Poison Ivy, Oak, and Sumac in Kids
Sarah Mitchell
Sarah Mitchell is a Registered Pediatric Nurse and a mother of three who has spent over a decade helping families navigate the beautiful, chaotic early years of childhood. She combines evidence-based medical knowledge with real-world parenting experience to offer practical, compassionate advice. At Awesome Parent, Sarah's mission is to help exhausted parents find solutions, trust their instincts, and finally get some sleep.
If your child comes inside from “just a quick backyard adventure” and suddenly has angry, itchy lines on their skin, you are not alone. Poison ivy, poison oak, and poison sumac are incredibly common, and the rash can feel dramatic even when it is not dangerous.
As a pediatric nurse and a mom, here is my calm, evidence-based plan: identify the pattern, wash as soon as you can, treat the itch safely, and know the red flags that mean it is time to get medical help. Also, if you are feeling guilty because you “should have noticed the plant,” take a breath. This happens to careful families all the time.
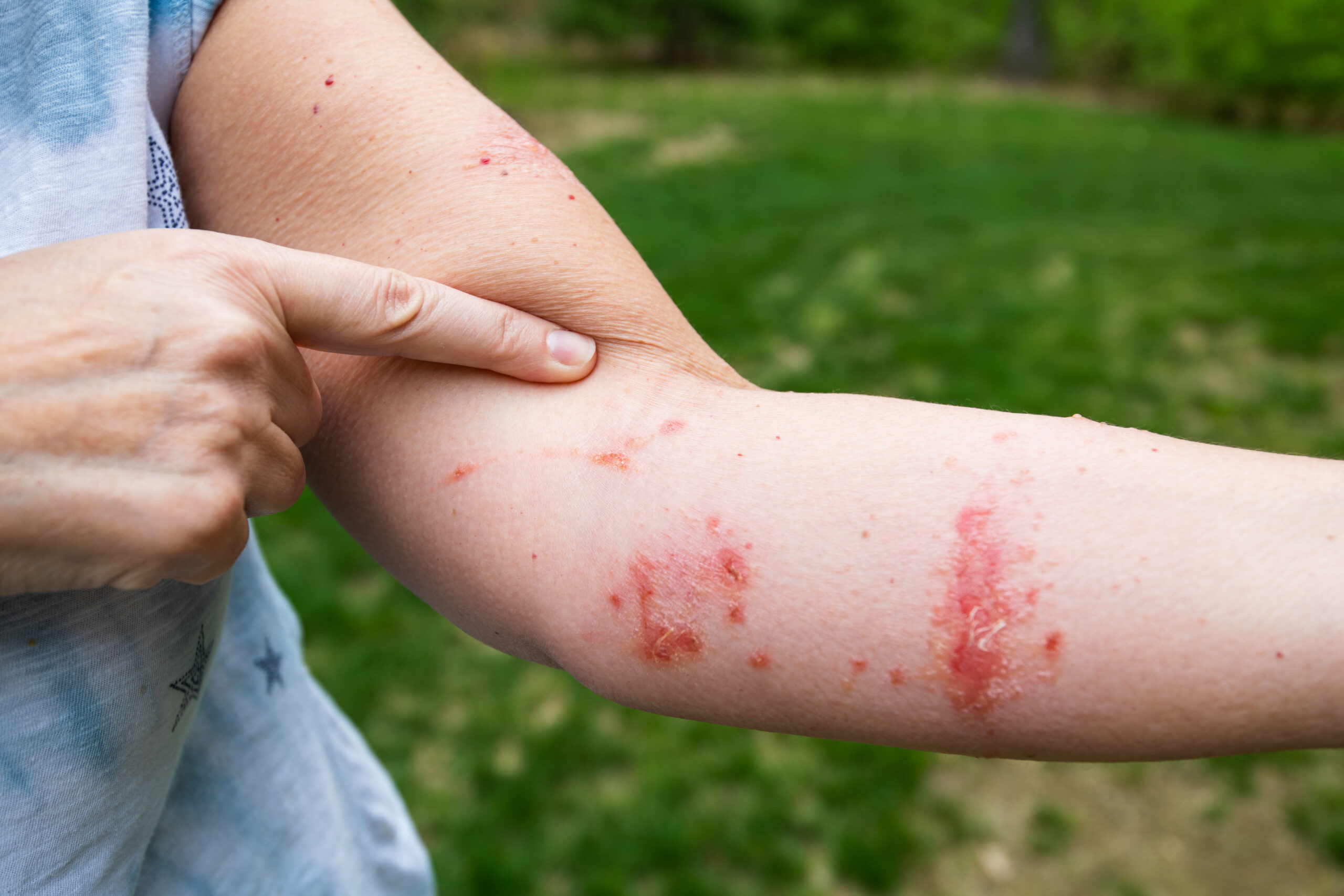
What causes the rash
Poison ivy, oak, and sumac contain an oily resin called urushiol. When it touches the skin, it can trigger an allergic skin reaction. The key things to know are:
- The fluid from blisters does not spread the rash. The rash “spreading” over days is usually delayed reaction timing, not contagious ooze.
- Urushiol oil can cause repeat exposure. Oil left on hands, under nails, clothing, shoes, pets’ fur, sports gear, or car seats can keep re-exposing skin.
- Urushiol can stick around. On unwashed items, it can remain active for a long time (often months, sometimes longer) until it is properly cleaned.
- Lines happen because plants brush the skin. Streaks and stripes are classic, especially on arms, legs, and ankles.
How to identify it in kids
Common clues
- Itching that can be intense, often worse at night.
- Red bumps or raised patches that may become tiny blisters.
- Linear streaks where the plant brushed the skin.
- Appears 12 to 48 hours after exposure for many kids, sometimes up to several days.
What it can look like
- Bug bites: often round, scattered, and centered on a puncture point rather than streaky lines.
- Eczema flare: usually in familiar spots and looks more dry and scaly than blistery.
- Impetigo: honey-colored crusting and spreading sores, often around the nose or mouth.
- Hives: raised welts that move around and change shape quickly, rather than fixed streaks.
- Other contact rashes: linear rashes can also come from other plants, plant sap, sunscreen, fragrances, or chemicals from yard and sports gear.
If you are unsure, take a clear photo in good light. If it worsens, that photo is surprisingly helpful for your pediatrician (or your child’s clinician) and can speed up the right treatment.
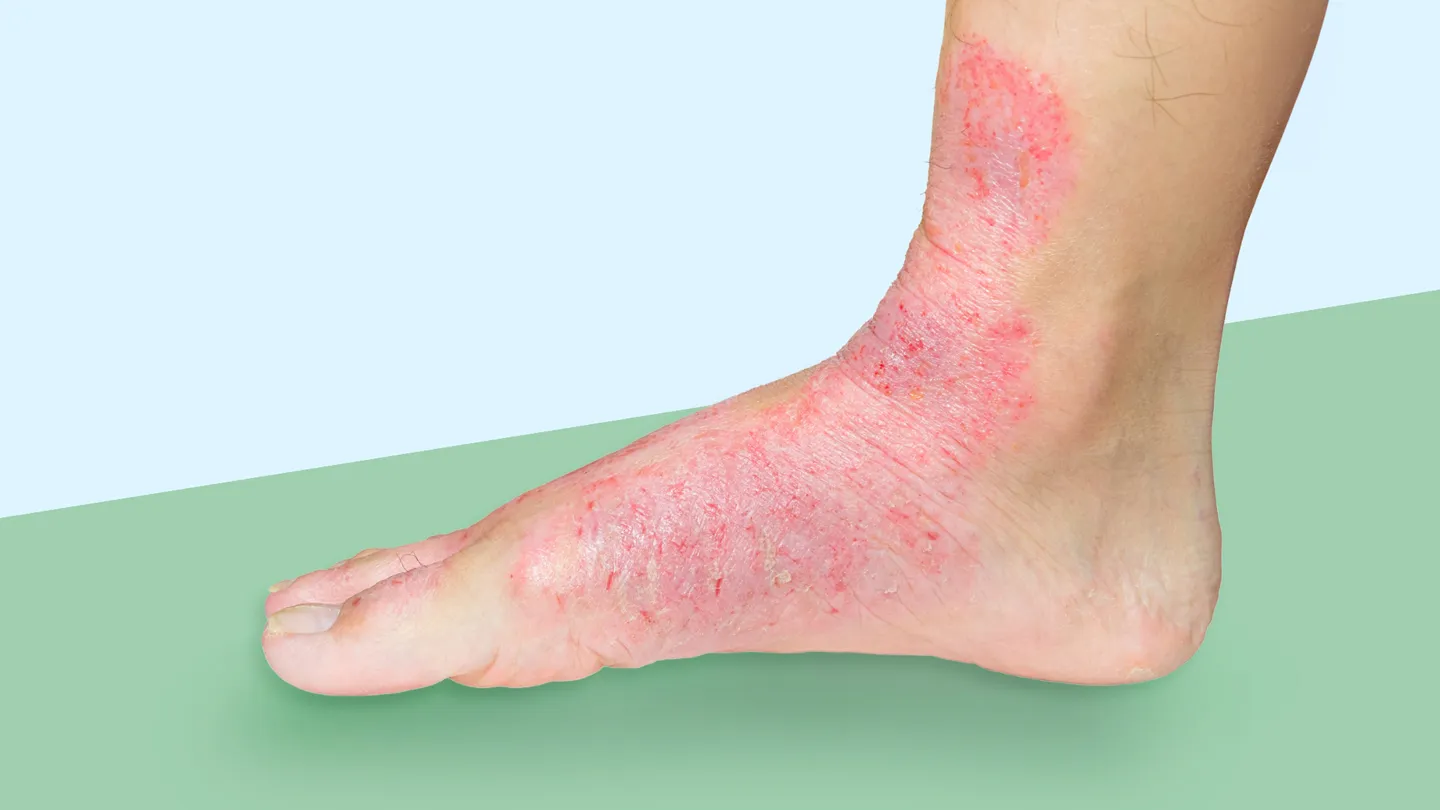
Do this first: wash it off
If you think poison ivy, oak, or sumac touched your child’s skin, wash as soon as possible. Earlier is better, ideally within minutes to an hour, but washing can still help later by removing any remaining oil and preventing re-exposure.
Step-by-step: skin
- Do not scrub hard. Scrubbing can irritate skin and does not help remove oil better.
- Rinse with cool or lukewarm water first. Hot water can increase itching and may make it easier for oil to move around if it has not been removed yet.
- Wash with soap. Use regular soap and lots of running water. Pay attention to wrists, ankles, behind knees, and under fingernails.
- Clean under nails. Use a soft nail brush if you have one.
- Pat dry. Use a clean towel. Then wash that towel.
Step-by-step: clothes, shoes, gear
- Clothing: remove carefully, avoiding rubbing it across the face. Wash separately in hot water with detergent if possible.
- Shoes: wipe down with soap and water, especially laces and edges.
- Jackets, backpacks, sports gear: wipe hard surfaces with soap and water. For fabric items, wash if you can.
Do not forget pets
Urushiol can stick to fur. If your dog ran through brush and then cuddled your child, your child may be the only one with a rash. Bathe pets with pet shampoo and water, and consider gloves if you are sensitive.

Itch relief: home options
The goal is to reduce itching and inflammation so your child can sleep and avoid scratching, which can break skin and invite infection.
Good first-line options
- Cool compresses: 10 to 15 minutes at a time, several times a day.
- Oatmeal baths: colloidal oatmeal in lukewarm water can be very soothing.
- Calamine lotion: can dry oozing spots and reduce itch. Apply a thin layer.
- 1% hydrocortisone cream: helps inflammation and itch for mild cases on arms and legs. Use a thin layer 1 to 2 times daily. Limit use to up to 7 days unless your pediatrician tells you otherwise. Avoid using on large areas, on broken skin, or on the face, groin, or genitals unless you are specifically instructed.
Antihistamines: what to expect
Antihistamines do not treat the underlying allergic contact dermatitis itself. They may help some kids with itching, and sedating ones can be most useful for sleep. They tend to help more if your child also has hives or seasonal allergies going on.
- Non-drowsy options (daytime): cetirizine or loratadine are commonly used. Follow the label for age and weight, or ask your pediatrician.
- Drowsy option (nighttime): diphenhydramine is sometimes used for short-term nighttime itch. Use only as directed for age and weight, and avoid combining with other sedating medicines unless your pediatrician says it is ok.
Age notes
- Babies and toddlers: call your pediatrician before using medicated creams on large areas, or any oral antihistamine under age 2. Cool compresses and oatmeal baths are usually a safe starting place.
- School-age kids: topical hydrocortisone and calamine are often helpful for mild rashes when used as directed.
- Teens: similar approach, but teens often have larger exposure from sports and yard work and may need stronger treatment if widespread.
What to skip
- Topical antibiotics “just in case”: not needed unless there are signs of infection, and they can irritate skin.
- Topical anesthetics (like benzocaine): can trigger additional contact reactions in some kids.
- Bleach, rubbing alcohol baths, harsh cleansers: too irritating and unsafe for skin.
Face, eyes, or genitals
These areas are more sensitive, swell more easily, and deserve a lower threshold for calling the pediatrician.
Face and eyelids
- Call your pediatrician if there is significant swelling, eyelid involvement, or the rash is close to the eye.
- Go to urgent care or ER if the eye is swollen shut, your child has trouble seeing, or there are any breathing symptoms.
- Avoid putting hydrocortisone right near the eye unless your pediatrician specifically recommends it.
Genitals or groin
- Call your pediatrician the same day for significant swelling, pain with urination, or widespread blistering in this area.
- Comfort measures like cool compresses and loose cotton clothing can help while you wait for guidance.
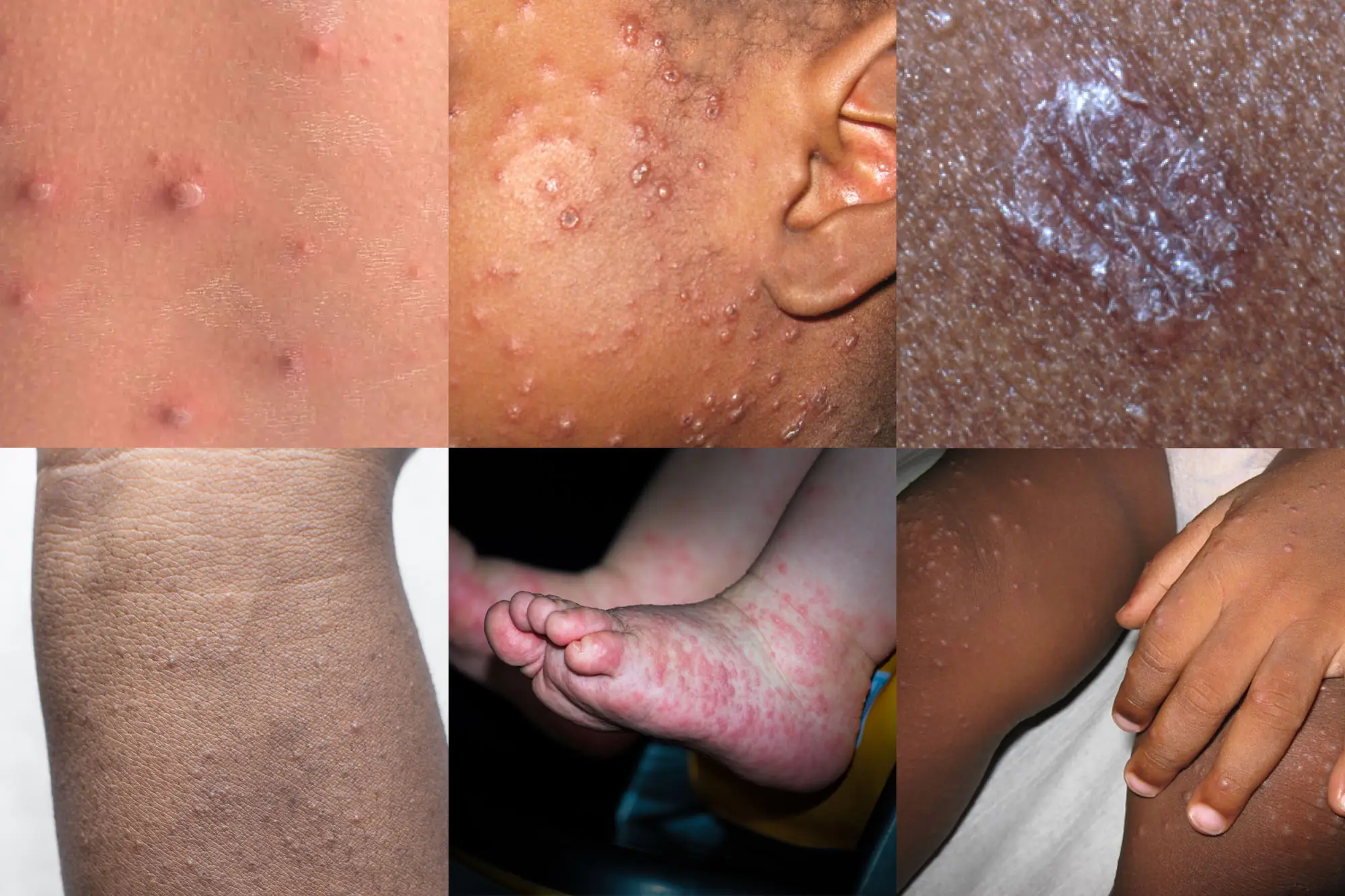
When to call or go in
Call your pediatrician within 24 hours if:
- The rash is widespread or rapidly worsening.
- It involves the face, eyelids, lips, or genitals.
- Your child is miserable despite home care, especially if sleep is impossible.
- The rash is on a child with a history of severe allergies or significant skin conditions.
- You suspect exposure was heavy, like camping, yard clearing, or burning brush.
- There is fever, rapidly increasing pain, or a child who seems sicker than “just a rash.”
Go to urgent care or emergency care now if:
- Your child has trouble breathing, wheezing, throat tightness, drooling, or trouble swallowing.
- There is severe facial swelling or eye swelling affecting vision.
- You think your child inhaled smoke from burning poison ivy/oak/sumac. Inhaled urushiol can irritate the airways and can be serious.
- Your child looks very ill, is very sleepy and hard to wake, or has signs of dehydration.
Signs it may be infected
Scratching can break skin, and then bacteria can move in. Call your pediatrician if you see:
- Increasing redness, warmth, swelling around the rash
- Pus or thick yellow drainage
- Honey-colored crusting
- Fever or worsening pain
- Red streaks spreading away from the rash
How long it lasts
Most poison plant rashes peak around days 3 to 5 and improve over 1 to 3 weeks, depending on exposure and your child’s sensitivity.
- New spots can show up for days. That does not automatically mean it is spreading person-to-person.
- Oozing can happen. Clear fluid from blisters is common. Keep it clean and avoid popping blisters.
- Skin may look darker or lighter as it heals. Post-inflammatory color change is common and fades with time.
When steroids are needed
Some kids need prescription treatment, especially if the rash is widespread, very swollen, or on the face or genitals. Your pediatrician may prescribe a stronger topical steroid or, for more severe cases, an oral steroid with a specific plan and taper.
- Do not use leftover oral steroids from an old prescription. The dose and length matter for this type of rash.
If the rash is not improving after about a week, or it is getting worse instead of better, it is worth checking in.
Preventing the next round
Prevention is partly plant know-how and mostly boring, practical routines.
Simple habits
- Long sleeves and pants for wooded trails and yard edges.
- Shoes, not sandals, in brushy areas.
- Teach “leaves of three, let it be” for poison ivy and oak. (Poison sumac often has more leaflets, commonly 7 to 13, and is frequently found in wetter areas, depending on region.)
- Wash hands right after outdoor play, especially before snacks.
- Rinse gear like baseball gloves, shin guards, and garden tools if they were in brush.
Optional: barrier products
For older kids doing yard work, hiking, or camp, a barrier lotion designed for poison ivy (for example, bentoquatam) can help prevent urushiol from reaching the skin. Use only as directed, and remember it does not replace washing and changing clothes after exposure.
A quick reality check
Even careful families get poison ivy. Kids are basically magnets for the exact patch of weeds you hoped they would not touch. The win is knowing what to do early, so the rash stays as small and manageable as possible.

Fast checklist
- Suspected exposure: rinse, then wash with soap and water. Clean under nails.
- Wash the sources: clothes, shoes, gear, and pets.
- Itch relief: cool compresses, oatmeal bath, calamine, thin layer of 1% hydrocortisone on appropriate areas, and consider an age-appropriate antihistamine for sleep if needed.
- Call the pediatrician: face, eyes, genitals, widespread rash, severe swelling, fever, worsening pain, or signs of infection.
- Go now: breathing trouble or smoke inhalation exposure.
Quick medical note
This article is for general education and does not replace medical care. If you are worried about your child’s symptoms or you are not sure what you are seeing, trust that instinct and call your pediatrician.