Rocky Mountain Spotted Fever in Kids
Sarah Mitchell
Sarah Mitchell is a Registered Pediatric Nurse and a mother of three who has spent over a decade helping families navigate the beautiful, chaotic early years of childhood. She combines evidence-based medical knowledge with real-world parenting experience to offer practical, compassionate advice. At Awesome Parent, Sarah's mission is to help exhausted parents find solutions, trust their instincts, and finally get some sleep.
If your child has a fever after a tick bite, your brain does what every loving parent brain does: it opens 37 tabs and imagines the worst. Let me be the steady voice here. Rocky Mountain spotted fever (RMSF) is uncommon, but it is one of the tick-borne illnesses where waiting to see can be risky. The good news is that when RMSF is recognized and treated early, kids usually do very well.
This article will walk you through what to look for, what the classic timeline really looks like, how RMSF differs from Lyme disease and everyday viral bugs, and what information to capture after a tick bite so your child’s clinician can make fast, confident decisions.
Skim-friendly takeaway: High fever plus severe headache and/or belly symptoms during tick season is worth a same-day call, even if there is no rash yet. RMSF treatment works best when started early.

What is Rocky Mountain spotted fever?
RMSF is an infection caused by a bacterium called Rickettsia rickettsii. It is spread through bites from infected ticks, most commonly the American dog tick, the Rocky Mountain wood tick, and the brown dog tick.
Despite the name, RMSF is not limited to the Rocky Mountains. In the US, it is reported most often in the Southeastern and South Central states. North Carolina, Tennessee, Missouri, Arkansas, and Oklahoma are frequently cited in public health reporting.
In kids, RMSF can start like a generic flu or stomach virus, which is why it is sometimes missed early. The key difference is that RMSF can become severe quickly without the right antibiotics.
The classic RMSF timeline in kids
Real life does not always follow textbook rules, but RMSF often has a recognizable pattern. Think in terms of days after symptoms start, not just days after the tick bite.
- Incubation (after a tick bite): Symptoms usually begin about 2 to 14 days after the bite (most often 3 to 12 days).
- Early illness (days 1 to 3 of symptoms): Sudden fever, headache, body aches, and tiredness. Many kids also have belly pain, nausea, vomiting, or diarrhea.
- Rash window (often days 2 to 5 of symptoms): Rash may appear, often around day 2 to 4, but it may start subtle, show up later, or be absent.
- Worsening risk (after day 5 of symptoms): This is the danger zone for delayed treatment. RMSF can affect blood vessels and organs, and kids can become very sick.
Important: A child can have RMSF without a known tick bite or before a rash appears. That is why clinicians are taught to treat based on suspicion and timing, not “perfect” symptoms.
Fever pattern: what parents notice
Parents often describe the fever as high and persistent, and not acting like a typical daycare cold. You might see:
- Fevers that climb quickly, often 102°F to 104°F (38.9°C to 40°C)
- Fever that keeps returning when medication wears off
- A child who looks more ill than you would expect for “just a virus”
That said, fever alone cannot diagnose RMSF. It is the combination of timing, symptoms, rash features, and exposure risk that matters.
RMSF rash: what it can look like
The RMSF rash is famous, but it is also famously inconsistent early on. Some kids never develop the classic pattern, and many have no rash in the first few days.
Typical progression
- Early: Small flat pink spots (often described as “macules”).
- Then: Spots can become raised (maculopapular).
- Later (more concerning): Spots may look red-purple and bruise-like (petechiae or purpura). This can suggest more advanced disease.
Where it often starts
Classically, the rash can begin on wrists and ankles and spread inward toward the trunk. It may involve palms and soles, which is a helpful clue, but not every child has this.
One more real-world note: In children with darker skin tones, rash can be harder to see. Sometimes what you notice first is texture change or areas that look slightly darker or “bruised.” If you are concerned, take well-lit photos for your clinician.

RMSF vs Lyme vs viral illness
Parents are often told to “watch for a bullseye” because Lyme disease gets a lot of coverage. That can accidentally steer families away from thinking about RMSF. Here are the high-yield differences.
RMSF vs Lyme disease
- Timing: RMSF symptoms usually begin within days to about two weeks after a bite. Lyme symptoms can appear 3 to 30 days after a bite, and some later symptoms occur weeks to months later.
- Rash type: Lyme is known for an expanding erythema migrans rash that often grows larger over days and may look like a target, though it can also be a uniformly red expanding patch. RMSF rash is more often multiple small spots and can become bruise-like.
- Fever feel: RMSF often causes a more intense, sudden febrile illness early on. Lyme can have fever and fatigue, but many kids with early localized Lyme primarily have the expanding rash and milder “flu-like” symptoms.
- Urgency: Both need treatment, but RMSF is the one where delaying antibiotics raises the risk of severe illness in a short timeframe.
RMSF vs a typical viral bug
- GI symptoms plus high fever: Viruses can do this, yes, but when it happens after tick exposure, it raises suspicion.
- Rash timing: Many viral rashes show up as the fever is breaking or after several days of cold symptoms. RMSF rash often shows up while the child is still quite ill with fever.
- How the child looks: This is subjective but important. RMSF kids often look “sicker than expected,” and parents are frequently right about that gut feeling.
If your child has a high fever and new rash during tick season, especially with headache or belly pain, it is worth a same-day call to your pediatrician or urgent care. If they look very ill, head to the ER.
Antibiotics: why clinicians do not wait
For RMSF, clinicians are trained to treat based on clinical suspicion. That is because early blood tests can be normal, and confirmation tests often take time.
The standard first-line antibiotic for RMSF is doxycycline, and yes, it is recommended for children of all ages when RMSF is suspected. This can surprise families because they have heard doxycycline is not for young kids. For RMSF, the benefit of prompt treatment outweighs that concern. Short courses used for suspected RMSF are considered safe, and do not cause clinically meaningful tooth staining in this setting.
Why the rush?
- Starting appropriate antibiotics early, ideally within the first 5 days of symptoms, is associated with better outcomes.
- Delays beyond day 5 are linked with a higher risk of severe disease.
- Waiting for a “classic” rash or a positive test can delay care.
What you can do: When you call, lead with the highest-value facts: fever start date, rash start date, tick exposure, and your child’s current symptoms.
Small but helpful perspective: Not all ticks carry RMSF, and not every tick that crawls on skin transmits illness. Transmission is generally more likely the longer a tick is attached, but you cannot safely rule RMSF out based on “I think it was on there briefly” if a child is now sick.
Tick removal aftercare
If you find a tick on your child, take a breath. Most tick bites do not lead to disease. But good removal and good documentation help your clinician immensely if symptoms show up later.
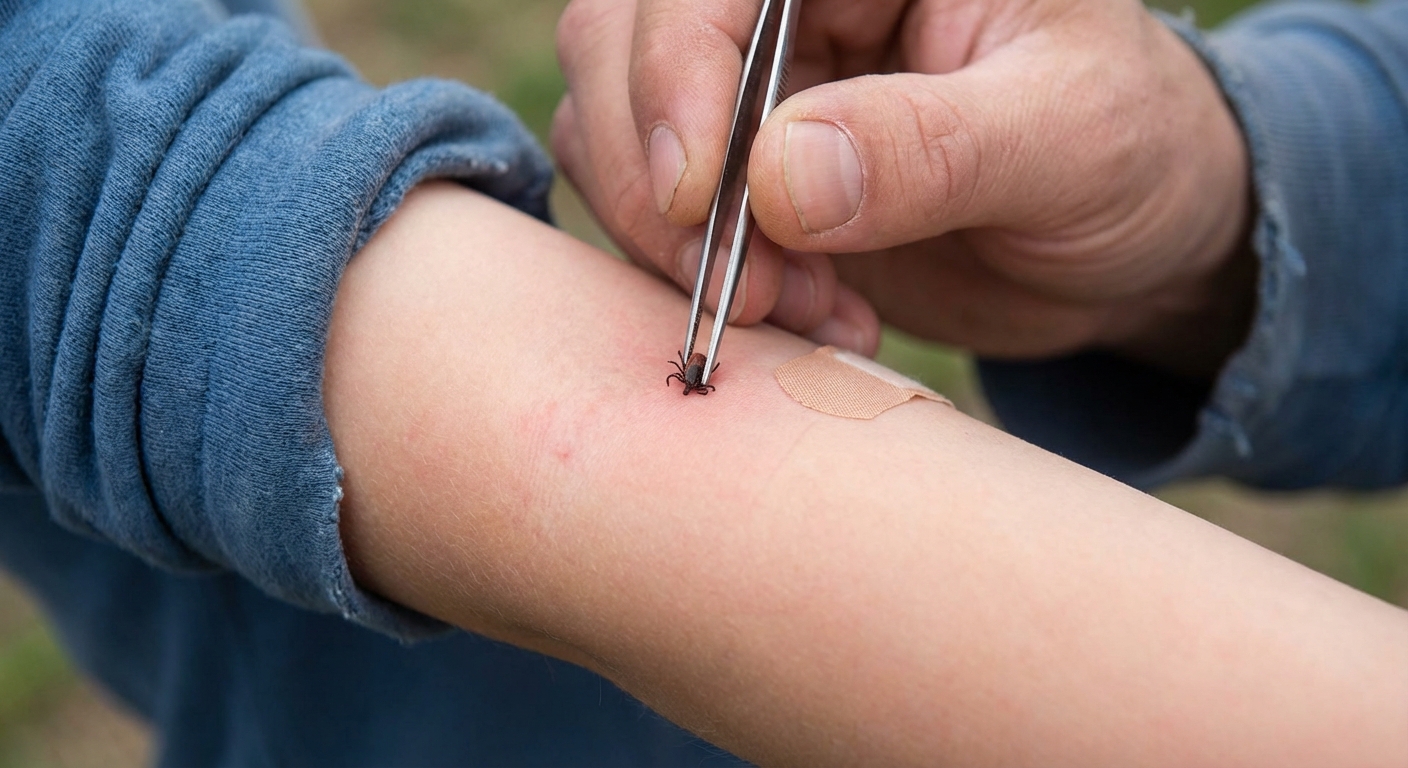
How to remove a tick safely
- Use fine-tipped tweezers.
- Grasp the tick as close to the skin as possible.
- Pull upward with steady, even pressure. Do not twist.
- If mouthparts remain, do not dig aggressively. Clean the area and let the skin heal.
- Wash the bite area and your hands with soap and water. You can also clean the skin with alcohol after removal.
What not to do
- Do not use petroleum jelly, nail polish, or heat to try to force detachment. Remove it with tweezers.
- Avoid crushing the tick with your fingers.
What to document for your clinician
In triage, the fastest visits happen when parents bring clear details. Here is what to capture after a tick bite.
- Date and approximate time you found the tick
- Where on the body (example: behind left ear, right ankle)
- Likely exposure location (backyard, hiking trail, campground)
- Was it attached? If yes, did it look flat or engorged?
- Estimated attachment time if you have any clue (example: “not there at bath last night”)
- Photo of the tick (clear, close, in good light)
- Photo of the bite site right after removal and again 24 to 48 hours later
- New symptoms with dates (fever start, rash start, headache, belly pain, vomiting)
If you can, place the tick in a sealed container or zip-top bag. Some clinics or local health departments may advise whether identification is useful in your area. Do not delay medical care for a sick child while trying to track the tick down.
When to seek urgent care or the ER
Call your child’s pediatrician the same day for guidance if your child has fever after tick exposure, especially with rash, headache, or significant fatigue.
Go to urgent care or the ER now if your child has:
- Fever plus a new rash that is spreading quickly
- Rash that looks purple, bruised, or like tiny blood spots
- Severe headache, stiff neck, confusion, extreme sleepiness, or difficulty waking
- Trouble breathing
- Signs of dehydration (very dry mouth, no tears, peeing much less)
- Persistent vomiting or severe belly pain
- A child who just looks very ill to you
Trust your instincts. Parents are often the first to notice when an illness is not following the usual script.
What testing might be done
This varies by setting and your child’s symptoms, but commonly includes:
- Blood work to look for signs of infection or inflammation
- Tests that can suggest tick-borne disease effects (like platelets and liver enzymes)
- Specific RMSF antibody testing, often as paired acute and follow-up (convalescent) tests to confirm the diagnosis
In some settings, clinicians may also use PCR testing. PCR from blood early in illness can miss cases, and PCR from a rash skin sample can sometimes be helpful when a rash is present.
Here is the frustrating part, said gently: early RMSF testing can be negative. Clinicians often start treatment first when suspicion is high.
Can RMSF be prevented?
You cannot eliminate all tick exposure if your kids go outdoors, and I would never ask you to stop letting them be kids. But you can reduce risk:
- Use an age-appropriate tick repellent as directed (your pediatrician can recommend options for your child’s age).
- Dress in long pants when hiking or in tall grass, and consider tucking pants into socks.
- Consider permethrin-treated clothing and gear (treat clothing, not skin, and follow label directions).
- Do a full-body tick check after outdoor play, especially scalp, behind ears, armpits, waistband, and behind knees.
- Shower soon after coming indoors when possible.
- Keep yards trimmed and leaf litter cleared in high-tick areas.

Quick checklist: what to say when you call
If you are calling a nurse line, pediatrician, urgent care, or the on-call provider at 2 AM, keep it simple and specific:
- My child’s fever started on: ___ (highest temp: ___)
- Rash started on: ___ (where it began: ___)
- Other symptoms: headache, belly pain, vomiting, diarrhea, muscle aches, very tired
- Tick exposure: yes or no
- Tick removal: date/time, where on body, attached or engorged, photos available
- How they look right now: drinking, peeing, alertness, breathing
A final reassuring note
If you made it this far, you are doing exactly what good parents do. RMSF is serious, but it is treatable, and early care makes a big difference. If your child has fever and rash in the days after tick exposure, do not try to puzzle it out alone at midnight. Call, describe the timeline, and let your clinician help you decide the safest next step.
Medical note: This article is educational and cannot diagnose your child. If you are concerned about RMSF or your child looks very ill, seek in-person care urgently.