RSV in Toddlers: Symptoms, Home Care, and When to Get Emergency Help
Sarah Mitchell
Sarah Mitchell is a Registered Pediatric Nurse and a mother of three who has spent over a decade helping families navigate the beautiful, chaotic early years of childhood. She combines evidence-based medical knowledge with real-world parenting experience to offer practical, compassionate advice. At Awesome Parent, Sarah's mission is to help exhausted parents find solutions, trust their instincts, and finally get some sleep.
RSV is one of those viruses that loves to show up when you are already running on fumes. In babies, we worry a lot about tiny airways and feeding. In toddlers, RSV often looks more like a “monster cold” or a wheezy cough that drags on. The tricky part is that toddlers can compensate for breathing trouble until they suddenly cannot.
So let’s make this simple and calm: what RSV looks like in toddlers, what you can safely do at home, how to spot breathing distress in a walking, talking kid, and exactly when symptoms cross into emergency territory.

What RSV is and why toddlers are different
RSV stands for respiratory syncytial virus. It is extremely common and spreads through droplets, close contact, and contaminated hands and surfaces. Many kids get RSV by age 2, and reinfections happen.
Why toddlers can look different than babies: toddlers have bigger airways and stronger muscles, so they often manage RSV better than infants. Instead of severe feeding issues, the “problem zone” tends to be cough, congestion, fever, poor sleep, and sometimes wheezing or an asthma-like flare.
That said, some toddlers do get quite sick, especially if they have asthma or reactive airway disease, a history of prematurity, congenital heart disease, chronic lung disease, or a weakened immune system.
RSV symptoms in toddlers
RSV in toddlers often starts like a cold and then causes more cough and lower-airway symptoms.
Common symptoms
- Runny nose and congestion
- Cough that can sound wet, harsh, or barky
- Fever (often in the first few days)
- Sore throat, decreased appetite
- Low energy, crankiness, poor sleep
- Wheezing or noisy breathing in some kids
How long does RSV last in toddlers?
Many toddlers are noticeably sick for about 5 to 7 days, but it can vary. The cough can linger for 2 to 4 weeks, especially if they tend to wheeze with viruses.
Often the roughest stretch is around days 3 to 5, when inflammation and mucus in the airways tend to peak. If breathing trouble is going to show up, it commonly shows up in this window.
When a lingering cough is worth a check: If cough is getting worse after the first week, lasts beyond about 3 to 4 weeks, disrupts sleep night after night, or comes with fever returning, fast breathing, chest pain, or poor energy, call your pediatrician to rule out complications (like pneumonia, an ear infection, or an asthma flare).
How to tell if breathing is a problem
With babies, we obsess over tiny nostrils and subtle chest movements. Toddlers are often a little louder and more obvious, which is actually helpful. The goal is to spot increased work of breathing, not just a noisy cough.
Watch for breathing distress
- Fast breathing that does not settle when they are resting
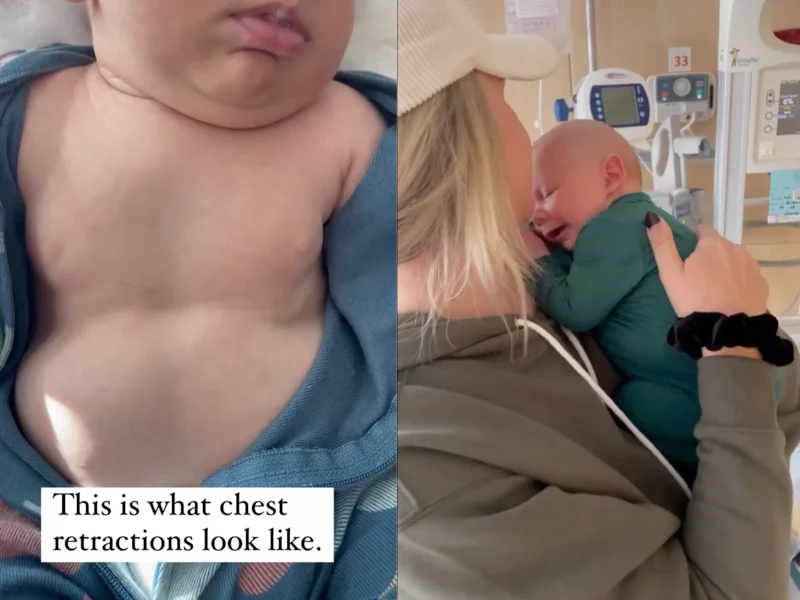
- Retractions: skin sucking in between ribs, under the ribs, or at the base of the neck
- Nasal flaring
- Head bobbing or using belly muscles to breathe
- Grunting with breaths
- Wheezing (a whistling sound, usually on exhale) or persistent tight, “can’t get air out” breathing
- Trouble speaking or crying normally because they cannot catch their breath
- Difficulty staying awake, unusual limpness, or “zoning out” with breathing that looks labored
- Color changes: blue or gray lips or face, or very pale and sweaty
Tip you can use tonight: Count breaths when your child is calm or asleep. A number by itself does not diagnose anything, but a clear jump from their normal plus visible work of breathing is a useful red flag to share with your clinician.
Home care for RSV in toddlers
There is no medication that “kills” RSV for most otherwise healthy toddlers. Home care is about keeping them comfortable, hydrated, and breathing as easily as possible while their body clears the virus. In specific high-risk situations, some hospitals use specialized treatments, but that is not routine for most toddlers and is guided by a clinician.
1) Clear the nose, especially before sleep
- Use saline spray or drops and encourage gentle nose blowing.
- If your toddler cannot blow well, you can use suction sparingly. Do not overdo it, since frequent suctioning can irritate the nose.
- A cool-mist humidifier can help with dry air and thick mucus. Clean it daily per manufacturer instructions.
2) Fluids, fluids, fluids
Dehydration sneaks up when kids are breathing fast and refusing food. Aim for frequent sips.
- Water is great.
- Oral rehydration solution is helpful if they have poor intake.
- Warm fluids like broth can soothe a scratchy throat if your child accepts them.
Good hydration signs: peeing at least every 6 to 8 hours (or at least several times a day), tears when crying, mouth not overly dry, and energy that perks up a bit after drinking.
3) Fever and comfort care
- Use acetaminophen or ibuprofen if your child is uncomfortable or not sleeping. Follow the dosing on the label or your pediatrician’s guidance based on weight and age.
- Do not give aspirin to children or teens.
- Be careful with combination “cold” products so you do not accidentally double-dose acetaminophen or ibuprofen.
- Dress in light layers.
- Skip “cold and cough” medicines for young children unless your pediatrician specifically recommends them.
4) Rest, but do not force strict bed rest
Quiet play, extra sleep, and low expectations are the vibe. Let your toddler choose books, shows, or calm activities. Fighting about naps rarely improves anyone’s oxygen levels.
5) If your toddler has asthma or has wheezed before
RSV can trigger wheezing. If your child has an asthma action plan or a prescribed rescue inhaler or nebulizer medication, follow your plan and call your pediatrician if symptoms are escalating.
If your child has never wheezed before and you hear a new whistling sound, that is worth a call to your clinic for guidance. Some clinicians will do a monitored bronchodilator trial, especially if there is an asthma history, but it is not helpful for every child with RSV.
Nurse-mom note: A toddler can have a loud cough and still be moving air just fine. What matters most is work of breathing, hydration, and responsiveness.
A note on home pulse oximeters: Consumer devices can be finicky on little fingers and can cause false reassurance or unnecessary panic. If you are worried about breathing, go by how your child looks and acts and get checked.
What not to do
- Do not use honey under age 1. For toddlers over 1, honey can help cough, especially at night.
- Avoid essential oils in humidifiers, especially around kids with sensitive airways.
- Do not smoke or vape around your child. Even “just outside” can increase symptoms, since residue clings to clothes and hair.
- Do not give leftover antibiotics. RSV is a virus. Antibiotics only help if your child develops a bacterial complication like an ear infection or pneumonia, and that needs a clinician assessment.
When RSV is an emergency
If you are debating whether it “counts,” you are not overreacting. Breathing problems in kids deserve fast attention. Trust that little internal alarm bell.
Go to the ER now or call emergency services if your toddler has:
- Blue, gray, or very pale lips or face
- Severe trouble breathing, including gasping, grunting, or pronounced retractions
- Cannot speak or cry normally due to breathing effort
- Struggling to stay awake, unusually limp, or hard to wake
- Pauses in breathing
- Signs of dehydration with lethargy, no urine for about 8 to 10 hours (or much less than usual), or inability to keep fluids down
- Any sudden worsening where your child looks or acts “not right”
Seek same-day care (call your pediatrician, urgent care) if:
- Breathing is faster than usual and not improving with rest
- Wheezing is new, worsening, or not responding to prescribed rescue medication
- Fever lasts more than 3 days, is very high, or fever returns after improving
- Your child has ear pain, persistent irritability, or new drainage from the ear (possible ear infection)
- Cough is worsening after day 5 to 7, or you are worried about pneumonia
- Your toddler has a high-risk medical condition (asthma, prematurity history, heart or lung disease, immunocompromise)

Daycare and preschool return
This is the question every parent asks, usually while staring at a calendar and trying to figure out how many favors they have left to call in.
RSV spreads easily, and toddlers are very efficient at sharing germs. Most childcare policies follow the same general illness guidelines.
A practical return checklist
- Fever-free for 24 hours without fever-reducing medicine
- Breathing comfortably during normal play, not working hard to breathe
- Energy is reasonably back (they can participate without crashing)
- Hydrating well and able to manage secretions
What about the cough? A lingering cough alone is common after RSV and does not always mean contagiousness is high. If your toddler is otherwise improving and can handle the day, many kids can return even with some cough, as long as fever is gone and breathing looks okay. If the cough is constant, disrupts sleep heavily, or your child is too worn out, give them another day if you can.
Contagious window: RSV is usually most contagious in the first several days of illness, and kids can spread it before symptoms are obvious. Some young children can shed virus longer, especially if immunocompromised.
How clinicians test and treat RSV
Many toddlers do not need a test. Clinicians often diagnose RSV based on symptoms and what they hear on the lung exam.
You may see:
- A nasal swab test for RSV or a respiratory panel in some settings
- Oxygen level check (pulse oximeter)
- An exam for complications like ear infections
Treatment may include:
- Supportive care advice (fluids, suction, fever management)
- Sometimes a monitored bronchodilator trial if wheezing is present, especially with an asthma history
- Supplemental oxygen or hospital monitoring if oxygen levels are low or work of breathing is high
Most toddlers recover at home. Hospital care is mainly for breathing support, hydration, and monitoring.
Preventing RSV and protecting siblings
You cannot bubble-wrap your toddler, and you should not have to. But you can reduce spread in ways that actually work.
- Hand washing before meals and after wiping noses
- Teach “catch your cough” into elbow, even if it is imperfect
- Clean high-touch surfaces like doorknobs, tablet screens, and toy handles
- Avoid sharing cups and utensils during illness
- Keep sick kids away from young infants when possible
If you have a new baby at home, RSV precautions matter a lot more. Consider having your toddler wash hands when they come home, change clothes if they were exposed to lots of germs, and keep kisses off the baby’s face during peak illness season. Hard? Yes. Worth it? Also yes.
Prevention update: There are newer RSV antibody immunization options (often called monoclonal antibodies) that can help protect some babies and certain high-risk young children during RSV season. Eligibility depends on age, medical history, and local guidance, so ask your pediatrician what applies to your family.

Quick recap
If your toddler has RSV, it is normal to see congestion, cough, fever, and lousy sleep. What is not normal is increasing work of breathing, blue or gray color, dehydration, or a child who is too tired to engage.
If you are unsure, call your pediatrician’s nurse line. As a former triage nurse, I can tell you: we would much rather talk you through a “probably okay” situation than miss the one kid who needs help.