Pyloric Stenosis in Babies: Projectile Vomiting and When to Go to the ER
Sarah Mitchell
Sarah Mitchell is a Registered Pediatric Nurse and a mother of three who has spent over a decade helping families navigate the beautiful, chaotic early years of childhood. She combines evidence-based medical knowledge with real-world parenting experience to offer practical, compassionate advice. At Awesome Parent, Sarah's mission is to help exhausted parents find solutions, trust their instincts, and finally get some sleep.
If your baby is suddenly vomiting with surprising force, it can feel like your brain flips into emergency mode. As a pediatric nurse and a mom who has cleaned more milk off more surfaces than I care to admit, I want you to know two things can be true at once: most spit-up is harmless, and classic projectile vomiting in a young baby is something you should take seriously.
Pyloric stenosis is one of those conditions where early recognition matters. The good news is that it is very treatable, and most babies do beautifully once they get the right care.
What pyloric stenosis is (plain English)
At the bottom of the stomach there is a small muscular “gate” called the pylorus that opens to let feeds pass into the small intestine. In pyloric stenosis, that muscle becomes abnormally thick and tight. As it tightens, feeds cannot move forward like they should.
So the stomach does what stomachs do when they cannot empty: it squeezes harder. That is why the vomiting becomes forceful and progressive.
When it usually shows up: most commonly between 2 and 8 weeks old (often around 3 to 6 weeks), and it is less common in older infants.
Classic signs parents notice at home
Pyloric stenosis has a pretty recognizable pattern. Not every baby has every sign, but these are the “classic” clues:
- Vomiting that becomes more forceful over time, often described as projectile (it shoots out rather than dribbles).
- Vomiting soon after feeds (often within 30 to 60 minutes), especially after the baby seemed to feed normally.
- Vomit is typically non-bilious, meaning it is usually not green. (Bright green vomit is a different emergency red flag, listed below.)
- Hungry again right after vomiting. Parents often say, “They throw up and then act starving.”
- Fewer wet diapers or smaller amounts of urine.
- Fewer stools or constipation.
- Weight loss or poor weight gain.
- Fussiness that can look like hunger or discomfort.
Some families also notice a baby’s stomach looks like it is “working hard” after a feed, with visible waves of movement across the upper belly.
Pyloric stenosis vs reflux vs stomach bug
In triage, the story matters as much as the vomiting itself. Here is how pyloric stenosis tends to differ from two common look-alikes.
Reflux (spit-up)
- Typical pattern: small to moderate spit-ups, often effortless, sometimes with burping or when lying flat.
- Growth: many babies with reflux still gain weight well.
- Course: may come and go, not usually a steady progression to more and more forceful vomiting.
- Hunger after: can be normal either way.
Stomach bug (viral gastroenteritis)
- Typical pattern: vomiting plus other illness signs such as fever, diarrhea, sick contacts, or a sudden start in an older baby.
- Course: tends to be more abrupt, then improves over a couple of days.
- Important note: true “stomach bugs” are less common in newborns, and vomiting in very young babies (with or without diarrhea) deserves prompt medical advice.
Key takeaway: Pyloric stenosis is often described as progressive and feed-related, with vomit that is usually not green. Reflux is usually more “spitty.” A stomach bug often comes with other infection symptoms and a different timeline.
Go to the ER now or call 911
If you are seeing signs that your baby is dehydrated or not acting like themselves, do not wait for a routine appointment.
Go to the ER now
- Projectile vomiting in a young baby, especially if it is happening repeatedly or getting worse.
- Significantly fewer wet diapers than usual. As a general guide, no wet diaper for about 6 to 8 hours in a young baby is concerning.
- Dry mouth, no tears when crying, or a sunken soft spot (fontanelle).
- Baby cannot keep feeds down or vomits most feeds.
- Green (bright green) vomit or vomit with blood.
- Weight loss, very poor feeding, or you are worried your baby is not gaining.
Call 911
- Severe lethargy (hard to wake, floppy, not responding normally).
- Breathing trouble, bluish color, or repeated choking with vomiting.
- Signs of shock like very pale or cool skin, extreme weakness, or you feel your baby is dangerously unwell.
If you are on the fence, it is okay to trust your instincts. A quick evaluation is never “overreacting” when the concern is dehydration or a surgical condition.
What doctors look for
When pyloric stenosis is on the list, the medical team focuses on three things: your baby’s story, hydration status, and confirming the diagnosis safely.
1) History and exam
You will be asked about:
- When the vomiting started and whether it is getting worse
- How often your baby vomits and how forceful it is
- Wet diapers, stools, and weight changes
- Feeding volume and whether baby seems hungry after vomiting
On exam, clinicians look for dehydration and may feel the upper belly. Sometimes a small firm “olive-like” lump can be felt in the upper abdomen, but it is not always detectable.
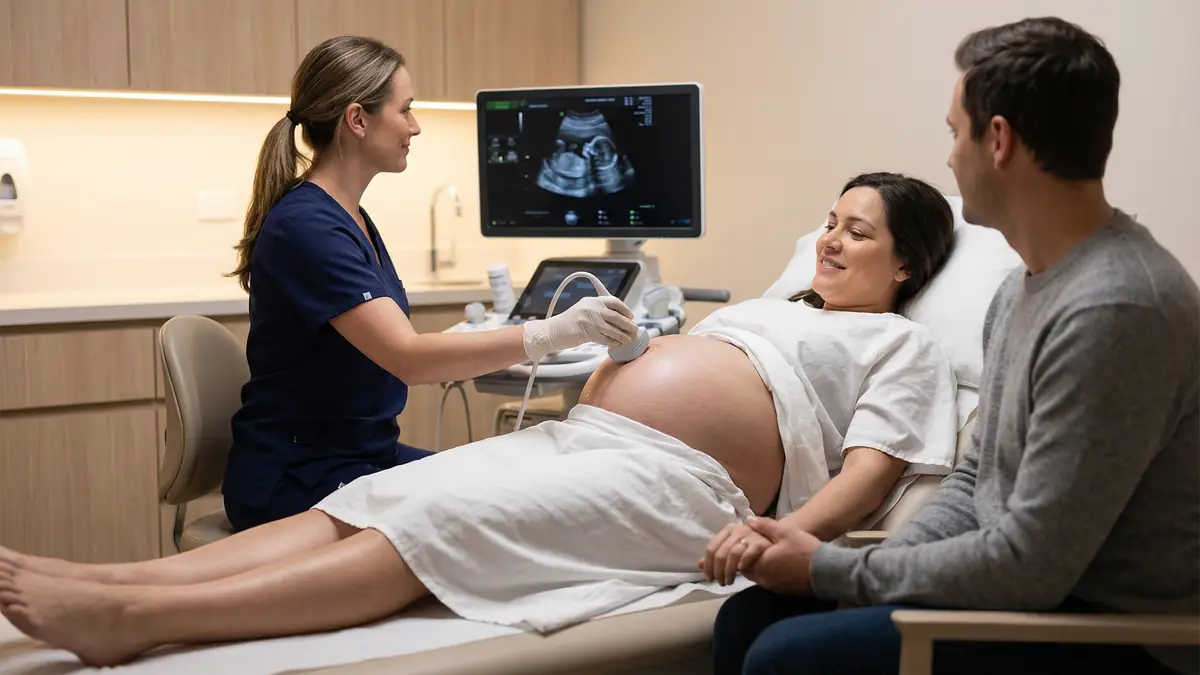
2) Ultrasound
The most common test is an abdominal ultrasound. It is painless, does not use radiation, and can usually show whether the pylorus muscle is thickened and blocking stomach emptying.
3) Bloodwork (sometimes)
If vomiting has been going on long enough, babies can get dehydrated and their salt balance can get off. In simple terms, too much vomiting can throw off electrolytes, which can make babies feel weak, extra sleepy, or just not themselves. Blood tests help guide safe rehydration before treatment.
4) Another imaging test (sometimes)
If the ultrasound is not clear, the team may order an upper GI series to look at how fluid moves through the stomach and intestine.
Risk factors (quickly)
Pyloric stenosis can happen in any baby, but it is seen more often in boys (especially firstborn boys) and in babies with a family history. Some studies have found an association with early exposure to certain antibiotics (macrolides like erythromycin or azithromycin). That does not mean an antibiotic “caused” it in any one baby, but it is worth mentioning to your clinician if it applies.
Treatment and outlook
Pyloric stenosis is treated with a routine surgery called a pyloromyotomy. It is done under general anesthesia. The surgeon splits the overgrown muscle so the passage can open and feeds can move through normally.
What typically happens first
- IV fluids to correct dehydration
- Sometimes electrolyte correction (salt balance) before surgery
- Your baby may need to pause oral feeds for a period while the team prepares
After surgery
- Most babies start back on small feeds fairly soon, per hospital protocol.
- Some spit-up or small vomits can still happen during the first day or two as the stomach settles. The pattern should improve, not worsen.
- Many babies go home within 1 to 2 days, depending on feeding and hydration.
Long-term outlook: excellent. Once fixed, pyloric stenosis usually does not come back, and babies typically go on to feed and grow normally.
What to do while heading in
If you suspect pyloric stenosis and you are going to urgent care or the ER:
- Do not force extra feeding to “make up” for the vomit.
- If your baby is having repeated projectile vomiting, it is usually best to avoid more oral feeds while you are on the way in, unless a clinician tells you otherwise. (This helps lower choking risk and keeps the focus on getting evaluated and hydrated.)
- Bring details: when it started, how many episodes in 24 hours, wet diapers, stool frequency, and any weight checks you have.
- Bring a change of clothes for baby and you. Not because you did anything wrong, but because vomiting babies are extremely committed.
Common questions
Can pyloric stenosis be mistaken for reflux?
Yes, especially early on. The clue is the trend: pyloric stenosis typically becomes more frequent and more forceful, and babies often stay very hungry after vomiting.
Is projectile vomiting always pyloric stenosis?
No. Other conditions can cause forceful vomiting. But in a young baby, projectile vomiting is a big enough red flag that it should be evaluated promptly.
What if my baby vomits once like a fountain, then seems fine?
One episode can happen for lots of reasons. But if your baby is in the common age range and you see repeat forceful vomiting, decreasing wet diapers, or that “vomit then immediately hungry” pattern, get checked.
Bottom line
Pyloric stenosis is a treatable cause of vomiting in young babies, and it often shows up as progressive, forceful vomiting after feeds with a baby who still seems hungry. Vomit is usually not green, so bright green vomit is an emergency that should be evaluated right away.
If your baby is showing signs of dehydration, lethargy, green vomit, or repeated projectile vomiting, go to the ER now.
And if you are reading this at an exhausted hour with a burp cloth in one hand and your phone in the other: you are not alone. You do not need to diagnose it perfectly. You just need to get your baby evaluated when the pattern looks concerning.
Medical disclaimer
This article is for general education and is not a substitute for medical advice, diagnosis, or treatment. If you think your baby may be seriously ill or dehydrated, seek emergency care.