Pediatric Blepharitis: Crusty Eyelashes That Keep Coming Back
Sarah Mitchell
Sarah Mitchell is a Registered Pediatric Nurse and a mother of three who has spent over a decade helping families navigate the beautiful, chaotic early years of childhood. She combines evidence-based medical knowledge with real-world parenting experience to offer practical, compassionate advice. At Awesome Parent, Sarah's mission is to help exhausted parents find solutions, trust their instincts, and finally get some sleep.
If you are wiping yellowish crust off your child’s eyelashes again and again, and it never quite turns into full-blown “pinkeye,” you are not alone. In pediatric triage, this is one of those sneaky problems that keeps families stuck in a cycle: irritated eyes, a little redness, messy lashes, then a temporary improvement, then it comes right back.
That pattern is often blepharitis, which is inflammation along the eyelid margins. It is not usually dangerous, but it is stubborn. The goal is less about a one-time cure and more about a simple maintenance routine that keeps symptoms under control.
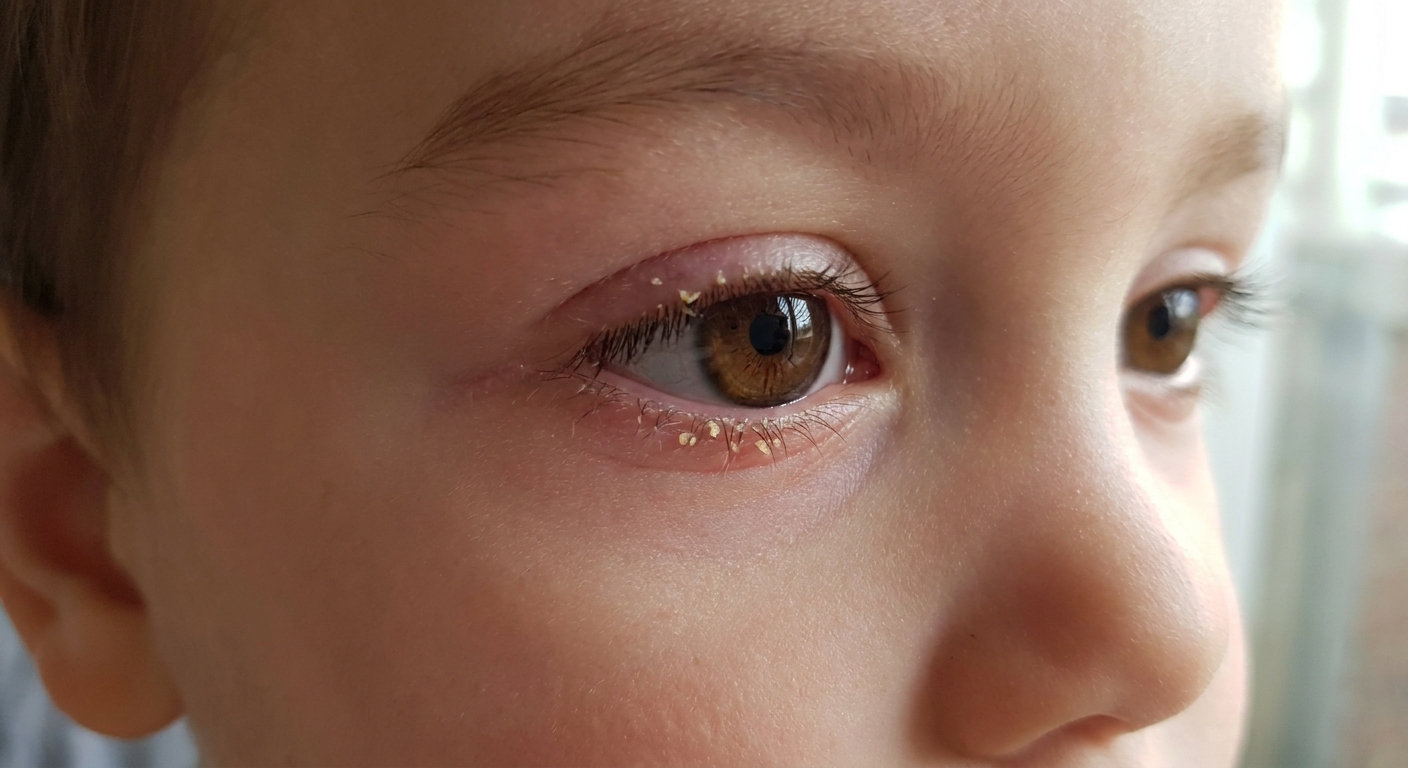
What it looks like in kids
Blepharitis is inflammation where the eyelashes grow. In children, it can be related to skin oil gland blockage, normal skin bacteria overgrowing at the lid edge, dandruff-type skin conditions, or irritation from rubbing and allergies.
Common symptoms
- Crusty or flaky eyelashes, especially after sleep
- Redness along the lid margin (the lash line), though the white of the eye can look irritated too
- Itchy, gritty, “sand in the eye” feeling
- Watery eyes or mild stringy discharge
- Burning or stinging with blinking
- Frequent eye rubbing
- Recurrent episodes that improve then return
Some kids also get recurrent styes because the same glands that get inflamed in blepharitis can clog and swell.
Blepharitis vs pinkeye
Parents are usually told: red eye equals pinkeye. But blepharitis often behaves differently than typical conjunctivitis. Symptoms can overlap, and blepharitis can also coexist with conjunctivitis, so sometimes an exam is the only way to be sure.
How it tends to differ
- Blepharitis: crusting and flaking at the lash line, chronic or recurring, often worse in the morning, irritation more than dramatic redness.
- Viral conjunctivitis: “pinkeye” look with watery discharge, often starts in one eye then spreads, commonly comes with a cold. Often contagious.
- Bacterial conjunctivitis: thicker discharge that reappears quickly after wiping, eyelids can stick shut, more goopy throughout the day. (Not a perfect rule, but a common pattern.)
- Allergic conjunctivitis: intense itching, watery eyes, often both eyes, may come with sneezing or seasonal symptoms.
Here is a practical clue: blepharitis is often most obvious at the lid margin. Conjunctivitis is primarily inflammation of the conjunctiva, the thin tissue over the white of the eye and inside the eyelids.

Blepharitis vs stye vs chalazion
These often get lumped together because they can happen together.
- Blepharitis: diffuse irritation and crusting along the lash line.
- Stye (hordeolum): a tender, red bump near the lash line. It can look like a pimple and is often painful.
- Chalazion: a firmer, usually less painful lump in the eyelid from a blocked oil gland. It can linger for weeks.
If your child keeps getting styes or chalazia, it is worth treating the underlying blepharitis, not just the bump of the week.
At-home treatment that helps
Blepharitis care is refreshingly low-tech. The mainstays are warm compresses and lid hygiene. If you only do one thing, start with warmth. Warmth loosens crust, softens thickened oils in the lid glands, and makes cleaning gentler.
Step 1: Warm compress
- Use a clean washcloth soaked in warm (not hot) water.
- Hold it over the closed eyelids for 5 to 10 minutes.
- Re-warm as needed so it stays comfortably warm.
- Aim for once or twice daily during flares, then taper to a few times per week for maintenance if symptoms return easily.
Step 2: Gentle lid cleaning
After the warm compress, gently clean the lash line to remove loosened crust and debris.
- Wash your hands first.
- Use a clean, damp cotton pad or soft washcloth.
- Wipe along the base of the eyelashes with the eye closed.
- Use a fresh pad or a clean section of cloth for each eye.
- Do not share washcloths or towels, and wash cloths after use.
What to use for lid cleansing
Many families do well with plain warm water. Some clinicians recommend diluted baby shampoo, but it can sting and irritate sensitive eyes. Over-the-counter eyelid cleansing wipes or foams can be convenient, especially for older kids, but you do not need anything fancy if warm water works.
Avoid essential oils or tea tree oil products around children’s eyes unless a clinician specifically recommends them. They can irritate the delicate eyelid skin, and dosing and safety are not straightforward in kids.
Step 3: Supportive comfort
- Artificial tears can help the gritty feeling, especially if screens or allergies worsen symptoms. Use preservative-free drops if you are using them often.
- Discourage rubbing as much as you can. Rubbing makes inflammation worse and spreads germs.
- If your child has dandruff or eczema, addressing skin flares can reduce eyelid irritation too.
My realistic parent note: for toddlers, do the warm compress while they watch a short show or listen to a story. For school-age kids, let them hold the cloth themselves while you supervise the temperature. Consistency matters more than perfection.
What not to do
- Do not use leftover prescription eye drops (especially steroid drops) from an old episode.
- Do not scrape crust aggressively. Let the warm compress do the work.
- Do not use hot compresses. Warm and comfortable is the goal.
Do kids need antibiotic drops?
Sometimes, but not always. Classic conjunctivitis antibiotics target infection in the eye, but blepharitis is primarily a lid-margin inflammation and gland issue. Many children improve with warm compresses and lid hygiene alone.
Your pediatrician or eye clinician might recommend:
- Antibiotic ointment applied to the lid margin for certain cases, especially if there is significant crusting and suspected bacterial overgrowth. Ointment is often preferred because it stays on the lid edge longer than drops.
- Treatment for associated conditions like allergies or eczema.
- In selected older kids and teens with more severe meibomian gland dysfunction or rosacea-spectrum disease, an eye clinician may consider additional therapies. This is not typical for toddlers and preschoolers.
Please avoid using leftover prescription eye drops from an old episode. The wrong medication can irritate the eye or miss the real problem.
When to call the doctor
Blepharitis is usually manageable at home, but some symptoms should move you from “routine care” to “get evaluated.”
Call promptly if your child has
- Eye pain that is more than mild irritation
- Light sensitivity (photophobia)
- Vision changes, blurry vision, or your child says they cannot see well
- Significant swelling of the eyelid or redness spreading around the eye
- Thick discharge with worsening redness (could be bacterial conjunctivitis)
- Contact lens use and any redness or pain (higher-risk situation)
- No improvement after 1 to 2 weeks of consistent warm compresses and lid hygiene
Seek urgent care or emergency evaluation if you notice
- Severe photophobia or the eye cannot comfortably stay open
- Severe pain
- New cloudy spot on the cornea (the clear front surface of the eye)
- Suspected corneal injury (scratch, foreign body, chemical exposure)
- Protruding eyeball, worsening swelling, or fever with eyelid redness (concern for deeper infection)
These red flags matter because blepharitis can sometimes irritate the cornea, especially if inflammation is significant or if a child is rubbing constantly.
Keeping it from coming back
Blepharitis tends to be chronic and recurring. That sounds discouraging, but it also means you are not failing when it reappears. You are managing a condition that behaves like dandruff or eczema: it flares, then settles.
Simple prevention habits
- Continue warm compresses a few times per week if your child flares often.
- Clean the lid margins gently during high-pollen seasons or when symptoms start to creep back.
- Wash hands often and keep nails trimmed to reduce rubbing damage.
- Replace eye makeup if your teen uses it and symptoms are recurring.
- Address allergies if itching is a big driver of rubbing.
How long does it last?
With consistent home care, many kids improve noticeably within one to two weeks. Recurrence is common, and some children do best with ongoing, low-effort maintenance even after things look better.
When an eye referral helps
If it is not improving, or if styes and chalazia keep happening, an eye referral is worth it. Your clinician may look for drivers like meibomian gland dysfunction, ocular allergy, atopic dermatitis, or, less commonly, Demodex. Identifying the “why” can change the plan.
FAQ
Is blepharitis contagious?
Blepharitis itself is usually not considered highly contagious like viral conjunctivitis. That said, kids touch their faces constantly, so good hand hygiene is still smart, especially if there is discharge or a concurrent infection. Avoid sharing towels and washcloths.
Can my child go to school or daycare?
Most children with blepharitis can attend as long as they feel well and can participate. Schools often exclude for contagious conjunctivitis with significant discharge, so if you are unsure whether it is conjunctivitis, check with your clinician.
Is it safe to use warm compresses on toddlers?
Yes, as long as the cloth is warm, not hot, and you supervise the whole time. Test it on the inside of your wrist first.
What if only one eye is affected?
Blepharitis can be worse on one side, especially if your child rubs one eye more. Still, watch for signs of a stye, nasolacrimal duct obstruction in younger babies (often more chronic tearing and discharge than lash-line scale), or infectious conjunctivitis if redness and discharge ramp up quickly.
The bottom line
If your child has chronic crusty lashes and recurring eyelid irritation that does not quite match the typical pinkeye story, blepharitis is a strong possibility. The good news is that most cases respond well to a steady routine of warm compresses and gentle lid hygiene. The most important thing is knowing the red flags, especially light sensitivity, significant pain, and vision changes, which deserve prompt evaluation.
If you are in the bleary-eyed “why is this happening again?” stage, I see you. This is one of those parenting problems that often gets better when you stop chasing a quick fix and switch to a simple, repeatable plan.