Pneumonia in Kids: Symptoms, Treatment, and Recovery Timeline
Sarah Mitchell
Sarah Mitchell is a Registered Pediatric Nurse and a mother of three who has spent over a decade helping families navigate the beautiful, chaotic early years of childhood. She combines evidence-based medical knowledge with real-world parenting experience to offer practical, compassionate advice. At Awesome Parent, Sarah's mission is to help exhausted parents find solutions, trust their instincts, and finally get some sleep.
Pneumonia can be one of those words that instantly spikes your heart rate. I get it. As a pediatric nurse (and a mom), I saw plenty of parents come in worried because their child had a cough that just felt different. The good news is that most kids recover very well with the right care and close monitoring.
This guide will walk you through what pneumonia is, the different types (viral, bacterial, and walking pneumonia), what symptoms can look like at different ages, how it is diagnosed, what treatment usually involves, and a realistic recovery timeline. I will also tell you exactly which warning signs mean you should seek urgent care.

What pneumonia is (plain English)
Pneumonia is an infection in the lungs. Instead of the airways staying open and clear, the tiny air sacs in the lungs can become inflamed and fill with fluid or mucus. That makes it harder to move oxygen in and carbon dioxide out, which is why breathing can look faster or more effortful.
Pneumonia is not the same thing as a regular cold. It can start after a cold, flu, RSV, or another respiratory virus and then settle into the lungs. It can also show up more suddenly, especially with some bacterial infections, without a clear “first it was a cold” stage.
Is pneumonia contagious?
What spreads is usually the virus or bacteria that can cause pneumonia. Kids can pass those germs through coughing, sneezing, and close contact. In some cases, pneumonia is part of the same illness that is spreading through a family or classroom.
Types of pneumonia in children
Most pneumonia in kids falls into one of these buckets. The type matters because it changes what helps and what does not.
Viral pneumonia
- Common causes: RSV, influenza, parainfluenza, adenovirus, and others.
- Typical pattern: Often starts like a cold with runny nose and cough, then breathing gets worse over a few days.
- Treatment: Supportive care. Antibiotics do not treat viruses.
- Recovery: Many children gradually improve over 1 to 2 weeks, but cough can linger for several weeks.
Bacterial pneumonia
- Common causes: Streptococcus pneumoniae is a classic one, among others.
- Typical pattern: Can come on more suddenly, often with higher fever and a child who looks more sick or more tired.
- Treatment: Antibiotics are often helpful. Many children start to improve within 24 to 72 hours once on the right antibiotic, especially in fever and overall comfort.
- Recovery: Fever often improves within a few days once on the right antibiotic, but energy and cough can take longer.
Walking pneumonia (often atypical pneumonia)
- Common cause: Mycoplasma pneumoniae (more common in school-age kids and teens).
- Typical pattern: Persistent cough, low-grade fever, sore throat, fatigue. Kids may seem “not that sick” but the cough drags on.
- Treatment: Sometimes specific antibiotics are used, depending on age and clinician judgment.
- Recovery: Often a longer cough, even as fever fades.
Note: Kids can also get aspiration pneumonia (from inhaling food, liquid, or vomit), or pneumonia related to underlying conditions. Those situations deserve prompt medical evaluation. Also, in preschoolers, many pneumonias are viral, which is one reason antibiotics are not always the right answer.

Pneumonia symptoms by age
Kids do not read the textbook, so symptoms can vary. Here is what I look for as a nurse and as a mom.
Babies (newborn to 12 months)
- Fast breathing or breathing that looks like hard work (ribs pulling in, nostrils flaring, head bobbing)
- Poor feeding, fewer wet diapers
- Sleepier than usual, harder to wake
- Fever, or sometimes low temperature in very young infants
- Cough may be mild at first
Toddlers and preschoolers (1 to 5 years)
- Fever (sometimes high)
- Cough that is persistent and worsening
- Fast breathing
- Vomiting with coughing, belly pain, or poor appetite
- Less playful, clingier, looks unwell
School-age kids and teens
- Cough (often the main symptom, especially with walking pneumonia)
- Chest pain, especially with deep breaths or coughing
- Fever or chills
- Shortness of breath with activity
- Fatigue, headache, sore throat
What does trouble breathing look like?
It can be hard to tell at first, especially when you are tired and it is the middle of the night. Here is what to look for:
- Breathing faster than usual, even at rest (clinicians use age-based cutoffs, so if you are unsure, call)
- Using extra muscles to breathe: skin pulling in between ribs or above the collarbone
- Nasal flaring
- Grunting in babies
- Struggling to speak in full sentences (older kids)
- Blue or gray lips or face (emergency)
How pneumonia is diagnosed
Diagnosis is usually a combination of the story you tell, the exam, and sometimes testing.
What your clinician listens for
When we listen to lungs, we are paying attention to things like crackles, decreased breath sounds, wheezing, and how well air is moving. We also look at breathing rate, oxygen level, hydration, and overall appearance.
Will my child need a chest X-ray?
Not always. Chest X-rays are often used when:
- Symptoms are moderate to severe
- Oxygen levels are low
- The diagnosis is unclear
- Your child is not improving as expected
- There is concern for complications
A chest X-ray can show areas of inflammation or consolidation in the lungs, but it does not always perfectly separate viral from bacterial pneumonia.
Other tests you might see
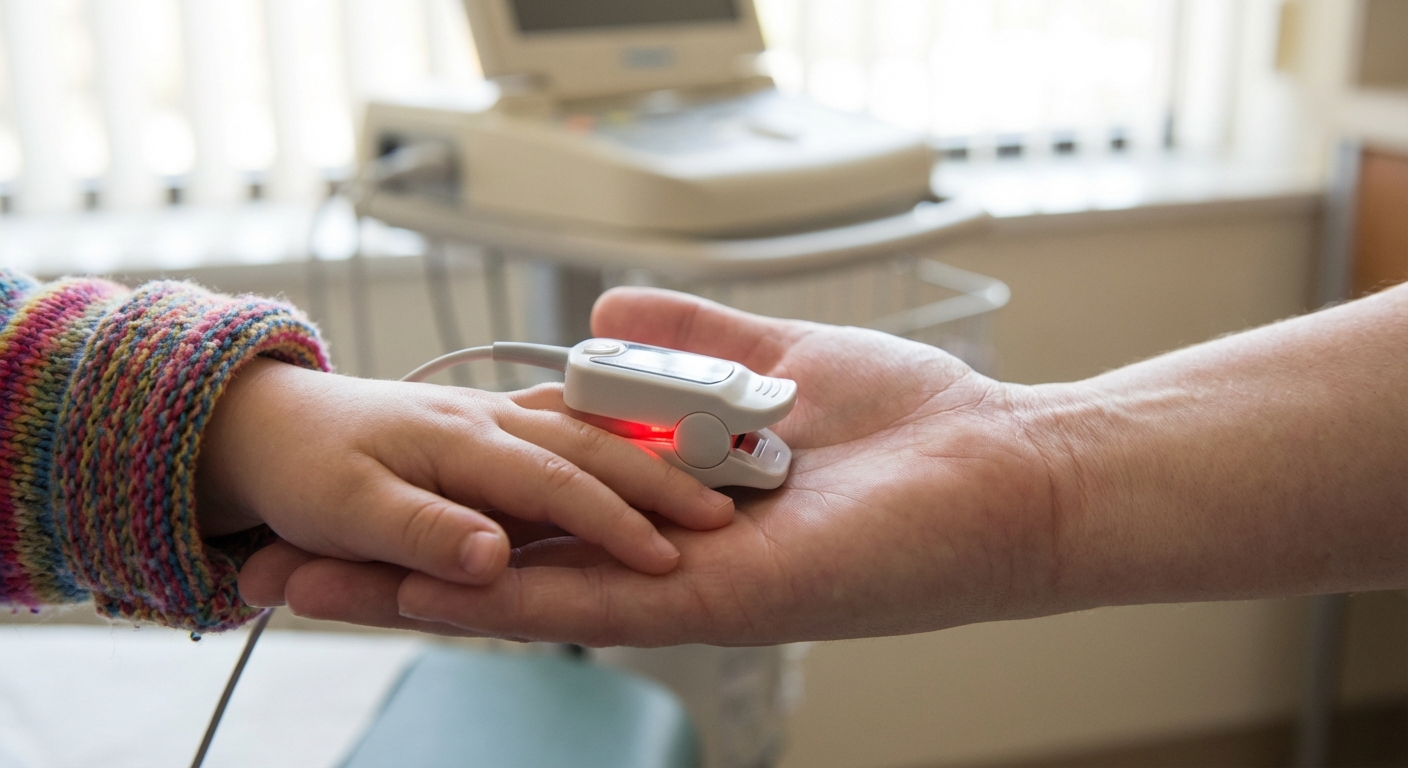
- Pulse oximetry: A painless clip on the finger or toe to measure oxygen saturation.
- Viral testing: Depending on season and symptoms (flu, RSV, COVID).
- Blood work: Sometimes used in sicker kids or hospitalized kids.
- Sputum testing: Not common in younger kids, more in older kids in certain cases.
Treatment basics
The right treatment depends on the likely cause and how your child is doing overall.
When antibiotics help
Antibiotics treat bacterial pneumonia. They do not help viral pneumonia, and using them “just in case” can cause side effects and contribute to antibiotic resistance.
Your child’s clinician may lean toward antibiotics when:
- Symptoms and exam suggest bacterial infection
- There is high fever with a child who appears more ill
- There is a focal finding on exam or X-ray
- Your child is at higher risk for complications
Important: If antibiotics are prescribed, take them exactly as directed and finish the course unless your clinician tells you otherwise.
Supportive care that helps
- Fluids: Small frequent sips are fine. Hydration helps thin mucus and supports recovery.
- Fever and pain relief: Acetaminophen or ibuprofen when age-appropriate and dosed correctly. Fever itself is not dangerous in most kids, but comfort matters.
- Rest: Expect extra sleep and lower energy for a while.
- Honey for cough: For kids over 1 year, honey can reduce nighttime cough.
- Humidified air: A cool-mist humidifier can make breathing feel easier for some kids.
What to skip (or be cautious with)
- Over-the-counter cough and cold meds: Not recommended for young children and often not helpful.
- Leftover antibiotics: Please do not. Wrong drug or wrong dose can delay proper care.
- Forcing big meals: Focus on hydration. Appetite often returns later.
Do breathing treatments help?
Sometimes. If your child has wheezing or underlying asthma or reactive airway disease, inhalers or nebulized medications may be part of the plan. Pneumonia itself is not always a wheeze problem, so this is individualized.
Recovery timeline
Parents often expect a straight line from “sick” to “better.” Pneumonia recovery is usually more like a slow staircase.
Typical improvement
- First 24 to 72 hours: With bacterial pneumonia on the right antibiotic, many children start to improve in fever and breathing effort. With viral pneumonia, progress can be slower and symptoms may peak around days 3 to 5 of illness.
- Days 4 to 7: Energy starts to return. Appetite improves. Cough is still common.
- Weeks 2 to 4: Cough gradually fades. Some kids have a lingering cough longer, especially after viral infections or walking pneumonia.
How long is my child contagious?
It depends on the germ and your child’s age. As a practical rule, many kids are less contagious once fever-free for 24 hours (without fever reducers) and symptoms are improving, but some viruses can spread before fever and can keep shedding after a child seems better. If your child has bacterial pneumonia and is on antibiotics, many clinicians consider them less contagious after about 24 hours on antibiotics. Always follow your doctor’s guidance and your daycare or school policies.
Back to daycare or school
- Fever-free for 24 hours without medicine
- Breathing comfortably enough to participate (significant shortness of breath or low oxygen is a no-go)
- Drinking well and able to get through the day
If your child is still coughing but otherwise well, they often can return. Cough can linger even when the infection is resolving.

When to get help
I never want you to panic, but I do want you to have clear lines in the sand. If your child is very young (especially under 3 months) or has a chronic condition or immune compromise, your threshold to call and be seen should be lower.
Call your pediatrician today if
- Fever lasts more than 3 days, or returns after being gone
- Cough is worsening, not improving after several days, or disrupting sleep significantly
- Your child has mild increased work of breathing
- Your child is drinking less and peeing less
- Chest pain is present, especially with breathing
- Your child has a chronic condition (asthma, heart disease, prematurity, immune compromise) and is getting sicker
Go to urgent care or the ER now if
- Breathing is hard work: ribs pulling in, nasal flaring, grunting, head bobbing
- Blue, gray, or very pale lips or face
- Oxygen saturation is low if you were instructed to monitor at home
- Severe lethargy: very hard to wake, not interacting
- Dehydration: very dry mouth, no tears, significantly fewer wet diapers, unable to keep fluids down
- Newborns and young infants with fever or breathing concerns should be evaluated urgently
Why some kids are hospitalized
Some children need hospital care for oxygen support, IV fluids, close monitoring, or treatment of complications. Clinicians consider:
- Low oxygen levels
- Moderate to severe breathing distress
- Young age (especially infants)
- Inability to stay hydrated
- Failure of outpatient treatment
- Concern for complications like pleural effusion (fluid around the lung) or empyema (infected fluid), and more rarely respiratory failure
FAQ
Can pneumonia sound like just a bad cough?
Yes. Especially walking pneumonia or viral pneumonia can present with a stubborn cough and fatigue. The deciding factor is often breathing effort, fever pattern, and how your child looks overall.
Does pneumonia always cause a high fever?
No. Some kids have low-grade fever or none at all, especially with walking pneumonia or in certain viral cases. Focus on the whole picture, including breathing and hydration.
Can my child get pneumonia after the flu or RSV?
Yes. Viral infections can inflame the airways and make it easier for bacteria to take hold. If your child seems to be improving and then suddenly gets worse again, that is a good reason to call your pediatrician.
Will my child need a follow-up visit or repeat X-ray?
Many children do not need a repeat X-ray if symptoms resolve as expected. Follow-up is more likely if symptoms linger, your child had severe illness, or complications were suspected.
Comfort for long nights
When your child has pneumonia, nights can feel endless. These small steps can help:
- Keep your child slightly upright to rest if it helps their breathing and your pediatrician says it is safe for their age and sleep setup.
- Safe sleep reminder for infants: Place babies on their back on a firm, flat surface with no wedges, positioners, or extra pillows.
- Offer fluids every hour or two while awake.
- Use a cool-mist humidifier and keep the room comfortably cool.
- For kids over 1 year, a spoonful of honey before bed can reduce coughing.
- Track breathing effort, wet diapers, and fever so you are not relying on exhausted memory at 2 AM.
If you are staring at your child and thinking, “Something is not right,” you are allowed to trust that feeling. You do not need to wait until it is dramatic to get help.
Prevention
You cannot prevent every respiratory illness, but you can lower the odds of severe infection and complications:
- Vaccines: Keep routine vaccines up to date, including pneumococcal, plus seasonal flu and COVID vaccines when eligible.
- Hand hygiene: Handwashing still matters, especially during cold and flu season.
- Smoke exposure: Avoid cigarette or vape smoke around kids. It irritates airways and raises infection risk.
- Sick-day basics: Teach kids to cover coughs, and keep them home when they have fever and feel unwell.
Bottom line
Pneumonia sounds scary because it can be serious, but most children recover fully with timely care, rest, and close monitoring. The biggest things I want you to watch are breathing effort, hydration, and your child’s overall alertness. If breathing looks hard, your child is not staying hydrated, or your gut says this is more than a routine virus, reach out to your pediatrician or seek urgent care.
Medical note: This article provides general education and is not a substitute for medical advice. If you are worried about your child’s breathing, seek care right away.