Pink Eye in Babies: Causes, Care, and When It’s an Emergency
Sarah Mitchell
Sarah Mitchell is a Registered Pediatric Nurse and a mother of three who has spent over a decade helping families navigate the beautiful, chaotic early years of childhood. She combines evidence-based medical knowledge with real-world parenting experience to offer practical, compassionate advice. At Awesome Parent, Sarah's mission is to help exhausted parents find solutions, trust their instincts, and finally get some sleep.
If you are reading this with one hand while holding a sleepy baby with a crusty eye, I see you. Pink eye can go from “huh, that looks a little watery” to “why is the eyelid glued shut” in what feels like five minutes.
The good news is that many cases in babies are treatable and not dangerous. Quick safety note up front: newborns (especially under 4 weeks) and any baby with fever, significant swelling, a hazy-looking eye surface, severe pain, or trouble opening the eye need prompt medical evaluation. You will see exactly what “call now” looks like below, so you can stop panic-searching at 2 AM.
This baby-focused guide covers what pink eye is, what causes it, how it is different from a blocked tear duct, what you can safely do at home, and exactly when it crosses into “call now” territory.

What “pink eye” means in babies
Pink eye is the everyday name for conjunctivitis, which is inflammation of the thin, clear tissue that covers the white of the eye and lines the eyelid. In babies, that inflammation often shows up as:
- Redness of the white of the eye
- Goopy discharge (clear, yellow, or green)
- Crusting along the lashes after sleep
- Swollen eyelids
- Extra tearing
- Rubbing the eye or fussiness (older infants especially)
Sometimes it is only one eye at first and then the second eye joins the party a day or two later.
Common causes: viral vs bacterial
In clinic triage, one of the biggest questions is whether the conjunctivitis is viral or bacterial. They can look similar, and there is a lot of overlap.
Important reality check: you cannot always tell the cause by discharge color or thickness alone. Clinicians usually diagnose based on the whole picture (symptoms, exposures, age, exam, and how things are progressing).
Viral conjunctivitis
This is common during cold season and often travels with typical upper respiratory symptoms.
- Discharge: watery or thin mucus
- Eye redness: can be quite pink
- Other symptoms: runny nose, cough, sneezing, low-grade fever
- Course: often starts in one eye and spreads to the other
- Contagious: yes, very
Antibiotic eye drops do not help viral conjunctivitis, but comfort care helps a lot.
Bacterial conjunctivitis
Bacterial pink eye tends to be goopier and more “stuck shut” in the mornings.
- Discharge: thicker yellow or green pus-like drainage
- Crusting: lashes may be matted after naps and overnight
- Other symptoms: may occur with an ear infection or after a cold
- Course: can be one or both eyes
- Contagious: yes
Many pediatricians treat suspected bacterial conjunctivitis with prescription antibiotic eye drops or ointment, especially for daycare-aged children. For babies, your clinician may be more cautious about confirming the diagnosis and making sure nothing more serious is going on.
Allergic conjunctivitis (less common in young infants)
True seasonal allergies are less common in very young babies, but not impossible. You might see:
- Itchy, watery eyes
- Both eyes involved
- Sneezing and clear runny nose
- Symptoms that come and go with exposures
If your baby is under 6 months and looks like they have “allergies,” it is worth checking with your pediatrician rather than assuming.
Pink eye or blocked tear duct?
This is the mix-up I see most with infants. A blocked tear duct (nasolacrimal duct obstruction) is very common in babies and can cause persistent tearing and goop, especially after sleep. It can look a lot like pink eye at 2 AM.
Clues it may be a blocked tear duct
- Eye itself is usually not very red. The white of the eye often looks fairly normal.
- Constant tearing even when baby is not sick or upset.
- Goop returns quickly after you wipe it away.
- Often one eye (but can be both).
Clues it may be conjunctivitis
- Noticeable redness of the white of the eye
- More sudden onset
- Other cold symptoms or known exposure
- Spreads to the other eye within a day or two (common with viral)
Important note: a blocked tear duct can sometimes get infected (called dacryocystitis). If you see increasing redness, swelling, warmth, or tenderness near the inner corner of the eye, especially with fever, call urgently. This is not a “wait and see” situation.
Newborns need faster care
If your baby is a newborn (especially under 4 weeks) and develops eye redness or discharge, it deserves a prompt call to your pediatrician. Some newborn eye infections can be more serious and need specific treatment quickly.
Neonatal conjunctivitis can be caused by bacteria or viruses that require urgent, targeted treatment, including chlamydia, gonorrhea, and herpes. Many newborns receive antibiotic eye ointment at birth to help prevent certain infections, but it does not cover every cause and it is not a guarantee.
Other causes to know
Not every red, watery, goopy eye is classic conjunctivitis. Call your clinician promptly or seek urgent evaluation if you suspect:
- Something in the eye (foreign body) or a corneal scratch, especially if baby cannot stop squeezing the eye shut.
- Herpes eye infection, especially if you see blisters near the eye or baby was exposed to a cold sore.
- Rare glaucoma signs: lots of tearing with light sensitivity plus a cloudy or enlarged-looking cornea. This needs urgent evaluation.
What you can do at home
Whether the cause is viral, bacterial, or a blocked tear duct, these steps are generally safe and helpful for infants. If your baby has a medical condition or was born early, follow your clinician’s guidance.
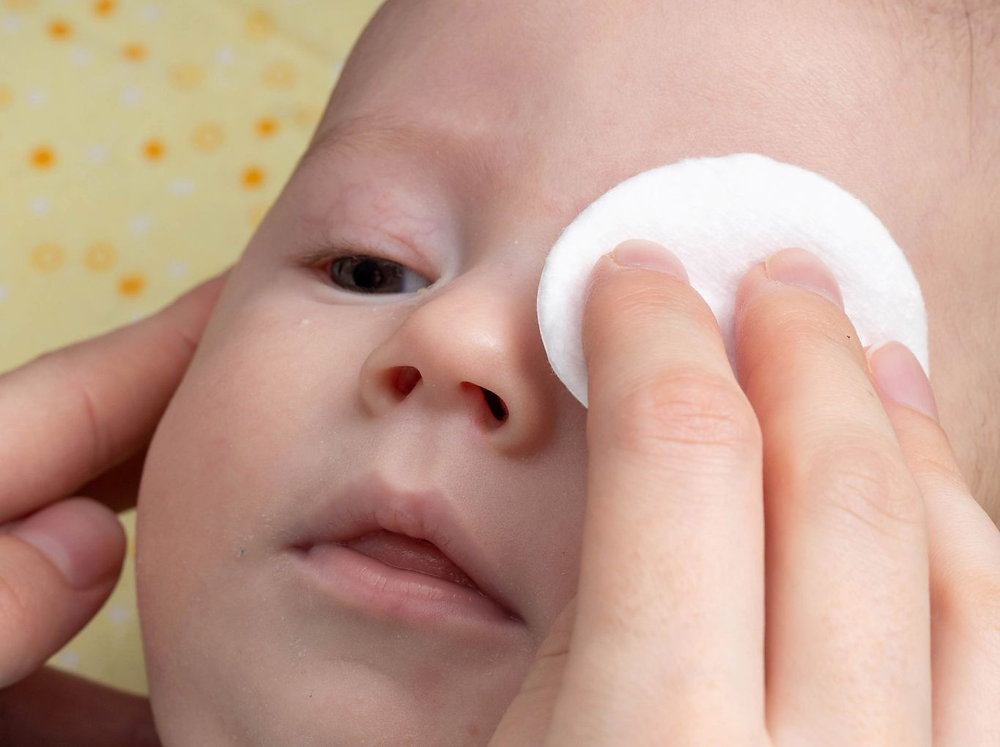
1) Clean the eye gently
- Wash your hands first.
- Use sterile saline or clean warm water on a soft cotton pad or clean washcloth.
- Wipe from the inner corner (near the nose) outward.
- Use a new pad/clean area for each wipe, and a separate cloth for each eye.
2) Warm compress for crusting
A warm compress can loosen sticky lashes and make baby more comfortable.
- Use warm (not hot) water.
- Hold on the closed eyelid for 1 to 2 minutes, then wipe gently.
- Repeat as needed, especially after sleep.
3) Cool compress for irritation
If the eyelid looks puffy or baby seems irritated, a cool, clean compress can feel soothing for short periods.
4) Keep hands away as much as possible
Easier said than done, I know. If your baby is rubbing, keeping nails trimmed and using mittens during sleep can help prevent skin breakdown and secondary infection.
5) Skip these common temptations
- No breast milk in the eye. I know this gets passed around parenting groups, but it is not a proven or sterile treatment.
- No leftover antibiotic drops. Wrong medication, wrong dose, and contamination risk.
- No redness-relief drops. Many are not appropriate for infants.
- No essential oils near the eyes.
- No eye patching. Patching can trap discharge and irritate the eye.
If your pediatrician prescribes eye drops or ointment, ask for a quick demo. Technique matters, especially with a wiggly baby.
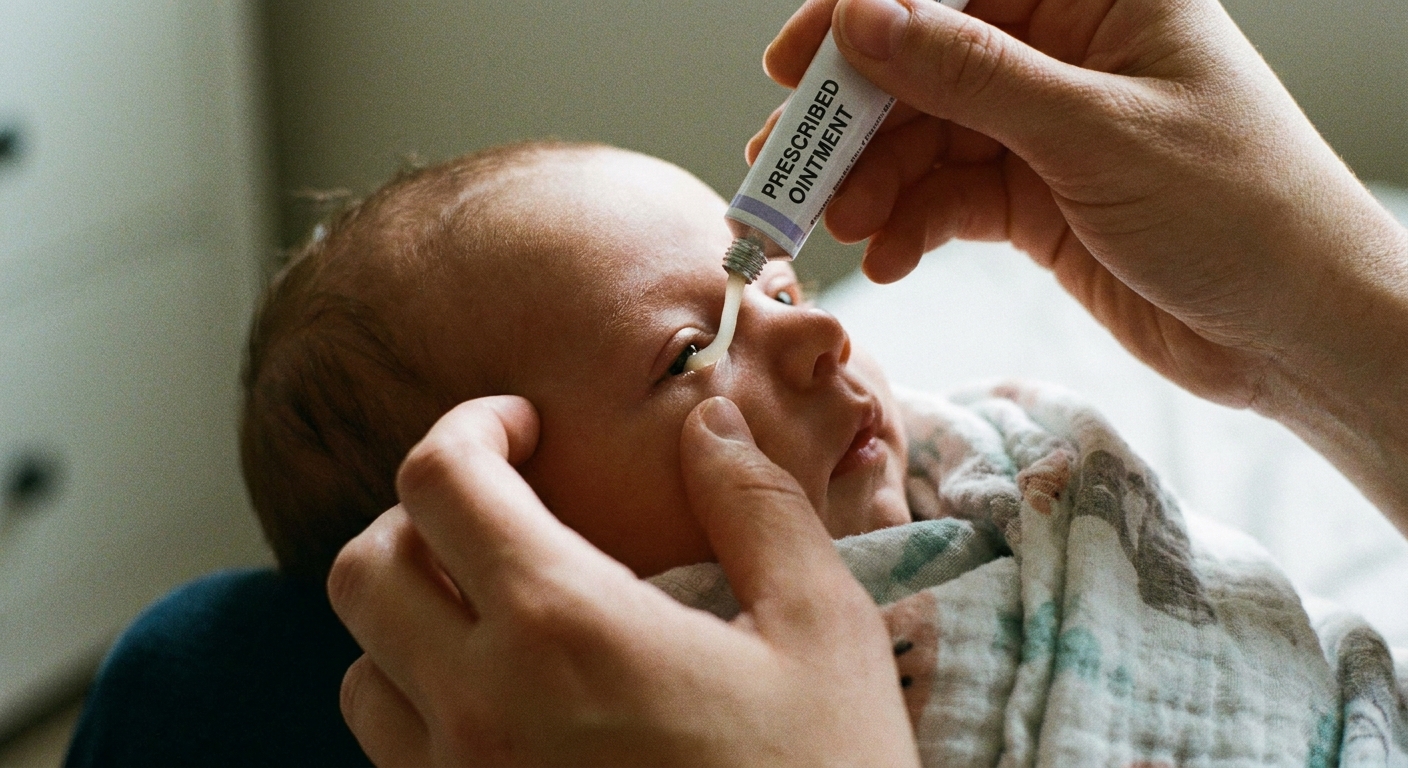
If antibiotic drops are prescribed
If your clinician thinks it is bacterial conjunctivitis, they may prescribe antibiotic drops or ointment. A few practical tips:
- Ointment is often easier for babies because it stays in the eye longer, even though it blurs vision briefly.
- Do not touch the tip of the tube or bottle to the eye or eyelashes.
- Finish the course as directed unless your clinician tells you otherwise.
- Expect improvement within 24 to 48 hours for many bacterial cases. If it is not improving, follow up.
How contagious is pink eye?
Viral and bacterial conjunctivitis are both contagious. They spread through hand-to-eye contact and shared items, and some viruses can spread through respiratory droplets too.
Reduce spread at home
- Wash hands before and after cleaning the eye or giving medication.
- Use separate washcloths for baby and change them daily.
- Change pillowcases and crib sheets if they get soiled with discharge.
- Avoid sharing towels with siblings.
- Avoid contact with anyone’s eye secretions, especially if an adult or sibling has an active eye infection.
- Wipe down commonly touched surfaces, especially if other kids are around.
Daycare and returning to care
This is the part parents hate, because policies vary. Many daycare centers still require 24 hours of antibiotics, even though that rule does not fit every cause of pink eye.
Here is a practical approach:
- Ask your daycare for their exact policy (written if possible).
- If your baby has fever, significant discomfort, or cannot be comfortably cared for (not feeding/sleeping normally, discharge is not manageable), keep them home regardless.
- If your clinician prescribes antibiotics for suspected bacterial conjunctivitis, many centers allow return after 24 hours of treatment.
- If it is likely viral, your baby may be contagious for several days. In the real world, centers often base return on overall wellness and ability to manage discharge.
If you need a note, your pediatric office can usually help, but they cannot override a daycare’s internal rules.
One nuance: with bacterial conjunctivitis, contagion risk likely decreases after about 24 hours of effective treatment, but it is not a magic off switch. Keep up the hygiene either way.
When to call (soon)
Call your pediatrician within the same day (or the next morning if it is the middle of the night and your baby is otherwise well) if:
- Your baby is under 3 months and has new eye discharge or redness
- The white of the eye is clearly pink/red
- Discharge is thick yellow/green or the eye is repeatedly crusted shut
- Symptoms are not improving after 24 to 48 hours of comfort care
- Your baby also has ear pain signs (extra fussiness lying down, tugging, poor sleep) or a fever
- You suspect a blocked tear duct infection (redness/tenderness/swelling near the inner corner)
- Someone in the home has a confirmed contagious eye infection and your baby develops symptoms
When it’s an emergency
Trust your gut here. Seek urgent care or emergency evaluation now if any of the following are present:
- Swelling around the eye that is rapidly worsening, especially if the eyelid looks very puffy or firm
- Red, hot, tender skin around the eye or spreading onto the face
- Fever in a young infant (follow your pediatrician’s fever guidance, especially under 2 to 3 months)
- Eye pain that seems significant (inconsolable crying when eye is touched or opened)
- Trouble opening the eye due to swelling
- Light sensitivity that seems intense
- Cloudy-looking cornea (the clear front surface of the eye looks hazy)
- Change in vision (hard to assess in babies, but concern if baby will not track as usual once the eye is cleaned)
- Trauma or chemical exposure to the eye
- Blisters or a rash near the eye
- Your baby looks very unwell, unusually sleepy, or hard to wake
These symptoms can signal conditions more serious than simple conjunctivitis, like periorbital or orbital cellulitis, corneal involvement, dacryocystitis, or other infections that need urgent treatment.
Quick FAQ
Can pink eye go away on its own?
Viral conjunctivitis often improves on its own with time and supportive care. Some mild bacterial cases can also improve, but in babies we typically want a clinician to weigh in, especially if there is thick discharge or swelling.
Will antibiotics help if it’s viral?
No. Antibiotics treat bacteria, not viruses. They also can irritate the eye and contribute to antibiotic resistance, so it is best to use them when they are truly needed.
How long is my baby contagious?
It depends on the cause. Viral pink eye can be contagious for several days. With bacterial conjunctivitis, the risk of spread often decreases after about 24 hours of effective antibiotics, but good hand hygiene still matters.
What if it’s only in one eye?
That can happen with viral, bacterial, or a blocked tear duct. One eye does not rule anything in or out, so look at the whole picture: redness, type of discharge, and other symptoms.
Is this the same as the “pink eye” older kids get?
The basics are similar, but babies have a couple of extra considerations: blocked tear ducts are common look-alikes, newborns need faster evaluation, and we are more cautious about severe swelling, fever, and anything that suggests deeper infection.
A calm next step
If your baby’s eye is goopy but they are otherwise acting like themselves, start with gentle cleaning, compresses, and frequent handwashing. Then call your pediatrician for guidance, especially if your baby is very young or the eye looks truly red.
And if you are staring at swelling, fever, a baby who cannot open their eye, a hazy-looking cornea, or a parent gut feeling that something is off, skip the waiting and get evaluated urgently. You are not overreacting. You are parenting.