Nipple Thrush While Breastfeeding
Sarah Mitchell
Sarah Mitchell is a Registered Pediatric Nurse and a mother of three who has spent over a decade helping families navigate the beautiful, chaotic early years of childhood. She combines evidence-based medical knowledge with real-world parenting experience to offer practical, compassionate advice. At Awesome Parent, Sarah's mission is to help exhausted parents find solutions, trust their instincts, and finally get some sleep.
If breastfeeding suddenly went from “a little tender at first latch” to “why does it feel like my nipples are on fire,” you are not alone. One possible culprit is nipple thrush, a yeast overgrowth (often Candida species) that can irritate the nipples and, less commonly, cause radiating breast pain. The tricky part is that thrush can look and feel a lot like other common problems, so it can drag on if it is mislabeled or missed.
As a pediatric nurse and a mom who has done the 3 AM Googling with a baby attached to me, I want you to know two things: you are not doing anything wrong, and help is available. Nipple pain is real, and it deserves a real assessment. This article is for education, not a diagnosis. If symptoms are intense, persistent, or worsening, loop in your clinician and an IBCLC if you can.

What it feels like
Nipple thrush can show up with or without obvious changes on the skin. The pain often feels out of proportion to what you see. That said, these symptoms are not exclusive to yeast, so it is worth considering other look-alikes too.
Common symptoms in the breastfeeding parent
- Burning, stinging, or itching nipple pain, often described as “raw” or “on fire.”
- Pain that continues after feeds or between feeds, not just at latch-on.
- Shiny, smooth, or flaky nipples. Some parents notice peeling skin.
- Pink or red nipples or areola, sometimes with a rashy look.
- Cracked nipples that will not heal despite a decent latch and good care.
- Radiating or shooting breast pain during or after feeds (reported by some parents, but it is not specific to yeast and can have other causes).
Thrush is more likely if you or baby recently had antibiotics, if you have diabetes, if you are dealing with nipple damage, or if you have a history of yeast infections.
Thrush vs. latch pain
Many breastfeeding problems cause nipple pain, so it helps to look for patterns.
More suggestive of latch or positioning
- Pain is worst only at the start of feeding and improves as baby settles.
- Nipple looks lipstick-shaped or pinched after feeds.
- You see obvious issues like clicking, slipping, or shallow latch.
More suggestive of thrush
- Pain is burning and persists during and after feeds.
- Nipples look shiny, flaky, or unusually pink.
- Symptoms started after antibiotics or after baby had mouth sores or a stubborn diaper rash.
Other common look-alikes
Vasospasm (Raynaud’s of the nipple): If the nipple turns white or blue after feeding and then throbs as color returns, that points more toward vasospasm than thrush.
Nipple dermatitis or eczema: This can be from sensitive skin, a reaction to lanolin or other nipple creams, breast pads, detergents, or even friction. It can look red, scaly, itchy, or weepy. Antifungals often do not help much if dermatitis is the real cause.
Bacterial infection: Sometimes persistent nipple damage, crusting, or worsening pain is related to bacteria (such as staph), especially if there are cracks that are not healing.
If you have severe pain, open sores, fever, or a hot red wedge-shaped area on the breast, get evaluated promptly. Those can signal mastitis, an abscess, or another issue that needs specific treatment.
Baby signs
Nipple thrush often travels with baby oral thrush, but not always. The reason we talk about baby so much in a “parent nipple pain” article is simple: if only one of you is treated, yeast can bounce back and forth.
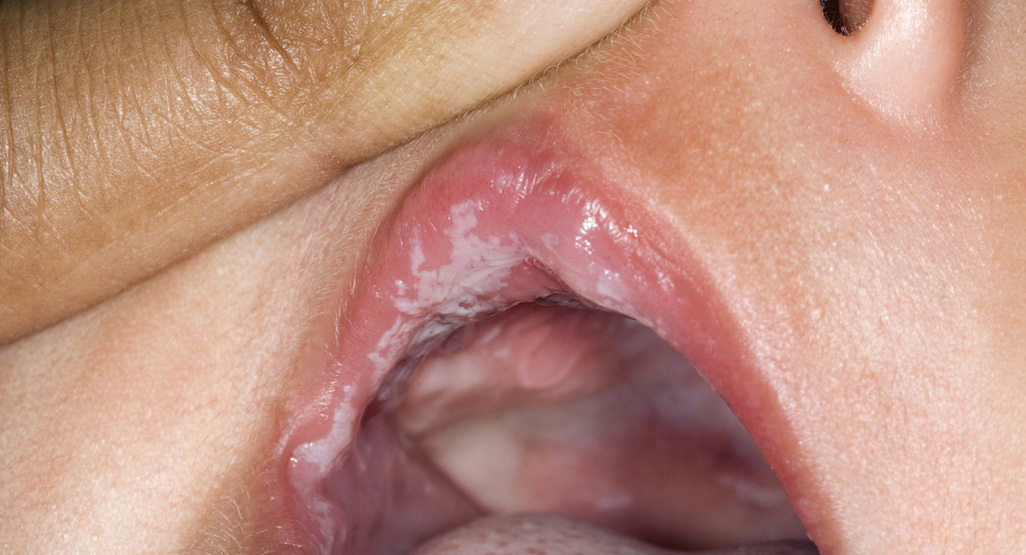
Possible signs of oral thrush in babies
- White patches on the tongue, inner cheeks, or gums that do not wipe away easily.
- Fussiness at the breast or bottle or popping on and off.
- Diaper rash that is beefy red, persistent, or has satellite spots.
Some babies have very subtle symptoms. In real life, I have seen plenty of cases where the baby’s mouth looks normal but the breastfeeding parent has classic thrush-type pain, or vice versa.
Diagnosis
Most of the time, diagnosis is based on symptoms and exam. Cultures are not always necessary and can be tricky, but sometimes your clinician may swab the nipple or baby’s mouth if the picture is unclear or symptoms keep returning.
It is also worth saying out loud: in lactation medicine, yeast can be over-assigned because symptoms overlap so much with dermatitis, vasospasm, and bacterial causes. Many families do best with a two-part approach:
- Latch support to reduce trauma that keeps skin irritated
- Targeted treatment when symptoms fit, with reassessment if things are not improving
What to do first
- Get a latch check (IBCLC or trained clinician), especially if pain started with a new latch change, pumping change, or visible nipple damage.
- Call your clinician if burning pain persists beyond 48 to 72 hours, if pain is severe, or if baby has signs of thrush or a yeast diaper rash.
- Avoid DIY “kitchen sink” treatments. Gentian violet and other remedies can irritate tissue or be unsafe if misused. If you are considering any non-prescription approach, ask your clinician first.
Treatment
Treatment plans vary by region and clinician, but the goal is consistent: reduce yeast on the nipple and in baby’s mouth (when involved), and prevent the frustrating ping-pong cycle.
For the breastfeeding parent
- Topical antifungal cream is often first-line. Common choices include miconazole or clotrimazole applied to the nipple and areola after feeds.
- Do I wipe it off before nursing? This is a very common worry. In many cases, you can apply a thin layer after feeds and gently wipe off any visible excess before the next feed if there is still residue. Follow your prescriber’s directions and local guidance, especially if baby is premature or medically fragile.
- All-Purpose Nipple Ointment (APNO) may be prescribed in some practices, especially when there is nipple damage and mixed irritation. APNO typically combines an antifungal plus other components (often antibacterial and anti-inflammatory). It can be helpful for some families, but it is prescription-based and not one-size-fits-all.
- Oral antifungal medication (like fluconazole) may be used for stubborn cases or persistent radiating pain, depending on your medical history and local guidance.
- Address nipple trauma: if latch is shallow or pumping settings are too strong, healing will be slow even with the right medication.
Important: Use medications exactly as prescribed. Stopping when you feel better is one of the fastest ways thrush-type symptoms come right back, usually on a Friday night.
For baby (when oral thrush is suspected or confirmed)
- Oral antifungal medication (often nystatin suspension) may be prescribed.
- Miconazole oral gel is used in some locations, but it is not appropriate for all infants. In many guidelines it is avoided in young babies due to choking risk (often under 4 months, depending on local recommendations). Only use it if prescribed and you are instructed exactly how to apply it safely.
- Diaper yeast rash treatment may be recommended at the same time if present.
Even if baby has minimal symptoms, many clinicians treat both parent and baby together to reduce reinfection. Ask your pediatrician what they recommend for your specific situation.
Can I keep breastfeeding?
In most cases, yes. Continuing to breastfeed is usually safe and can help maintain supply while you treat. If pain is intense, ask about temporary strategies like short, frequent feeds, pumping breaks, or a latch check to reduce friction while things heal.
How fast should it improve?
Many parents notice at least some improvement within a few days of effective treatment, but the timeline varies. If you are not improving after several days, or if things keep coming back, you may need reassessment for dermatitis, vasospasm, bacterial infection, or a different treatment plan.
Hygiene that helps
You do not need to boil everything you own for weeks, but you do want to reduce yeast buildup during treatment.
Daily habits
- Wash hands well after diaper changes and before applying any nipple cream.
- Change breast pads often and skip pads that trap moisture.
- Keep nipples dry between feeds. Yeast loves warm, damp environments.
- Use a clean bra daily. If you leak a lot, consider changing midday.
- Wash bras, burp cloths, and cloth nursing pads in hot water (if the fabric allows) and dry thoroughly to help kill lingering yeast on fabrics.
Pump and bottle cleanup
- Clean pump parts thoroughly after each use and allow them to fully dry.
- Follow manufacturer instructions for sanitizing pump parts, bottle nipples, and pacifiers. Many families choose daily sanitizing during active treatment.
- Replace pacifiers and bottle nipples if thrush keeps recurring quickly despite good treatment and cleaning. Replacement is not always required, but it can help in stubborn cases.
Preventing reinfection
That “we treated it and it came right back” experience is often reinfection or an incorrect initial diagnosis, not a failure on your part.
Common reasons it returns
- Parent treated but baby was not, or vice versa.
- Treatment stopped too early.
- Pacifiers, bottle nipples, pump parts, bras, or pads were reintroducing yeast.
- Ongoing nipple trauma from latch issues kept skin irritated and vulnerable.
- The real cause was dermatitis, vasospasm, or bacterial infection rather than yeast.
Simple checklist
- Make a plan to treat both parent and baby if your clinician recommends it.
- Complete the full course of medication.
- Get a latch and positioning check from an IBCLC or trained clinician.
- Keep nipples as clean and dry as possible between feeds.
When to call
Please reach out if any of the following are true:
- You have fever, feel flu-like, or have a painful red area on the breast.
- Pain is severe enough that you are considering stopping feeds.
- Symptoms are not improving after several days of treatment.
- You have recurrent symptoms, especially if you have risk factors like diabetes or frequent antibiotics.
- Baby is not feeding well, has fewer wet diapers, or seems dehydrated.
If you are unsure who to call first: baby symptoms go to the pediatrician, and nipple or breast symptoms go to your OB-GYN, midwife, family doctor, or a breastfeeding medicine clinician. Many families benefit from looping in a lactation consultant at the same time.
Comfort tips
Treatment tackles the cause, but you still have to get through the next few feeds. These can help while medication kicks in:
- Start on the less painful side first if one side is worse.
- Try different positions to change pressure points on the nipple.
- Air-dry nipples after feeds for a few minutes.
- Ask about safe pain relief options for you if you need them.
You deserve care that takes your pain seriously. If someone tells you “breastfeeding just hurts” and stops there, get a second opinion.
Bottom line
Thrush-type nipple pain can feel intense and confusing because it often masquerades as latch pain, dermatitis, vasospasm, or bacterial irritation. The winning combo is usually: getting eyes on latch, using the right medication when yeast is likely, treating baby when indicated, and cleaning the items and fabrics that stay warm and damp so symptoms cannot keep staging a comeback.
If you are in the thick of it, take a breath. This is fixable. And you do not have to white-knuckle your way through every feed to prove you are a good parent.