies by condition, so let your clinician guide the timeline.
- You did not cause this. Newborn screening flags biology, not parenting.
Practical ideas
- Pick one point person to call the clinic for updates, so you are not both spiraling and dialing.
- Write down feeds and diapers. It gives you something concrete and helpful to share if asked.
- Limit late-night searching. If you must Google, stick to reputable sources and stop after 10 minutes.
- Ask for the exact name of what was flagged. “Metabolic screen abnormal” is vague. A specific marker is easier to discuss.
- Let someone help with food, laundry, or older kids. Stress is real, and support matters.
When to seek urgent care
Most families waiting on a repeat screen do not need emergency care. But you should contact your pediatrician right away or seek urgent evaluation if your newborn has:
- Poor feeding or refuses multiple feeds in a row
- Vomiting repeatedly
- Unusual sleepiness that makes it hard to wake for feeds
- Breathing difficulty, bluish color around lips, or persistent fast breathing
- Fever: a rectal temperature of 100.4°F (38°C) or higher in a baby under 3 months is typically treated as urgent. Follow your local guidance and your clinician’s instructions.
- Signs of dehydration: very few wet diapers, very dry mouth, sunken soft spot
If your clinic told you a specific screen requires urgent same-day testing, follow that plan even if your baby looks well. Some conditions are safest to address early, before symptoms begin.
If a condition is confirmed
If confirmatory tests show your baby truly has a screened condition, your care team will move quickly into “next steps” mode. That often includes:
- A clear treatment plan
- Education on what to watch for
- Specialty follow-up
- Support resources, including nutrition support for diet-based conditions
I know that is not the outcome any parent hopes for. But I also want you to know this: many of the conditions found on newborn screening have dramatically better outcomes precisely because we catch them early. Early detection is the whole point.
Quick FAQ
Does the heel prick hurt?
It is briefly uncomfortable, yes. Hospitals often use comfort measures like swaddling, skin-to-skin, breastfeeding during the poke, or a small amount of sugar solution depending on policy. The discomfort is short, and the benefit is big.
How long does it take to get results?
It varies by location, but commonly several days to a couple of weeks. Many parents are only contacted if something needs follow-up. If you are worried results were missed, call your pediatrician and ask them to check the state or regional portal or lab report.
We were discharged early. Will that affect it?
Possibly. Early collection is one reason a repeat may be recommended. It is common and usually straightforward.
Can I decline newborn screening?
Some places allow refusal for specific reasons, but rules vary. If you are considering declining, talk with your baby’s clinician about what would be missed and what alternatives exist. Many of these conditions are not visible at birth.
Where can I read more from a reliable source?
If your publication format allows links, good starting points include the CDC’s newborn screening overview, your state or country’s newborn screening program page, the Cystic Fibrosis Foundation (for CF), and reputable children’s hospitals.
Bottom line
Newborn screening is a routine heel-prick blood test designed to catch rare but serious conditions early, often before a baby shows symptoms. The panel and timing vary by location, and some places routinely do two screens.
Abnormal results are common enough that pediatric clinics have well-worn follow-up pathways, and many flagged screens do not end up being a diagnosis. The most important thing is to get the specifics and follow the next step your pediatrician recommends.
And if you are reading this at 3 AM with one hand on your phone and the other on your baby’s back, I want you to hear this clearly: you are doing exactly what a good parent does. One step at a time.