Pityriasis Rosea in Kids: Herald Patch, Timeline, and Rash Look-Alikes
Sarah Mitchell
Sarah Mitchell is a Registered Pediatric Nurse and a mother of three who has spent over a decade helping families navigate the beautiful, chaotic early years of childhood. She combines evidence-based medical knowledge with real-world parenting experience to offer practical, compassionate advice. At Awesome Parent, Sarah's mission is to help exhausted parents find solutions, trust their instincts, and finally get some sleep.
If your child suddenly has a rash that seems to be multiplying, it is hard not to picture it marching through the house like a tiny skin-based invasion. The good news is that one common cause, pityriasis rosea (pit-uh-RYE-uh-sis ROH-zee-uh), is usually harmless and self-limited.
As a pediatric nurse and a mom, I can tell you the two biggest parent questions are: Is it contagious? and Is it ringworm? This guide will walk you through what to expect, what to do for itch, and when to call your child’s clinician to make sure it is not a look-alike that needs treatment.

What is pityriasis rosea?
Pityriasis rosea is a common rash that most often shows up in teens and young adults, but it can happen in school-age kids and, less commonly, younger children too. It sometimes follows a mild viral-like illness and then fades on its own.
It is considered an inflammatory rash that behaves like many post-viral rashes: it looks dramatic, spreads for a bit, then slowly resolves.
Is it contagious?
Most experts consider pityriasis rosea not usually contagious. The exact cause is not fully settled (it is sometimes associated with viruses like HHV-6/7), but it typically does not spread from child to child the way colds do.
In practical terms, most children can stay in school or daycare if they feel well and do not have a fever. Follow your school’s policy and your clinician’s advice, especially if the diagnosis is uncertain.
Typical timeline
Pityriasis rosea has a pretty recognizable rhythm. Not every child follows the script perfectly, but this is the typical sequence.
1) Prodrome
Some kids have a mild “coming down with something” phase first. You might notice:
- Low energy or just a bit off
- Headache
- Sore throat
- Low-grade fever
- Mild runny nose
Many kids have no prodrome at all.
2) Herald patch
The rash often starts with one larger patch called the herald patch. Parents frequently describe it as “a big ringworm-looking spot,” which is completely understandable.
Common herald patch features:
- One oval or round patch, often on the chest, belly, back, or upper thigh
- Pink to salmon colored in lighter skin tones, or violaceous, brown, or grayish in darker skin tones
- A slightly raised border with a fine scale (in deeper skin tones, redness and scaling can be subtler)
- Often about 2 to 10 cm across (about 1 to 4 inches)
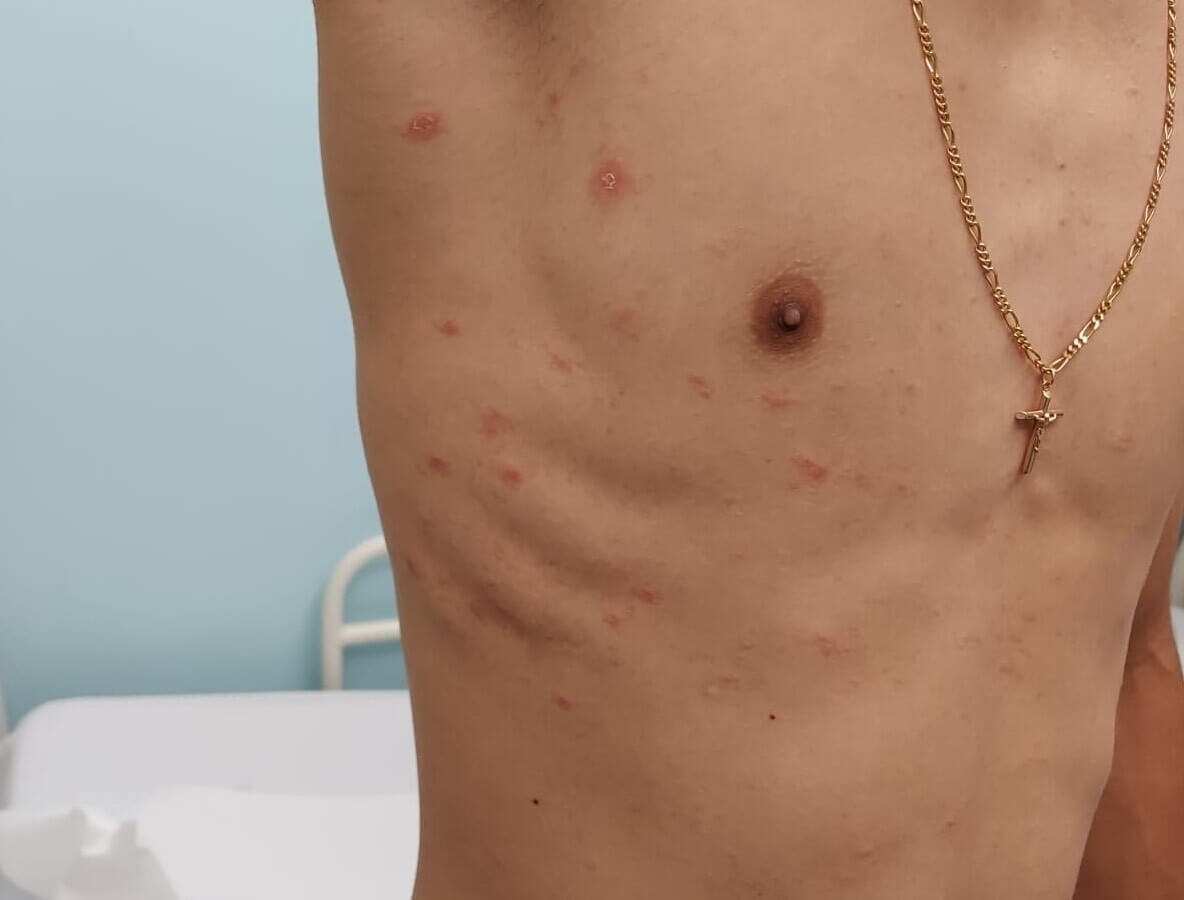
3) Secondary rash
After the herald patch, multiple smaller spots appear, most often on the trunk and sometimes the upper arms and upper thighs.
Key pattern clues:
- Many small oval patches that follow skin lines
- On the back, it can form a “Christmas tree” distribution
- The face, hands, and feet are usually spared in classic cases
How long does it last?
Most cases last about 6 to 8 weeks. Some clear sooner, and a minority can linger up to 12 weeks (about 3 months).
A very typical parent experience is:
- Week 1: One larger patch
- Weeks 2 to 3: A noticeable spread of smaller patches
- Weeks 4 to 8: Gradual fading, sometimes with lingering dry scale
Itch relief at home
Some kids do not itch at all. Others itch enough that bedtime becomes a full-contact sport. Heat and sweating often make it worse.
What you can try today
- Keep baths lukewarm and short. Hot water strips skin oils and ramps up itching.
- Use a gentle, fragrance-free cleanser or skip soap on the rashy areas if your child tolerates it.
- Moisturize within 3 minutes of bathing using a thick, fragrance-free cream or ointment.
- Cool compresses for 5 to 10 minutes on extra-itchy spots.
- Loose, breathable clothing to reduce friction and overheating.
- Consider an OTC anti-itch option like calamine lotion, or a low-strength steroid cream such as 1% hydrocortisone for short-term itch control, if your clinician agrees. Do not use prescription-strength steroid creams unless directed.
- Oral antihistamines can help some kids sleep if itching is disrupting rest. Ask your pediatrician for age-appropriate choices and dosing.
What to avoid
- Scrubbing the rash with washcloths or exfoliants
- Strong fragranced products that irritate sensitive skin
- Overheating from heavy pajamas, long hot showers, or intense exercise right before bed
If your child has eczema, their skin may be extra reactive. In that case, “boring skincare” is your best friend: simple cleanser, thick moisturizer, and fewer products overall.
Look-alikes
Here is the honest truth: many rashes can resemble pityriasis rosea. The key is spotting the situations where the “wait it out” approach is not the right one.
Ringworm
Ringworm is a fungus, not a worm, and it often starts as a round patch that can look like a herald patch.
Clues it might be ringworm:
- One or a few lesions that slowly expand
- A more obvious raised scaly border with central clearing
- Often itchy
- Exposure to wrestling mats, shared sports gear, or pets with patchy hair loss
Why it matters: Ringworm needs an antifungal. Steroid creams alone can make it look temporarily better while the fungus continues to grow.
Guttate psoriasis
Guttate psoriasis can pop up after strep throat and cause lots of small, drop-like scaly spots.
Clues it might be guttate psoriasis:
- Sudden shower of many small red or pink scaly spots
- History of psoriasis in the child or family
- Recent sore throat, fever, or known strep exposure
- Scale may be more noticeable than in pityriasis rosea
Why it matters: Your clinician may want to check for strep and discuss psoriasis-specific treatment.
Medication rash
Some medication-related rashes can mimic viral rashes and can be widespread.
Clues it might be a medication rash:
- Rash starts within days to a few weeks of a new medication
- Often more diffuse and symmetric
- May come with fever or feeling unwell
Why it matters: Some drug rashes are mild, but others require urgent evaluation, especially if there are mouth sores, facial swelling, or blistering.
Eczema or contact dermatitis
Dry, itchy, inflamed patches from eczema or contact irritation can sometimes look similar, especially if the child has sensitive skin.
Clues:
- Very itchy, dry patches
- Common in elbow creases, behind knees, wrists, and neck
- Flare after a new soap, detergent, lotion, or swimsuit
Atypical pityriasis rosea
Sometimes pityriasis rosea does not read the textbook. It can show up more in the armpits or groin (inverse pattern), look more papular (small bumps), or rarely have small blister-like spots. If the location or appearance seems “off,” it is worth checking in with your clinician.
Other rashes to keep on the radar
- Scabies: intense itching, worse at night, often affects wrists, finger webs, waistline, or groin, and can spread through households.
- Hand-foot-and-mouth disease: mouth sores plus rash on hands and feet.
- Secondary syphilis: uncommon in kids, but clinicians consider it in teens, especially if rash involves palms and soles.
When to call
Pityriasis rosea is usually a “watch and support” situation. But these are the times I want you to reach out promptly, because the diagnosis or treatment plan may need to change.
Call within 24 to 48 hours if:
- The rash is very itchy and your child cannot sleep even with basic measures
- The rash is on the face or heavily involves hands and feet
- Your child has significant scaling or thick plaques (possible psoriasis)
- The rash started after a new medication
- Your child had recent strep symptoms (sore throat, fever, swollen glands)
- The diagnosis is uncertain or you are seeing fast changes day to day
Seek urgent care today if:
- Fever plus your child looks very ill, very sleepy, or unusually irritable
- Blistering, skin peeling, or widespread skin pain
- Mouth sores, red eyes, or trouble swallowing
- Facial swelling, wheezing, vomiting, or signs of allergic reaction
- Purple spots that do not fade when pressed (a clinician should check these)
Trust your gut. If your child looks sicker than “just a rash,” you are not overreacting by getting them seen.
What the visit may include
Most of the time, diagnosis is made by history and exam. Sometimes, your clinician may do a quick test if a look-alike is likely.
- Skin scraping to check for fungus if ringworm is suspected. This is usually quick and minimally uncomfortable. The sample is often examined with a simple bedside test called a KOH prep.
- Strep test if symptoms suggest recent strep and guttate psoriasis is possible
- A review of all medications, including antibiotics, seizure meds, supplements, and new OTC products
Treatment is usually focused on comfort: itch control, gentle skincare, and reassurance about the timeline. In more severe or very itchy cases, clinicians sometimes consider options like phototherapy or an antiviral, depending on timing and the overall picture.
Parent FAQs
Can my child go to school or daycare?
Usually, yes. If your child feels fine and has no fever, pityriasis rosea alone typically is not a reason to stay home. If the rash is actually ringworm or scabies, school attendance rules may be different and treatment is needed.
Will it leave scars?
It usually does not scar. Some kids, especially those with deeper skin tones, may have temporary post-inflammatory color changes that fade over weeks to months.
Should we avoid sunlight?
Some people notice gentle sun exposure helps, and dermatology sometimes uses light-based treatments. That said, evidence is mixed, and sunburn can worsen inflammation. If you are outside, use sunscreen suitable for your child’s age and keep them cool and hydrated. If sun or heat seems to flare the rash or itch, back off.
Can it come back?
Recurrence is uncommon, but it can happen.
Next-week game plan
If your child seems well otherwise and the rash looks like classic pityriasis rosea:
- Take a few clear photos in good light every 3 to 4 days, so you can track change without guessing.
- Focus on itch control: lukewarm baths, thick moisturizer, cool compresses.
- Keep an eye out for red flags like fever, blistering, face swelling, or mouth sores.
- If the rash is not improving by about 8 to 12 weeks, or if it is rapidly worsening, check back with your pediatrician or ask about dermatology.
Rashes are unsettling because they are so visible, and they make kids look “sicker” than they often feel. Most of the time, pityriasis rosea is annoying but not dangerous. You are not failing because you do not recognize it at first glance. Most parents do not. You are doing exactly what good parents do: getting good information and keeping your child comfortable.