Psoriasis in Kids: Plaques, Scalp Signs, and Eczema Look-Alikes
Sarah Mitchell
Sarah Mitchell is a Registered Pediatric Nurse and a mother of three who has spent over a decade helping families navigate the beautiful, chaotic early years of childhood. She combines evidence-based medical knowledge with real-world parenting experience to offer practical, compassionate advice. At Awesome Parent, Sarah's mission is to help exhausted parents find solutions, trust their instincts, and finally get some sleep.
If you are staring at a stubborn patch on your child’s skin and thinking, “Is this eczema… or something else?”, you are not alone. In my own pediatric triage work, psoriasis was a rash I saw get mislabeled more than once, especially when it showed up on the scalp or in skin folds.
Psoriasis in children is very real, very manageable, and very often mistaken for eczema, dandruff, fungus, or “just dry skin.” Let’s walk through what it typically looks like, where it likes to live on kids, how itching usually behaves, and when it is worth getting dermatology involved.
Quick note: This is educational and parent-focused, not a diagnosis. If you are unsure what you are looking at, getting the right eyes on it can save a lot of trial and error.

What it is
Psoriasis is a chronic inflammatory skin condition where the immune system tells the skin to grow and shed too quickly. Instead of a smooth “turnover,” skin cells stack up, creating thickened areas that look scaly.
It is not contagious. Your child did not “catch” it from another kid, a pool, or a pet.
Psoriasis tends to come and go. Many families notice flare-ups with certain triggers, then calmer stretches where the skin looks much better.
What it looks like
The most common type overall is plaque psoriasis (raised patches), though guttate psoriasis is also relatively common in children, often after strep.
Typical features
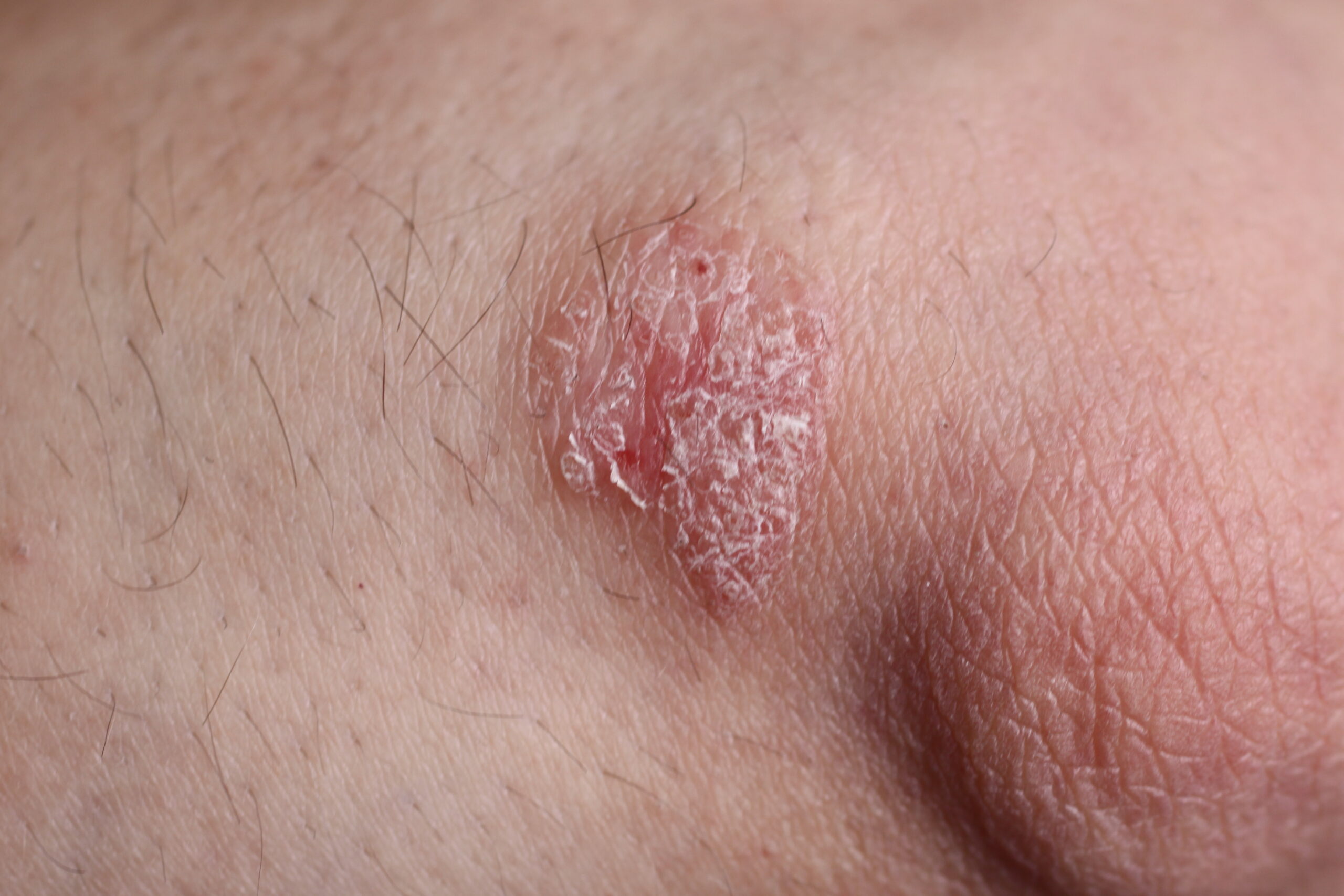
- Well-defined patches: edges are often sharp and easy to trace with your eyes.
- Pink to red skin underneath (or darker, violaceous, or brownish tones on deeper skin tones).
- Dry scale that can look silvery-white or flaky.
- Thicker feel than the surrounding skin, sometimes described as “stuck on.”
In children, plaques can be thinner and less scaly than in adults, which is one reason it gets mistaken for eczema.
Common spots
Psoriasis has favorite hangouts. If a rash keeps returning to these areas, it nudges psoriasis higher on the list.
- Scalp: thick scale, patches at the hairline, or “dandruff” that does not respond to typical dandruff shampoo.
- Elbows and knees: classic locations, even in kids.
- Behind the ears: especially along the crease and hairline.
- Lower back: sometimes small plaques near the waistband.
- Skin folds (inverse psoriasis): armpits, groin, belly button, between buttocks. In folds it may look more shiny and red with less visible scale.
- Nails: pitting (tiny dents), thickening, or lifting from the nail bed can happen.
One important note: babies and toddlers can get psoriasis in the diaper area. It can look like a bright, stubborn diaper rash that keeps coming back despite “doing everything right.” It can also mimic irritant diaper dermatitis and yeast, so persistent rashes in that zone are worth a closer look.
If psoriasis runs in the family, that detail can be a helpful clue. Not required, but helpful.
Scalp: psoriasis vs dandruff
The scalp is where things get confusing fast, because seborrheic dermatitis (cradle cap in babies, dandruff in older kids) is common and can overlap with psoriasis.
Clues for scalp psoriasis
- Thicker, drier scale that clings to the scalp and hair.
- Well-demarcated patches, often extending beyond the hairline (onto the forehead, behind ears, or neck).
- Other psoriasis spots elsewhere, like elbows, knees, belly button, or nails.
- Persistent recurrence even with good basic dandruff care.
Clues for seborrhea
- Greasier, yellowish scale.
- Less sharply defined redness.
- More diffuse involvement (not as patchy).
And yes, there is a well-known overlap pattern sometimes called sebopsoriasis, especially around the scalp and face. This is one of those times when a dermatologist’s eyes can shorten the trial-and-error period.
Psoriasis vs eczema
Eczema (atopic dermatitis) and psoriasis can both cause red, irritated skin. But they often behave a little differently.
Edges and texture
- Psoriasis: more likely to have clear edges, a thicker “plaque” feel, and dry scale that can look silvery or powdery.
- Eczema: often has blurrier edges, looks more like a patch of irritated dry skin, and can ooze or crust when flared.
Common locations
- Psoriasis: scalp, elbows, knees, behind ears, belly button, lower back, folds.
- Eczema: often the cheeks and outer surfaces in babies, then more commonly the creases (inside elbows, behind knees, wrists, ankles) in older kids.
Itch patterns
Both can itch. But in many kids:
- Eczema tends to be intensely itchy, the kind that keeps kids up at night and leads to a scratch cycle.
- Psoriasis may itch, sting, or feel sore, but sometimes it is more “annoying” than relentlessly itchy. Some kids report burning or tightness.
There is plenty of overlap, so if you are thinking, “This doesn’t fit neatly,” you are probably not doing anything wrong. Skin loves to be complicated.
Other patterns
Guttate psoriasis
This form can pop up after a sore throat or strep infection. It looks like many small, drop-shaped pink spots across the trunk and limbs.
If your child develops a sudden “sprinkling” of spots after fever or throat pain, it is worth asking your pediatrician about strep testing. Treating strep matters for overall health, and may help the skin in some cases, but the rash does not always quickly clear just because antibiotics were started.
Inverse psoriasis
This shows up in folds and can look like a smooth, shiny red rash. Because folds are moist, the classic silvery scale may be minimal. It is frequently mistaken for yeast.
Common triggers
Triggers are not the same for every child, and you do not have to become a full-time rash detective. But these are common ones:
- Infections (especially strep throat)
- Skin injury like scratches, friction, sunburn, or bug bites (new plaques can appear where skin was irritated). This is called the Koebner phenomenon.
- Cold, dry weather
- Stress (including big transitions, school changes, family stress)
- Some medications (your clinician can review this if needed)
If you notice a repeat pattern, jot it in your phone notes. That small detail can be very helpful at appointments.
How it is diagnosed
Most of the time, psoriasis is diagnosed by history and a skin exam.
Sometimes clinicians will do a quick test to rule out look-alikes, especially in kids, for example:
- Fungal infections (tinea corporis on the body, tinea capitis on the scalp) can mimic psoriasis or eczema. A scraping for a KOH test or a fungal culture may be used when the pattern suggests it.
- Yeast in folds can look similar to inverse psoriasis.
- Nail fungus or trauma can also mimic psoriasis-related nail changes.
A skin biopsy is rarely needed in children, but it can be done when the diagnosis is still unclear.
Gentle care basics
Psoriasis treatment is different from eczema in some key ways, so I am not going to recycle an eczema routine here. Instead, these are psoriasis-friendly basics that support the skin barrier and reduce unnecessary irritation.
Bathing and moisturizing
- Short, lukewarm baths or showers. Hot water tends to inflame and dry.
- Use a mild, fragrance-free cleanser on dirty areas only. You do not need to soap the whole child daily.
- Moisturize after bathing while skin is still slightly damp. Thick, fragrance-free creams or ointments are usually best tolerated.
Scale care
It is tempting to lift scale, especially on the scalp. Try not to pick. Picking can lead to skin injury, bleeding, and sometimes more psoriasis in that spot.
- For thick body plaques, a longer soak plus moisturizer can help soften scale.
- For scalp scale, gently loosening with a soft brush after softening (as advised by your clinician) is usually safer than scraping.
Clothing and friction
- Soft, breathable fabrics (cotton is a classic for a reason).
- Avoid tight waistbands or scratchy seams over plaques when possible.
Sun
Some kids improve with careful sun exposure, but sunburn is a known trigger. Stick with sun protection and ask dermatology before intentionally using sun as a treatment strategy.
When to get help
As a triage nurse, this is the part I cared about most: getting you to the right level of help without unnecessary panic.
Make an appointment soon if:
- The rash is not improving after 1 to 2 weeks of gentle skin care, or it is worsening, spreading, or clearly needs more than over-the-counter care.
- You see thick scalp scale or patches at the hairline plus plaques elsewhere.
- Your child has recurrent “yeast” rashes in folds or diaper area that do not behave like yeast.
- There are nail changes (pitting, thickening, lifting).
- The rash is affecting sleep, school, sports, or self-esteem.
Ask for dermatology referral if:
- Diagnosis is unclear (eczema vs psoriasis vs seborrhea overlap, or concern for fungus).
- Lesions are on the face, genitals, or large body areas.
- There are frequent flares or you need more than basic measures to keep it controlled.
Seek urgent care today if:
- Your child has fever and looks ill with a rapidly worsening rash.
- Skin is very painful, blistering, or peeling.
- There are signs of skin infection: increasing warmth, swelling, pus, or rapidly spreading redness.
Psoriasis itself is not usually an emergency, but kids can get secondary infections from scratched or broken skin, and that part deserves quick attention.
Psoriatic arthritis
A small number of children with psoriasis develop joint inflammation called psoriatic arthritis. Most kids with psoriasis will never deal with this, but it is important to recognize early.
Call your pediatrician if your child has psoriasis plus:
- Persistent joint pain or morning stiffness
- Swollen fingers or toes (sometimes “sausage-like”)
- Limping, refusing to bear weight, or new trouble with stairs
If you are seeing this, you are not being dramatic by asking for evaluation.
Treatment options
Treatment depends on your child’s age, where the plaques are, and how much skin is involved. Dermatology often uses a stepwise approach, such as:
- Targeted prescription topicals to calm inflammation and slow overgrowth in plaques
- Scalp-specific options if the scalp is a main site
- Phototherapy for more widespread disease in some cases
- Systemic medications (including newer biologics) for moderate to severe cases, when appropriate
Many of these treatments are very effective, but they are also age and location specific. In children especially, topical steroids, vitamin D analogs, and other prescription medications should be used with clinician guidance so the strength, duration, and application sites are safe.
If you are nervous about the word “chronic,” I get it. Chronic does not mean hopeless. It usually means you and your care team are aiming for control, fewer flares, and a plan you can actually follow in real life.
Whole-child check-in
This is not meant to be alarming, just grounding: psoriasis can affect more than skin. Some children with psoriasis have higher rates of stress, anxiety, low mood, or body confidence struggles. In some kids, clinicians also keep an eye on healthy growth habits and weight because inflammation and lifestyle factors can travel together.
If your child seems withdrawn, irritable, or is avoiding activities they used to love, that is a valid reason to bring it up. It counts as “medical,” too.
For tired parents
Psoriasis can be stubborn. It can also be incredibly responsive once the diagnosis is correct and the plan matches the pattern of your child’s skin.
If you have been treating “eczema” for months and nothing adds up, it is okay to ask, “Could this be psoriasis?” That is not second-guessing your pediatrician. That is advocating for your kid, and it is exactly what good parents do at 3 AM with a worried heart and a phone flashlight.