Raynaud’s of the Nipple While Breastfeeding
Sarah Mitchell
Sarah Mitchell is a Registered Pediatric Nurse and a mother of three who has spent over a decade helping families navigate the beautiful, chaotic early years of childhood. She combines evidence-based medical knowledge with real-world parenting experience to offer practical, compassionate advice. At Awesome Parent, Sarah's mission is to help exhausted parents find solutions, trust their instincts, and finally get some sleep.
If your nipple pain feels like a deep, burning, pins-and-needles zing that hits after a feed, and your nipple turns white, then blue/purple, then red, you are not being dramatic. You might be dealing with Raynaud’s of the nipple, also called nipple vasospasm.
In triage, this is one of those issues that often gets mislabeled, sometimes as thrush. The good news: once you recognize the pattern, small, realistic changes can bring real relief.

What Raynaud’s of the nipple is
Raynaud’s happens when tiny blood vessels clamp down too hard in response to a trigger (often cold, sometimes stress or pressure). When this happens in the nipple after breastfeeding or pumping, it can cause:
- Sudden nipple pain that is sharp, burning, or electric
- Color changes in the nipple (often a clear cycle)
- Pain that worsens with cold air, like stepping out of the shower or opening the freezer
This can occur even if you have never been diagnosed with Raynaud’s in your fingers or toes, although some parents do notice both.
The nipple color cycle
The color changes are a huge clue. Not everyone gets all three phases, but many do:
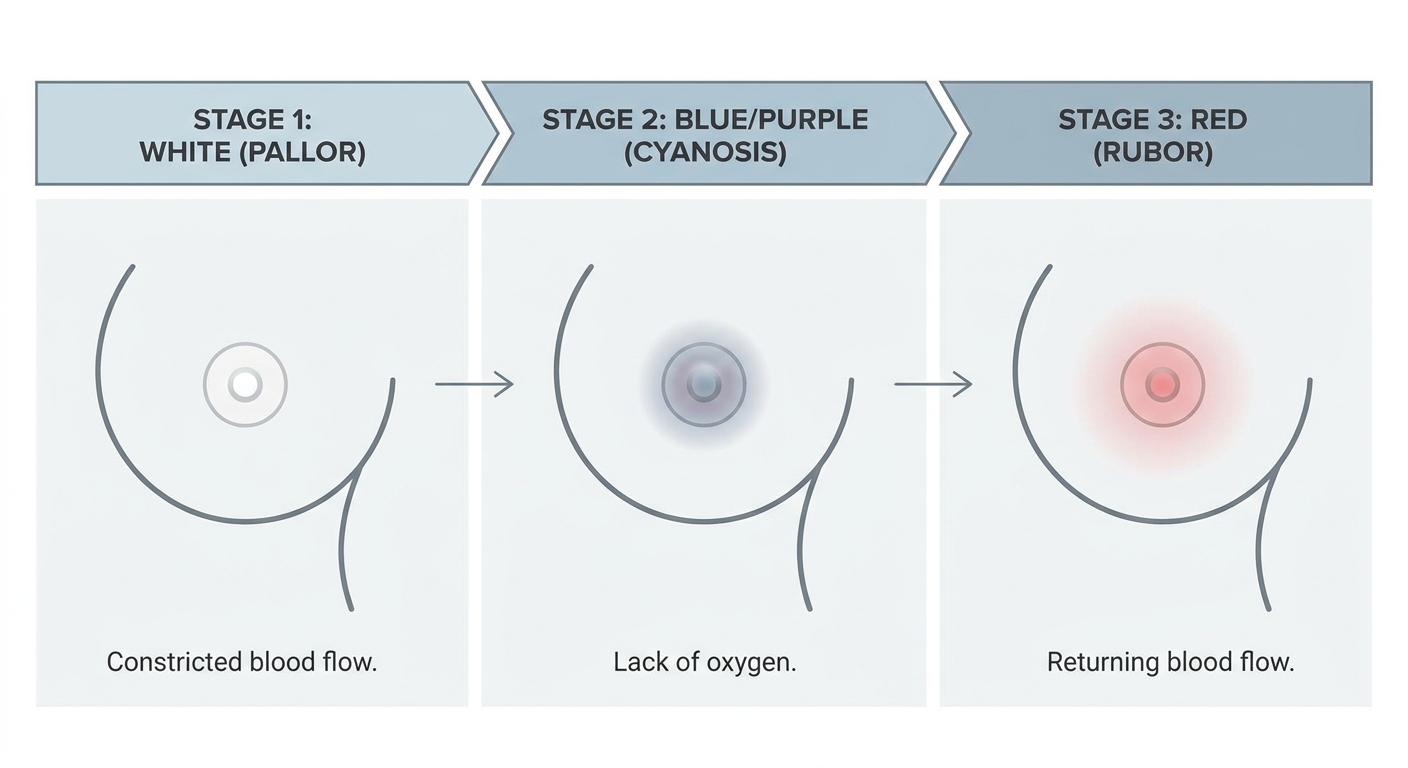
- White (blanching): Blood flow temporarily decreases. The nipple may look pale, bright white, or “drained.”
- Blue or purple: Blood returns slowly and oxygen levels are lower for a moment.
- Red: Blood flow rushes back, which can throb or burn.
That painful flare often shows up after baby unlatches or when you finish pumping. Parents will tell me, “It’s fine during the feed, then it hits me like a truck.” That timing is very Raynaud’s.
Common triggers
Vasospasm is basically your nipple’s blood vessels overreacting. Common triggers include:
- Cold exposure: air-drying nipples, cold rooms, going braless in winter, wet breast pads
- Compression or friction: shallow latch, baby sliding toward the nipple tip, tight bras, tight pump flanges
- Sudden temperature shift: warm shower to cool air, taking off a bra after a warm feed
- Stress and caffeine: not always, but they can increase vessel spasm in some people
- Systemic vasoconstrictors: nicotine and some cold medications (for example, pseudoephedrine) can make Raynaud’s worse in some people
A key point: latch issues can trigger or worsen Raynaud’s. If the nipple is being pinched, the blood vessels have an easier time clamping down afterward. The flip side is encouraging too: when compression improves, vasospasm often improves right along with it.
Relief you can try today
1) Warmth first
Warmth is the simplest, highest-payoff tool.
- Cover immediately after feeds: If cold triggers you, do not air-dry. Pat dry, then cover.
- Use a warm compress for 5 to 10 minutes after nursing or pumping.
- Keep your core warm: a cozy layer or scarf can help more than you would expect.
- Try “dry heat” in your bra: reusable hand warmers (wrapped in cloth) can be helpful for short periods.
If pain ramps up post-feed, warming the nipple right away can blunt the worst of the spasm.
Safety note: keep heat comfortably warm, not hot. Avoid falling asleep with heating pads or very hot packs against your skin (postpartum exhaustion is real, and burns are not fun).
2) Check latch and positioning
I know, I know. Everyone says “it’s the latch.” But with Raynaud’s, reducing nipple compression really matters.
- Look at your nipple shape after a feed: If it comes out flattened, creased like a new lipstick, or sharply angled, that suggests compression. Persistent blanching on one side can be a sign that something is pinching or irritating that area.
- Aim for a deeper latch: baby’s mouth wide, lips flanged, chin tucked into the breast, more areola in the mouth on the lower side.
- Try laid-back nursing: it can help baby stay deeper without sliding.
- Address tongue tie concerns thoughtfully: if latch is persistently shallow and painful despite good support, an IBCLC can help assess function.
If you have access to a lactation consultant (IBCLC), this is a great reason to book a visit. One small adjustment can make vasospasm dramatically less frequent.
3) Reduce irritants and friction
- Swap wet breast pads quickly and choose breathable materials.
- Avoid tight bras that press directly on the nipple.
- Use nipple ointment as a friction barrier if you have rubbing (plain lanolin or other breastfeeding-safe options).
If you pump
Pumping can absolutely trigger vasospasm, especially if the flange is too small or suction is cranked up to “industrial vacuum.” Consider:
- Recheck flange size: too small or too large can cause rubbing and swelling, which increases compression.
- Turn down suction: higher suction does not always equal more milk, but it often equals more trauma.
- Warm before and after pumping: a warm compress before can improve letdown, and after can help prevent the painful spasm wave.
- Consider cushion inserts if you have elastic tissue or rubbing, but make sure sizing is still correct.

Raynaud’s vs thrush vs mastitis
These can overlap, and online advice can get messy fast. Here are some practical distinguishing clues.
Raynaud’s (vasospasm) is more likely if:
- Pain is worst after feeds or after pumping
- You see white, blue, then red color changes
- Cold makes it much worse and warmth helps
- Nipple may look normal between episodes
Thrush may be more likely if:
- Pain is burning and persistent, not mainly tied to cold or post-feed timing
- You have itching or shiny, flaky skin on the areola
- Baby has white patches in the mouth that do not wipe away easily, or a beefy red diaper rash
One nuance from clinic life: thrush is commonly suspected, and yeast can absolutely happen, but nipple yeast is also sometimes overdiagnosed. Those baby signs are not definitive. If antifungal treatment is not helping within several days, it is worth revisiting the diagnosis with a clinician or lactation consultant. Dermatitis, vasospasm, and bacterial imbalance can look similar.
Mastitis needs attention if you have:
- Fever (100.4°F / 38°C or higher) or chills
- Flu-like body aches
- A hot, tender, wedge-shaped area of redness on the breast
- Rapidly worsening pain or you feel truly unwell
Call your clinician promptly for mastitis symptoms. Some cases are mostly inflammation and improve with targeted comfort measures, while others are bacterial and may need antibiotics. Your clinician can help you sort out what fits your situation.
Risk factors
You can get nipple vasospasm without any of these, but it is more common in people with a personal or family history of Raynaud’s, migraines, autoimmune disease, or nicotine exposure. Certain medications that constrict blood vessels can also play a role. If you suspect a medication trigger, check with your clinician before stopping anything.
When to contact a clinician
Please reach out if:
- Pain is severe, you are dreading feeds, or you are considering weaning because of it
- You have nipple damage that is not improving (cracks, bleeding, scabbing)
- You are not sure if it is thrush, dermatitis, trauma, or vasospasm
- You have signs of mastitis or infection (fever, worsening redness, feeling sick)
- You notice worsening swelling, pus-like drainage, or rapidly spreading redness
In some cases, if warmth and latch support are not enough, clinicians may discuss prescription options that relax blood vessels (for example, nifedipine). That is a decision to make with your provider based on your health history and breastfeeding goals.
A quick action plan
- After feeding: warm compress, cover the nipple, avoid cold air
- Within 24 to 48 hours: assess latch and nipple shape post-feed, adjust positioning
- If pumping: reassess flange fit, reduce suction, add warmth before and after
- If symptoms persist: book an IBCLC visit or clinician evaluation to rule out thrush, dermatitis, trauma, or infection
If your pain has a clear color-change pattern, you are not “just sensitive.” Your body is doing a vasospasm thing, and it deserves a practical plan, not scary internet guesses at 2 AM.
Safety note
This article is for general education and does not replace medical care. If you have fever, rapidly spreading redness, severe pain, pus-like drainage, or you feel unwell, contact your clinician or urgent care right away.