Postpartum Preeclampsia: High Blood Pressure After Birth
Sarah Mitchell
Sarah Mitchell is a Registered Pediatric Nurse and a mother of three who has spent over a decade helping families navigate the beautiful, chaotic early years of childhood. She combines evidence-based medical knowledge with real-world parenting experience to offer practical, compassionate advice. At Awesome Parent, Sarah's mission is to help exhausted parents find solutions, trust their instincts, and finally get some sleep.
Most parents expect the tough stuff to happen during pregnancy and delivery. Then the baby arrives, you go home, and everyone assumes the danger zone is over. But there is one postpartum complication I always want families to have on their radar: postpartum preeclampsia.
It can show up after birth, even if your blood pressure was normal during pregnancy. And the tricky part is that early symptoms can masquerade as “normal new parent life” like headaches, swelling, and exhaustion.
If you are reading this at 3 AM with a pounding head and that nagging feeling that something is off, I want you to have clear, calm guidance on what matters, what to watch, and when to go in.

What is postpartum preeclampsia?
Preeclampsia is a condition involving high blood pressure and signs that organs like the liver, kidneys, brain, or blood-clotting system are under stress. When it happens after delivery, it is called postpartum preeclampsia.
It usually shows up in the first week after birth (many clinicians see a lot of cases in the first several days after discharge), but it can occur up to 6 weeks postpartum. Postpartum blood pressure also commonly peaks around days 3 to 6, which is one reason symptoms can show up “out of nowhere” after you get home. It can happen after a vaginal birth or C-section, and it can affect people who never had high blood pressure before.
Why it matters
Untreated postpartum preeclampsia can become severe quickly and may lead to complications like stroke, seizures (eclampsia), fluid in the lungs, liver injury, or other serious issues. The good news is that when it is recognized early, treatments are very effective.
Common signs and symptoms
Postpartum recovery is uncomfortable, and many symptoms are common and harmless. Postpartum preeclampsia is different because it tends to involve symptoms that feel intense, unusual for you, worsening, or not relieved by usual remedies.
Key warning signs
- Severe headache that is new, persistent, or does not improve with rest, hydration, caffeine, or typical medication your provider says is safe
- Vision changes such as blurry vision, flashing lights, seeing spots, or temporary loss of vision
- Right upper abdomen pain (under the right ribs) or upper abdominal pain that feels sharp, intense, or new
- Nausea or vomiting that is new after you were already starting to feel more stable
- Shortness of breath, chest tightness, or feeling like you cannot get a full breath
- Sudden swelling of face or hands, or rapid swelling that seems to appear quickly
- Rapid weight gain over 1 to 2 days that feels out of proportion (this is supportive context, not a stand-alone sign)
- High blood pressure readings at home or at a visit
Some people describe a general sense of doom or feeling “weird” or “off.” That feeling is nonspecific, and it is not diagnostic by itself, but as a triage nurse I learned to respect that instinct. If you feel like something is wrong, it is worth a call, especially if it is paired with any of the symptoms above.

Normal recovery or a red flag?
After birth, headaches and swelling can happen for plenty of non-emergency reasons: sleep deprivation, dehydration, hormone shifts, tension, caffeine withdrawal, anemia, and the physical aftermath of labor.
Here is the difference I teach families to look for.
Routine postpartum discomfort often looks like:
- A headache that improves with water, food, rest, and provider-approved pain relief
- Mild swelling in feet and ankles that slowly improves over days
- Feeling worn down but still able to have moments of relief
Postpartum preeclampsia concerns look more like:
- A headache that is severe, new, or not improving
- Headache plus vision changes or right upper abdomen pain
- Swelling that is sudden or involves the face and hands
- Symptoms that are escalating, not trending better
- High blood pressure readings, especially when paired with symptoms
One practical way to think about it: postpartum fatigue is miserable, but it is usually predictable. Postpartum preeclampsia can feel like your body is throwing up red flags you cannot ignore.
Blood pressure numbers
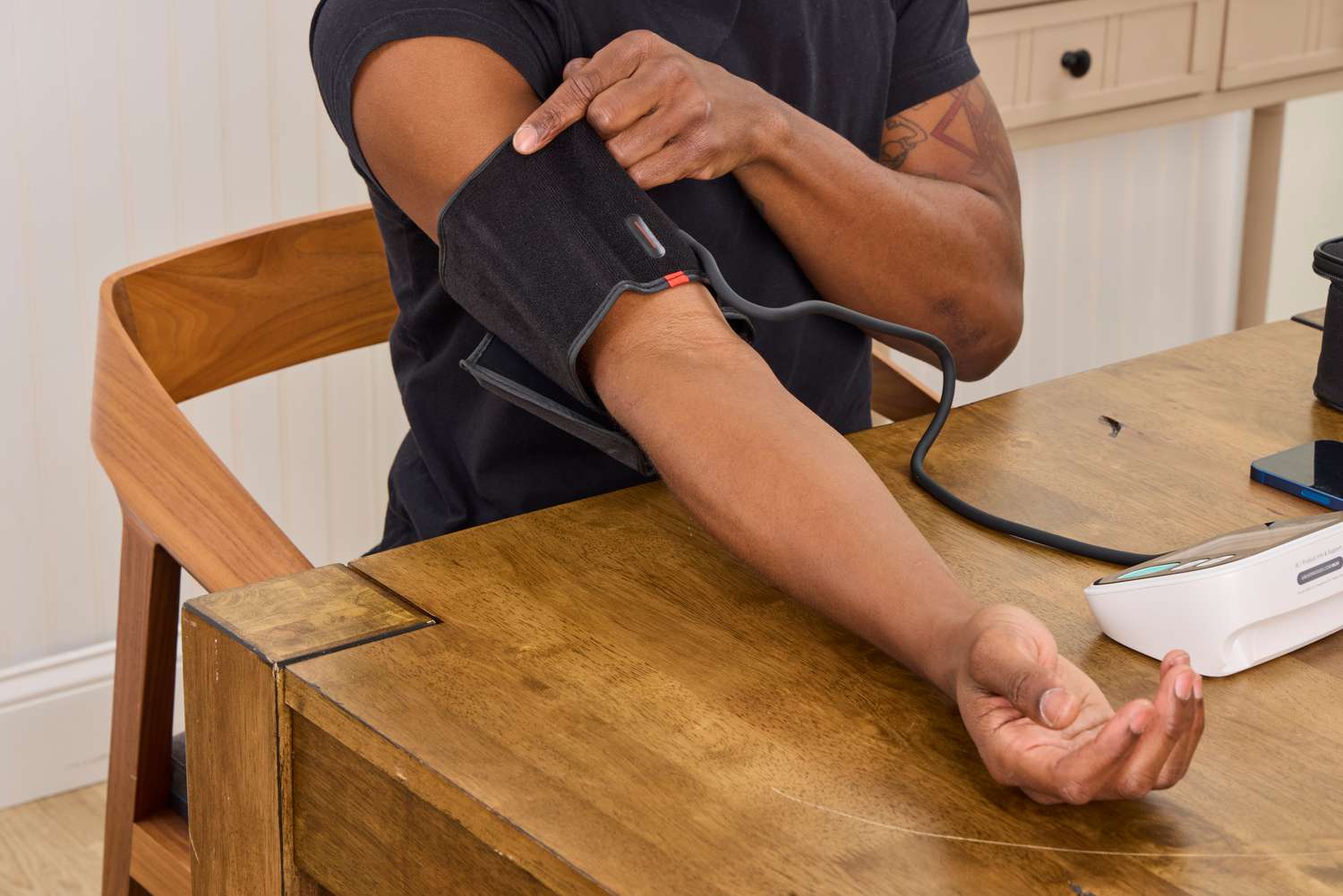
If your care team asked you to check blood pressure at home, those numbers are important. If you have a home cuff, use an upper arm cuff (more accurate than a wrist cuff for most people) and take readings when you have been sitting quietly for about 5 minutes.
One detail that matters more than people realize: cuff size and fit. A cuff that is too small can read falsely high, and a cuff that is too big can read falsely low. Use the size recommended for your arm circumference if you can.
Call your provider urgently (or follow their plan) if:
- Your blood pressure is 140/90 or higher on repeat readings, especially if you have symptoms
Get emergency care now if:
- Your blood pressure is 160 systolic or 110 diastolic or higher, even once, or you have severe symptoms regardless of the number
If you get a severe-range number (160/110 or higher), many protocols suggest a quick repeat after a few minutes of quiet rest, but from a patient safety standpoint I do not want you waiting around to see if it “settles.” Recheck while you are seeking urgent help, not instead of it.
If you do not have a blood pressure cuff and you have symptoms like severe headache or vision changes, do not wait to “get numbers.” Get evaluated.
When to go to the ER
I am going to be very direct here because postpartum people often minimize symptoms.
Go to the ER now (or call emergency services) for any of the following:
- Severe headache that is new or not improving
- Vision changes (spots, flashing lights, blurry vision)
- Right upper abdominal pain or severe upper abdominal pain
- Shortness of breath, chest pain, or trouble breathing
- Seizure, fainting, new confusion, or weakness on one side
- Blood pressure 160/110 or higher
If you are worried about being dismissed, use clear language: “I am postpartum and I am concerned about postpartum preeclampsia.” That phrase helps teams triage appropriately.
Quick reassurance: You are not being dramatic. You are being appropriately cautious. In postpartum care, getting checked early is almost always easier than trying to catch up later.
Who is at higher risk?
Postpartum preeclampsia can happen to anyone, but risk is higher if you have or had:
- Preeclampsia or gestational hypertension during pregnancy
- Chronic high blood pressure
- Diabetes, kidney disease, or autoimmune conditions
- Multiple gestation (twins or more)
- Obesity
- A history of preeclampsia in a previous pregnancy
- Age 35 or older (risk increases with age)
That said, I have cared for plenty of postpartum parents who had no obvious risk factors. So please do not use “I was low risk” as a reason to ignore symptoms.
What to expect if you are evaluated
One of the scariest parts is not knowing what will happen once you go in, especially if you are breastfeeding, recovering from birth, and worried about your baby at home. Here is what evaluation commonly includes:
- Blood pressure checks repeated over time
- Urine testing (protein can be a clue)
- Blood tests to look at liver function, kidney function, and platelets
- Assessment of symptoms like headache and vision changes
- Sometimes imaging or additional tests if there are neurologic symptoms or breathing issues
Also, not every scary postpartum headache is preeclampsia. Postpartum headache can have other urgent causes (for example: a post-dural puncture headache after an epidural, blood clots, infection). The takeaway is the same: do not self-diagnose at home. Get evaluated.
Treatment basics
Treatment depends on severity, but may include:
- Blood pressure medications (many are compatible with breastfeeding, and your team will choose what fits your situation; common examples include labetalol and nifedipine)
- Magnesium sulfate in the hospital to prevent seizures in severe cases
- Close monitoring and a follow-up plan for blood pressure checks
If you need hospital care, it is okay to ask: “Can my baby stay with me if I am stable?” Many units can accommodate rooming-in or supportive visitation, depending on hospital policy and your condition.

Home blood pressure routine
If your provider recommended monitoring at home, here is a straightforward routine I often suggest:
- Check at the same times daily for consistency, often morning and evening
- Sit with feet on the floor, back supported, arm at heart level
- Avoid caffeine, nicotine, or exercise for about 30 minutes beforehand if possible
- Take two readings 1 minute apart and record the lower one or the average, based on your provider’s guidance
- Write down symptoms with the reading, especially headache or vision changes
If numbers are rising or you feel worse, do not try to “out-monitor” the problem. Call.
Anxiety vs preeclampsia
This is important, especially for postpartum parents who have been told, “It’s probably just anxiety.”
Postpartum anxiety can cause physical symptoms like racing heart, shakiness, nausea, chest tightness, and insomnia. Postpartum preeclampsia is a medical condition involving blood pressure and organ stress.
They can also overlap. Feeling anxious because you have a severe headache is a normal response. And having postpartum anxiety does not protect you from medical complications.
If you are unsure which bucket your symptoms fall into, choose the safer option: get checked, especially if you have severe headache, vision changes, right upper abdominal pain, shortness of breath, or high blood pressure readings.
Questions parents ask
Can postpartum preeclampsia happen if my pregnancy blood pressure was normal?
Yes. It can appear for the first time after delivery.
Can it happen weeks after birth?
Yes. It is most common in the first week, but it can occur up to about 6 weeks postpartum. If you have concerning symptoms at any point in that window, get advice promptly.
Is swelling always a sign?
No. Some swelling is common postpartum. What raises concern is sudden swelling, swelling of the face and hands, or swelling plus other symptoms like headache or vision changes.
Will I need to stop breastfeeding if I need treatment?
Usually, no. Many blood pressure medications used postpartum are compatible with breastfeeding, and magnesium sulfate is commonly used while patients continue pumping or feeding with support. Always confirm with your care team and pediatrician, but do not assume you must stop.
If you only remember one thing
Postpartum preeclampsia is not rare enough to ignore, and it is not subtle enough to “push through” when it turns severe.
Severe headache, vision changes, right upper abdominal pain, shortness of breath, or blood pressure 160/110 or higher are emergency signs. You deserve prompt care, and getting evaluated is the responsible choice for you and your baby.
If you are worried and you want a script for calling: “Hi, I am postpartum and I have symptoms that concern me for postpartum preeclampsia. I have a severe headache and my blood pressure is ____. What should I do right now?”
And one last practical note: if your clinician set up an early postpartum blood pressure check (often within the first 3 to 10 days for people with risk factors), keep that appointment and follow their individualized plan. If you feel worse before then, do not wait for the visit.