Petechiae in Kids: Tiny Red Spots After Coughing or Vomiting
Sarah Mitchell
Sarah Mitchell is a Registered Pediatric Nurse and a mother of three who has spent over a decade helping families navigate the beautiful, chaotic early years of childhood. She combines evidence-based medical knowledge with real-world parenting experience to offer practical, compassionate advice. At Awesome Parent, Sarah's mission is to help exhausted parents find solutions, trust their instincts, and finally get some sleep.
If you have ever picked your child up after a big coughing fit or a stomach-bug vomit and noticed tiny red pinpoints on their face, you are not alone. Parents ask about this in triage all the time, usually at night, usually panicked, usually after a very loud cough that shook the whole house.
The good news: petechiae after coughing, vomiting, or crying hard are often a pressure effect and can be benign, especially when they are limited to the face and your child is otherwise well-appearing. The important news: petechiae can also be a warning sign when they show up with fever, spreading spots, unusual sleepiness, or a child who just looks “off.”
Let’s walk through what petechiae are, what they are not, what to watch for, and how to capture useful photos if your clinician is doing a telehealth visit.
What petechiae are
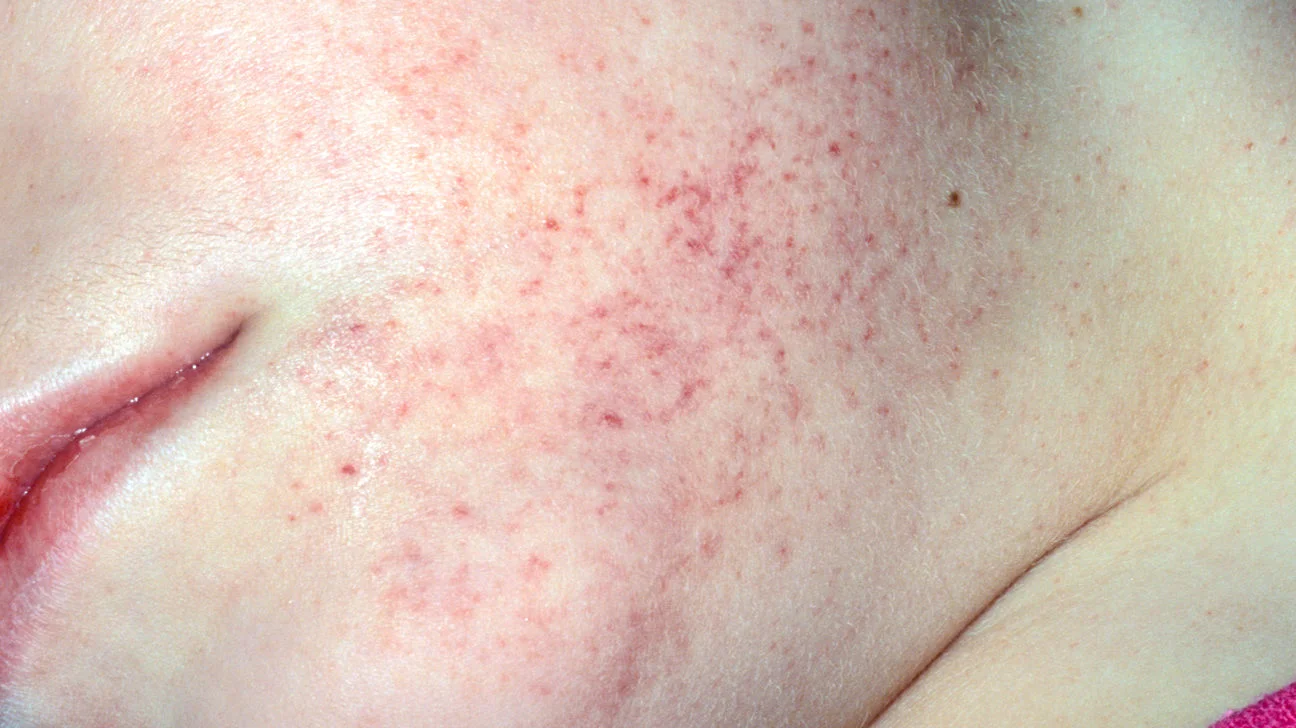
Petechiae (peh-TEE-kee-eye) are pinpoint red, purple, or brownish-red spots caused by tiny amounts of bleeding under the skin. They are usually very small, often the size of a pinhead.
A key feature is that petechiae typically do not turn white when you press on them because the color is from blood that has leaked out of a tiny blood vessel, not from temporary skin redness.
The “glass test” (helpful, not perfect)
If you have a clear glass, you can press it gently and briefly against the spots to see if they blanch (fade) under pressure.
- Blanching spots (they fade with pressure) are more consistent with many common rashes and irritation.
- Non-blanching spots (they stay red or purple) can be petechiae or purpura and deserve a closer look in context.
Important: lighting matters, and it can be hard to tell at home. If you are unsure, treat it as “possibly non-blanching” and keep reading for when to get checked.
Petechiae vs. other common kid rashes
Not every red dot is petechiae. Here are the usual look-alikes I see in clinic.
Heat rash (miliaria)
- Look: tiny red bumps, sometimes with a prickly feel
- Where: neck, chest, back, diaper area, skin folds
- Clues: hot day, fever, overdressed, sweaty
Eczema or irritation
- Look: red patches, rough texture, sometimes tiny scratches
- Where: cheeks, behind knees, inside elbows
- Clues: itching, dry skin, history of eczema
Hives (urticaria)
- Look: raised, puffy welts that move around
- Where: anywhere
- Clues: itchy, changes shape and location over hours
Insect bites
- Look: individual bumps, often with a center dot
- Where: exposed skin
- Clues: itchy, outdoor time, bites in clusters
Broken capillaries from rubbing or suction
- Look: tiny red dots or small bruised-looking spots
- Where: around eyes/cheeks after face rubbing, or in a clear circle after suction
- Clues: localized shape, known rubbing or suction
Why it can happen after coughing or vomiting
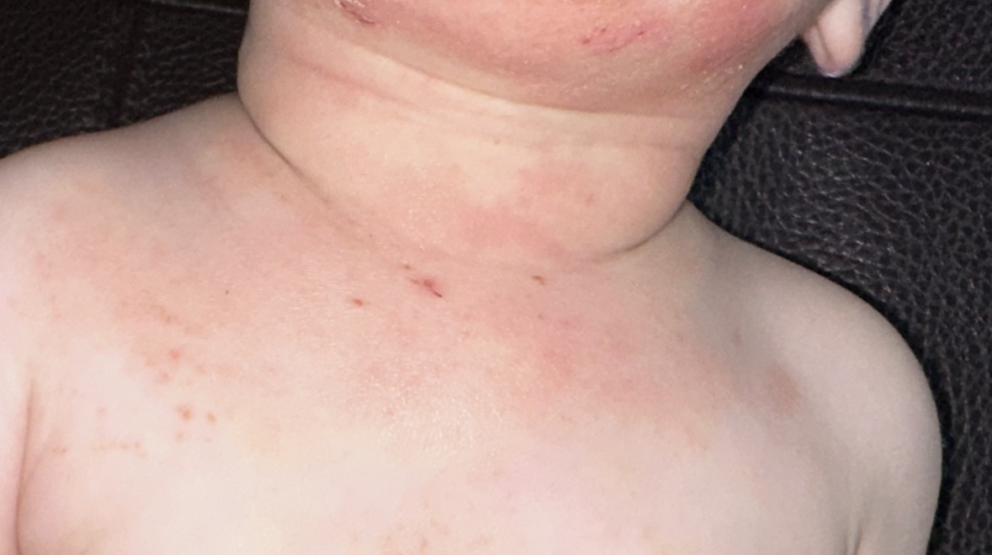
The most common benign scenario is pressure-related petechiae.
When a child coughs hard, vomits, or cries intensely, venous pressure in facial capillaries can rise briefly. That pressure can cause a few capillaries to leak, especially in delicate areas like around the eyes.
What benign pressure petechiae look like
- Location: typically on the face, especially around the eyes, cheeks, and sometimes upper neck
- Timing: show up right after a hard coughing or vomiting episode or intense crying
- Pattern: scattered pinpoints, not large patches
- How your child seems: acting mostly like themselves for the situation (tired from illness, but responsive, making eye contact, not struggling to breathe)
How long do they last?
Pressure petechiae often fade over 1 to 3 days, occasionally up to a week. They do not usually multiply rapidly once the triggering episode is over.
If your child is improving and the dots are staying in the same area and slowly fading, that is reassuring.
Distribution matters
One simple clue clinicians use is where the spots are.
- More reassuring: facial-only petechiae that appear right after a coughing or vomiting episode, with a child who looks reasonably well.
- More concerning: spots on the trunk, arms, legs, widespread distribution, or mucosal spots (inside the mouth), especially if there was no clear pressure trigger.
If your child will safely allow it, you can take a quick look in the mouth (especially the roof of the mouth). Do not force it. A photo is often easier than a prolonged “say ahhh” battle.
When it can be a red flag
This is the part I would read twice if it is 2 AM and you are debating what to do.
Petechiae can be associated with serious infections and blood or immune problems. The spots alone do not diagnose anything, but certain combinations raise urgency. In particular, fever plus a non-blanching rash is often treated as urgent until proven otherwise, because illnesses like meningococcal disease and other bloodstream infections can progress quickly.
Get urgent care now (ER or urgent care) if petechiae happen with:
- Fever and your child looks very ill (floppy, hard to wake, confused, inconsolable, or unusually lethargic)
- Rapidly spreading spots or spots appearing in new areas over minutes to hours
- Purpura (larger, bruise-like purple spots or patches, often more than about 2 to 3 mm)
- Neck stiffness, severe headache, sensitivity to light
- Trouble breathing, bluish lips, or signs of respiratory distress
- Seizure
- New petechiae not explained by pressure (no coughing, vomiting, or straining and the spots are on the trunk, arms, legs, or inside the mouth)
- Signs of abnormal bleeding such as frequent nosebleeds, bleeding gums, blood in urine or stool, or lots of new bruises without clear injury
Call your pediatrician same day if:
- Your child is overall doing okay but has fever plus petechiae and you are not sure of the cause
- The spots are not confined to the face or are not clearly linked to coughing, vomiting, or straining
- Petechiae keep appearing repeatedly with minor triggers
- Your child has a chronic condition or takes medications that could affect bleeding (your pediatrician can guide you based on specifics)
- Any infant under 3 months with petechiae, with or without fever (babies this age are evaluated promptly because the risk of serious infection and blood count issues is higher)
Nuance that matters: a well-appearing, fully immunized child with facial-only petechiae right after a clear coughing or vomiting episode may not always need an ER visit, even if they also have a viral fever. But because guidelines vary and the stakes can be high, it is still a same-day “talk to a clinician” situation.
If your gut is telling you, “This is not my kid,” listen to that. You do not need to prove it is urgent before you seek help.
Common causes clinicians consider
Parents often ask, “What does it mean?” The honest answer is: it depends on the whole picture, including fever, behavior, where the spots are, and how quickly they are changing.
More common and often less concerning
- Pressure petechiae from coughing, vomiting, constipation straining, or intense crying
- Minor viral illnesses (some viruses can cause temporary platelet changes or rash patterns that include petechial-looking dots)
- Local skin trauma (rubbing, scratching, suction)
Causes that need prompt evaluation
- Serious bacterial infection (including bloodstream infection or meningococcal disease). Some of these illnesses can progress quickly.
- Low platelets (platelets help blood clot). This can happen for different reasons, including immune-related conditions.
- Vasculitis (inflammation of blood vessels) in specific patterns, often with other symptoms like belly pain or joint pain
This is why clinicians often ask about fever timing, immunizations, recent infections, medications, bruising, and whether your child is acting normally.
What to do at home
If the spots appeared after coughing or vomiting and your child seems okay
- Check breathing: no persistent struggle, no ribs pulling in, no grunting
- Take a temperature and write it down (and how you took it)
- Offer fluids and treat the underlying trigger (for example, follow your vomiting plan from your pediatrician)
- Watch for change over the next few hours: spreading, fever developing or rising, behavior worsening
Avoid these common traps
- Do not assume “no fever” means “no problem.” Fever is important, but behavior and spreading pattern matter too.
- Do not keep checking so aggressively that you irritate the skin. Repeated rubbing can create more redness and confusion.
- Do not delay care if your child looks very sick, even if you think the dots are from vomiting.
Photos for telehealth
A clear photo can save you time and help your clinician decide what to do next. I cannot tell you how many times a blurry, dark photo turns a 5 minute plan into a back-and-forth message thread while everyone stays anxious.
How to take a useful rash photo
- Use natural light near a window if possible. Avoid harsh yellow bathroom lighting.
- Take two distances: one close-up (showing detail) and one pulled back (showing where it is on the body).
- Include a size reference like a clean fingertip or a coin held near the area (not covering the spots).
- Use the back camera if you can, and tap the screen to focus on the spots.
- Take a short video if the child is wiggly. Sometimes a single frame from a video is the clearest image.
Capture the glass test too (if you do it)
- Take one photo before pressing.
- Take one photo with the clear glass pressed gently against the skin, from the side enough to show pressure without blocking the view.
And yes, I know this is a lot to do with a sick kid. Do your best. One decent photo in good light is better than twelve frantic blurry ones.

Triage questions
Will pressure petechiae keep appearing every time my child coughs?
Some kids are more prone to it, especially with forceful coughing or vomiting. If it happens frequently, mention it to your pediatrician so they can consider whether there is an underlying issue like severe coughing spells, constipation straining, or less commonly a bleeding tendency.
Are petechiae contagious?
Petechiae themselves are not contagious. The illness causing coughing, vomiting, or fever might be.
Do I need to treat the spots?
No specific cream is needed for petechiae. Focus on the trigger and on monitoring for red flags. If there is associated skin irritation from wiping vomit or rubbing the face, a gentle moisturizer can help the irritated skin around the area, but it will not “treat” petechiae.
Simple decision guide
- Facial-only + right after coughing, vomiting, or crying + child acting mostly like themselves: often reasonable to monitor and message or call your pediatrician for guidance.
- With fever, spreading rash, larger purple bruisy areas, mouth spots, or a child who looks very unwell: seek urgent evaluation.
- Any infant under 3 months with petechiae: urgent same-day medical assessment.
If you want a script for calling, try: “My child has pinpoint non-blanching red spots that started at (time). They had (coughing/vomiting) and their current temperature is (number). They are acting (normal/sleepy/hard to wake). The spots are located (location) and are (spreading/not spreading).”
You are not overreacting. You are noticing something new on your child’s body and asking the right questions, which is basically the job description of parenting.
This article is for education and cannot diagnose your child. If you are worried about how your child looks or is acting, seek medical care.