Periorbital Cellulitis in Children: When a Swollen Eyelid Is More Than Pinkeye
Sarah Mitchell
Sarah Mitchell is a Registered Pediatric Nurse and a mother of three who has spent over a decade helping families navigate the beautiful, chaotic early years of childhood. She combines evidence-based medical knowledge with real-world parenting experience to offer practical, compassionate advice. At Awesome Parent, Sarah's mission is to help exhausted parents find solutions, trust their instincts, and finally get some sleep.
If your child wakes up with a puffy, red eyelid, it’s easy to assume it’s pinkeye, a bug bite, or just a rough night of sleep. Sometimes it is. But when the eyelid itself is red, swollen, and tender, especially with fever or a child who looks unwell, we start thinking about periorbital cellulitis, also called preseptal cellulitis.
This is one of those parenting moments where you don’t need to panic, but you do need to pay attention. Most kids do very well with the right antibiotics. The key is recognizing when it’s not a simple eye irritation and when you need same-day care.
Quick note: This article is for education, not a diagnosis. If you’re worried, trust that instinct and get your child checked.
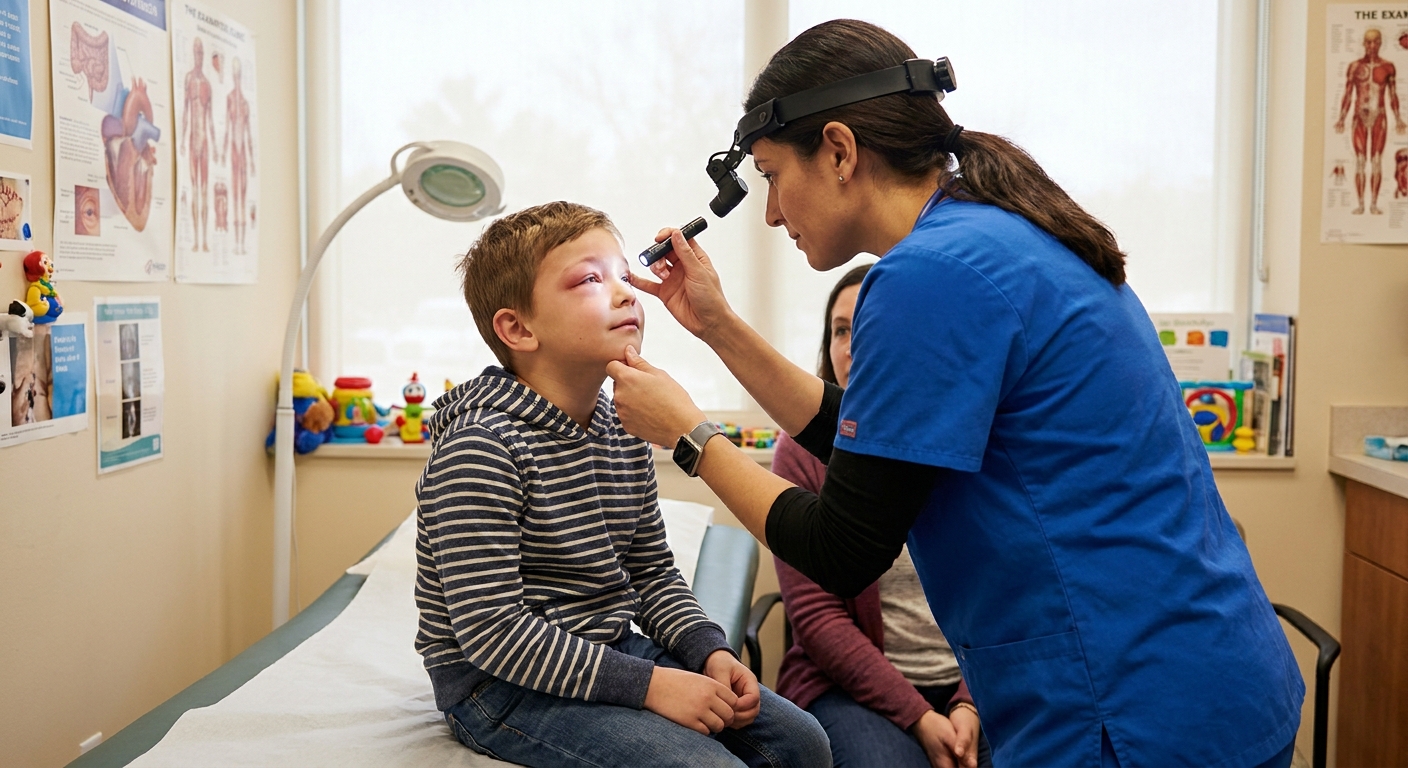
What it is
Periorbital cellulitis is a bacterial infection of the soft tissues of the eyelid and skin around the eye. It happens in front of the orbital septum, a thin layer that helps separate the eyelid tissues from the deeper structures in the eye socket.
That detail matters because infection behind that barrier is called orbital cellulitis, which is more serious and can affect eye movement, vision, and overall health.
Common causes
- Skin cuts or scratches near the eye, including from fingernails
- Bug bites that get infected after lots of rubbing and scratching
- Styes or infected eyelid glands
- Nearby skin infections (like impetigo) that spread
- Sinus infections can be involved too, especially when symptoms are prolonged or worsening
In real life, we often hear: “They had a cold all week, then woke up with a swollen eyelid.” That can happen with preseptal cellulitis, but sinus infections are also a classic driver of orbital cellulitis, which is why we ask so many sinus questions.
Which germs usually cause it?
You don’t need to memorize bacteria names, but it helps to know what clinicians are treating. Common culprits include Staphylococcus aureus (including MRSA in some communities) and Strep species. Before vaccines were routine, Hib was a bigger cause of severe eye-area infections. That’s one reason immunizations matter.
What it looks like
Periorbital cellulitis typically shows up as:
- One-sided eyelid swelling (often just one eye)
- Red or pink skin on the eyelid and around the eye
- Tenderness or pain when touched
- Warmth of the skin
- Sometimes drainage if there’s a stye or skin infection nearby
- Fever may or may not be present
Many kids can still open the eye, but it may take effort due to swelling. Some kids act mostly fine. Others feel run-down, especially if there’s also sinus infection symptoms.

Cellulitis vs pinkeye
Pinkeye is common and annoying. Periorbital cellulitis is less common and needs quicker evaluation. Here’s how parents often describe the difference.
Pinkeye (conjunctivitis)
- Redness on the white of the eye more than on the eyelid skin
- Thick discharge or crusting on lashes (especially in the morning)
- Itching or gritty feeling, more than deep tenderness
- Mild eyelid puffiness can happen, but the eyelid skin isn’t usually hot, very red, and sore
Periorbital cellulitis
- Red, swollen eyelid skin that can look “angry”
- More pain and tenderness, not just irritation
- Swelling that seems out of proportion to how red the actual eyeball is
- Often one-sided
Important note: Kids can have both. A child can start with conjunctivitis, rub the eye nonstop, and then develop a skin infection around the eyelid. When the eyelid skin becomes significantly swollen and tender, it’s time to be seen.
The sinus connection
The sinuses sit close to the eye socket. When bacteria set up shop in the sinuses, infection can spread into nearby tissues. This is especially important because sinus-related infections are a common pathway to orbital cellulitis.
You might notice eye-area swelling after:
- Several days of a cold followed by thicker nasal drainage
- Facial pressure or headache in older kids
- Bad breath that’s new and persistent
- Fever that returns after seeming to improve
This doesn’t mean every kid with a stuffy nose and puffy eyes has cellulitis. But if the eyelid is red, hot, and sore, or your child looks ill, it deserves same-day evaluation.
When fever matters
Fever doesn’t automatically mean “emergency,” but with an eye-area infection, it matters.
Get same-day care
Call your child’s doctor the same day (or go to urgent care) if:
- Eyelid swelling and redness is worsening over hours
- There’s a fever, especially with eyelid pain
- Your child has recent or current sinus symptoms
- Your child is less playful, not drinking well, or just seems “off”
- Your teen wears contact lenses and has eye pain or swelling
- There was eye or facial trauma (even “minor”) and swelling is developing
Go to the ER now
Go to the emergency room now if you notice any signs of possible orbital cellulitis:
- Pain with eye movement (looking up, down, side to side hurts)
- Limited eye movement or the eye seems “stuck”
- Vision changes: blurry vision, double vision, trouble seeing, or your child says they can’t see well
- The eye looks pushed forward or bulging
- New significant swelling of the whites of the eyes (conjunctival swelling, sometimes called chemosis)
- Severe headache, vomiting, confusion, or unusual sleepiness
- High fever or your child looks very ill
For babies and young infants, the threshold is lower. If your child is under 12 months and has eyelid swelling with fever, rapid worsening, poor feeding, or any signs above, choose urgent evaluation and don’t hesitate to use the ER.
If you’re debating whether it’s “bad enough” for the ER, use this simple rule: any vision change or pain with eye movement is ER-worthy.

What to expect at the visit
Clinicians usually diagnose periorbital cellulitis based on the exam and your child’s symptoms. They’ll look at:
- How red and swollen the eyelid skin is
- Whether your child can move the eye normally
- Vision (age-appropriate checks)
- Fever, heart rate, hydration, and overall appearance
- Nose and throat exam for sinus infection signs
Will my child need imaging?
Not always. If the provider is concerned about orbital cellulitis, an abscess, or the exam is limited by swelling or pain, they may recommend imaging (often a CT or MRI depending on the situation and facility). This is one reason ER evaluation is sometimes the right call.
Oral vs IV antibiotics
Treatment depends on how your child looks, their age, and whether there are hints the infection is deeper than the eyelid tissues.
Oral antibiotics
Oral antibiotics are often used when:
- Your child is otherwise well-appearing
- There are no vision changes and no pain with eye movement
- Swelling is mild to moderate
- Your child can drink fluids and keep medicine down
- You can reliably do follow-up within 24 to 48 hours
Parents are often surprised by how quickly oral antibiotics can help. You may see improvement within 24 to 48 hours, but finishing the full course is important even if the eyelid looks “back to normal.”
IV antibiotics and hospital care
IV antibiotics and hospital care are more likely when:
- Your child looks sick or has significant fever
- There’s concern for orbital cellulitis
- The swelling is severe or rapidly worsening
- Your child is very young (especially infants)
- Your child can’t take oral medication reliably
- There are medical conditions that affect immunity
Sometimes kids start with IV antibiotics in the hospital for a day or two and then step down to oral meds at home once they’re clearly improving.
One practical tip: If you’re sent home with oral antibiotics, ask what improvement should look like and when you should worry. Also ask who to call after hours if symptoms worsen.
Home care
While you’re waiting for a same-day appointment, or after treatment starts, focus on comfort and safe monitoring.
- Don’t apply leftover antibiotic eye drops unless a clinician tells you to. Periorbital cellulitis is a skin and soft tissue infection, not just an eye surface problem.
- Warm compresses can help if there’s a stye component. Use a clean, warm washcloth for 10 minutes a few times a day.
- Cold compresses can help reduce swelling and discomfort if your child prefers it.
- Pain and fever relief: use acetaminophen or ibuprofen if your child can take them and your pediatrician has okayed dosing.
- Discourage rubbing. Easier said than done, I know. Clean hands and short nails help.
- Monitor changes: take a quick photo every few hours in similar lighting. If the redness is on the cheek or forehead, you can lightly mark the outer edge of redness with a washable marker on skin only (not near the eye itself) so you can tell if it’s spreading.
Avoid pressure bandages, essential oils, or “drawing salves” near the eye. This area is too delicate, and irritation can make swelling look worse.
When to call back
Even with the right antibiotic, expect gradual improvement, not an overnight miracle. That said, cellulitis shouldn’t keep marching in the wrong direction.
Get urgent reassessment
Call your clinician urgently or return for care if:
- Swelling or redness is worsening or not improving within 24 to 48 hours on antibiotics
- Fever persists, or a new fever appears after starting antibiotics
- Your child develops pain with eye movement, vision changes, or a new severe headache
- Your child isn’t drinking, isn’t peeing normally, or seems significantly more tired
If your gut says something is off, trust that. You don’t need to “wait it out” with an infection near the eye.
Is it contagious?
Periorbital cellulitis itself isn’t typically spread person-to-person like viral pinkeye. However, the underlying triggers can be contagious, like colds, and sometimes skin bacteria can spread through close contact, shared towels, or poor hand hygiene.
Practical prevention steps:
- Handwashing for everyone
- Don’t share towels, washcloths, pillowcases, or eye makeup
- Keep fingernails trimmed to reduce skin breaks from scratching
- Treat and cover obvious cuts or insect bites, especially near the face
- Keep childhood vaccinations up to date, including Hib and pneumococcal vaccines
FAQ
Can allergies cause a swollen eyelid?
Yes. Allergies can cause puffiness, usually with itching, watery eyes, and often both eyes involved. Allergy swelling typically isn’t hot, very tender, or sharply red on the eyelid skin.
What about a bug bite?
Bug bites near the eye can swell dramatically and still be harmless. The clues that it may be getting infected are worsening redness, warmth, tenderness, fever, or swelling that keeps increasing after the first 24 hours.
My child’s eye is swollen shut. Is that always the ER?
Not always, but it’s a strong reason for same-day urgent evaluation. If the eye is swollen shut plus fever, severe pain, pain with eye movement, or any vision concern, choose the ER.
Will this damage my child’s vision?
Periorbital (preseptal) cellulitis treated promptly usually doesn’t cause vision problems. The reason we take it seriously is to make sure it isn’t progressing to orbital cellulitis, which can threaten vision if not treated quickly.
Bottom line
A swollen eyelid can be “no big deal,” but a swollen, red, tender eyelid is different. When you add fever or a child who looks unwell, periorbital cellulitis moves high on the list and deserves same-day medical care.
If your child has vision changes or pain with eye movement, skip the internet rabbit hole and head to the ER. You’re not overreacting. You’re protecting an eye and a brain sitting very close together.
Sources
- American Academy of Ophthalmology (AAO). Preseptal (Periorbital) Cellulitis and Orbital Cellulitis overview pages (accessed 2026).
- American Academy of Pediatrics (AAP). Red Book and AAP guidance on skin and soft tissue infections and periorbital/orbital infections (most recent editions, accessed 2026).
- Infectious Diseases Society of America (IDSA). Practice Guidelines for the Diagnosis and Management of Skin and Soft Tissue Infections (updated guideline, accessed 2026).